Abstract
Purpose
To determine the prevalence of Meibomian gland dysfunction (MGD) and its risk factors in an elderly Iranian population
Methods
This cross-sectional study was conducted in 2019. The target population was the subjects aged 60 and over living in Tehran. Multistage cluster sampling was done to select the subjects from all Tehran districts. After an initial interview, all subjects underwent complete ophthalmic examinations including the measurement of visual acuity and refraction as well as slit lamp biomicroscopy to evaluate Meibomian glands.
Results
Of 3791 selected subjects, 3310 participated in the study. The data of 3284 participants were analyzed. The mean age of the subjects was 68.24 ± 6.53 years (range: 60–97 years) and 57.8% of them were female.
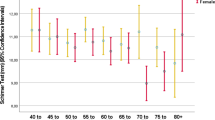
The total prevalence of MGD was 71.2% (68.3–74.1), and 38.1% (8.35–40.4), 30.3% (27.4–33.2), and 2.8% (2–3.6) of the subjects had MGD stage 2, 3, and 4, respectively. The prevalence of MGD was significantly higher in men (p < 0.001) and increased with age from 64.4% in the age group 60–64 years to 82.4% in subjects aged 80 years and over. There was no significant difference in the prevalence of MGD between smokers and nonsmokers; however, severe MGD was more common in smokers. The prevalence of MGD was 76.3% and 68.52% in subjects with and without a history of ocular surgery, respectively. The prevalence of MGD stage 3 and 4 was higher in subjects with a history of ocular surgery.
Conclusions
In line with the results of other studies in Asian countries, this study found a high prevalence of MGD in an elderly population of Iran. It was found that male gender and advanced age were risk factors of MGD and smoking and history of ocular surgery might worsen this disease in MGD patients.

Similar content being viewed by others
References
Nichols KK, Foulks GN, Bron AJ et al (2011) The international workshop on meibomian gland dysfunction: executive summary. Invest Ophthalmol Vis Sci 52:1922–1929. https://doi.org/10.1167/iovs.10-6997a
Leiske DL, Miller CE, Rosenfeld L et al (2012) Molecular structure of interfacial human meibum films. Langmuir 28:11858–11865. https://doi.org/10.1021/la301321r
Viso E, Gude F, Rodríguez-Ares MT (2011) The association of meibomian gland dysfunction and other common ocular diseases with dry eye: a population-based study in Spain. Cornea 30:1–6. https://doi.org/10.1097/ICO.0b013e3181da5778
Lam PY, Shih KC, Fong PY et al (2020) A review on evidence-based treatments for meibomian gland dysfunction. Eye Contact Lens 46:3–16. https://doi.org/10.1097/icl.0000000000000680
Stapleton F, Alves M, Bunya VY et al (2017) TFOS DEWS II Epidemiology Report. Ocul Surf 15:334–365. https://doi.org/10.1016/j.jtos.2017.05.003
Friedman NJ (2010) Impact of dry eye disease and treatment on quality of life. Curr Opin Ophthalmol 21:310–316. https://doi.org/10.1097/ICU.0b013e32833a8c15
Oleñik A, Mahillo-Fernández I, Alejandre-Alba N et al (2014) Benefits of omega-3 fatty acid dietary supplementation on health-related quality of life in patients with meibomian gland dysfunction. Clin Ophthalmol 8:831–836. https://doi.org/10.2147/opth.s62470
Uchino M, Dogru M, Yagi Y et al (2006) The features of dry eye disease in a Japanese elderly population. Optom Vis Sci 83:797–802. https://doi.org/10.1097/01.opx.0000232814.39651.fa
