Abstract
Purpose
To assess the effects of oocyte central granularity and its underlying endocrine environment on developmental competence of dysmorphic and morphologically normal oocytes.
Methods
Retrospective cohort study including 1,082 patients undergoing autologous ICSI cycles. Of these, 211 patients provided 602 oocytes with central granularity (CG) and 427 morphologically normal cycle companion oocytes (NCG). The remaining 871 patients provided only morphologically normal oocytes in cycles not yielding dysmorphic oocytes (N). Patient profile associated with CG was characterized, and fertilization rates, early morphokinetics and live birth rates were compared between N, CG and NCG groups. Patient characteristics associated with implantation and delivery performance of CG-derived embryos were assessed.
Results
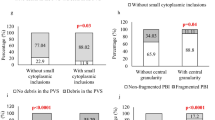
CG was associated with higher maternal age, basal FSH concentrations and total FSH dose, but with lower circulating AMH (p ≤ 0.035). Fertilization rates were reduced and early morphokinetic parameters were delayed in CG (p < 0.025) and NCG (p < 0.05) groups as compared to the N group. Embryos derived from CG oocytes achieved a markedly lower live birth rate (14.9%) as compared to those derived from NCG (36.8%; p = 0.03) and N oocytes (29.8%; p = 0.002). The negative relationship between CG and live birth was confirmed by a multivariate analysis controlling for potential confounders (OR:2.59, IC:1.27–5.31; P = 0.009). Implantation and delivery rates following transfers of CG-derived embryos were inversely associated with maternal age.
Conclusion
CG oocytes, but not their morphologically normal cycle companions, have severely compromised developmental competence. Maternal age should be a key parameter in deciding whether or not to utilize CG oocytes in ICSI cycles.


Similar content being viewed by others
Data Availability
The anonymized database assessed in the present study is available upon request
References
Balaban B, Urman B, Sertac A, Alatas C, Aksoy S, Mercan R. Oocyte morphology does not affect fertilization rate, embryo quality and implantation rate after intracytoplasmic sperm injection. Hum Reprod. 1998;13:3431–3. https://doi.org/10.1093/humrep/13.12.3431.
Ebner T, Moser M, Tews G. Is oocyte morphology prognostic of embryo developmental potential after ICSI? Reprod Biomed Online. 2006;12:507–12. https://doi.org/10.1016/S1472-6483(10)62006-8.
Rienzi L, Vajta G, Ubaldi F. Predictive value of oocyte morphology in human IVF: a systematic review of the literature. Hum Reprod Update. 2010;17:34–45. https://doi.org/10.1093/humupd/dmq029.
Braga DP, Setti AS, Figueira Rde C, Machado RB, Iaconelli A Jr, Borges E Jr. Influence of oocyte dysmorphisms on blastocyst formation and quality. Fertil Steril. 2013;100:748–54. https://doi.org/10.1016/j.fertnstert.2013.05.021.
Rienzi L, Balaban B, Ebner T, Mandelbaum J. The oocyte. Hum Reprod. 2012;27(Suppl 1):i2-21. https://doi.org/10.1093/humrep/des200.
Dal Canto M, Guglielmo MC, Mignini Renzini M, Fadini R, Moutier C, Merola M, De Ponti E, Coticchio G. Dysmorphic patterns are associated with cytoskeletal alterations in human oocytes. Hum Reprod. 2017;32:750–7. https://doi.org/10.1093/humrep/dex041.
Hu J, Molinari E, Darmon S, Zhang L, Patrizio P, Barad DH, Gleicher N. Predictive value of cytoplasmic granulation patterns during in vitro fertilization in metaphase II oocytes: Part I, poor-prognosis patients. Fertil Steril. 2021;116:431–43. https://doi.org/10.1016/j.fertnstert.2021.02.022.
Hu J, Molinari E, Darmon SK, Zhang L, Patrizio P, Barad DH, Gleicher N. Predictive value of cytoplasmic granulation patterns during in vitro fertilization in metaphase II oocytes: part II, donor oocyte cycles. Fertil Steril. 2021;116:1330–40. https://doi.org/10.1016/j.fertnstert.2021.06.026.
