Abstract
Purpose
To review all case series of refractive corneal inlay implantation: Flexivue (Presbia, Netherlands), Invue (BioVision, Brügg, Switzerland) and Icolens (Neoptics, Hünenberg, Switzerland) performed in presbyopia patients and to evaluate the reported visual outcomes. In addition, our aim is to provide assessment for complications and to report the satisfaction rates.
Methods
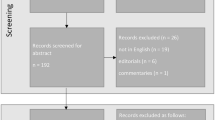
PubMed, Web of Science and Scopus databases were consulted using “refractive corneal inlay”, “Flexivue Inlay”, “Invue Inlay” and “Icolens inlay” as keywords. 147 articles were found, and they were assessed considering the inclusion and exclusion criteria. After filtering, this systemic review included ten articles, published between 2011 and 2020.
Results
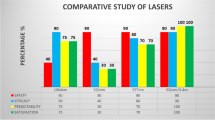
308 eyes from 308 participants were enrolled in this systematic review. Mean maximum follow-up was 13.9 months. Nine of the ten case series included used femtosecond laser for the corneal pocket creation. Mean pocket depth was 293.75 µm. 77.5% of the eyes reported a postoperative uncorrected near visual acuity of 20/32 or better, and 19.20% of the inlay-implanted eyes achieved an uncorrected distance visual acuity of 20/20 or better. The most prominent complications were halos, pain, photophobia, and poor distance visual acuity. 27 eyes (8.7%) had to be explanted due to complications, such as near-distance spectacle dependence or blurred distance vision.
Conclusion
Refractive corneal inlay outcomes demonstrated high efficacy, safety, and satisfaction rates. Furthermore, it is a reversible technique. However, the findings must be viewed with caution due potential conflict of interest. Further research with higher sample size is needed to validate these findings.

Similar content being viewed by others
Availability of data and material
Data available on demand.
References
Kim T-im, del Barrio JLA, Wilkins M et al (2019) Refractive surgery. Lancet 393:2085–2098. https://doi.org/10.1016/S0140-6736(18)33209-4
Lindstrom RL, MacRae SM, Pepose JS, Hoopes PC (2013) Corneal inlays for presbyopia correction. Curr Opin Ophthalmol 24:281–287
Alio JL, Plaza-Puche AB, Férnandez-Buenaga R et al (2017) Multifocal intraocular lenses: an overview. Surv Ophthalmol 62:611–634
Lafosse E, Wolffsohn JS, Talens-Estarelles C, García-Lázaro S (2020) Presbyopia and the aging eye: existing refractive approaches and their potential impact on dry eye signs and symptoms. Contact Lens Anterior Eye 43:103–114
Sánchez-González J-M, Alonso-Aliste F, Amián-Cordero J et al (2019) Refractive and visual outcomes of SUPRACOR TENEO 317 LASIK for presbyopia in hyperopic eyes: 24-month follow-up. J Refract Surg 35:591–598. https://doi.org/10.3928/1081597X-20190815-01
Duignan ES, Farrell S, Treacy MP et al (2016) Corneal inlay implantation complicated by infectious keratitis. Br J Ophthalmol 100:269–273. https://doi.org/10.1136/bjophthalmol-2015-306641
Bouzoukis DI, Kymionis GD, Limnopoulou AN et al (2011) Femtosecond laser-assisted corneal pocket creation using a mask for inlay implantation. J Refract Surg 27:818–820. https://doi.org/10.3928/1081597X-20110706-01
Parkhurst GD, Garza EB, Medina AA (2015) Femtosecond laser-assisted cataract surgery after implantation of a transparent near vision corneal inlay. J Refract Surg 31:206–208. https://doi.org/10.3928/1081597X-20150224-05
Burkhard Dick H (2019) Small-aperture strategies for the correction of presbyopia. Curr Opin Ophthalmol 30:236–242. https://doi.org/10.1097/ICU.0000000000000576
Limnopoulou AN, Bouzoukis DI, Kymionis GD et al (2013) Visual outcomes and safety of a refractive corneal inlay for presbyopia using femtosecond laser. J Refract Surg 29(1):12–18. https://doi.org/10.3928/1081597X-20121210-01
Bouzoukis DI, Kymionis GD, Panagopoulou SI et al (2012) Visual outcomes and safety of a small diameter intrastromal refractive inlay for the corneal compensation of presbyopia. J Refract Surg 28:168–173. https://doi.org/10.3928/1081597X-20120124-02
Baily C, Kohnen T, O’Keefe M (2014) Preloaded refractive-addition corneal inlay to compensate for presbyopia implanted using a femtosecond laser: one-year visual outcomes and safety. J Cataract Refract Surg 40:1341–1348. https://doi.org/10.1016/j.jcrs.2013.11.047
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6:e1000100. https://doi.org/10.1371/journal.pmed.1000100
Zeng X, Zhang Y, Kwong JS et al (2015) The methodological quality assessment tools for preclinical and clinical studies, systematic review and meta-analysis, and clinical practice guideline: a systematic review. J Evid Based Med 8(1):2–10
