Abstract
Objectives
This paper examines the gestational age at first antenatal care (ANC) visit and factors associated with timely initiation of ANC in Malawi in a context where maternal and child health services are generally provided for free.
Methods
Lognormal survival models are applied to Demographic and Health Survey data from a nationally representative sample of women (n = 13,588) of child-bearing age.
Results
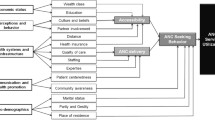
The findings of this study show that less than 30 % of pregnant women initiate ANC within the World Health Organization recommended gestational timeframe of 16 weeks or earlier. The hazard analysis shows a gradient in the initiation of ANC by maternal education level, with least educated mothers most likely to delay their first ANC visit. However, after adjusting for variables capturing intimate partner violence in the multivariate models, the effect of maternal education attenuated and lost statistical significance. Other significant predictors of gestational age at first ANC include media exposure, perceived distance from health facility, age, and birth order.
Conclusions for Practice
The findings of the study link domestic violence directly with the gestational age at which mothers initiate ANC, suggesting that gender-based violence may operate through delayed initiation of ANC to undermine maternal and child health outcomes.


Similar content being viewed by others
References
World Health Organization. (2001). Who antenatal care randomized trial: Manual for the implementation of the new model. Geneva: WHO.
World Health Organization. (2002). Antenatal care randomized trial: Manual for implementation of the new model. Geneva: WHO.
Lawn, J. E., Cousens, S., & Zupan, J. (2005). 4 million neonatal deaths: When? Where? Why? The Lancet, 365(9462), 891–900.
Alderliesten, M., Vrijkotte, T. G. M., Van Der Wal, M., & Bonsel, G. (2007). Late start of antenatal care among ethnic minorities in a large cohort of pregnant women. BJOG: An International Journal of Obstetrics and Gynaecology, 114(10), 1232–1239.
Say, L., Chou, D., Gemmill, A., Tunçalp, Ö., Moller, B., Daniels, J., et al. (2014). Global causes of maternal death: A WHO systematic analysis. The Lancet Global Health, 2, e323–e333.
Magadi, M., Madise, N. J., & Rodrigues, R. N. (2000). Frequency and timing of antenatal care in Kenya: Explaining the variations between women of different communities. Social Science and Medicine, 51(4), 551–561.
Mrisho, M., Brigit Obrist, B., Schellenberg, J. A., Haws, R. A., Mushi, A. K., Mshinda, H., et al. (2009). The use of antenatal and postnatal care: Perspectives and experiences of women and health care providers in rural southern Tanzania. BMC Pregnancy and Childbirth, 9(1), 1–12.
Anya, S., Abba, H., & Lamin, E. (2008). Antenatal care in The Gambia: Missed opportunity for information, education and communication. BMC Pregnancy and Childbirth, 8(1), 9.
Simkhada, B., Teijlingen, E., Porter, M., & Simkhada, P. (2008). Factors affecting the utilization of antenatal care in developing countries: Systematic review of the literature. Journal of Advanced Nursing, 61(3), 244–260.
Myer, L., & Harrison, A. (2003). Why do women seek antenatal care late? Perspectives from rural South Africa. Journal of Midwifery and Women’s Health, 48(4), 268–272.
Cleland, J. G., & van Ginneken, J. (1988). Maternal education and child survival in developing countries: The search for pathways of influence. Social Science and Medicine, 27(12), 1357–1368.
Caldwell, J. C. (1996). Routes to low mortality m poor countries. Population and Development Review, 12, 171.
Malawi Government. (2010). Malawi Demographic and Health Survey Report, Lilongwe.
Royston, P. (2001). The lognormal distribution as a model for survival time in cancer, with an emphasis on prognostic factors. Statistica Neerlandica, 55, 89–104.
Lawless, J. F. (1982). Statistical models and methods for lifetime data. New York: Wiley.
Tripepi, G. K., Jager, J., Dekker, F., & Zoccali, C. (2008). Linear and logistic regression analysis. Kidney International, 73(7), 806–810.
Snijders, T., & Bosker, R. (2012). Multilevel analysis: An introduction to basic and advanced multi-level modelling (2nd ed.). Los Angeles: Sage.
Singer, J. D., & Willett, J. B. (2003). Applied longitudinal data analysis: Modeling change and event occurrence. New York: Oxford University Press.
Fisher, J. D., Fisher, W. A., Bryan, A. D., & Misovich, S. J. (2002). Information-motivation-behavioral skills model-based HIV risk behavior change intervention for inner-city high school youth. Health Psychology, 21(2), 177.
Jamisse, L., Songane, F., Libombo, A., Bique, C., & Faúndes, A. (2004). Reducing maternal mortality in Mozambique: Challenges, failures, successes and lessons learned. International Journal of Gynecology and Obstetrics, 85(2), 203–212.
Hart, J. T. (1971). The inverse care law. Lancet, 297(7696), 405–412.
Stock, R. (1983). Distance and the utilization of health facilities in rural Nigeria. Social Science and Medicine, 17(9), 563–570.
Horton, S. (1988). Birth order and child nutritional status: Evidence from the Philippines. Economic Development and Cultural Change, 36(2), 341–354.
Ministry of Health and Social Welfare and ICF Macro. (2010). Lesotho Demographic and Health Survey, 2009. Maseru.
Granja, A. C., Zacarias, E., & Bergström, S. (2002). Violent deaths: The hidden face of maternal mortality. BJOG: International Journal of Obstetrics and Gynaecology, 109(1), 5–8.
Malawi Government. (2004). Malawi Demographic and Health Survey Report, Lilongwe.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mkandawire, P. Gestational Age at First Antenatal Care Visit in Malawi. Matern Child Health J 19, 2366–2374 (2015). https://doi.org/10.1007/s10995-015-1754-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-015-1754-6