Serhal PF, Ranieri DM, Kinis A, Marchant S, Davies M, Khadum IM. Oocyte morphology predicts outcome of intracytoplasmic sperm injection. Hum Reprod. 1997;12:1267–70. https://doi.org/10.1093/humrep/12.6.1267.
Kahraman S, Yakın K, Dönmez E, Samlı H, Bahce M, Cengiz G, Sertyel S, Samlı M, İmirzalıoğlu N. Relationship between granular cytoplasm of oocytes and pregnancy outcome following intracytoplasmic sperm injection. Hum Reprod. 2000;15:2390–3. https://doi.org/10.1093/humrep/15.11.2390.
Rienzi L, Ubaldi FM, Iacobelli M, Minasi MG, Romano S, Ferrero S, Sapienza F, Baroni E, Litwicka K, Greco E. Significance of metaphase II human oocyte morphology on ICSI outcome. Fertil Steril. 2008;90:1692–700. https://doi.org/10.1016/j.fertnstert.2007.09.024.
Lemmen JG, Agerholm I, Ziebe S. Kinetic markers of human embryo quality using time-lapse recordings of IVF/ICSI-fertilized oocytes. Reprod Biomed Online. 2008;17:385–91. https://doi.org/10.1016/S1472-6483(10)60222-2.
Armstrong S, Bhide P, Jordan V, Pacey A, Marjoribanks J, Farquhar C. Time-lapse systems for embryo incubation and assessment in assisted reproduction. Cochrane Database Syst Rev. 2019;5:1–69. https://doi.org/10.1002/14651858.CD011320.pub4.
Bartolacci A, Buratini J, Moutier C, Guglielmo MC, Novara PV, Brambillasca F, Renzini MM, Dal Canto M. Maternal body mass index affects embryo morphokinetics: a time-lapse study. J Assist Reprod Genet. 2019;36:1109–16. https://doi.org/10.1007/s10815-019-01456-3.
Del Gallego R, Remohi J, Meseguer M. Time-lapse imaging: the state of the artdagger. Biol Reprod. 2019;101:1146–54. https://doi.org/10.1093/biolre/ioz035.
Dal Canto M, Bartolacci A, Turchi D, Pignataro D, Lain M, De Ponti E, Brigante C, Mignini Renzini M, Buratini J. Faster fertilization and cleavage kinetics reflect competence to achieve a live birth after intracytoplasmic sperm injection, but this association fades with maternal age. Fertil Steril. 2020. https://doi.org/10.1016/j.fertnstert.2020.06.023.
Siristatidis C, Komitopoulou MA, Makris A, Sialakouma A, Botzaki M, Mastorakos G, Salamalekis G, Bettocchi S, Palmer GA. Morphokinetic parameters of early embryo development via time lapse monitoring and their effect on embryo selection and ICSI outcomes: a prospective cohort study. J Assist Reprod Genet. 2015;32:563–70. https://doi.org/10.1007/s10815-015-0436-z.
Fishel S, Campbell A, Montgomery S, Smith R, Nice L, Duffy S, Jenner L, Berrisford K, Kellam L, Smith R. Time-lapse imaging algorithms rank human preimplantation embryos according to the probability of live birth. Reprod Biomed Online. 2018;37:304–13. https://doi.org/10.1016/j.rbmo.2018.05.016.
Bartolacci A, Dal Canto M, Guglielmo MC, Mura L, Brigante C, Renzini MM, Buratini J. Early embryo morphokinetics is a better predictor of post-ICSI live birth than embryo morphology: speed is more important than beauty at the cleavage stage. Zygote. 2021;29:495–502. https://doi.org/10.1017/S0967199421000253.
ALPHA Scientists In Reproductive Medicine, ESHRE Special Interest Group Embryology. Istanbul consensus workshop on embryo assessment: proceedings of an expert meeting. Reprod Biomed Online. 2011;22:632–46. https://doi.org/10.1016/j.rbmo.2011.02.001.
Practice Committee of American Society for Reproductive Medicine, Practice Committee of Society for Assisted Reproductive Technology. Criteria for number of embryos to transfer: a committee opinion. Fertil Steril. 2013;99:44–6. https://doi.org/10.1016/j.fertnstert.2012.09.038.
