Summary
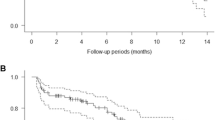
Background Vandetanib is a tyrosine kinase inhibitor of both the vascular endothelial growth factor (VEGFR) and epidermal growth factor (EGFR) receptors. The primary objectives of this study were to determine the maximum tolerated dose of vandetanib with capecitabine and oxaliplatin, without and with bevacizumab, for the first line treatment of metastatic colorectal cancer (mCRC), and to define the dose limiting toxicities. Materials and methods Three cohorts of patients were studied, with capecitabine at 1,000 mg/m2 twice daily p.o. on days 1–14 of a 3 week cycle, with oxaliplatin i.v. at 130 mg/m2 on day 1. Vandetanib dosing was 100 mg/day in cohort 1 and 300 mg/day in cohorts 2 and 3. Bevacizumab was added in cohort 3 at 7.5 mg/kg IV on day 1 every 3 weeks. Results Thirteen patients were enrolled and received from one to eight cycles per patient. Grade 4 dermatitis developed in one patient in the first cohort, and the cohort was expanded to six patients with no further dose limiting toxicities (DLT). The second cohort of 3 patients was well tolerated. The third cohort resulted in grade 3 diarrhea, requiring several days of hospitalization and IV hydration, in 3 of the 4 patients. Given the severity and duration of diarrhea, each of these was considered a DLT, and therefore cohort 3 was considered to be above the maximum tolerated dose. Six of the 13 patients achieved a partial or complete remission (46%). The time to progression ranged from 2 to 14 months. Conclusions Vandetanib at doses of 100 mg and 300 mg daily in combination with capecitabine and oxaliplatin was well tolerated. However, the addition of bevacizumab resulted in severe diarrhea in three out of four patients. Bevacizumab was not well tolerated with vandetanib and XELOX in combination.
Similar content being viewed by others
References
Mayer A, Takimoto M, Fritz E, Schellander G, Kofler K, Ludwig H (1993) The prognostic significance of proliferating cell nuclear antigen, epidermal growth factor receptor, and mdr gene expression in colorectal cancer. Cancer 71:2454–2460
Kawamoto T, Sato JD, Le A, McClure DB, Sato GH (1983) Biological effects in vitro of monoclonal antibodies to human epidermal growth factor receptors. Mol Biol Med 1:511–529
Masui H, Kawamoto T, Sato JD, Wolf B, Sato G, Mendelsohn J (1984) Growth inhibition of human tumor cells in athymic mice by anti-epidermal growth factor receptor monoclonal antibodies. Cancer Res 44:1002–1007
Yang XD, Jia XC, Corvalan JR, Wang P, Davis CG, Jakobovits A (1999) Eradication of established tumors by a fully human monoclonal antibody to the epidermal growth factor receptor without concomitant chemotherapy. Cancer Res 15:1236–1243
Pollack VA, Savage DM, Baker DA et al (1999) Inhibition of epidermal growth factor receptor-associated tyrosine phosphorylation in human carcinomas with CP-358,774: dynamics of receptor inhibition in situ and antitumor effects in athymic mice. J Pharmacol Exp Ther 291:739–748
Lichtner RB, Menrad A, Sommer A, Klar U, Schneider MR (2001) Signaling-inactive epidermal growth factor receptor/ligand complexes in intact carcinoma cells by quinazoline tyrosine kinase inhibitors. Cancer Res 61:5790–5795
Kuo T, Cho CD, Halsey J, Wakelee HA, Advani RH, Ford JM, Fisher GA, Sikic BI (2005) A Phase II Study of IFOX Therapy (Gefitinib, 5-Fluorouracil, Leucovorin, Oxaliplatin) in Previously Treated Patients with Metastatic Colorectal Cancer. J Clin Oncol 23:5613–5619
Folkman J (1972) Anti-angiogenesis: new concept for therapy of solid tumors. Ann Surg 175:409–416
Ellis LM, Takahashi Y, Liu W et al (2000) Vascular endothelial growth factor in human colon cancer: biology and therapeutic implications. Oncologist 5:11–15
