Abstract
Purpose
To report our experience on homologous intrauterine insemination (IUI) with gonadotropin controlled ovarian stimulation (COS) cycles and to examine different variables which could predict IUI success.
Materials and methods
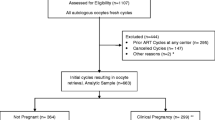
This is a retrospective analysis of IUIs performed between January 1997 and December 2017. A total of 7359 COS IUI’s procedures (2901 couples) were reviewed. Clinical pregnancy, live birth rate and age, body mass index (BMI), smoking habit, duration of infertility, sperm characteristics before and after treatment (total motile count, morphology, and vitality), day 3 FSH, total gonadotropin dose, and number of follicles were assessed by multivariate logistic regression analysis, and data were expressed as odds ratio (OR).
Results
The mean female age at the time of COS was 35.10 ± 3.93 years. The most common single infertility diagnoses were unexplained infertility (53.55%), mild male factor (19.69%), and anovulation (10.95%). The total progressive motile sperm count (TPMC) was > 1 × 106/ml (mean 1.34 ± 1.08 × 106/ml). The clinical pregnancy rate was 9.38%, and the live birth rate was 7.19% per cycle. Twin pregnancies were 12.17%. Cumulative pregnancy was 21.89% and cumulative live birth rate was 17.58% per couple. Clinical pregnancy and live birth rates were significantly associated with female age [OR 0.97 (95% CI 0.95–0.99) and 0.95 (95% CI 0.93–0.97), respectively] and day 3 FSH [OR 0.91 (95% CI 0.87–0.94) e 0.90 (95% CI 0.87–0.94), respectively].
Conclusions
Clinical pregnancy rate and live birth rates after COS-IUIs were significantly influenced by female age and FSH levels.
Trial registration
Clinical trial registration number: NCT03836118


Similar content being viewed by others
Data availability
The datasets generated for this study are available on request to the corresponding author.
References
Templeton A. Infertility-epidemiology, aetiology and effective management. Health Bull (Edinb). 1995;53:294–8.
World Health Organization (WHO). Infertility is a Global Public Health Issue. In: Sexual and Reproductive Health; 2014.
Ombelet W. The revival of intrauterine insemination: evidence-based data have changed the picture. Facts Views Vis Obgyn. 2017;9:131–2.
Cohlen B, Bijkerk A, Van der Poel S, Ombelet W. IUI: review and systematic assessment of the evidence that supports global recommendations. Hum Reprod Update. 2018;24:300–19.
Group ECW. Intrauterine insemination. Hum Reprod Update. 2009;15:265–77.
O'Flynn N. Assessment and treatment for people with fertility problems: NICE guideline. Br J Gen Pract. 2014;64:50–1.
Bhattacharya S, Harrild K, Mollison J, Wordsworth S, Tay C, Harrold A, et al. Clomifene citrate or unstimulated intrauterine insemination compared with expectant management for unexplained infertility: pragmatic randomised controlled trial. BMJ. 2008;337:a716.
Reindollar RH, Regan MM, Neumann PJ, Levine BS, Thornton KL, Alper MM, et al. A randomized clinical trial to evaluate optimal treatment for unexplained infertility: the fast track and standard treatment (FASTT) trial. Fertil Steril. 2010;94:888–99.
Wordsworth S, Buchanan J, Mollison J, Harrild K, Robertson L, Tay C, et al. Clomifene citrate and intrauterine insemination as first-line treatments for unexplained infertility: are they cost-effective? Hum Reprod. 2011;26:369–75.
Farquhar CM, Liu E, Armstrong S, Arroll N, Lensen S, Brown J. Intrauterine insemination with ovarian stimulation versus expectant management for unexplained infertility (TUI): a pragmatic, open-label, randomised, controlled, two-Centre trial. Lancet. 2018;391:441–50.
Nandi A, El-Toukhy T. Stimulated intrauterine insemination for unexplained subfertility. Lancet. 2018;391:404–5.
Bensdorp AJ, Tjon-Kon-Fat RI, Bossuyt PM, Koks CA, Oosterhuis GJ, Hoek A, et al. Prevention of multiple pregnancies in couples with unexplained or mild male subfertility: randomised controlled trial of in vitro fertilisation with single embryo transfer or in vitro fertilisation in modified natural cycle compared with intrauterine insemination with controlled ovarian hyperstimulation. BMJ. 2015;350:g7771.
Tjon-Kon-Fat RI, Bensdorp AJ, Bossuyt PM, Koks C, Oosterhuis GJ, Hoek A, et al. Is IVF-served two different ways-more cost-effective than IUI with controlled ovarian hyperstimulation? Hum Reprod. 2015;30:2331–9.
Luco SM, Agbo C, Behr B, Dahan MH. The evaluation of pre and post processing semen analysis parameters at the time of intrauterine insemination in couples diagnosed with male factor infertility and pregnancy rates based on stimulation agent. A retrospective cohort study. Eur J Obstet Gynecol Reprod Biol. 2014;179:159–62.
Dinelli L, Courbière B, Achard V, Jouve E, Deveze C, Gnisci A, et al. Prognosis factors of pregnancy after intrauterine insemination with the husband's sperm: conclusions of an analysis of 2,019 cycles. Fertil Steril. 2014;101:994–1000.
Zegers-Hochschild F, Adamson GD, de Mouzon J, Ishihara O, Mansour R, Nygren K, et al. International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) revised glossary of ART terminology, 2009. Fertil Steril. 2009;92:1520–4.
