Abstract
Background
Esophageal diverticulum (ED) is an uncommon structural disorder with heterogenous manifestations and elusive pathophysiology. Our aim was to investigate esophageal motility and associated symptom profiles in patients with ED based on high-resolution impedance manometry (HRIM).
Methods
Consecutive patients with ED referred to our motility laboratory between 2015 to 2022 were identified in our electronic database. All patients were evaluated based on an upper endoscopy, HRIM, and standardized symptom questionnaires. Patients with ED were further stratified into upper, middle, and lower (epiphrenic) cases. Esophageal motility was evaluated with HRIM and the updated Chicago Classification v4.0.
Results
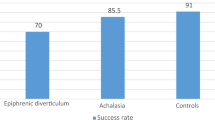
Twenty-four patients with ED (9 upper, 4 middle, and 11 epiphrenic) were analyzed. Patients with ED were generally older (mean: 65 ± 13.3 years) and predominantly women (58.3%). Most ED cases were unilaterally located (95.8%) and left-side predominant (62.5%). Mean symptom duration was 20 months (range: 1–120) and the most common symptoms were dysphagia (70.8%) and regurgitation (37.5%). Erosive esophagitis was noted in 16 patients (69.6%), while barium stasis was noted in 5 patients (20.8%). Fourteen patients (58.3%) were diagnosed with esophageal motility disorders using HRIM, with achalasia being the most common diagnosis (n = 5, 20.8%). Patients with epiphrenic diverticulum had significantly higher symptom scores and achalasia prevalence.
Conclusion
Patients with ED tended to be older and was associated with a high prevalence of EMD. A multi-disciplinary evaluation, including complete anatomical and motility surveys, may help clarify the underlying pathophysiology and tailor further treatment strategies.
Graphical Abstract




Similar content being viewed by others
References
Herbella FA, Patti MG. Modern pathophysiology and treatment of esophageal diverticula. Langenbecks Arch Surg 2012;397:29–35.
Martinez-Paredes JF, Alfakir R, Kasperbauer JL et al. Zenker Diverticulum: does size correlate with preoperative symptoms? Int Arch Otorhinolaryngol 2022;26:e334–e338.
Fasano NC, Levine MS, Rubesin SE et al. Epiphrenic diverticulum: clinical and radiographic findings in 27 patients. Dysphagia 2003;18:9–15.
Law R, Katzka DA, Baron TH. Zenker's Diverticulum. Clin Gastroenterol Hepatol 2014;12:1773–1782; quiz e111–2.
Cassivi SD, Deschamps C, Nichols FC III et al. Diverticula of the esophagus. Surg Clin North Am 2005;85(495–503):ix.
do Nascimento FAP, Lemme EMO, Costa MMB. Esophageal diverticula: pathogenesis, clinical aspects, and natural history. Dysphagia 2006;21:198–205.
Nehra D, Lord RV, DeMeester TR et al. Physiologic basis for the treatment of epiphrenic diverticulum. Ann Surg 2002;235:346–354.
Nguyen HN, Domingues GR, Lammert F. Technological insights: combined impedance manometry for esophageal motility testing-current results and further implications. World J Gastroenterol 2006;12:6266–6273.
Tutuian R, Castell DO. Esophageal function testing: role of combined multichannel intraluminal impedance and manometry. Gastrointest Endosc Clin N Am 2005;15:265–275.
Nguyen NQ, Rigda R, Tippett M et al. Assessment of oesophageal motor function using combined perfusion manometry and multi-channel intra-luminal impedance measurement in normal subjects. Neurogastroenterol Motil 2005;17:458–465.
Yadlapati R, Kahrilas PJ, Fox MR et al. Esophageal motility disorders on high-resolution manometry: Chicago classification version 4.0(©). Neurogastroenterol Motil 2021;33:e14058.
Taft TH, Carlson DA, Triggs J et al. Evaluating the reliability and construct validity of the Eckardt symptom score as a measure of achalasia severity. Neurogastroenterol Motil 2018;30:e13287.
Shaw M, Dent J, Beebe T et al. The Reflux Disease Questionnaire: a measure for assessment of treatment response in clinical trials. Health Qual Life Outcomes 2008;6:31.
