Abstract
Purpose
To determine the effect of phacoemulsification surgery, which is one of the types of cataract surgery by using ultrasonic power to break up the crystalline lens and clean it with vacuum, on anterior chamber flare (ACF) and choroidal vascular index (CVI).
Methods
For this cross-sectional study, patients were included if they had cataract with nucleus hardness grade 2 or 3, no systemic inflammatory disease, and not use of anti-inflammatory drugs/prostaglandins preoperatively. ACF using a laser flare meter and CVI in patients underwent uncomplicated phacoemulsification was recorded preoperatively, on the postoperative 1st day, 1st week, and 1st month.
Results
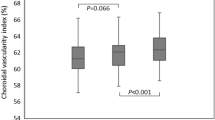
Fifty-six eyes were included. ACF was 9.00 ± 2.90 ph/ms preoperatively. Although ACF increased significantly on postoperative day-1 (39.38 ± 23.31ph/ms) and decreased gradually until the 1st month (14.03 ± 6.03ph/ms) after the operation, it was still significantly higher at the 1st month (p < 0.001). Macular and peripapillary CVI increased significantly on postoperative day-1 (0.64 ± 0.03/0.63 ± 0.05) and week-1 (0.64 ± 0.04/0.62 ± 0.04) (p = 0.01, p < 0.001); the postoperative 1st month was similar to the preoperative one (0.59 ± 0.06/0.58 ± 0.06). The relationship between the change in ACF and the change in CVI was not significant.
Conclusion
Phacoemulsification causes raises in ACF and CVI due to increased intraocular inflammation. The fact that ACF was significantly higher in postoperative month-1 and CVI returned to its preoperative value suggests that the effect of uncomplicated phacoemulsification surgery on the increase in inflammation in the anterior segment lasts longer than in the posterior segment. These results suggest that ACF and CVI follow-up may be clinically important in the follow-up of postoperative inflammation.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
Not applicable.
References
Organization, WH (2007) Global initiative for the elimination of avoidable blindness: action plan 2006–2011.
Chen H, Wu Z, Chen Y, He M, Wang J (2018) Short-term changes of choroidal vascular structures after phacoemulsification surgery. BMC Ophthalmol 18:1–7
De Maria M, Coassin M, Mastrofilippo V, Cimino L, Iannetta D, Fontana L (2020) Persistence of inflammation after uncomplicated cataract surgery: a 6-month laser flare photometry analysis. Adv Ther 37:3223–3233
Ikegami Y, Takahashi M, Amino K (2020) Evaluation of choroidal thickness, macular thickness, and aqueous flare after cataract surgery in patients with and without diabetes: a prospective randomized study. BMC Ophthalmol 20:1–7
Kahloun R, Attia S, Ksiaa I, Kacem I, Bouanene I, Zaouali S, Jelliti B, Khairallah M (2016) Anterior chamber aqueous flare, pseudoexfoliation syndrome, and glaucoma. Int Ophthalmol 36:671–674
Buyuk K, Ozkagnici A (2012) Effectiveness of topical corticosteroid on anterior chamber flare reaction after phacoemulsification surgery/Fakoemulsifikasyon cerrahisi sonrasi on kamara flare reaksiyonu uzerine topikal kortikosteroid etkinligi. Turk J Ophthalmol 42:120–125
Tugal-Tutkun I, Herbort CP (2010) Laser flare photometry: a noninvasive, objective, and quantitative method to measure intraocular inflammation. Int Ophthalmol 30:453–464
Cheong KX, Tan CS (2015) Long-term increase in subfoveal choroidal thickness after surgery for senile cataracts. Am J Ophthalmol 3:608–609
Ohsugi H, Ikuno Y, Ohara Z, Imamura H, Nakakura S, Matsuba S, Kato Y, Tabuchi H (2014) Changes in choroidal thickness after cataract surgery. J Cataract Refract Surg 40:184–191
Agrawal R, Chhablani J, Tan KA, Shah S, Sarvaiya C, Banker A (2016) Choroidal vascularity index in central serous chorioretinopathy. Retina 36:1646–1651
Yao H, Gao S, Liu X, Zhou Y, Cheng Y, Shen X (2020) Choroidal structural changes assessed with swept-source optical coherence tomography after cataract surgery in eyes with diabetic retinopathy. J Ophthalmol 2020:1–9
Yip VCH, Laude A, Tan KA, Ding J, Wong E, Agrawal R (2019) A longitudinal study of choroidal changes following cataract surgery in patients with diabetes. Diab Vasc Dis Res 16:369–377
Chylack LT, Wolfe JK, Singer DM, Leske MC, Bullimore MA, Bailey IL, Friend J, McCarthy D, Wu SY (1993) The lens opacities classification system III. Arch Ophthalmol 111:831–836
Ladas JG, Wheeler NC, Morhun PJ, Rimmer SO, Holland GN (2005) Laser flare-cell photometry: methodology and clinical applications. Surv Ophthalmol 50:27–47
De Maria M, Coassin M, Iannetta D, Fontana L (2021) Laser flare and cell photometry to measure inflammation after cataract surgery: a tool to predict the risk of cystoid macular edema. Int Ophthalmol 41:2293–2300
Abell RG, Allen PL, Vote BJ (2013) Anterior chamber flare after femtosecond laser–assisted cataract surgery. J Cataract Refract Surg 39:1321–1326
Siriwardena D, Kotecha A, Minassian D, Dart J, Khaw P (2000) Anterior chamber flare after trabeculectomy and after phacoemulsification. Br J Ophthalmol 84:1056–1057
Cakir I, Altan C, Yalcinkaya G, Ozveren M, Kabakci AK, Taskapili M (2022) Evaluation of post phacoemulsification inflammation in eyes with and without pseudoexfoliation syndrome according to phaco parameters via laser flare photometry. Photodiagn Photodyn Ther 38:102805
Schumacher S, Nguyen NX, Küchle M, Naumann GO (1999) Quantification of aqueous flare after phacoemulsification with intraocular lens implantation in eyes with pseudoexfoliation syndrome. Arch Ophthalmol 117:733–735
Liu YC, Setiawan M, Ang M, Yam GHF, Mehta JS (2019) Changes in aqueous oxidative stress, prostaglandins, and cytokines: comparisons of low-energy femtosecond laser–assisted cataract surgery versus conventional phacoemulsification. J Cataract Refract Surg 45:196–203
Karslioglu MZ, Kesim C, Yucel O, Yildiz Tas A, Torun S, Altan C, Sahin A (2021) Choroidal vascularity index in pseudoexfoliative glaucoma. Int Ophthalmol 41:4197–4208
Ozcelik Kose A, Imamoglu S, Balci S, Yenerel NM (2022) Comparison of choroidal vascularity index in patients with pseudoexfoliation glaucoma, pseudoexfoliation syndrome, and healthy controls. Curr Eye Res 47:154–160
Funding
No financial support was received.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by GYC and IC. The first draft of the manuscript was written by GYC, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Written informed consent was obtained from all individual participants who were included in the study.
Consent to publish
Patients signed informed consent regarding publishing their data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yalçınkaya Çakır, G., Altan, Ç. & Çakır, İ. Anterior chamber flare and choroidal vascular index as inflammatory markers after uncomplicated phacoemulsification surgery. Int Ophthalmol 44, 35 (2024). https://doi.org/10.1007/s10792-024-02959-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10792-024-02959-4