Abstract
Major depression disorder (MDD) is a neuropsychiatric disorder associated with a high suicide rate and a higher disability rate than any other disease. Evidence suggests that the pathological mechanism of MDD is related to astrocyte dysfunction. Depression is mainly associated with the expression of connexin 43 (Cx43) and the function of Cx43-mediated gap junctions and hemichannels in astrocytes. Moreover, neuroinflammation has been a hotspot in research on the pathology of depression, and Cx43-mediated functions are thought to be involved in neuroinflammation-related depression. However, the specific mechanism of Cx43-mediated functions in neuroinflammation-related depression pathology remains unclear. Therefore, this review summarizes and discusses Cx43 expression, the role of gap junction intercellular communication, and its relationship with neuroinflammation in depression. This review also focuses on the effects of antidepressant drugs (e.g., monoamine antidepressants, psychotropic drugs, and N-methyl-d-aspartate receptor antagonists) on Cx43-mediated function and provides evidence for Cx43 as a novel target for the treatment of MDD.
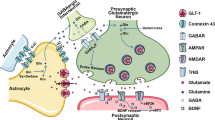
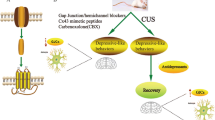
Graphical Abstract
The pathogenesis of MDD is related to astrocyte dysfunction, with reduced Cx43 expression, GJ dysfunction, decreased GJIC and reduced BDNF expression in the depressed brain. The effect of Cx43 on neuroinflammation-related depression involving inflammatory cytokines, glutamate excitotoxicity, and HPA axis dysregulation. Antidepressant drugs targeting Cx43 can effectively relieve depressive symptoms.



Similar content being viewed by others
Data Availability
Enquiries about data availability should be directed to the authors.
Abbreviations
- AMPA receptor:
-
α-Amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid receptor
- BBB:
-
Blood–brain barrier
- BDNF:
-
Brain-derived neurotrophic factor
- CBX:
-
Carbenoxolone
- CMS:
-
Chronic mild stress
- CNS:
-
Central nervous system
- CORT:
-
Corticosterone
- CRS:
-
Chronic resistance stress
- CSDS:
-
Chronic social defeat stress
- CUMS:
-
Chronic unpredictable mild stress
- CUS:
-
Chronic unpredictable stress
- Cx43:
-
Connexin 43
- EAAT:
-
Excitatory amino acid transporters
- FST:
-
Forced swim test
- GFAP:
-
Glial fibrillary acidic protein
- GJ:
-
Gap junction
- GJC:
-
Gap junction channel
- GJIC:
-
Gap junction intercellular communication
- Gln:
-
Glutamine
- Glu:
-
Glutamate
- GS:
-
Glutamine synthetase
- HC:
-
Hemichannel
- HIP:
-
Hippocampus
- HPA axis:
-
Hypothalamic–pituitary–adrenal axis
- IL-6:
-
Interleukin-6
- IL-10:
-
Interleukin-10
- IL-1β:
-
Interleukin-1beta
- MDD:
-
Major depression disorder
- mPFC:
-
Medial prefrontal cortex
- NMDA receptor:
-
N-Methyl-d-aspartate receptor
- PFC:
-
Prefrontal cortex
- PSD:
-
Poststroke depression
- SNI:
-
Spared nerve injury
- SNRI:
-
Serotonin and norepinephrine reuptake inhibitor
- SSRI:
-
Selective serotonin reuptake inhibitor
- TCA:
-
Tricyclic antidepressant
- TGF-β:
-
Transforming growth factor-beta
- TNF-α:
-
Tumor necrosis factor-α
- TrkB:
-
Tropomyosin receptor kinase B
References
Aasen T, Johnstone S, Vidal-Brime L, Lynn KS, Koval M (2018) Connexins: synthesis, post-translational modifications, and trafficking in health and disease. Int J Mol Sci 19(5):1296. https://doi.org/10.3390/ijms19051296