Buratini J, Dal Canto M, De Ponti E, Brambillasca F, Brigante C, Gippone S, Mignini Renzini M, La Marca A. Maternal age affects the relationship of basal FSH and anti-Mullerian hormone concentrations with post-ICSI/IVF live birth. Reprod Biomed Online. 2021. https://doi.org/10.1016/j.rbmo.2020.12.005.
Buratini J, Dellaqua TT, Dal Canto M, La Marca A, Carone D, Mignini Renzini M, Webb R. The putative roles of FSH and AMH in the regulation of oocyte developmental competence: from fertility prognosis to mechanisms underlying age-related subfertility. Hum Reprod Update. 2021;28:232–54. https://doi.org/10.1093/humupd/dmab044.
Lin Y, Yang P, Chen Y, Zhu J, Zhang X, Ma C. Factors inducing decreased oocyte maturation rate: a retrospective analysis of 20,939 ICSI cycles. Arch Gynecol Obstet. 2019;299:559–64. https://doi.org/10.1007/s00404-018-4958-3.
Pellatt L, Rice S, Dilaver N, Heshri A, Galea R, Brincat M, Brown K, Simpson ER, Mason HD. Anti-Mullerian hormone reduces follicle sensitivity to follicle-stimulating hormone in human granulosa cells. Fertil Steril. 2011;96:1246–51. https://doi.org/10.1016/j.fertnstert.2011.08.015.
Chang HM, Klausen C, Leung PC. Antimullerian hormone inhibits follicle-stimulating hormone-induced adenylyl cyclase activation, aromatase expression, and estradiol production in human granulosa-lutein cells. Fertil Steril. 2013;100:585–92. https://doi.org/10.1016/j.fertnstert.2013.04.019.
Ciepiela P, Duleba AJ, Kario A, Chelstowski K, Branecka-Wozniak D, Kurzawa R. Oocyte matched follicular fluid anti-Mullerian hormone is an excellent predictor of live birth after fresh single embryo transfer. Hum Reprod. 2019;34:2244–53. https://doi.org/10.1093/humrep/dez186.
Ebner T, Moser M, Shebl O, Sommerguber M, Tews G. Prognosis of oocytes showing aggregation of smooth endoplasmic reticulum. Reprod Biomed Online. 2008;16:113–8. https://doi.org/10.1016/S1472-6483(10)60563-9.
Combelles CM, Carabatsos MJ, Kumar TR, Matzuk MM, Albertini DF. Hormonal control of somatic cell oocyte interactions during ovarian follicle development. Mol Reprod Dev. 2004;69:347–55. https://doi.org/10.1002/mrd.20128.
Macaulay AD, Gilbert I, Scantland S, Fournier E, Ashkar F, Bastien A, Saadi HA, Gagne D, Sirard MA, Khandjian EW, et al. Cumulus cell transcripts transit to the bovine oocyte in preparation for maturation. Biol Reprod. 2016;94:16. https://doi.org/10.1095/biolreprod.114.127571.
Macaulay AD, Gilbert I, Caballero J, Barreto R, Fournier E, Tossou P, Sirard MA, Clarke HJ, Khandjian EW, Richard FJ, et al. The gametic synapse: RNA transfer to the bovine oocyte. Biol Reprod. 2014;91:90. https://doi.org/10.1095/biolreprod.114.119867.
Alviggi C, Andersen CY, Buehler K, Conforti A, De Placido G, Esteves SC, Fischer R, Galliano D, Polyzos NP, Sunkara SK, et al. A new more detailed stratification of low responders to ovarian stimulation: from a poor ovarian response to a low prognosis concept. Fertil Steril. 2016;105:1452–3. https://doi.org/10.1016/j.fertnstert.2016.02.005.
Acknowledgements
The authors thank Thaisy T. Dellaqua and Matilde Fantacci for assistance during manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Buratini, J., Moutier, C., Guglielmo, M.C. et al. The impact of oocyte central granularity on ICSI practice: developmental competence of dysmorphic and morphologically normal companion oocytes. J Assist Reprod Genet 40, 2375–2384 (2023). https://doi.org/10.1007/s10815-023-02895-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-023-02895-9