Abstract
Background
The difficulties in the identification of C. auris and the delays in the implementation of infection control precautions contribute to outbreaks. This study analyzed 10 patients with COVID-19 and C. auris candidemia, their characteristic and clinical features and phylogenetic features, and the antifungal susceptibilities of the isolates.
Method
C. auris were detected in the COVID-19 ICU of a university hospital between January and August 2021. Identification to species level was performed using MALDI-TOF MS. Antifungal susceptibilities were determined by the Sensititre YeastOne YO10 panel. The isolates were whole genome sequenced to assess genetic relatedness and a phylogenetic tree was drawn including various C. auris clades.
Results
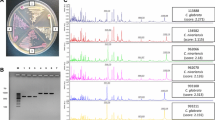
The mean growth time in blood cultures was 38.8 h. C. auris candidemia developed on the average 27th day of ICU admission. All were susceptible to anidulafungin and micafungin, while they were resistant to fluconazole and amphotericin B. Only three isolates were found to be resistant to caspofungin. All patients died. With the WGS method, all isolates were found in a close resemblance to each other in terms of total nucleotide similarity (with a minimum of 96% pairwise alignment). Our isolates showed the closest similarity to South Asian clade (Clade I).
Conclusions
This study is the first to evaluate the phylogenetic characteristics of C. auris using WGS and to determine antifungal susceptibilities in Türkiye on COVID-19 patients. The mortality rate was very high in patients who have both COVID-19 and C. auris candidemia.

Similar content being viewed by others
References
Centers for Disease Control and Prevention. Infection Prevention and Control for Candida auris. https://www.cdc.gov/fungal/candida-auris/c-auris-infection-control.html. Accessed 2022, July 12.
Kathuria S, Singh PK, Sharma C, Prakash A, Masih A, Kumar A, et al. Multidrug-resistant candida auris misidentified as candida haemulonii: characterization by matrix-assisted laser desorption ionization-time of flight mass spectrometry and DNA sequencing and its antifungal susceptibility profile variability by Vitek 2, CLSI broth microdilution, and Etest method. J Clin Microbiol. 2015;53(6):1823–30. https://doi.org/10.1128/JCM.00367-15.
Kim TH, Kweon OJ, Kim HR, Lee MK. Identification of uncommon Candida species using commercial identification systems. J Microbiol Biotechnol. 2016;26(12):2206–13. https://doi.org/10.4014/jmb.1609.09012.
Di Pilato V, Codda G, Ball L, Giacobbe DR, Willison E, Mikulska M, et al. Molecular epidemiological investigation of a nosocomial cluster of C. auris: evidence of recent emergence in Italy and ease of transmission during the COVID-19 pandemic. J Fungi (Basel). 2021;7(2). https://doi.org/10.3390/jof7020140
Chow NA, de Groot T, Badali H, Abastabar M, Chiller TM, Meis JF. Potential Fifth Clade of Candida auris, Iran, 2018. Emerg Infect Dis. 2019;25(9):1780–1. https://doi.org/10.3201/eid2509.190686.
Rudramurthy SM, Chakrabarti A, Paul RA, Sood P, Kaur H, Capoor MR, et al. Candida auris candidaemia in Indian ICUs: analysis of risk factors. J Antimicrob Chemother. 2017;72(6):1794–801. https://doi.org/10.1093/jac/dkx034.
Hoenigl M, Seidel D, Sprute R, Cunha C, Oliverio M, Goldman GH, et al. COVID-19-associated fungal infections. Nat Microbiol. 2022;7(8):1127–40. https://doi.org/10.1038/s41564-022-01172-2.
Reslan L, Araj GF, Finianos M, El Asmar R, Hrabak J, Dbaibo G, et al. Molecular characterization of Candida auris isolates at a major tertiary care center in Lebanon. Front Microbiol. 2021;12:770635. https://doi.org/10.3389/fmicb.2021.770635
Centers for Disease Control and Prevention (CDC), Tracking C.auris. https://www.cdc.gov/fungal/candida-auris/tracking-c-auris.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Ffungal%2Fdiseases%2Fcandidiasis%2Ftracking-c-auris.html. Accessed 21 July 2022.
Jeffery-Smith A, Taori SK, Schelenz S, Jeffery K, Johnson EM, Borman A, et al. Candida auris: a Review of the Literature. Clin Microbiol Rev. 2018;31(1). https://doi.org/10.1128/CMR.00029-17
Phua J, Weng L, Ling L, Egi M, Lim CM, Divatia JV, et al. Intensive care management of coronavirus disease 2019 (COVID-19): challenges and recommendations. Lancet Respir Med. 2020;8(5):506–17. https://doi.org/10.1016/S2213-2600(20)30161-2.
Komec S, Karabicak N, Ceylan AN, Gulmez A, Ozalp O. Three Candida auris case reports from Istanbul, Turkey. Mikrobiyol Bul. 2021;55(3):452–60. https://doi.org/10.5578/mb.20219814.
Bolukbasi Y, Erkose Genc G, Orhun G, Kuskucu MA, Cagatay A, Onel M, et al. First case of COVID-19 positive Candida auris Fungemia in Turkey. Mikrobiyol Bul. 2021;55(4):648–55. https://doi.org/10.5578/mb.20219716.
Kurt AF, Kuskucu MA, Balkan II, Baris A, Yazgan Z, Serife Oz A, et al. Candida auris Fungemia and a local spread taken under control with infection control measures: First report from Turkey. Indian J Med Microbiol. 2021;39(2):228–30. https://doi.org/10.1016/j.ijmmb.2021.03.007.