Abudara V, Roux L, Dallérac G, Matias I, Dulong J, Mothet JP, Rouach N, Giaume C (2015) Activated microglia impairs neuroglial interaction by opening Cx43 hemichannels in hippocampal astrocytes. Glia 63(5):795–811. https://doi.org/10.1002/glia.22785
Ahmad MH, Rizvi MA, Fatima M, Mondal AC (2021) Pathophysiological implications of neuroinflammation mediated HPA axis dysregulation in the prognosis of cancer and depression. Mol Cell Endocrinol 520:111093. https://doi.org/10.1016/j.mce.2020.111093
Altshuler LL, Abulseoud OA, Foland-Ross L, Bartzokis G, Chang S, Mintz J, Hellemann G, Vinters HV (2010) Amygdala astrocyte reduction in subjects with major depressive disorder but not bipolar disorder. Bipolar Disord 12(5):541–549. https://doi.org/10.1111/j.1399-5618.2010.00838.x
Aten S, Du Y, Taylor O, Dye C, Collins K, Thomas M, Kiyoshi C, Zhou M (2023) Chronic stress impairs the structure and function of astrocyte networks in an animal model of depression. Neurochem Res 48(4):1191–1210. https://doi.org/10.1007/s11064-022-03663-4
Autry AE, Adachi M, Nosyreva E, Na ES, Los MF, Cheng PF, Kavalali ET, Monteggia LM (2011) NMDA receptor blockade at rest triggers rapid behavioural antidepressant responses. Nature 475(7354):91–95. https://doi.org/10.1038/nature10130
Baeten KM, Akassoglou K (2011) Extracellular matrix and matrix receptors in blood–brain barrier formation and stroke. Dev Neurobiol 71(11):1018–1039. https://doi.org/10.1002/dneu.20954
Benarroch EE (2005) Neuron-astrocyte interactions: partnership for normal function and disease in the central nervous system. Mayo Clin Proc 80(10):1326–1338. https://doi.org/10.4065/80.10.1326
Bergami M, Rimondini R, Santi S, Blum R, Götz M, Canossa M (2008) Deletion of TrkB in adult progenitors alters newborn neuron integration into hippocampal circuits and increases anxiety-like behavior. Proc Natl Acad Sci USA 105(40):15570–15575. https://doi.org/10.1073/pnas.0803702105
Bose A, Basu R, Maulik M, Das Sarma J (2018) Loss of Cx43-mediated functional gap junction communication in meningeal fibroblasts following mouse hepatitis virus infection. Mol Neurobiol 55(8):6558–6571. https://doi.org/10.1007/s12035-017-0861-3
Bravo-Tobar ID, Fernández P, Sáez JC, Dagnino-Subiabre A (2021) Long-term effects of stress resilience: hippocampal neuroinflammation and behavioral approach in male rats. J Neurosci Res 99(10):2493–2510. https://doi.org/10.1002/jnr.24902
Carlen PL (2012) Curious and contradictory roles of glial connexins and pannexins in epilepsy. Brain Res 1487:54–60. https://doi.org/10.1016/j.brainres.2012.06.059
Chan SWY, Harmer CJ, Norbury R, O’sullivan U, Goodwin GM, Portella MJ (2016) Hippocampal volume in vulnerability and resilience to depression. J Affect Disord 189:199–202. https://doi.org/10.1016/j.jad.2015.09.021
Charveriat M, Mouthon F, Rein W, Verkhratsky A (2021) Connexins as therapeutic targets in neurological and neuropsychiatric disorders. Biochim Biophys Acta Mol Basis Dis 1867(5):166098. https://doi.org/10.1016/j.bbadis.2021.166098
Chavez CE, Oyarzun JE, Avendano BC, Mellado LA, Inostroza CA, Alvear TF, Orellana JA (2019) The opening of connexin 43 hemichannels alters hippocampal astrocyte function and neuronal survival in prenatally LPS-exposed adult offspring. Front Cell Neurosci 13:460. https://doi.org/10.3389/fncel.2019.00460