Dvorak HF (2002) Vascular permeability factor/vascular endothelial growth factor: a critical cytokine in tumor angiogenesis and a potential target for diagnosis and therapy. J Clin Oncol 20:4368–4380
Wedge SR, Ogilvie DJ, Dukes M, Kendrew J, Chester R, Jackson JA, Boffey SJ, Valentine PJ, Curwen JO, Musgrove HL, Graham GA, Hughes GD, Thomas AP, Stokes ES, Curry B, Richmond GH, Wadsworth PF, Bigley AL, Hennequin LF (2002) ZD6474 inhibits vascular endothelial growth factor signaling, angiogenesis, and tumor growth following oral administration. Cancer Res 62:4645–4655
Carlomagno F, Vitagliano D, Guida T, Ciardiello F, Tortora G, Vecchio G, Ryan AJ, Fontanini G, Fusco A, Santoro M (2002) ZD6474, an orally available inhibitor of KDR tyrosine kinase activity, efficiently blocks oncogenic RET kinases. Cancer Res 62:7284–7290
Holden SN, Eckhardt SG, Basser R et al (2005) Clinical evaluation of Zd6474, an orally active inhibitor of VEGF and EGF receptor signaling, in patients with solid, malignant tumors. Ann Oncol 16:1391–1397
Tamura T, Minami H, Yamada Y et al (2006) A Phase I dose-escalation study of ZD6474 in Japanese patients with solid, malignant tumors. J Thorac Oncol 1:1002–1009
Natale RB, Bodkin D, Govindan R et al (2009) Vandetanib versus gefitinib in patients with advanced non-small cell lung cancer: results from a two-part, double-blind, randomized phase II study. J Clin Oncol 27:2523–2529
Heymach JV, Johnson BE, Prager D et al (2007) Randomized placebo-controlled phase II study of vandetanib plus docetaxel in previously treated non small-cell lung cancer. J Clin Oncol 25:4270–4277
Heymach JV, Paz-Ares L, Braud D et al (2008) Randomized phase II study of vandetanib alone or with paclitaxel and carboplatin as first-line treatment for advanced non-small cell lung cancer. J Clin Oncol 26:5407–5415
Michael M, Gibbs P, Smith R et al (2009) Open-label phase I trial of vandetanib in combination with mFOLFOX6 in patients with advanced colorectal cancer. Invest New Drugs 27:253–261, Epub 2008 Nov 11
Evelhoch JL, LoRusso PM, He Z, DelProposto Z, Polin L, Corbett TH, Langmuir P, Wheeler C, Stone A, Leadbetter J, Ryan AJ, Blakey DC, Waterton JC (2004) Magnetic resonance imaging measurements of the response of murine and human tumors to the vascular-targeting agent ZD6126. Clin Cancer Res 10:3650–3657
Howe FA, Robinson SP, McIntyre DJ, Stubbs M, Griffiths JR (2001) Issues in flow and oxygenation dependent contrast (FLOOD) imaging of tumours. NMR Biomed 14:497–506
Mross K, Fasol U, Frost A et al (2009) DCE-MRI assessment of the effect of vandetanib on tumor vasculature in patients with advanced colorectal cancer and liver metastases: a randomized phase I study. J Angiogenesis Res 1:5
Hecht JR, Mitchell E, Chidiac T et al (2009) A randomized phase IIIB trial of chemotherapy, bevacizumab, and panitumumab compared with chemotherapy and bevacizumab alone for metastatic colorectal cancer J Clin Oncol 27:672–680
Tol J, Koopman M, Cats A et al (2009) Chemotherapy, bevacizumab, and cetuximab in metastatic colorectal cancer. New Engl J Med 360:563–572
Saltz LB, Lenz H-J, Kindler HL et al (2007) Randomized phase II trial of cetuximab, bevacizumab, and irinotecan compared with cetuximab and bevacizumab alone in irinotecan-refractory colorectal cancer: the BOND-2 study J Clin Oncol 25:4557–4561
Acknowledgments
This study was sponsored by AstraZeneca Pharmaceuticals, Inc.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cabebe, E.C., Fisher, G.A. & Sikic, B.I. A phase I trial of vandetanib combined with capecitabine, oxaliplatin and bevacizumab for the first-line treatment of metastatic colorectal cancer. Invest New Drugs 30, 1082–1087 (2012). https://doi.org/10.1007/s10637-011-9656-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-011-9656-y