Abstract
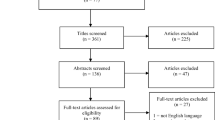
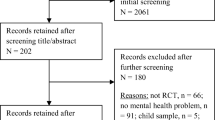
This study consists of an integrative review of the scientific literature that aimed to know the religious and spiritual practices used by children and adolescents to cope with cancer. From searches in the databases/libraries CINAHL, PsycINFO, PubMed, SciELO and Lilacs (2009–2019), the final sample consisted of 20 articles. Prayers were the most widely used practices, followed by sacred books and objects, going to sacred places and the use of music. Improvements in well-being, physical and emotional health have been reported. It is concluded that such practices should be recognized as important resources in coping with cancer illness in this population.

Similar content being viewed by others
Change history
26 June 2021
A Correction to this paper has been published: https://doi.org/10.1007/s10943-021-01315-5
References
Afungchwi, G. M., Hesseling, P. B., & Ladas, E. J. (2017). The role of traditional healers in the diagnosis and management of Burkitt lymphoma in Cameroon: Understanding the challenges and moving forward. BMC Complementary and Alternative Medicine, 17(209), 1–7.
Ahmadi, F., et al. (2018). Religion, culture and illness: A sociological study on religious coping in Iran. Mental Health, Religion & Culture, 21(7), 721–736.
Al Omari, O., Wynaden, D., Al-Omari, H., & Khatatbeh, M. (2017). Coping strategies of Jordanian adolescents with cancer: An interpretive phenomenological analysis study. Journal of Pediatric Oncology Nursing, 34(1), 35–43.
Austin, P., Macdonald, J., & MacLeod, R. (2018). Measuring spirituality and religiosity in clinical settings: A scoping review of available instruments. Religions, 9(3), 70.
Barton, K. S., et al. (2018). I’m not a spiritual person. How hope might facilitate conversations about spirituality among teens and young adults with cancer. Journal of Pain and Symptom Management, 55(6), 1599–1608.
Beyea, S., & Nichll, L. H. (1998). Writing an integrative review. AORN Journal, 67(4), 877–881.
Cadge, W., & Ecklund, E. H. (2009). Prayers in the clinic: How pediatric physicians respond. Southern Medical Journal, 102(12), 1218–1221.
Carey, L. B., & Cohen, J. (2010). Health care chaplains and their role on institutional ethics committees: An Australia study. Journal of Religion and Health, 49(2), 221–232. https://doi.org/10.1007/s10943-009-9241-2.
Carey, L. B., Swinton, J., & Grossoehme, D. (2018). Chaplaincy and spiritual care. In L. B. Carey & B. A. Mathisen (Eds.), Spiritual care for allied health practice: A person-centered approach (pp. 229–256). London: Jessica Kingsley Publishers. https://aus.jkp.com/products/spiritual-care-for-allied-health-practice.
Cheng, Y. C., et al. (2016). The lived experiences of aboriginal adolescent survivors of childhood cancer during the recovering process in Taiwan: A descriptive qualitative research. European Journal of Oncology Nursing, 22, 78–84.
Cohen, A. B., & Koenig, H. G. (2003). Religion, religiosity and spirituality in the biopsychosocial model of health and ageing. Ageing International, 28(3), 215–241.
Corrêa, C. V., Batista, J. S., & Holanda, A. F. (2016). Coping religioso/espiritualemprocessos de saúde e doença: Revisão da produçãoemperiódicosbrasileiros (2000–2013). RevistaPsicoFAE: PluralidadesemSaúde Mental, 5(1), 61–78.
Cunha, V. F. D., Pillon, S. C., Zafar, S., Wagstaff, C., & Scorsolini-Comin, F. (2020). Brazilian nurses’ concept of religion, religiosity, and spirituality: A qualitative descriptive study. Nursing & Health Sciences, 22(4), 1161–1168.
Darby, K., Nash, P., & Nash, S. (2014). Understanding and responding to spiritual and religious needs of young people with cancer. Cancer Nursing Practice, 13(2), 32–37.
De Vries, M. C., et al. (2013). What constitutes the best interest of a child? Views of parents, children, and physicians in a pediatric oncology setting. AJOB Primary Research, 4(2), 1–10.
Fitchett, G., et al. (2011). The role of professional chaplains on pediatric palliative care teams: Perspectives from physicians and chaplains. Journal of Palliative Medicine, 14(6), 704–707.
Galvão, T. F., Pansani, T. D. S. A., & Harrad, D. (2015). Principaisitens para relatarrevisõessistemáticas e meta-análises: A recomendação PRISMA. Epidemiologia e Serviços de Saúde, 24, 335–342.
Gardner, M. H., et al. (2017). Demographic, medical, and psychosocial predictors of benefit finding among caregivers of childhood cancer survivors. Psycho-Oncology, 26(1), 125–132.
Guedes, A. K. C., Pedrosa, A. P. A., Osório, M. O., & Pedrosa, T. F. (2019). Cuidadospaliativosemoncologiapediátrica: Perspectivas de profissionais de saúde. Revista da SBPH, 22(2), 128–148.