Chen J, Wang ZZ, Zuo W, Zhang S, Chu SF, Chen NH (2016) Effects of chronic mild stress on behavioral and neurobiological parameters—role of glucocorticoid. Horm Behav 78:150–159. https://doi.org/10.1016/j.yhbeh.2015.11.006
Cheslow L, Alvarez JI (2016) Glial-endothelial crosstalk regulates blood–brain barrier function. Curr Opin Pharmacol 26:39–46. https://doi.org/10.1016/j.coph.2015.09.010
Chever O, Pannasch U, Ezan P, Rouach N (2014) Astroglial connexin 43 sustains glutamatergic synaptic efficacy. Philos Trans R Soc Lond B Biol Sci 369(1654):20130596. https://doi.org/10.1098/rstb.2013.0596
Chew SS, Johnson CS, Green CR, Danesh-Meyer HV (2010) Role of connexin 43 in central nervous system injury. Exp Neurol 225(2):250–261. https://doi.org/10.1016/j.expneurol.2010.07.014
Cibelli A, Stout R, Timmermann A, De Menezes L, Guo P, Maass K, Seifert G, Steinhauser C, Spray DC, Scemes E (2021) Cx43 carboxyl terminal domain determines AQP4 and Cx30 endfoot organization and blood brain barrier permeability. Sci Rep. https://doi.org/10.1038/s41598-021-03694-x
Cobb JA, O’Neill K, Milner J, Mahajan GJ, Lawrence TJ, May WL, Miguel-Hidalgo J, Rajkowska G, Stockmeier CA (2016) Density of GFAP-immunoreactive astrocytes is decreased in left hippocampi in major depressive disorder. Neuroscience 316:209–220. https://doi.org/10.1016/j.neuroscience.2015.12.044
Cunha AB, Frey BN, Andreazza AC, Goi JD, Rosa AR, Gonçalves CA, Santin A, Kapczinski F (2006) Serum brain-derived neurotrophic factor is decreased in bipolar disorder during depressive and manic episodes. Neurosci Lett 398(3):215–219. https://doi.org/10.1016/j.neulet.2005.12.085
Czeh B, Di Benedetto B (2013) Antidepressants act directly on astrocytes: evidences and functional consequences. Eur Neuropsychopharmacol 23(3):171–185. https://doi.org/10.1016/j.euroneuro.2012.04.017
Dalton VS, Kolshus E, Mcloughlin DM (2014) Epigenetics and depression: return of the repressed. J Affect Disord 155:1–12. https://doi.org/10.1016/j.jad.2013.10.028
Daniele S, Zappelli E, Martini C (2015) Trazodone regulates neurotrophic/growth factors, mitogen-activated protein kinases and lactate release in human primary astrocytes. J Neuroinflamm 12:225. https://doi.org/10.1186/s12974-015-0446-x
Davidson JO, Green CR, Bennet L, Nicholson LF, Danesh-Meyer H, O’carroll SJ, Gunn AJ (2013) A key role for connexin hemichannels in spreading ischemic brain injury. Curr Drug Targets 14(1):36–46. https://doi.org/10.2174/138945013804806479
De Pitta M, Brunel N, Volterra A (2016) Astrocytes: orchestrating synaptic plasticity? Neuroscience 323:43–61. https://doi.org/10.1016/j.neuroscience.2015.04.001
Decrock E, De Bock M, Wang N, Bultynck G, Giaume C, Naus CC, Green CR, Leybaert L (2015) Connexin and pannexin signaling pathways, an architectural blueprint for CNS physiology and pathology? Cell Mol Life Sci 72(15):2823–2851. https://doi.org/10.1007/s00018-015-1962-7
Delvaeye T, Vandenabeele P, Bultynck G, Leybaert L, Krysko DV (2018) Therapeutic targeting of connexin channels: new views and challenges. Trends Mol Med 24(12):1036–1053. https://doi.org/10.1016/j.molmed.2018.10.005