Centers for Disease Control and Prevention (CDC). C. auris: Antifungal susceptibility testing and interpretation, 2020. https://www.cdc.gov/fungal/candida-auris/c-auris-antifungal.html. Accessed May 29, 2020.
Gosselin S, Fullmer MS, Feng Y, Gogarten JP. Expanding the utility of sequence comparisons using data from whole genomes. bioRxiv. 2020:2020.01.15.908137. https://doi.org/10.1101/2020.01.15.908137
Letunic I, Bork P. Interactive Tree Of Life (iTOL) v5: an online tool for phylogenetic tree display and annotation. Nucleic Acids Res. 2021;49(W1):W293–6. https://doi.org/10.1093/nar/gkab301.
Rhodes J, Fisher MC. Global epidemiology of emerging Candida auris. Curr Opin Microbiol. 2019;52:84–9. https://doi.org/10.1016/j.mib.2019.05.008.
Mirhendi H, Charsizadeh A, Aboutalebian S, Mohammadpour M, Nikmanesh B, de Groot T, et al. South Asian (Clade I) Candida auris meningitis in a paediatric patient in Iran with a review of the literature. Mycoses. 2022;65(2):134–9. https://doi.org/10.1111/myc.13396.
Chybowska AD, Childers DS, Farrer RA. Nine things genomics can tell us about Candida auris. Front Genet. 2020;11:351. https://doi.org/10.3389/fgene.2020.00351.
Chen J, Tian S, Han X, Chu Y, Wang Q, Zhou B, et al. Is the superbug fungus really so scary? A systematic review and meta-analysis of global epidemiology and mortality of Candida auris. BMC Infect Dis. 2020;20(1):827. https://doi.org/10.1186/s12879-020-05543-0.
Lone SA, Ahmad A. Candida auris-the growing menace to global health. Mycoses. 2019;62(8):620–37. https://doi.org/10.1111/myc.12904.
Kayaaslan B, Eser F, Kaya Kalem A, Bilgic Z, Asilturk D, Hasanoglu I, et al. Characteristics of candidemia in COVID-19 patients; increased incidence, earlier occurrence and higher mortality rates compared to non-COVID-19 patients. Mycoses. 2021;64(9):1083–91. https://doi.org/10.1111/myc.13332.
Riche CVW, Cassol R, Pasqualotto AC. Is the frequency of Candidemia increasing in COVID-19 patients receiving corticosteroids? J Fungi (Basel). 2020;6(4). https://doi.org/10.3390/jof6040286
Zhang Z, Zhu R, Luan Z, Ma X. Risk of invasive candidiasis with prolonged duration of ICU stay: a systematic review and meta-analysis. BMJ Open. 2020;10(7):e036452. https://doi.org/10.1136/bmjopen-2019-036452
Public Health England. Guidance for the labrotory investigation, management and infection prevention and control for cases of Candida auris. . https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/637685/Updated_Candida_auris_Guidance_v2.pdf. Accessed 2017, August 11.
Alsuhaibani M, Kobayashi T, McPherson C, Holley S, Marra AR, Trannel A, et al. Impact of COVID-19 on an infection prevention and control program, Iowa 2020–2021. Am J Infect Control. 2022;50(3):277–82. https://doi.org/10.1016/j.ajic.2021.11.015.
Prestel C, Anderson E, Forsberg K, Lyman M, de Perio MA, Kuhar D, et al. Candida auris Outbreak in a COVID-19 Specialty Care Unit—Florida, July–August 2020. MMWR Morb Mortal Wkly Rep. 2021;70(2):56–7. https://doi.org/10.15585/mmwr.mm7002e3
Villanueva-Lozano H, Trevino-Rangel RJ, Gonzalez GM, Ramirez-Elizondo MT, Lara-Medrano R, Aleman-Bocanegra MC, et al. Outbreak of Candida auris infection in a COVID-19 hospital in Mexico. Clin Microbiol Infect. 2021. https://doi.org/10.1016/j.cmi.2020.12.030.
Lockhart SR, Etienne KA, Vallabhaneni S, Farooqi J, Chowdhary A, Govender NP, et al. Simultaneous emergence of multidrug-resistant Candida auris on 3 continents confirmed by whole-genome sequencing and epidemiological analyses. Clin Infect Dis. 2017;64(2):134–40. https://doi.org/10.1093/cid/ciw691.
Sharma C, Kumar N, Pandey R, Meis JF, Chowdhary A. Whole genome sequencing of emerging multidrug resistant Candida auris isolates in India demonstrates low genetic variation. New Microbes New Infect. 2016;13:77–82. https://doi.org/10.1016/j.nmni.2016.07.003.
Funding
This study was supported by Gilead Sciences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the authorship and/or publication of this article.
Ethical approval
Marmara University School of Medicine Institutional Ethical Review Board issued approval 09.2021.578. The collected data did not include any patient or employee identifying information.
Additional information
Handling Editor: Macit Ilkit.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Erturk Sengel, B., Ekren, B.Y., Sayin, E. et al. Nosocomial infection of C. auris in COVID-19 Intensive Care Unit in Türkiye and Phylogenetic Analysis of Isolates. Mycopathologia 188, 765–773 (2023). https://doi.org/10.1007/s11046-023-00782-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-023-00782-6