Abstract
Purpose
To assess the feasibility of Transcranial Doppler ultrasonography (TCD) neuromonitoring in a general intensive care environment, in the prognosis and outcome prediction of patients who are in coma due to a variety of critical conditions.
Methods
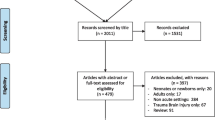
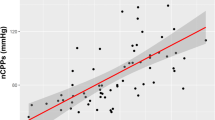
The prospective trial was performed between March 2017 and March 2019 Addenbrooke’s Hospital, Cambridge, UK. Forty adult patients who failed to awake appropriately after resuscitation from cardiac arrest or were in coma due to conditions such as meningitis, seizures, sepsis, metabolic encephalopathies, overdose, multiorgan failure or transplant were eligible for inclusion. Gathered data included admission diagnosis, duration of ventilation, length of stay in the ICU, length of stay in hospital, discharge status using Cerebral Performance Categories (CPC). All patients received intermittent extended TCD monitoring following inclusion in the study. Parameters of interest included TCD-based indices of cerebral autoregulation, non-invasive intracranial pressure, autonomic system parameters (based on heart rate variability), critical closing pressure, the cerebrovascular time constant and indices describing the shape of the TCD pulse waveform.
Results
Thirty-seven patients were included in the final analysis, with 21 patients classified as good outcome (CPC 1-2) and 16 as poor neurological outcomes (CPC 3-5). Three patients were excluded due to inadequacies identified in the TCD acquisition. The results indicated that irrespective of the primary diagnosis, non-survivors had significantly disturbed cerebral autoregulation, a shorter cerebrovascular time constant and a more distorted TCD pulse waveform (all p<0.05).
Conclusions
Preliminary results from the trial indicate that multi-parameter TCD neuromonitoring increases outcome-predictive power and TCD-based indices can be applied to general intensive care monitoring.

Similar content being viewed by others
References
Gofton TE, Young GB. Sepsis-associated encephalopathy. Nat Rev Neurol. 2012;8:557–66.
Hoesch RE, Koenig MA, Geocadin RG. Coma after global ischemic brain injury: pathophysiology and emerging therapies. Crit Care Clin. 2008;24:25–44. vii-viii.
Khot S, Tirschwell DL. Long-term neurological complications after hypoxic-ischemic encephalopathy. Semin Neurol. 2006;26:422–31.
Sandroni C, Geocadin RG. Neurological prognostication after cardiac arrest. Curr Opin Crit Care. 2015;21:209–14.
Aaslid R, Lindegaard KF, Sorteberg W, Nornes H. Cerebral autoregulation dynamics in humans. Stroke. 1989;20:45–52.
Aaslid R, Markwalder TM, Nornes H. Noninvasive transcranial Doppler ultrasound recording of flow velocity in basal cerebral arteries. J Neurosurg. 1982;57:769–74.
Cardim D, Griesdale DE, Ainslie PN, Robba C, Calviello L, Czosnyka M, et al. A comparison of non-invasive versus invasive measures of intracranial pressure in hypoxic ischaemic brain injury after cardiac arrest. Resuscitation. 2019;137:221–8.
Abecasis F, Cardim D, Czosnyka M, Robba C, Agrawal S. Transcranial Doppler as a non-invasive method to estimate cerebral perfusion pressure in children with severe traumatic brain injury. Childs Nerv Syst. 2020;36:125–31.
Cardim D, Smielewski P, Czosnyka M. Spectral Cerebral Blood Volume Accounting for Noninvasive Estimation of Changes in Cerebral Perfusion Pressure in Patients with Traumatic Brain Injury. Acta Neurochir Suppl. 2021;131:193–9.
Czosnyka M, Matta BF, Smielewski P, Kirkpatrick PJ, Pickard JD. Cerebral perfusion pressure in head-injured patients: a noninvasive assessment using transcranial Doppler ultrasonography. J Neurosurg. 1998;88:802–8.
Cardim D, Robba C, Bohdanowicz M, Donnelly J, Cabella B, Liu X, et al. Non-invasive Monitoring of Intracranial Pressure Using Transcranial Doppler Ultrasonography: Is It Possible? Neurocrit Care. 2016;25:473–91.
Robba C, Goffi A, Geeraerts T, Cardim D, Via G, Czosnyka M, et al. Brain ultrasonography: methodology, basic and advanced principles and clinical applications. A narrative review. Intensive Care Med. 2019;45:913–27.
Cardim D, Robba C, Matta B, Tytherleigh-Strong G, Kang N, Schmidt B, et al. Cerebrovascular assessment of patients undergoing shoulder surgery in beach chair position using a multiparameter transcranial Doppler approach. J Clin Monit Comput. 2019;33:615–25.
Cardim D, Robba C, Schmidt E, Schmidt B, Donnelly J, Klinck J, et al. Transcranial Doppler Non-invasive Assessment of Intracranial Pressure, Autoregulation of Cerebral Blood Flow and Critical Closing Pressure during Orthotopic Liver Transplant. Ultrasound Med Biol. 2019;45:1435–45.
Westhall E, Rossetti AO, van Rootselaar AF, Wesenberg Kjaer T, Horn J, Ullén S, et al. Standardized EEG interpretation accurately predicts prognosis after cardiac arrest. Neurology. 2016;86:1482–90.
Nasr N, Gaio R, Czosnyka M, Budohoski K, Liu X, Donnelly J, et al. Baroreflex Impairment After Subarachnoid Hemorrhage Is Associated With Unfavorable Outcome. Stroke. 2018;49:1632–8.
Tymko MM, Donnelly J, Smielewski P, Zeiler FA, Sykora M, Haubrich C, et al. Changes in cardiac autonomic activity during intracranial pressure plateau waves in patients with traumatic brain injury. Clin Auton Res. 2019;29:123–6.