Dong R, Han YQ, Jiang LH, Liu S, Zhang FJ, Peng LY, Wang ZM, Ma ZL, Xia TJ, Gu XP (2022) Connexin 43 gap junction-mediated astrocytic network reconstruction attenuates isoflurane-induced cognitive dysfunction in mice. J Neuroinflamm 19(1):64. https://doi.org/10.1186/s12974-022-02424-y
Dowlati Y, Herrmann N, Swardfager W, Liu H, Sham L, Reim EK, Lanctôt KL (2010) A meta-analysis of cytokines in major depression. Biol Psychiatry 67(5):446–457. https://doi.org/10.1016/j.biopsych.2009.09.033
Dupont AC, Guilloteau D, Kassiou M, Ribeiro MJ, Vercouillie J, Katsifis A, Arlicot N (2016) Radiopharmaceuticals for PET imaging of neuroinflammation. Med Nucl 40(1):72–81. https://doi.org/10.1016/j.mednuc.2016.01.001
Dwivedi Y (2010) Brain-derived neurotrophic factor and suicide pathogenesis. Ann Med 42(2):87–96. https://doi.org/10.3109/07853890903485730
Enache D, Pariante CM, Mondelli V (2019) Markers of central inflammation in major depressive disorder: a systematic review and meta-analysis of studies examining cerebrospinal fluid, positron emission tomography and post-mortem brain tissue. Brain Behav Immun 81:24–40. https://doi.org/10.1016/j.bbi.2019.06.015
Ezan P, Andre P, Cisternino S, Saubamea B, Boulay AC, Doutremer S, Thomas MA, Quenech’du N, Giaume C, Cohen-Salmon M (2012) Deletion of astroglial connexins weakens the blood–brain barrier. J Cereb Blood Flow Metab 32(8):1457–1467. https://doi.org/10.1038/jcbfm.2012.45
Fatemi SH, Folsom TD, Reutiman TJ, Lee S (2008a) Expression of astrocytic markers aquaporin 4 and connexin 43 is altered in brains of subjects with autism. Synapse 62(7):501–507. https://doi.org/10.1002/syn.20519
Fatemi SH, Folsom TD, Reutiman TJ, Pandian T, Braun NN, Haug K (2008b) Chronic psychotropic drug treatment causes differential expression of connexin 43 and GFAP in frontal cortex of rats. Schizophr Res 104(1–3):127–134. https://doi.org/10.1016/j.schres.2008.05.016
Faustmann PM, Haase CG, Romberg S, Hinkerohe D, Szlachta D, Smikalla D, Krause D, Dermietzel R (2003) Microglia activation influences dye coupling and Cx43 expression of the astrocytic network. Glia 42(2):101–108. https://doi.org/10.1002/glia.10141
Froger N, Orellana JA, Cohen-Salmon M, Ezan P, Amigou E, Saez JC, Giaume C (2009) Cannabinoids prevent the opposite regulation of astroglial connexin43 hemichannels and gap junction channels induced by pro-inflammatory treatments. J Neurochem 111(6):1383–1397. https://doi.org/10.1111/j.1471-4159.2009.06407.x
Froger N, Orellana JA, Calvo CF, Amigou E, Kozoriz MG, Naus CC, Saez JC, Giaume C (2010) Inhibition of cytokine-induced connexin 43 hemichannel activity in astrocytes is neuroprotective. Mol Cell Neurosci 45(1):37–46. https://doi.org/10.1016/j.mcn.2010.05.007
Fukuyama K, Okada M (2021) Effects of atypical antipsychotics, clozapine, quetiapine and brexpiprazole on astroglial transmission associated with connexin 43. Int J Mol Sci. https://doi.org/10.3390/ijms22115623
Fukuyama K, Motomura E, Shiroyama T, Okada M (2022) Impact of 5-HT7 receptor inverse agonism of lurasidone on monoaminergic tripartite synaptic transmission and pathophysiology of lower risk of weight gain. Biomed Pharmacother. https://doi.org/10.1016/j.biopha.2022.112750