Zegers-Hochschild F, Adamson GD, Dyer S, Racowsky C, de Mouzon J, Sokol R, et al. The international glossary on infertility and fertility care, 2017. Fertil Steril. 2017;108:393–406.
Duran HE, Morshedi M, Kruger T, Oehninger S. Intrauterine insemination: a systematic review on determinants of success. Hum Reprod Update. 2002;8:373–84.
Istituto Superiore di Sanità (ISS). Italian assisted reproductive technology national summer report. In: Monitoring the activity and outcomes of Italian ART centers in 2016: Italian national registry of Assisted Reproductive Technologies (ART); 2016.
Campana A, Sakkas D, Stalberg A, Bianchi PG, Comte I, Pache T, et al. Intrauterine insemination: evaluation of the results according to the woman's age, sperm quality, total sperm count per insemination and life table analysis. Hum Reprod. 1996;11:732–6.
Thijssen A, Creemers A, Van der Elst W, Creemers E, Vandormael E, Dhont N, et al. Predictive value of different covariates influencing pregnancy rate following intrauterine insemination with homologous semen: a prospective cohort study. Reprod BioMed Online. 2017;34:463–72.
Wiser A, Shalom-Paz E, Reinblatt SL, Son WY, Das M, Tulandi T, et al. Ovarian stimulation and intrauterine insemination in women aged 40 years or more. Reprod BioMed Online. 2012;24:170–3.
Merviel P, Heraud MH, Grenier N, Lourdel E, Sanguinet P, Copin H. Predictive factors for pregnancy after intrauterine insemination (IUI): an analysis of 1038 cycles and a review of the literature. Fertil Steril. 2010;93:79–88.
C M, N V, M S, G SR. Day 2 follicles stimulating hormone (FSH) and estradiol (E2): could these values be used as markers to predict pregnancy outcomes in women undergoing ovulation induction (OI) therapy with intrauterine insemination (IUI) cycles? Fertil Steril. 2005;84(Suppl):S162.
Soria M, Pradillo G, García J, Ramón P, Castillo A, Jordana C, et al. Pregnancy predictors after intrauterine insemination: analysis of 3012 cycles in 1201 couples. J Reprod Infertil. 2012;13:158–66.
Collins JA, Burrows EA, Wilan AR. The prognosis for live birth among untreated infertile couples. Fertil Steril. 1995;64:22–8.
Snick HK, Snick TS, Evers JL, Collins JA. The spontaneous pregnancy prognosis in untreated subfertile couples: the Walcheren primary care study. Hum Reprod. 1997;12:1582–8.
Nuojua-Huttunen S, Tomas C, Bloigu R, Tuomivaara L, Martikainen H. Intrauterine insemination treatment in subfertility: an analysis of factors affecting outcome. Hum Reprod. 1999;14:698–703.
Goverde AJ, McDonnell J, Vermeiden JP, Schats R, Rutten FF, Schoemaker J. Intrauterine insemination or in-vitro fertilisation in idiopathic subfertility and male subfertility: a randomised trial and cost-effectiveness analysis. Lancet. 2000;355:13–8.
Merviel P, Cabry R, Lourdel E, Barbier F, Scheffler F, Mansouri N, et al. Intrauterine insemination. Rev Prat. 2014;64:87–91.
Cabry-Goubet R, Scheffler F, Belhadri-Mansouri N, Belloc S, Lourdel E, Devaux A, et al. Effect of gonadotropin types and indications on homologous intrauterine insemination success: a study from 1251 cycles and a review of the literature. Biomed Res Int. 2017;2017:3512784.
Vlahos NF, Coker L, Lawler C, Zhao Y, Bankowski B, Wallach EE. Women with ovulatory dysfunction undergoing ovarian stimulation with clomiphene citrate for intrauterine insemination may benefit from administration of human chorionic gonadotropin. Fertil Steril. 2005;83:1510–6.
van Weert JM, Repping S, Van Voorhis BJ, van der Veen F, Bossuyt PM, Mol BW. Performance of the postwash total motile sperm count as a predictor of pregnancy at the time of intrauterine insemination: a meta-analysis. Fertil Steril. 2004;82:612–20.
Mankus EB, Holden AE, Seeker PM, Kampschmidt JC, McLaughlin JE, Schenken RS, et al. Prewash total motile count is a poor predictor of live birth in intrauterine insemination cycles. Fertil Steril. 2019;111:708–13.
Pereira N. Total motile count as predictor of live birth in intrauterine insemination cycles. Fertil Steril. 2019;111:674.
Bensdorp AJ, Cohlen BJ, Heineman MJ, Vandekerckhove P. Intra-uterine insemination for male subfertility. Cochrane Database Syst Rev. 2007;(4):CD000360. https://doi.org/10.1002/14651858.CD000360.pub4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the Independent Ethical Committee of our Institution. Consent was obtained from each patient after full explanation of the purpose and nature of all procedures used.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 17 kb)
Rights and permissions
About this article
Cite this article
Immediata, V., Patrizio, P., Parisen Toldin, M.R. et al. Twenty-one year experience with intrauterine inseminations after controlled ovarian stimulation with gonadotropins: maternal age is the only prognostic factor for success. J Assist Reprod Genet 37, 1195–1201 (2020). https://doi.org/10.1007/s10815-020-01752-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-020-01752-3