Abstract
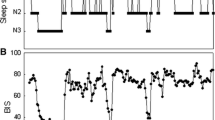
The assessment and management of sleep are increasingly recommended in the clinical practice. Polysomnography (PSG) is considered the gold standard test to monitor sleep objectively, but some practical and technical constraints exist due to environmental and patient considerations. Bispectral index (BIS) monitoring is commonly used in clinical practice for guiding anesthetic administration and provides an index based on relationships between EEG components. Due to similarities in EEG synchronization between anesthesia and sleep, several studies have assessed BIS as a sleep monitor with contradictory results. The aim of this study was to evaluate objectively both the feasibility and reliability of BIS for sleep monitoring through a robust methodology, which included full PSG recordings at a baseline situation and after 40 h of sleep deprivation. Results confirmed that the BIS index was highly correlated with the hypnogram (0.89 ± 0.02), showing a progressive decrease as sleep deepened, and an increase during REM sleep (awake: 91.77 ± 8.42; stage N1: 83.95 ± 11.05; stage N2: 71.71 ± 11.99; stage N3: 42.41 ± 9.14; REM: 80.11 ± 8.73). Mean and median BIS values were lower in the post-deprivation night than in the baseline night, showing statistical differences for the slow wave sleep (baseline: 42.41 ± 9.14 vs. post-deprivation: 39.49 ± 10.27; p = 0.02). BIS scores were able to discriminate properly between deep (N3) and light (N1, N2) sleep. BIS values during REM overlapped those of other sleep stages, although EMG activity provided by the BIS monitor could help to identify REM sleep if needed. In conclusion, BIS monitors could provide a useful measure of sleep depth in especially particular situations such as intensive care units, and they could be used as an alternative for sleep monitoring in order to reduce PSG-derived costs and to increase capacity in ambulatory care.





Similar content being viewed by others
References
Friese RS, Diaz-Arrastia R, McBride D, Frankel H, Gentilello LM. Quantity and quality of sleep in the surgical intensive care unit: are our patients sleeping? J Trauma. 2007;63:1210–4.
Weinhouse GL, Schwab RJ. Sleep in the critically ill patient. Sleep. 2006;29:707–16.
Bourne RS, Minelli C, Mills GH, Kandler R. Clinical review: sleep measurement in critical care patients: research and clinical implications. Crit Care. 2007;11:226.
Gujar N, Yoo S-S, Hu P, Walker MP. Sleep deprivation amplifies reactivity of brain reward networks, biasing the appraisal of positive emotional experiences. J Neurosci. 2011;31:4466–74.
Vogel GW, Thurmond A, Gibbons P, Sloan K, Walker M. REM sleep reduction effects on depression syndromes. Arch Gen Psychiatry. 1975;32:765–77.
Rampil IJ. A primer for EEG signal processing in anesthesia. Anesthesiology. 1998;89:980–1002.
Nieuwenhuijs D, Coleman EL, Douglas NJ, Drummond GB, Dahan A. Bispectral index values and spectral edge frequency at different stages of physiologic sleep. Anesth Analg. 2002;94:125–9.
Sleigh JW, Andrzejowski J, Steyn-Ross A, Steyn-Ross M. The bispectral index: a measure of depth of sleep? Anesth Analg. 1999;88:659–61.
Iber C, Ancoli-Israel SS, Chesson ALAL, Quan SF. The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. 1st ed. Westchester, IL: American Academy of Sleep Medicine; 2007.
Burioka N, Miyata M, Cornélissen G, Halberg F, Takeshima T, Kaplan DT, et al. Approximate entropy in the electroencephalogram during wake and sleep. Clin EEG Neurosci. 2005;36:21–4.
Kirsch MR, Monahan K, Weng J, Redline S, Loparo KA. Entropy-based measures for quantifying sleep-stage transition dynamics: relationship to sleep fragmentation and daytime sleepiness. IEEE Trans Biomed Eng. 2012;59:787–96.
Brown EN, Lydic R, Schiff ND. General anesthesia, sleep, and coma. N Engl J Med. 2010;363:2638–50.
Tung A, Mendelson WB. Anesthesia and sleep. Sleep Med Rev. 2004;8:213–25.
Borbély AA. A two process model of sleep regulation. Hum Neurobiol. 1982;1:195–204.
Borbély AA, Baumann F, Brandeis D, Strauch I, Lehmann D. Sleep deprivation: effect on sleep stages and EEG power density in man. Electroencephalogr Clin Neurophysiol. 1981;51:483–95.
Carskadon MA, Dement WC. Chapter 2—normal human sleep: an overview. In: Dement MHKRC, editor. Principles and practice of sleep medicine. 5th ed. Philadelphia: W.B. Saunders; 2011. p. 16–26.
Dahaba AA, Xue JX, Xu GX, Liu QH, Metzler H. Bilateral bispectral index (BIS)-Vista as a measure of physiologic sleep in sleep-deprived anesthesiologists. Minerva Anestesiol. 2011;77:388–93.
Álvarez-Estévez D, Fernández-Pastoriza JM, Hernández-Pereira E, Moret-Bonillo V. A method for the automatic analysis of the sleep macrostructure in continuum. Expert Syst Appl. 2013;40:1796–803.
Schulz H. Rethinking sleep analysis. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med. 2008;4:99–103.
Tung A, Lynch JP, Roizen MF. Use of the BIS monitor to detect onset of naturally occurring sleep. J Clin Monit Comput. 2002;17:37–42.
Noirhomme Q, Boly M, Bonhomme V, Boveroux P, Phillips C, Peigneux P, et al. Bispectral index correlates with regional cerebral blood flow during sleep in distinct cortical and subcortical structures in humans. Arch Ital Biol. 2009;147:51–7.
Maquet P, Degueldre C, Delfiore G, Aerts J, Péters J-M, Luxen A, et al. Functional neuroanatomy of human slow wave sleep. J Neurosci. 1997;17:2807–12.
Nofzinger EA, Buysse DJ, Miewald JM, Meltzer CC, Price JC, Sembrat RC, et al. Human regional cerebral glucose metabolism during non-rapid eye movement sleep in relation to waking. Brain J Neurol. 2002;125:1105–15.
Schuller PJ, Newell S, Strickland PA, Barry JJ. Response of bispectral index to neuromuscular block in awake volunteers. Br J Anaesth. 2015;115:95–103.
Acknowledgments
The authors thank the staff at the Centre d’Investigació de Medicaments de l’Institut de Recerca de l’Hospital de la Santa Creu i Sant Pau for their technical assistance during data collection. The present research complies with the Spanish Law.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
This study was supported in part by the Ministerio de Economía y Competividad, under contract DPI2011-22680 and DPI2014-59049R. CIBER-BBN and CIBERSAM are an initiative of the Instituto de Salud Carlos III, Spain. The authors declare that there is no conflict of interest arising from this study.
Additional information
Sandra Giménez and Sergio Romero have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Giménez, S., Romero, S., Alonso, J.F. et al. Monitoring sleep depth: analysis of bispectral index (BIS) based on polysomnographic recordings and sleep deprivation. J Clin Monit Comput 31, 103–110 (2017). https://doi.org/10.1007/s10877-015-9805-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-015-9805-5