Siak JJ, Tong L, Wong WL et al (2012) Prevalence and risk factors of meibomian gland dysfunction: the Singapore Malay eye study. Cornea 31:1223–1228. https://doi.org/10.1097/ICO.0b013e31823f0977
Labbé A, Wang YX, Jie Y et al (2013) Dry eye disease, dry eye symptoms and depression: the Beijing eye study. Br J Ophthalmol 97:1399–1403. https://doi.org/10.1136/bjophthalmol-2013-303838
Amano S, Inoue K (2017) Estimation of prevalence of meibomian gland dysfunction in Japan. Cornea 36:684–688. https://doi.org/10.1097/ico.0000000000001208
Amano S, Inoue K (2017) Clinic-based study on meibomian gland dysfunction in Japan. Invest Ophthalmol Vis Sci 58:1283–1287. https://doi.org/10.1167/iovs.16-21374
Lin PY, Tsai SY, Cheng CY et al (2003) Prevalence of dry eye among an elderly Chinese population in Taiwan: the Shihpai Eye Study. Ophthalmology 110:1096–1101. https://doi.org/10.1016/s0161-6420(03)00262-8
Bukhari AA (2013) Associations between the grade of meibomian gland dysfunction and dyslipidemia. Ophthalmic Plast Reconstr Surg 29:101–103. https://doi.org/10.1097/IOP.0b013e31827a007d
Den S, Shimizu K, Ikeda T et al (2006) Association between meibomian gland changes and aging, sex, or tear function. Cornea 25:651–655. https://doi.org/10.1097/01.ico.0000227889.11500.6f
Hashemi H, Rastad H, Emamian MH et al (2017) Meibomian gland dysfunction and its determinants in Iranian adults: A population-based study. Cont Lens Anterior Eye 40:213–216. https://doi.org/10.1016/j.clae.2017.05.003
Geerling G, Tauber J, Baudouin C et al (2011) The international workshop on meibomian gland dysfunction: report of the subcommittee on management and treatment of meibomian gland dysfunction. Invest Ophthalmol Vis Sci 52:2050–2064. https://doi.org/10.1167/iovs.10-6997g
Alghamdi YA, Mercado C, Mcclellan AL et al (2016) Epidemiology of meibomian gland dysfunction in an elderly population. Cornea 35:731–735. https://doi.org/10.1097/ico.0000000000000815
Miljanović B, Dana R, Sullivan DA et al (2007) Impact of dry eye syndrome on vision-related quality of life. Am J Ophthalmol 143:409–415. https://doi.org/10.1016/j.ajo.2006.11.060
Nien CJ, Massei S, Lin G et al (2011) Effects of age and dysfunction on human meibomian glands. Arch Ophthalmol 129:462–469. https://doi.org/10.1001/archophthalmol.2011.69
Schaumberg DA, Nichols JJ, Papas EB et al (2011) The international workshop on meibomian gland dysfunction: report of the subcommittee on the epidemiology of, and associated risk factors for, MGD. Invest Ophthalmol Vis Sci 52:1994–2005. https://doi.org/10.1167/iovs.10-6997e
Mccarty CA, Bansal AK, Livingston PM et al (1998) The epidemiology of dry eye in Melbourne, Australia. Ophthalmology 105:1114–1119. https://doi.org/10.1016/s0161-6420(98)96016-x
Rabensteiner DF, Aminfar H, Boldin I et al (2018) The prevalence of meibomian gland dysfunction, tear film and ocular surface parameters in an Austrian dry eye clinic population. Acta Ophthalmol 96:e707–e711. https://doi.org/10.1111/aos.13732
Basak SK, Pal PP, Basak S et al (2012) Prevalence of dry eye diseases in hospital-based population in West Bengal, Eastern India. J Indian Med Assoc 110:789–794
Lekhanont K, Rojanaporn D, Chuck RS et al (2006) Prevalence of dry eye in Bangkok, Thailand. Cornea 25:1162–1167. https://doi.org/10.1097/01.ico.0000244875.92879.1a
Galor A, Feuer W, Lee DJ et al (2013) Ocular surface parameters in older male veterans. Invest Ophthalmol Vis Sci 54:1426–1433. https://doi.org/10.1167/iovs.12-10819