Belafsky PC, Postma GN, Koufman JA. Validity and reliability of the reflux symptom index (RSI). J Voice 2002;16:274–277.
Lu IC, Yen Jean MC, Lei SM et al. BSRS-5 (5-item Brief Symptom Rating Scale) scores affect every aspect of quality of life measured by WHOQOL-BREF in healthy workers. Qual Life Res 2011;20:1469–1475.
Buysse DJ, Reynolds CF 3rd, Monk TH et al. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 1989;28:193–213.
Hung JJ, Hsieh CC, Lin SC et al. Squamous cell carcinoma in a large epiphrenic esophageal diverticulum. Dig Dis Sci 2009;54:1365–1368.
Brandeis AE, Singhal S, Lee TH et al. Surgical management of epiphrenic diverticulum: a single-center experience and brief review of literature. Am J Surg 2018;216:280–285.
Onwugbufor MT, Obirieze AC, Ortega G et al. Surgical management of esophageal diverticulum: a review of the Nationwide Inpatient Sample database. J Surg Res 2013;184:120–125.
Gregersen H, Pedersen J, Drewes AM. Deterioration of muscle function in the human esophagus with age. Digestive Diseases and Sciences 2008;53:3065–3070.
Iwakiri K, Hayashi Y, Kotoyori M et al. Defective triggering of secondary peristalsis in patients with non-erosive reflux disease. J Gastroenterol Hepatol 2007;22:2208–2211.
Sato H, Fujiyoshi Y, Abe H et al. Development of dilated esophagus, sigmoid esophagus, and esophageal diverticulum in patients with achalasia: Japan Achalasia Multicenter Study. J Neurogastroenterol Motil 2022;28:222–230.
Carlson DA, Gluskin AB, Mogni B et al. Esophageal diverticula are associated with propagating peristalsis: a study utilizing high-resolution manometry. Neurogastroenterol Motil 2016;28:392–398.
Thomas ML, Anthony AA, Fosh BG et al. Oesophageal diverticula. Br J Surg 2001;88:629–642.
Klaus A, Hinder RA, Swain J et al. Management of epiphrenic diverticula. J Gastrointest Surg 2003;7:906–911.
Sato H, Sato Y, Takeuchi M, et al. Salvage peroral endoscopic myotomy for esophageal diverticulum. Endoscopy 2015;47(Suppl 1 UCTN):E14–E15.
Yang J, Novak S, Ujiki M et al. An international study on the use of peroral endoscopic myotomy in the management of Zenker’s diverticulum. Gastrointest Endosc 2020;91:163–168.
Sanaei O, Ichkhanian Y, Mondragón OVH et al. Impact of prior treatment on feasibility and outcomes of Zenker’s peroral endoscopic myotomy (Z-POEM). Endoscopy 2021;53:722–726.
Yang J, Zeng X, Yuan X et al. An international study on the use of peroral endoscopic myotomy (POEM) in the management of esophageal diverticula: the first multicenter D-POEM experience. Endoscopy 2019;51:346–349.
Facciorusso A, Ramai D, Ichkhanian Y et al. Peroral endoscopic myotomy for the treatment of esophageal diverticula: a systematic review and meta-analysis. J Clin Gastroenterol 2022;56:853–862.
Bergeron JL, Long JL, Chhetri DK. Dysphagia characteristics in Zenker’s diverticulum. Otolaryngol Head Neck Surg 2013;148:223–228.
Rezende DT, Herbella FA, Silva LC et al. Upper esophageal sphincter resting pressure varies during esophageal manometry. Arq Bras Cir Dig 2014;27:182–183.
Acknowledgments
This study was supported by research grants from the National Taiwan University Hospital (NTUH 112-S0320) and the Ministry of Science and Technology (MOST 111-2314-B-002-189-MY3). The funding agencies had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript. The authors would also like to thank Unit-Edit (www.uni-edit.net) for editing and proofreading this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no potential, perceived, or real conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yuan, MC., Chou, CK., Chen, CC. et al. Characteristics of Esophageal Motility and Associated Symptom Profiles in Patients with Esophageal Diverticulum: A Study Based on High-Resolution Impedance Manometry. Dig Dis Sci 69, 510–520 (2024). https://doi.org/10.1007/s10620-023-08196-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-023-08196-6