Abstract
Purpose
The objective of this study is to identify the pregnancy outcomes based on day-16 β-hCG level assessed with modern assays, in fresh single embryo transfers.
Methods
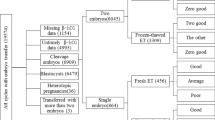
A retrospective cohort study at a single academic center between 2013 and 2017. A total of 1076 pregnancies were included.
Results
Pregnancies were divided into 10% groupings of 107–108 patients each. The 10 groups did not differ for baseline characteristics. There was no difference on outcomes based on cleavage or blastocyst transfer. At a serum β-hCG level of 103 ± 13 (range 74–135), 50% had a biochemical loss. Biochemical pregnancy losses remained 21% at serum β-hCG range (136–197). It was only once serum β-hCG level reached 199–252 that the probability of a biochemical pregnancy loss was 12%. Interestingly, if a clinical pregnancy is present even at low day-16 serum β-hCG levels, the likelihood of live birth is approximately 50%. This maximizes to 75% when the serum β-hCG level was at least 253 IU/L. The relationship between serum day-16 β-hCG levels and clinical pregnancy or live birth is quite strong with correlation coefficients above 0.8 which accounted for more than 75% of the variability in outcomes in both cases. Receiver operator curves determined that the cut-off for a clinical pregnancy was 190 and for live birth, it was 213 IU/L.
Conclusion
An increase in the serum β-hCG levels at which to expect a reassuring outcome is required based on modern assays, as compared with the old cut-off levels.



Similar content being viewed by others
References
Elliott MM, Kardana A, Lustbader JW, Cole LA. Carbohydrate and peptide structure of the alpha- and beta-subunits of human chorionic gonadotropin from normal and aberrant pregnancy and choriocarcinoma. Endocrine. 1997;7(1):15–32.
Fournier T, Guibourdenche J, Evain-Brion D. Review: hCGs: different sources of production, different glycoforms and functions. Placenta. 2015;36(Suppl 1):S60–5.
Fournier T. Human chorionic gonadotropin: different glycoforms and biological activity depending on its source of production. Ann Endocrinol (Paris). 2016;77(2):75–81.
Christodoulou CN, Zonas C, Loukaides T, Maniatis A, Giannikos L, Giannakopoulos C, et al. Low beta-hCG is associated with poor prognosis in association with an embryo with positive cardiac activity. Ultrasound Obstet Gynecol. 1995;5(4):267–70.
Morse CB, Barnhart KT, Senapati S, Sammel MD, Prochaska EC, Dokras A, et al. Association of the very early rise of human chorionic gonadotropin with adverse outcomes in singleton pregnancies after in vitro fertilization. Fertil Steril. 2016;105(5):1208–1214.e3.
Liu Y, Liu Y, Li X, Jiao X, Zhang R, Zhang J. Predictive value of serum beta-hCG for early pregnancy outcomes among women with recurrent spontaneous abortion. Int J Gynaecol Obstet. 2016;135(1):16–21.
Zeadna A, Son WY, Moon JH, Dahan MH. A comparison of biochemical pregnancy rates between women who underwent IVF and fertile controls who conceived spontaneously. Hum Reprod. 2015;30(4):783–8.
Lawler CC, Budrys NM, Rodgers AK, Holden A, Brzyski RG, Schenken RS. Serum beta human chorionic gonadotropin levels can inform outcome counseling after in vitro fertilization. Fertil Steril. 2011;96(2):505–7.
Naredi N, Singh SK, Sharma R. Does first serum beta-human chorionic gonadotropin value prognosticate the early pregnancy outcome in an in-vitro fertilisation cycle? J Hum Reprod Sci. 2017;10(2):108–13.
Kowalik A, Palermo GD, Barmat L, Veeck L, Rimarachin J, Rosenwaks Z. Comparison of clinical outcome after cryopreservation of embryos obtained from intracytoplasmic sperm injection and in-vitro fertilization. Hum Reprod. 1998;13(1o):2848–51.
Facchinetti F, Volpe A, Matteo ML, Genazzani AR, Artini GP. An increased vulnerability to stress is associated with a poor outcome of in vitro fertilization-embryo transfer treatment. Fertil Steril. 1997;67(2):309–14.
Wilcox AJ, Weinberg CR, O'Connor JF, Baird DD, Schlatterer JP, Canfield RE, et al. Incidence of early loss of pregnancy. N Engl J Med. 1988;319(4):189–94.
Sher G. IVF Authority 2010(March 24):Online.
Schreiber CA, Sammel M, Hillier SL, Barnhart KT. A little bit pregnant: modeling how the accurate detection of pregnancy can improve HIV prevention trials. Am J Epidemiol. 2009;169(4):515–21.
De Neubourg D, et al. Single top quality embryo transfer as a model for prediction of early pregnancy outcome. Hum Reprod. 2004;19(6):1476–9.
Liu L, Tong X, Jiang L, Li T, Zhou F, Zhang S. A comparison of implantation, miscarriage and pregnancy rates of single and double day 3 embryo transfer between fresh and frozen thawed transfer cycles: a retrospective study. Chin Med J. 2014;127(5):911–5.
Kathiresan ASQ, Cruz-Almeida Y, Barrionuevo MJ, Maxson WS, Hoffman DI, Weitzman VN, et al. Prognostic value of beta-human chorionic gonadotropin is dependent on day of embryo transfer during in vitro fertilization. Fertil Steril. 2011;96(6):1362–6.
Shamonki MI, Frattarelli JL, Bergh PA, Scott RT. Logarithmic curves depicting initial level and rise of serum beta human chorionic gonadotropin and live delivery outcomes with in vitro fertilization: an analysis of 6021 pregnancies. Fertil Steril. 2009;91(5):1760–4.
Cole LA, DuToit S, Higgins TN. Total hCG tests. Clin Chim Acta. 2011;412(23–24):2216–22.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research Ethics Board approval of the study was obtained (no. 2019-5548).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Al Mamari, N., Al Zawawi, N., Khayat, S. et al. Revisiting serum β-hCG cut-off levels and pregnancy outcomes using single embryo transfer. J Assist Reprod Genet 36, 2307–2313 (2019). https://doi.org/10.1007/s10815-019-01583-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-019-01583-x