James, W. (2017). Religião e neurologia. Asvariedades da experiênciareligiosa: Um estudosobre a naturezahumana. (pp. 15–35). São Paulo, Brasil.
Jim, H. S., et al. (2015). Religion, spirituality, and physical health in cancer patients: A meta-analysis. Cancer, 121(21), 3760–3768.
Jones, B. L., et al. (2010). The meaning of surviving cancer for latino adolescents and emerging young adults. Cancer Nursing, 33(1), 74–81.
Juvakka, T., & Kylmä, J. (2009). Hope in adolescents with cancer. European Journal of Oncology Nursing, 13(3), 193–199.
Kamper, R., Van Cleve, L., & Savedra, M. (2010). Children with advanced cancer: Responses to a spiritual quality of life interview. Journal for Specialists in Pediatric Nursing, 15(4), 301–306.
King, M. B., & Koenig, H. G. (2009). Conceptualising spirituality for medical research and health service provision. BMC Health Services Research, 9(1), 1–7.
Koenig, H. G. (2012). Religion, spirituality, and health: The research and clinical implications. ISRN Psychiatry, 2012, 278730.
Koenig, H., Al-Zaben, F., & VanderWeele, T. (2020). Religion and psychiatry: Recent developments in research. BJPsych Advances, 26(5), 262–272.
Kohi, T. W., Von Essen, L., Masika, G. M., Gottvall, M., & Dol, J. (2019). Cancer-related concerns and needs among young adults and children on cancer treatment in Tanzania: A qualitative study. BMC Cancer, 19(1), 82.
Laplantine, F. (1986). Antropologia da doença. . Martins Fontes.
Lazarus, R. S., De Longis, A., Folkman, S., & Gruen, R. (1985). Stress and adaptational outcomes: The problem of confounded measures. American Psychologist, 40(7), 770–779.
Lion, A. H., Skiles, J. L., Watson, B. N., Young, J. D., & Torke, A. M. (2019). Chaplain care in pediatric oncology: Insight for interprofessional collaboration. Pediatric Blood & Cancer, 66(12), e27971.
Loewenthal, K. M. (2013). Religion, spirituality, and culture: Clarifying the direction of effects. In K. I. Pargament, J. J. Exline, & J. W. Jones (Eds.), APA handbooks in psychology®. APA handbook of psychology, religion, and spirituality (Vol. 1): Context, theory, and research. (pp. 239–255). American Psychological Association.
Magni, M. C., et al. (2015). New strategies to ensure good patient–physician communication when treating adolescents and young adults with cancer: The proposed model of the Milan Youth Project. Clinical Oncology in Adolescents and Young Adults, 5, 63–73.
Mahayati, S. L., Allenidekania, & Happy, H. (2018). Spirituality in adolescents with cancer. Enfermeria Clinica, 28, 31-35
Marques, L. F. (2010). O conceito de espiritualidade e sua interface com a religiosidade e a PsicologiaPositiva. Psicodebate, 10, 135–152.
Martel, D., et al. (2005). Use of alternative and complementary therapies in children with cancer. Pediatric Blood & Cancer, 44(7), 660–668.
McNeil, S. B. (2016). Spirituality in adolescents and young adults with cancer: A review of literature. Journal of Pediatric Oncology Nursing, 33(1), 55–63.
Moore, K., Talwar, V., Gomez-Garibello, C., Bosacki, S., & Moxley-Haegert, L. (2017). Children’s spirituality: Exploring spirituality in the lives of cancer survivors and a healthy comparison group. Journal of Health Psychology, 25(7), 888–899.
Nash, P., Bartel, M., & Nash, S. (2018) (Eds). Paediatric chaplaincy: Principles, practices and skills. London: Jessica Kingsley Publishers.
Nash, S., Nash, P., & Darby, K. (2015). Spiritual care with sick children and young people: A handbook for chaplains, paediatric health professionals, arts therapists and youth workers. London: Jessica Kingsley Publishers.
Njuguna, F., et al. (2015). Parental experiences of childhood cancer treatment in Kenya. Supportive Care in Cancer, 23(5), 1251–1259.
Ouzzani, M., Hammady, H., Fedorowicz, Z., & Elmagarmid, A. (2016). Rayyan - A web and mobile app for systematic reviews. Systematic Reviews, 5(1), 210.
Paisley, M. A., Kang, T. I., Insogna, I. G., & Rheingold, S. R. (2011). Complementary and alternative therapy use in pediatric oncology patients with failure of frontline chemotherapy. Pediatric Blood & Cancer, 56(7), 1088–1091.
Park, C. L., Holt, C. L., Le, D., Christie, J., & Williams, B. R. (2018). Positive and negative religious coping styles as prospective predictors of well-being in African Americans. Psychology of Religion and Spirituality, 10(4), 318–326.
Pesut, B., Sinclair, S., Fitchett, G., Greig, M., & Koss, S. E. (2016). Health care chaplaincy: A scoping review of the evidence 2009–2014. Journal of Health Care Chaplaincy, 22(2), 67–84.