Malandrini A, Martone G, Menabuoni L et al (2015) Bifocal refractive corneal inlay implantation to improve near vision in emmetropic presbyopic patients. J Cataract Refract Surg 41:1962–1972. https://doi.org/10.1016/j.jcrs.2015.01.018
Stojanovic NR, Feingold V, Pallikaris IG (2016) Combined cataract and refractive corneal inlay implantation surgery: comparison of three techniques. J Refract Surg 32:318–325. https://doi.org/10.3928/1081597X-20160225-02
Beer SMC, Santos R, Nakano EM et al (2017) One-year clinical outcomes of a corneal inlay for presbyopia. Cornea 36:816–820. https://doi.org/10.1097/ICO.0000000000001195
Han G, Lim DH, Yang CM et al (2019) Refractive corneal inlay for presbyopia in emmetropic patients in Asia: 6-month clinical outcomes. BMC Ophthalmol 19(1):66. https://doi.org/10.1186/s12886-019-1069-2
Beer SMC, Werner L, Nakano EM et al (2020) A 3-year follow-up study of a new corneal inlay: clinical results and outcomes. Br J Ophthalmol 104:723–728. https://doi.org/10.1136/bjophthalmol-2019-314314
Naroo SA, Bilkhu PS (2016) Clinical utility of the KAMRA corneal inlay. Clin Ophthalmol 10:913–919. https://doi.org/10.2147/OPTH.S89132
Moshirfar M, Desautels JD, Wallace RT et al (2017) Comparison of FDA safety and efficacy data for KAMRA and raindrop corneal inlays. Int J Ophthalmol 10:1446–1451. https://doi.org/10.18240/ijo.2017.09.18
Ylmaz ÖF, Alagöz N, Pekel G et al (2011) Intracorneal inlay to correct presbyopia: long-term results. J Cataract Refract Surg 37:1275–1281. https://doi.org/10.1016/j.jcrs.2011.01.027
Xia LK, Yu J, Chai GR et al (2015) Comparison of the femtosecond Laser and mechanical microkeratome for flap cutting in LASIK. Int J Ophthalmol 8:784–790. https://doi.org/10.3980/j.issn.2222-3959.2015.04.25
Chen S, Feng Y, Stojanovic A et al (2012) Intralase femtosecond laser vs mechanical microkeratomes in LASIK for myopia: a systematic review and meta-analysis. J Refract Surg 28:15–24. https://doi.org/10.3928/1081597X-20111228-02
Igras E, O’Caoimh R, O’Brien P, Power W (2016) Long-term results of combined LASIK and monocular small-aperture corneal inlay implantation. J Refract Surg 32:379–384. https://doi.org/10.3928/1081597X-20160317-01
Antonios R, Jabbur NS, Ahmed MA, Awwad ST (2018) Refractory interface haze developing after epithelial ingrowth following laser in situ keratomileusis and small aperture corneal inlay implantation. Am J Ophthalmol Case Reports 10:10–12. https://doi.org/10.1016/j.ajoc.2018.01.034
Schanzlin DJ, Abbott RL, Asbell PA et al (2001) Two-year outcomes of intrastromal corneal ring segments for the correction of myopia. Ophthalmology 108:1688–1694. https://doi.org/10.1016/S0161-6420(01)00692-3
Randleman JB, Shah RD (2012) LASIK interface complications: etiology, management, and outcomes. J Refract Surg 28:575–586
Rubin GS, Bandeen-Roche K, Huang GH et al (2001) The association of multiple visual impairments with self-reported visual disability: SEE project. Investig Ophthalmol Vis Sci 42:64–72
Mai EL, Lian IB, Chang DC (2016) Assessment of contrast sensitivity loss after intrastromal femtosecond laser and LASIK procedure. Int J Ophthalmol. https://doi.org/10.18240/ijo.2016.12.16
Starr CE, Gupta PK, Farid M et al (2019) An algorithm for the preoperative diagnosis and treatment of ocular surface disorders. J Cataract Refract Surg 45:669–684
Shehadeh-Mashor R, Mimouni M, Shapira Y et al (2019) Risk factors for dry eye after refractive surgery. Cornea 38:1495–1499. https://doi.org/10.1097/ICO.0000000000002152
Funding
No funding support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no competing interest.
Ethical approval
This study was conducted in accordance with the tenets of the Helsinki Declaration and obtained Institutional Review Board approval.
Consent to participate
All patients included in this work were adequately informed verbally and in writing of the benefits, characteristics, and risks of the surgeries. All patients signed an informed consent prior to the surgery and after the interview performed with the ophthalmologist.
Consent for publication
All authors consent publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sánchez-González, JM., Borroni, D., Rachwani-Anil, R. et al. Refractive corneal inlay implantation outcomes: a preliminary systematic review. Int Ophthalmol 42, 713–722 (2022). https://doi.org/10.1007/s10792-021-02024-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-02024-4