Viso E, Rodríguez-Ares MT, Abelenda D et al (2012) Prevalence of asymptomatic and symptomatic meibomian gland dysfunction in the general population of Spain. Invest Ophthalmol Vis Sci 53:2601–2606. https://doi.org/10.1167/iovs.11-9228
Sullivan DA, Sullivan BD, Ullman MD et al (2000) Androgen influence on the meibomian gland. Invest Ophthalmol Vis Sci 41:3732–3742
Schirra F, Richards SM, Liu M et al (2006) Androgen regulation of lipogenic pathways in the mouse meibomian gland. Exp Eye Res 83:291–296. https://doi.org/10.1016/j.exer.2005.11.026
Krenzer KL, Dana MR, Ullman MD et al (2000) Effect of androgen deficiency on the human meibomian gland and ocular surface. J Clin Endocrinol Metab 85:4874–4882. https://doi.org/10.1210/jcem.85.12.7072
Schirra F, Suzuki T, Richards SM et al (2005) Androgen control of gene expression in the mouse meibomian gland. Invest Ophthalmol Vis Sci 46:3666–3675. https://doi.org/10.1167/iovs.05-0426
Baudouin C, Messmer EM, Aragona P et al (2016) Revisiting the vicious circle of dry eye disease: a focus on the pathophysiology of meibomian gland dysfunction. Br J Ophthalmol 100:300–306. https://doi.org/10.1136/bjophthalmol-2015-307415
Gutgesell VJ, Stern GA, Hood CI (1982) Histopathology of meibomian gland dysfunction. Am J Ophthalmol 94:383–387. https://doi.org/10.1016/0002-9394(82)90365-8
Watters GA, Turnbull PR, Swift S et al (2017) Ocular surface microbiome in meibomian gland dysfunction. Clin Exp Ophthalmol 45:105–111. https://doi.org/10.1111/ceo.12810
Shamsheer RP, Arunachalam C (2015) A clinical study of meibomian gland dysfunction in patients with diabetes. Middle East Afr J Ophthalmol 22:462–466. https://doi.org/10.4103/0974-9233.167827
Pinna A, Blasetti F, Zinellu A et al (2013) Meibomian gland dysfunction and hypercholesterolemia. Ophthalmology 120:2385–2389. https://doi.org/10.1016/j.ophtha.2013.05.002
Bu J, Wu Y, Cai X et al (2019) Hyperlipidemia induces meibomian gland dysfunction. Ocul Surf 17:777–786. https://doi.org/10.1016/j.jtos.2019.06.002
Han KE, Yoon SC, Ahn JM et al (2014) Evaluation of dry eye and meibomian gland dysfunction after cataract surgery. Am J Ophthalmol 157(1144–1150):e1141. https://doi.org/10.1016/j.ajo.2014.02.036
Park Y, Hwang HB, Kim HS (2016) Observation of Influence of Cataract Surgery on the Ocular Surface. PLoS ONE 11:e0152460. https://doi.org/10.1371/journal.pone.0152460
Kim JS, Lee H, Choi S et al (2018) Assessment of the tear film lipid layer thickness after cataract surgery. Semin Ophthalmol 33:231–236. https://doi.org/10.1080/08820538.2016.1208764
Funding
This project was financially supported by National Institute for Medical Research Development (NIMAD) affiliated with the Iranian Ministry of Health and Medical Education (Grant code: 963660).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflicting relationship exists for any author.
Ethical approval
This study was approved by the Ethics Committee of National Institute for Medical Research Development affiliated with the Iranian Ministry of Health and Medical Education.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hashemi, H., Asharlous, A., Aghamirsalim, M. et al. Meibomian gland dysfunction in geriatric population: tehran geriatric eye study. Int Ophthalmol 41, 2539–2546 (2021). https://doi.org/10.1007/s10792-021-01812-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-01812-2