Pourtsidis, A., et al. (2015). Prayer and blessings focused for healing is the most popular complementary intervention in a paediatric oncology unit in Greece. Journal of BUON, 20(2), 602–607.
Pravin, R. R., Enrica, T., & Moy, T. A. (2019). The portrait of a dying child. Indian Journal of Palliative Care, 25(1), 156–160.
Proserpio, T., et al. (2014). Spiritual aspects of care for adolescents with cancer. Tumori Journal, 100(4), 130–135.
Proserpio, T., et al. (2016). Spiritual support for adolescent cancer patients: A survey of pediatric oncology centers in Italy and Spain. Tumori Journal, 102(4), 376–380.
Proserpio, T., et al. (2020). Spirituality and sustaining hope in adolescents with cancer: The patients’ view. Journal of Adolescent and Young Adult Oncology, 9(1), 36–40.
Proserpio, T., Ferrari, A., Clerici, C. A., & Massimino, M. (2019). Spiritual support: A model of care not to forget. Pediatric Blood & Cancer, 66(10), e27818.
Proserpio, T., Piccinelli, C., & Clerici, C. A. (2011). Pastoral care in hospitals: A literature review. Tumori Journal, 97(5), 666–671. https://doi.org/10.1700/989.10729.
Puchalski, C., et al. (2009). Improving the quality of spiritual care as a dimension of palliative care: The report of the Consensus Conference. Journal of Palliative Medicine, 12(10), 885–904.
Puchalski, C. M., Vitillo, R., Hull, S. K., & Reller, N. (2014). Improving the spiritual dimension of whole person care: Reaching national and international consensus. Journal of Palliative Medicine, 17(6), 642–656.
Revuelta-Iniesta, R., et al. (2014). Complementary and alternative medicine usage in Scottish children and adolescents during cancer treatment. Complementary Therapies in Clinical Practice, 20(4), 197–202.
Siqueira, H. B. D. O. M., Santos, M. A., Gomez, R. R. F., Saltareli, S., & Sousa, F. A. E. F. (2015). Expressão da dornacriança com câncer: Uma compreensãofenomenológica. Estudos de Psicologia, 32(4), 663–674.
Snider, A. M., & McPhedran, S. (2014). Religiosity, spirituality, mental health, and mental health treatment outcomes in Australia: A systematic literature review. Mental Health, Religion & Culture, 17(6), 568–581.
Souza, V. D. M., Frizzo, H. C. F., Paiva, M. H. P. D., Bousso, R. S., & Santos, Á. D. S. (2015). Spirituality, religion and personal beliefs of adolescents with cancer. RevistaBrasileira de Enfermagem, 68(5), 791–796.
Sposito, A. M. P., et al. (2015). Coping strategies used by hospitalized children with cancer undergoing chemotherapy. Journal of Nursing Scholarship, 47(2), 143–151.
Sprik, P., et al. (2021). Feasibility and acceptability of a telephone-based chaplaincy intervention in a large, outpatient oncology center. Supportive Care in Cancer, 29(3), 1275–1285.
Steinhauser, K. E., et al. (2017). State of the science of spirituality and palliative care research part I: Definitions, measurement, and outcomes. Journal of Pain and Symptom Management, 54(3), 428–440.
Vazifeh, M. D., Hojjati, H., & Farhangi, H. (2019). Effect of spiritual care based on GhalbeSalim on anxiety in adolescent with cancer. Journal of Religion and Health, 59, 2857–2865. https://doi.org/10.1007/s10943-019-00869-9.
Velez-Florez, G., et al. (2018). Mind-body therapies in childhood cancer. Current Psychiatry Reports, 20(8), 58.
Victor, C. G. P., & Treschuk, J. V. (2020). Critical literature review on the definition clarity of the concept of faith, religion, and spirituality. Journal of Holistic Nursing, 38(1), 107–113.
Wilson, K., Mazhar, W., Rojas-Cooley, T., De Rosa, V., & Van Cleve, L. (2011). A glimpse into the lives of 3 children: Their cancer journey. Journal of Pediatric Oncology Nursing, 28(2), 100–106.
Yeh, C. H. (2001). Religious beliefs and practices of Taiwanese parents of pediatric patients with cancer. Cancer Nursing, 24(6), 476–482.
Zimmer, Z., et al. (2016). Spirituality, religiosity, aging and health in global perspective: A review. SSM-Population Health, 2, 373–381.
Funding
This study was financed by the Coordination for the Improvement of Higher Education Personnel (CAPES) and by the National Council for Scientific and Technological Development (CNPq).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The first autor has received research grants from Coordination for the Improvement of Higher Education Personnel (CAPES). Organization linked to the Ministry of Education of Brazil. The third author has financial support from the Nacional Council for Scientific and Technological Development (CNPq). According to ethical standards, this manuscript has no other conflict of interest.
Human and Animal Rights
This manuscript does not involve procedures with humans, animals or biological material.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rossato, L., Ullán, A.M. & Scorsolini-Comin, F. Religious and Spiritual Practices Used by Children and Adolescents to Cope with Cancer. J Relig Health 60, 4167–4183 (2021). https://doi.org/10.1007/s10943-021-01256-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10943-021-01256-z