García-García ML, Tovilla-Zárate CA, Villar-Soto M, Juárez-Rojop IE, González-Castro TB, Genis-Mendoza AD, Ramos-Méndez M, López-Nárvaez ML, Saucedo-Osti AS, Ruiz-Quiñones JA, Martinez-Magaña JJ (2022) Fluoxetine modulates the pro-inflammatory process of IL-6, IL-1β and TNF-α levels in individuals with depression: a systematic review and meta-analysis. Psychiatry Res 307:114317. https://doi.org/10.1016/j.psychres.2021.114317
Grippo AJ, Moffitt JA, Henry MK, Firkins R, Senkler J, Mcneal N, Wardwell J, MaL S, Dotson A, Schultz R (2015) Altered connexin 43 and connexin 45 protein expression in the heart as a function of social and environmental stress in the prairie vole. Stress 18(1):107–114. https://doi.org/10.3109/10253890.2014.979785
Guo A, Zhang H, Li H, Chiu A, García-Rodríguez C, Lagos CF, Sáez JC, Lau CG (2022) Inhibition of connexin hemichannels alleviates neuroinflammation and hyperexcitability in temporal lobe epilepsy. Proc Natl Acad Sci USA 119(45):e2213162119. https://doi.org/10.1073/pnas.2213162119
Hanani M, Verkhratsky A (2021) Satellite glial cells and astrocytes, a comparative review. Neurochem Res 46(10):2525–2537. https://doi.org/10.1007/s11064-021-03255-8
Hao T, Du X, Yang S, Zhang Y, Liang F (2020) Astrocytes-induced neuronal inhibition contributes to depressive-like behaviors during chronic stress. Life Sci 258:118099. https://doi.org/10.1016/j.lfs.2020.118099
Haroon E, Miller AH, Sanacora G (2017) Inflammation, glutamate, and glia: a trio of trouble in mood disorders. Neuropsychopharmacology 42(1):193–215. https://doi.org/10.1038/npp.2016.199
Hendriksen E, Van Bergeijk D, Oosting RS, Redegeld FA (2017) Mast cells in neuroinflammation and brain disorders. Neurosci Biobehav Rev 79:119–133. https://doi.org/10.1016/j.neubiorev.2017.05.001
Hinkerohe D, Smikalla D, Haghikia A, Heupel K, Haase CG, Dermietzel R, Faustmann PM (2005) Effects of cytokines on microglial phenotypes and astroglial coupling in an inflammatory coculture model. Glia 52(2):85–97. https://doi.org/10.1002/glia.20223
Hisaoka-Nakashima K, Kajitani N, Kaneko M, Shigetou T, Kasai M, Matsumoto C, Yokoe T, Azuma H, Takebayashi M, Morioka N, Nakata Y (2016) Amitriptyline induces brain-derived neurotrophic factor (BDNF) mRNA expression through ERK-dependent modulation of multiple BDNF mRNA variants in primary cultured rat cortical astrocytes and microglia. Brain Res 1634:57–67. https://doi.org/10.1016/j.brainres.2015.12.057
Hsieh CR, Qin XZ (2018) Depression hurts, depression costs: the medical spending attributable to depression and depressive symptoms in China. Health Econ 27(3):525–544. https://doi.org/10.1002/hec.3604
Hu HM, Li B, Wang XD, Guo YS, Hui H, Zhang HP, Wang B, Huang DG, Hao DJ (2018) Fluoxetine is neuroprotective in early brain injury via its anti-inflammatory and anti-apoptotic effects in a rat experimental subarachnoid hemorrhage model. Neurosci Bull 34(6):951–962. https://doi.org/10.1007/s12264-018-0232-8
Huang D, Li C, Zhang W, Qin J, Jiang W, Hu C (2019) Dysfunction of astrocytic connexins 30 and 43 in the medial prefrontal cortex and hippocampus mediates depressive-like behaviours. Behav Brain Res 372:111950. https://doi.org/10.1016/j.bbr.2019.111950
Hueston CM, Deak T (2020) Corticosterone and progesterone differentially regulate HPA axis and neuroimmune responses to stress in male rats. Stress 23(4):368–385. https://doi.org/10.1080/10253890.2019.1678025
