Abstract
Background
Chronic constipation can have one or more of many etiologies, and a diagnosis based on symptoms is not sufficient as a basis for treatment, in particular surgery.
Aim
To investigate the cause of chronic constipation in a patient with complete absence of spontaneous bowel movements.
Methods
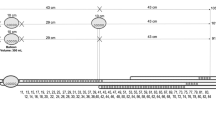
High-resolution colonic manometry was performed to assess motor functions of the colon, rectum, the sphincter of O’Beirne and the anal sphincters.
Results
Normal colonic motor patterns were observed, even at baseline, but a prominent high-pressure zone at the rectosigmoid junction, the sphincter of O’Beirne, was consistently present. In response to high-amplitude propagating pressure waves (HAPWs) that were not consciously perceived, the sphincter and the anal sphincters would not relax and paradoxically contract, identified as autonomous dyssynergia. Rectal bisacodyl evoked marked HAPW activity with complete relaxation of the sphincter of O’Beirne and the anal sphincters, indicating that all neural pathways to generate the coloanal reflex were intact but had low sensitivity to physiological stimuli. A retrograde propagating cyclic motor pattern initiated at the sphincter of O’Beirne, likely contributing to failure of content to move into the rectum.
Conclusions
Chronic constipation without the presence of spontaneous bowel movements can be associated with normal colonic motor patterns but a highly exaggerated pressure at the rectosigmoid junction: the sphincter of O’Beirne, and failure of this sphincter and the anal sphincters to relax associated with propulsive motor patterns. The sphincter of O’Beirne can be an important part of the pathophysiology of chronic constipation.








Similar content being viewed by others
Abbreviations
- HRCM:
-
High-resolution colonic manometry
- HAPW:
-
High-amplitude propagating pressure wave
- HAPW-SPW:
-
High-amplitude propagating pressure wave followed by a simultaneous pressure wave
- SPW:
-
Simultaneous pressure wave
- RAIR:
-
Recto-anal inhibitory reflex
References
Mugie SM, Benninga MA, Di Lorenzo C. Epidemiology of constipation in children and adults: a systematic review. Best Pract Res Clin Gastroenterol. 2011;25:3–18.
Lembo A, Camilleri M. Chronic constipation. N Engl J Med. 2003;349:1360–1368.
Rao SS, Rattanakovit K, Patcharatrakul T. Diagnosis and management of chronic constipation in adults. Nat Rev Gastroenterol Hepatol. 2016;13:295–305.
Bharucha AE, Pemberton JH, Locke GR. American Gastroenterological Association technical review on constipation. Gastroenterology. 2013;144:218–238.
Dudekula A, Huftless S, Bielefeldt K. Colectomy for constipation: time trends and impact based on the US Nationwide Inpatient Sample, 1998–2011. Aliment Pharmacol Ther. 2015;42:1281–1293.
Gladman MA, Knowles CH. Surgical treatment of patients with constipation and fecal incontinence. Gastroenterol Clin North Am. 2008;37:605–625.
Rodriguez L, Sood M, Di Lorenzo C, Saps M. An ANMS-NASPGHAN consensus document on anorectal and colonic manometry in children. Neurogastroenterol Motil. 2017;29:e12944.
Rao SS, Sadeghi P, Beaty J, Kavlock R, Ackerson K. Ambulatory 24-h colonic manometry in healthy humans. Am J Physiol Gastrointest Liver Physiol. 2001;280:G629–G639.
Chen J-H, Yu Y, Yang Z, et al. Intraluminal pressure patterns in the human colon assessed by high-resolution manometry. Sci. Rep.. 2017;7:41436. https://doi.org/10.1038/srep41436.
Chen J-H, Parsons SP, Shokrollahi M, et al. Characterization of simultaneous pressure waves as biomarkers for colonic motility assessed by high-resolution colonic manometry. Front Physiol Gastrointest Sci. 2018;9:1248. https://doi.org/10.3389/fphys.2018.01248.
Corsetti M, Pagliaro G, Demedts I, et al. Pan-colonic pressurizations associated with relaxation of the anal sphincter in health and disease: a new colonic motor pattern identified using high-resolution manometry. Am J Gastroenterol. 2017;112:479–489.
Rao SS, Sadeghi P, Batterson K, Beaty J. Altered periodic rectal motor activity: a mechanism for slow transit constipation. Neurogastroenterol Motil. 2001;13:591–598.
Lin AY, Du P, Dinning PG, et al. High-resolution anatomic correlation of cyclic motor patterns in the human colon: evidence of a rectosigmoid brake. Am J Physiol Gastrointest Liver Physiol. 2017;312:G508–G515.
Dinning PG, Wiklendt L, Maslen L, et al. Colonic motor abnormalities in slow transit constipation defined by high resolution, fibre-optic manometry. Neurogastroenterol Motil. 2015;27:379–388.
Pervez M, Ratcliffe E, Parsons SP, Chen J-H, Huizinga JD. The cyclic motor patterns in the human colon. Neurogastroenterol Motil. 2020;. https://doi.org/10.1111/nmo.13807.
