Abstract
Background
Colorectal cancer is the 4th leading cause of cancer related deaths affecting both men and women worldwide. In the present study, any probable role of MTDH mRNA expression in CRC tumorigenesis was explored using both discovery and validation cohorts.
Methods and results
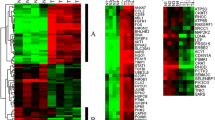
After prior ethical and biosafety approvals, tumor tissue samples along with their adjacent controls were collected for this study from Pakistani patients diagnosed with colorectal cancer. RNA was isolated using Trizol reagent, followed by cDNA synthesis. Transcript analysis of MTDH was performed by using qPCR. Moreover, genome-wide expression of MTDH was also determined through micro-array data analysis using BRB-array tools software. MTDH expression was significantly high in tumor tissue samples (p < 0.05) compared to their respective controls. Likewise, results of microarray analysis also revealed overamplification of MTDH in tumor samples as compared to controls. Expression of MTDH was also found to be positively correlated with KI-67 index (p < 0.05) and were observed to be significantly upregulated in advance tumor grade (p < 0.05) and stage (p < 0.05). However, no association of MTDH overexpression with age and gender could be established.
Conclusion
Hence, it can be concluded that MTDH is a core element that plays a pivotal role in colorectal tumorigenesis irrespective of patient’s age and gender. Molecular insight into the tumor microenvironment revealed MTDH as a niche, representing distinctive framework for cancer progression, thus, making it an innovative target strategy for colorectal cancer treatment.





Similar content being viewed by others
Data availability
Data used in this study can be obtained from corresponding author on special request. Data sets used for in-silico study can be assessed through GEO- NCBI website under the accession numbers provided in this study.
Abbreviations
- CRC:
-
Colorectal cancer
- MTDH:
-
Metadherin
- MMPs:
-
Matrix metallo proteases
- CIN:
-
Chromosomal instability
- MSI:
-
Microsatellite instability
References
Navarro M, Nicolas A, Ferrandez A, Lanas A (2017) Colorectal cancer population screening programs worldwide in 2016: an update. World J Gastroenterol 23(20):3632. https://doi.org/10.3748/wjg.v23.i20.3632
Porru M, Pompili L, Caruso C, Biroccio A, Leonetti C (2018) Targeting KRAS in metastatic colorectal cancer: current strategies and emerging opportunities. J Exp Clin Cancer Res. https://doi.org/10.1186/s13046-018-0719-1
Cox A, Fesik S, Kimmelman A, Luo J, Der C (2014) Drugging the undruggable RAS: mission possible? Nat Rev Drug Discov 13(11):828–851. https://doi.org/10.1038/nrd4389
Srivastava J, Siddiq A, Gredler R, Shen X, Rajasekaran D, Robertson C, Subler M, Windle J, Dumur C, Mukhopadhyay N, Garcia D, Lai Z, Chen Y, Balaji U, Fisher P, Sarkar D (2015) Astrocyte elevated gene-1 and c-Myc cooperate to promote hepatocarcinogenesis in mice. Hepatology 61(3):915–929. https://doi.org/10.1002/hep.25868
Sriramulu S, Nandy S, Ganesan H, Banerjee A, Pathak S (2021) In silico analysis and prediction of transcription factors of the proteins interacting with astrocyte elevated gene-1. Comput Biol Chem 92:107478. https://doi.org/10.1016/j.compbiolchem.2021.107478
Lin L, Lai P, Chen Y, Chen C (2021) Expression of astrocyte-elevated gene-1 indicates prognostic value of fluoropyrimidine-based adjuvant chemotherapy in resectable stage III colorectal cancer. Pathol Int. https://doi.org/10.1111/pin.13160
Wang X, Cai L, Ye F, Li M, Ma L, Geng C, Song Z, Liu Y (2019) Elevated expression of MTDH predicts better prognosis of locally advanced HER-2 positive breast cancer patients receiving neoadjuvant chemotherapy plus trastuzumab. Medicine 98(36):e16937. https://doi.org/10.1097/md.0000000000016937
Haan J, Bhaskaran R, Mittempergher L, Lujinovic E, Audeh W, Penault-Llorca F, Glas A (2020) 220P Annotating mammaprint and blueprint gene profile to the hallmarks of cancer and understanding the biology of mammaprint extreme risk groups. Ann Oncol 31:S329. https://doi.org/10.1016/j.annonc.2020.08.342
Zhang Y, Wang Y, Wang J (2017) MicroRNA-584 inhibits cell proliferation and invasion in non-small cell lung cancer by directly targeting MTDH. Exp Ther Med. https://doi.org/10.3892/etm.2017.5624
Rong C, Shi Y, Huang J, Wang X, Shimizu R, Mori Y et al (2020) The effect of metadherin on NF-κB activation and downstream genes in ovarian cancer. Cell Transplant. https://doi.org/10.1177/0963689720905506
Hu K, Mu X, Kolibaba H, Yin Q, Liu C, Liang X, Lu J (2018) Metadherin is an apoptotic modulator in prostate cancer through miR-342-3p regulation. Saudi J Biol Sci 25(5):975–981. https://doi.org/10.1016/j.sjbs.2018.04.015
Gnosa S, Ticha I, Haapaniemi S, Sun X (2016) MTDH genetic variants in colorectal cancer patients. Sci Rep. https://doi.org/10.1038/srep23163
Qadir J, Riaz S, Sahar N, Aman D, Khan M, Malik M (2019) Transcriptional elucidation of tumor necrosis factor-α-mediated nuclear factor-κB1 activation in breast cancer cohort of Pakistan. J Cancer Res Ther. https://doi.org/10.4103/jcrt.jcrt_484_18