Schmidt B, Czosnyka M, Raabe A, Yahya H, Schwarze JJ, Sackerer D, et al. Adaptive noninvasive assessment of intracranial pressure and cerebral autoregulation. Stroke. 2003;34:84–9.
Zeiler FA, Cardim D, Donnelly J, Menon DK, Czosnyka M, Smielewski P. Transcranial Doppler Systolic Flow Index and ICP-Derived Cerebrovascular Reactivity Indices in Traumatic Brain Injury. J Neurotrauma. 2018;35:314–22.
Cecil S, Chen PM, Callaway SE, Rowland SM, Adler DE, Chen JW. Traumatic brain injury: advanced multimodal neuromonitoring from theory to clinical practice. Crit Care Nurse. 2011;31:25–36. quiz 7.
Sorrentino E, Budohoski KP, Kasprowicz M, Smielewski P, Matta B, Pickard JD, et al. Critical thresholds for transcranial Doppler indices of cerebral autoregulation in traumatic brain injury. Neurocrit Care. 2011;14:188–93.
Liu X, Czosnyka M, Donnelly J, Budohoski KP, Varsos GV, Nasr N, et al. Comparison of frequency and time domain methods of assessment of cerebral autoregulation in traumatic brain injury. J Cereb Blood Flow Metab. 2015;35:248–56.
Czosnyka M, Richards HK, Whitehouse HE, Pickard JD. Relationship between transcranial Doppler-determined pulsatility index and cerebrovascular resistance: an experimental study. J Neurosurg. 1996;84:79–84.
Aries MJ, Czosnyka M, Budohoski KP, Steiner LA, Lavinio A, Kolias AG, et al. Continuous determination of optimal cerebral perfusion pressure in traumatic brain injury. Crit Care Med. 2012;40:2456–63.
Tas J, Beqiri E, van Kaam RC, Czosnyka M, Donnelly J, Haeren RH, et al. Targeting Autoregulation-Guided Cerebral Perfusion Pressure after Traumatic Brain Injury (COGiTATE): A Feasibility Randomized Controlled Clinical Trial. J Neurotrauma. 2021;38:2790–800.
Aries MJ, Wesselink R, Elting JW, Donnelly J, Czosnyka M, Ercole A, et al. Enhanced Visualization of Optimal Cerebral Perfusion Pressure Over Time to Support Clinical Decision Making. Crit Care Med. 2016;44:e996-9.
Güiza F, Meyfroidt G, Piper I, Citerio G, Chambers I, Enblad P, et al. Cerebral Perfusion Pressure Insults and Associations with Outcome in Adult Traumatic Brain Injury. J Neurotrauma. 2017;34:2425–31.
Donnelly J, Czosnyka M, Adams H, Robba C, Steiner LA, Cardim D, et al. Individualizing Thresholds of Cerebral Perfusion Pressure Using Estimated Limits of Autoregulation. Crit Care Med. 2017;45:1464–71.
Sekhon MS, Gooderham P, Menon DK, Brasher PMA, Foster D, Cardim D, et al. The Burden of Brain Hypoxia and Optimal Mean Arterial Pressure in Patients With Hypoxic Ischemic Brain Injury After Cardiac Arrest. Crit Care Med. 2019;47:960–9.
Zeiler FA, Smielewski P. Application of robotic transcranial Doppler for extended duration recording in moderate/severe traumatic brain injury: first experiences. Crit Ultrasound J. 2018;10:16.
Zeiler FA, Czosnyka M, Smielewski P. Optimal cerebral perfusion pressure via transcranial Doppler in TBI: application of robotic technology. Acta Neurochir (Wien). 2018;160:2149–57.
Acknowledgements
This study was sponsored by the Cambridge University Hospitals NHS Foundation Trust R&D and led by MSD (IRAS Project ID: 165207).
Funding
This work was supported by Cambridge Commonwealth, European & International Trust Scholarship (University of Cambridge) in the form of Scholarship funding for DC, and NIHR Brain Injury Healthcare Technology Co-operative, Cambridge, UK in the form of equipment funding for DC, LC, and MC. The sponsors had no role in the design or conduct of this manuscript.
Author information
Authors and Affiliations
Contributions
LC, DC, MC, MSD designed and led the study, performed the statistical analysis, and drafted the first version of the manuscript. All the authors participated in data interpretation, collection, and editing of the first version of the manuscript. All authors approved the final version of the manuscript and authorship requirements have been met.
Corresponding author
Ethics declarations
Conflict of interest
MC and PS share financial interest in a portion of ICM+ software licensing fees. The remaining authors disclose no conflicts of interest.
Ethics approval
This manuscript complies with all instructions to authors and adhere to ethical guidelines and indicate ethical approvals (IRB) and use of informed consent. The experimental protocol and informed consent were approved by the institutional review board at Addenbrooke’s Hospital, Cambridge University Hospitals Foundation Trust (“Non-invasive multimodal brain monitoring in Clinical Neuroscience”, IRAS ID 165207, REC (IRB) reference 16/LO/1971).
Consent to participate
Informed consent was obtained for all individual participants included in the study. As patients were unable to provide informed consent themselves at the point of inclusion, they were included either by a process of deferred assent by next of kin or of inclusion by professional assent through treating physicians, who were not involved in the trial.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Calviello, L.A., Cardim, D., Czosnyka, M. et al. Feasibility of non-invasive neuromonitoring in general intensive care patients using a multi-parameter transcranial Doppler approach. J Clin Monit Comput 36, 1805–1815 (2022). https://doi.org/10.1007/s10877-022-00829-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-022-00829-x