Milkova N, Parsons SP, Ratcliffe E, Huizinga JD, Chen JH. On the nature of high-amplitude propagating pressure waves in the human colon. Am J Physiol Gastrointest Liver Physiol. 2020;318:G646–G660. https://doi.org/10.1152/ajpgi.00386.2019.
Malcolm A, Camilleri M. Coloanal motor coordination in association with high-amplitude colonic contractions after pharmacological stimulation. Am J Gastroenterol. 2000;95:715–719.
Chen J-H, Nirmalathasan S, Milkova N, Huizinga JD. The Sphincter of O’Beirne – Part 1: Study of 18 Normal Subjects. Dig Dis Sci. 2020;. https://doi.org/10.1007/s10620-020-06657-w.
Dinning PG, Wiklendt L, Maslen L, et al. Quantification of in vivo colonic motor patterns in healthy humans before and after a meal revealed by high-resolution fiber-optic manometry. Neurogastroenterol Motil. 2014;. https://doi.org/10.1111/nmo.12408.
Bharucha AE. High amplitude propagated contractions. Neurogastroenterol Motil. 2012;24:977–982.
Corsetti M, Costa M, Bassotti G, et al. Translational consensus on terminology and definition of colonic motility by means of manometric and non-manometric techniques. Nat Rev Gastroenterol Hepatol. 2019;16:559–579.
Yarullina DR, Shafigullin MU, Sakulin KA, et al. Characterization of gut contractility and microbiota in patients with severe chronic constipation. PLoS One. 2020;15:e0235985.
Rao SS, Welcher K. Periodic rectal motor activity: the intrinsic colonic gatekeeper. Am J Gastroenterol. 1996;91:890–897.
Rodriguez L, Siddiqui A, Nurko S. Internal anal sphincter relaxation associated with bisacodyl-induced colonic high amplitude propagating contractions in children with constipation: a colo-anal reflex? Neurogastroenterol Motil. 2012;24:1023-e545.
Fogel GR, Cunningham PY, Esses SI. Coccygodynia: evaluation and management. J Am Acad Orthop Surg. 2004;12:49–54.
Knowles CH, Scott SM, Lunniss PJ. Slow transit constipation: a disorder of pelvic autonomic nerves? Dig Dis Sci. 2001;46:389–401. https://doi.org/10.1023/A:1005665218647.
Broens PM, Penninckx FM, Ochoa JB. Fecal continence revisited: the anal external sphincter continence reflex. Dis Colon Rectum. 2013;56:1273–1281.
Kock NG, Kewenter J, Sundin T. Studies on the defecation reflex in man. Scand J Gastroenterol. 1972;7:689–693.
Yuan Y, Ali MK, Mathewson KJ, et al. Associations between colonic motor patterns and autonomic nervous system activity assessed by high-resolution manometry and concurrent heart rate variability. Front Neurosci. 2019;13:1447. https://doi.org/10.3389/fnins.2019.01447.
Bampton PA, Dinning PG, Kennedy ML, Lubowski DZ, deCarle D, Cook IJ. Spatial and temporal organization of pressure patterns throughout the unprepared colon during spontaneous defecation. Am J Gastroenterol. 2000;95:1027–1035.
Devroede G, Lamarche J. Functional importance of extrinsic parasympathetic innervation to the distal colon and rectum in man. Gastroenterology. 1974;66:273–280.
Moszkowicz D, Peschaud F, Bessede T, Benoit G, Alsaid B. Internal anal sphincter parasympathetic-nitrergic and sympathetic-adrenergic innervation: a 3-dimensional morphological and functional analysis. Dis Colon Rectum. 2012;55:473–481.
Mills K, Hausman N, Chess-Williams R. Characterization of the alpha1-adrenoceptor subtype mediating contractions of the pig internal anal sphincter. Br J Pharmacol. 2008;155:110–117.
Mills K, Chess-Williams R. Pharmacology of the internal anal sphincter and its relevance to faecal incontinence. Auton Autacoid Pharmacol. 2009;29:85–95.
Roppolo JR, Nadelhaft I, de Groat WC. The organization of pudendal motoneurons and primary afferent projections in the spinal cord of the rhesus monkey revealed by horseradish peroxidase. J Comp Neurol. 1985;234:475–488.
Konishi A, Itoh K, Sugimoto T, et al. Leucine-enkephalin-like immunoreactive afferent fibers to pudendal motoneurons in the cat. Neurosci Lett. 1985;61:109–113.
Beckel JM, Holstege G. Neuroanatomy of the lower urinary tract. In: Anderson K-E, Michel MC, eds. Urinary Tract. Handb. Exp. Pharmacol.202.Berlin: Springer; 2011:99–116.
Kenefick NJ. Sacral nerve neuromodulation for the treatment of lower bowel motility disorders. Ann R Coll Surg Engl. 2006;88:617–623.
Connell AM. The motility of the pelvic colon. II. Paradoxical motility in diarrhoea and constipation. Gut. 1962;3:342–348.