Schmittgen T, Livak K (2008) Analyzing real-time PCR data by the comparative CT method. Nat Protoc 3(6):1101–1108. https://doi.org/10.1038/nprot.2008.73
Zhu Y, Zhou K, Ruan L, Sun F, Wang G, Li W (2019) Metadherin overexpression in perihilar cholangiocarcinoma is associated with lymph node metastasis and poor prognosis. Oncol Lett. https://doi.org/10.3892/ol.2019.10141
Buffart T, van Grieken N, Tijssen M, Coffa J, Ylstra B, Grabsch H, van de Velde C, Carvalho B, Meijer G (2009) High resolution analysis of DNA copy-number aberrations of chromosomes 8, 13, and 20 in gastric cancers. Virchows Arch 455(3):213–223. https://doi.org/10.1007/s00428-009-0814-y
de Krijger R, Claessen S, van der Ham F, van Unnik A, Hulsbergen-van de Kaa C, van Leuven L et al (2007) Gain of chromosome 8q is a frequent finding in pleuropulmonary blastoma. Mod Pathol 20(11):1191–1199. https://doi.org/10.1038/modpathol.3800953
Walker L, McDonald M, Wells J, Harris G, Robinson B, Morris C (2013) Dual-color fluorescence in situ hybridization reveals an association of chromosome 8q22 but not 8p21 imbalance with high grade invasive breast carcinoma. PLoS ONE 8(7):e70790. https://doi.org/10.1371/journal.pone.0070790
Tomita Y, Dorward H, Yool A, Smith E, Townsend A, Price T, Hardingham J (2017) Role of aquaporin 1 signalling in cancer development and progression. Int J Mol Sci 18(2):299. https://doi.org/10.3390/ijms18020299
Yusufu A, Shayimu P, Tuerdi R, Fang C, Wang F, Wang H (2019) TFF3 and TFF1 expression levels are elevated in colorectal cancer and promote the malignant behavior of colon cancer by activating the EMT process. Int J Oncol. https://doi.org/10.3892/ijo.2019.4854
Khatri A, Williams B, Fisher J, Brundage R, Gurvich V, Lis L, Skubitz K, Dudek A, Greeno E, Kratzke R, Lamba J, Kirstein M (2013) SLC28A3 genotype and gemcitabine rate of infusion affect dFdCTP metabolite disposition in patients with solid tumours. Br J Cancer 110(2):304–312. https://doi.org/10.1038/bjc.2013.738
Horn D, Hess J, Freier K, Hoffmann J, Freudlsperger C (2015) Targeting EGFR-PI3K-AKT-mTOR signaling enhances radiosensitivity in head and neck squamous cell carcinoma. Expert Opin Ther Targets 19(6):795–805. https://doi.org/10.1517/14728222.2015.1012157
Tsai W, Aiba I, Long Y, Lin H, Feun L, Savaraj N, Kuo M (2012) Activation of Ras/PI3K/ERK pathway induces c-Myc stabilization to upregulate argininosuccinate synthetase, leading to arginine deiminase resistance in melanoma cells. Can Res 72(10):2622–2633. https://doi.org/10.1158/1538-7445.am2012-5610
Yoo B, Emdad L, Su Z, Villanueva A, Chiang D, Mukhopadhyay N, Mills A, Waxman S, Fisher R, Llovet J, Fisher P, Sarkar D (2009) Astrocyte elevated gene-1 regulates hepatocellular carcinoma development and progression. J Clin Investig 119(3):465–477. https://doi.org/10.1172/JCI36460
Jiang T, Zhu A, Zhu Y, Piao D (2012) Clinical implications of AEG-1 in liver metastasis of colorectal cancer. Med Oncol 29(4):2858–2863. https://doi.org/10.1007/s12032-012-0186-z
Wang J, Li J, Chen L, Fan Z, Cheng J (2020) MicroRNA-499 suppresses the growth of hepatocellular carcinoma by downregulating astrocyte elevated gene-1. Technol Cancer Res Treat. https://doi.org/10.1177/1533033820920253
Yang S, Cho M, Kim N (2018) Difference between right-sided and left-sided colorectal cancers: from embryology to molecular subtype. Expert Rev Anticancer Ther 18(4):351–358. https://doi.org/10.1080/14737140.2018.1442217
Acknowledgements
Authors of this study are grateful to Higher Education Commission of Pakistan and COMSATS University, Islamabad for research facilitation for this study.
Funding
We are grateful to COMSATS University and HEC for needful funding and research support.
Author information
Authors and Affiliations
Contributions
AS drafted the project, executed wet lab and in-silico experiments, performed micro array data analysis and statistical data analysis, prepared tables and figures and wrote the research paper. NES contributed equally and performed lab experiments, microarray data analysis study and revised the manuscript. SKR helped in data analysis and preparation of table and figures. JQ revised and edited the manuscript. SHW and TK performed surgeries and helped in sample collection. MFAM designed and supervised the study and reviewed the final draft of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors of the study have no conflict of interest to declare.
Ethical approval
In order to conduct this study, ethical consent was obtained from the Ethical Committees of Pakistan Institute of Medical Sciences (PIMS) hospital and COMSATS University Islamabad.
Consent to participate
Informed consents of all participants (patients) were obtained to conduct this study.
Consent for publication
All authors of the study showed agreement to publish this study in Molecular Biology Reports journal.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sultan, A., Sahar, NE., Riaz, S.K. et al. Metadherin (MTDH) overexpression significantly correlates with advanced tumor grade and stages among colorectal cancer patients. Mol Biol Rep 48, 7999–8007 (2021). https://doi.org/10.1007/s11033-021-06834-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-021-06834-8