Bampton PA, Dinning PG, Kennedy ML, Lubowski DZ, Cook IJ. Prolonged multi-point recording of colonic manometry in the unprepared human colon: providing insight into potentially relevant pressure wave parameters. Am J Gastroenterol. 2001;96:1838–1848.
Quan X, Yang Z, Xue M, Chen J-H, Huizinga JD. Relationships between motor patterns and intraluminal pressure in the 3-taeniated proximal colon of the rabbit. Sci Rep. 2017;7:42293. https://doi.org/10.1038/srep42293.
O’Beirne J. Organic stricture of the rectum. The Lancet. 1834;21:712–719.
Ballantyne GH. Rectosigmoid sphincter of O’Beirne. Dis Colon Rectum. 1986;29:525–531.
Balli R. Le röntgendiagnostic surtout au point de vue des organes de l’abdomen. Acta Radiol. 1928;3:89–106.
Baker WNW, Mann CV. The rectosigmoid junction zone, another sphincter? In: Thomas PA, Mann CV, eds. Alimentary Sphincter and Their Disorders. London: Palgrave Macmillan; 1981:201–211.
Buntzen S, Nordgren S, Hultén L, Delbro D. The role of nitric oxide in the acetylcholine-induced relaxation of the feline internal anal sphincter, in vitro. Scand J Gastroenterol. 1996;31:1189–1194.
Cook TA, Brading AF, Mortensen NJ. The pharmacology of the internal anal sphincter and new treatments of ano-rectal disorders. Aliment Pharmacol Ther. 2001;15:887–898.
Chowdhury AR, Dinoso VP, Lorber SH. Characterization of a hyperactive segment at the rectosigmoid junction. Gastroenterology. 1976;71:584–588.
Lin AY, Dinning PG, Milne T, Bissett IP, O’Grady G. The “rectosigmoid brake”: review of an emerging neuromodulation target for colorectal functional disorders. Clin Exp Pharmacol Physiol. 2017;44:719–728.
Stoss F. Investigations of the muscular architecture of the rectosigmoid junction in humans. Dis Colon Rectum. 1990;33:378–383.
O’Beirne J. New Views of the Process of Defecation, and Their Application to the Pathology and Treatment of Diseases of the Stomach, Bowels, and Other Organs. Dublin: Hodges and Smith; 1833.
Shafik A, Shafik AA, El-Sibai O, Mostafa RM. Electric activity of the colon in subjects with constipation due to total colonic inertia: an electrophysiologic study. ArchSurg. 2003;138:1007–1011.
Hutson JM, Dughetti L, Stathopoulos L, Southwell BR. Transabdominal electrical stimulation (TES) for the treatment of slow-transit constipation (STC). Pediatr Surg Int. 2015;31:445–451.
Lu PL, Di Lorenzo C. Neurostimulation of the gastrointestinal tract in children: is it time to shock the gut? Curr Opin Pediatr. 2016;28:631–637.
Huang Z, Li S, Foreman RD, Yin J, Dai N, Chen JDZ. Sacral nerve stimulation with appropriate parameters improves constipation in rats by enhancing colon motility mediated via the autonomic-cholinergic mechanisms. Am J Physiol Gastrointest Liver Physiol. 2019;317:G609–G617.
Chen J-H, Ratcliffe E, Armstrong D, Bercik P, Huizinga JD. Simultaneous pressure waves are a key component of human colonic motor function assessment, using high-resolution colonic manometry (HRCM). J Can Assoc Gastroenterol. 2018;1:527–528.
Chen J-H, Yuan Y, Tan W, Matthewson K, Parsons S, Huizinga JD. Measuring reactivity of the extrinsic autonomic nervous system associated with human colon motor patterns via heart rate variability. Neurogastroenterol Motil. 2018;. https://doi.org/10.1111/nmo.13423.
Acknowledgments
JDH received a Canadian Foundation for Innovation John Evans Leadership Grant for the equipment used in this study. Operating funds were obtained from the Canadian Institutes of Health Research (CIHR, 152942) to JDH. The Farncombe Family Digestive Health Research Institute provided partial salary support for J-HC. The hardware was designed in collaboration with Medical Measurement Systems. The catheters were designed in collaboration with Howard Mui and staff at Mui Scientific. Parts of this research were presented at the Canadian Digestive Diseases Week of 2018 [56] and the Federation of Neurogastroenterology and Motility, 2018 [57].
Author information
Authors and Affiliations
Contributions
Study design, data interpretation and writing of manuscript, J-HC and JDH. Execution of HRCM and clinical care, J-HC. Clinical care, data interpretation, critical revision of the manuscript, SMC. Data analysis, data interpretation and manuscript writing NM, MP, SN, WT, AH. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there was no conflict of interest of any kind.
Informed consent
All procedures were approved by the Hamilton Integrated Research Ethics Board (HiREB); the patient gave written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, JH., Collins, S.M., Milkova, N. et al. The Sphincter of O’Beirne—Part 2: Report of a Case of Chronic Constipation with Autonomous Dyssynergia. Dig Dis Sci 66, 3529–3541 (2021). https://doi.org/10.1007/s10620-020-06723-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06723-3