Hurley LL, Tizabi Y (2013) Neuroinflammation, neurodegeneration, and depression. Neurotox Res 23(2):131–144. https://doi.org/10.1007/s12640-012-9348-1
Ishii K, Kubo KI, Nakajima K (2016) Reelin and neuropsychiatric disorders. Front Cell Neurosci 10:229. https://doi.org/10.3389/fncel.2016.00229
Iwata M, Shirayama Y, Ishida H, Hazama GI, Nakagome K (2011) Hippocampal astrocytes are necessary for antidepressant treatment of learned helplessness rats. Hippocampus 21(8):877–884. https://doi.org/10.1002/hipo.20803
Jeanson T, Pondaven A, Ezan P, Mouthon F, Charvériat M, Giaume C (2015) Antidepressants impact connexin 43 channel functions in astrocytes. Front Cell Neurosci 9:495. https://doi.org/10.3389/fncel.2015.00495
Ji RR, Xu ZZ, Gao YJ (2014) Emerging targets in neuroinflammation-driven chronic pain. Nat Rev Drug Discov 13(7):533–548. https://doi.org/10.1038/nrd4334
Jia X, Gao Z, Hu H (2021) Microglia in depression: current perspectives. Sci China Life Sci 64(6):911–925. https://doi.org/10.1007/s11427-020-1815-6
Kadriu B, Musazzi L, Henter ID, Graves M, Popoli M, Zarate CA Jr (2019) Glutamatergic neurotransmission: pathway to developing novel rapid-acting antidepressant treatments. Int J Neuropsychopharmacol 22(2):119–135. https://doi.org/10.1093/ijnp/pyy094
Kandouz M, Batist G (2010) Gap junctions and connexins as therapeutic targets in cancer. Expert Opin Ther Targets 14(7):681–692. https://doi.org/10.1517/14728222.2010.487866
Kielian T (2008) Glial connexins and gap junctions in CNS inflammation and disease. J Neurochem 106(3):1000–1016. https://doi.org/10.1111/j.1471-4159.2008.05405.x
Kim JW, Monteggia LM (2020) Increasing doses of ketamine curtail antidepressant responses and suppress associated synaptic signaling pathways. Behav Brain Res 380:112378. https://doi.org/10.1016/j.bbr.2019.112378
Kim Y, Davidson JO, Gunn KC, Phillips AR, Green CR, Gunn AJ (2016a) Role of hemichannels in CNS inflammation and the inflammasome pathway. Adv Protein Chem Struct Biol 104:1–37. https://doi.org/10.1016/bs.apcsb.2015.12.001
Kim YK, Na KS, Myint AM, Leonard BE (2016b) The role of pro-inflammatory cytokines in neuroinflammation, neurogenesis and the neuroendocrine system in major depression. Prog Neuropsychopharmacol Biol Psychiatry 64:277–284. https://doi.org/10.1016/j.pnpbp.2015.06.008
Kim Y, Griffin JM, Nor MNM, Zhang J, Freestone PS, Danesh-Meyer HV, Rupenthal ID, Acosta M, Nicholson LFB, O’carroll SJ, Green CR (2017) Tonabersat prevents inflammatory damage in the central nervous system by blocking connexin 43 hemichannels. Neurotherapeutics 14(4):1148–1165. https://doi.org/10.1007/s13311-017-0536-9
Kinoshita M, Hirayama Y, Fujishita K, Shibata K, Shinozaki Y, Shigetomi E, Takeda A, Le HPN, Hayashi H, Hiasa M, Moriyama Y, Ikenaka K, Tanaka KF, Koizumi S (2018) Anti-depressant fluoxetine reveals its therapeutic effect via astrocytes. EBioMedicine 32:72–83. https://doi.org/10.1016/j.ebiom.2018.05.036
Kohler O, Krogh J, Mors O, Benros ME (2016) Inflammation in depression and the potential for anti-inflammatory treatment. Curr Neuropharmacol 14(7):732–742. https://doi.org/10.2174/1570159x14666151208113700
Koo JW, Duman RS (2009) Evidence for IL-1 receptor blockade as a therapeutic strategy for the treatment of depression. Curr Opin Investig Drugs 10(7):664–671
Kuno R, Wang J, Kawanokuchi J, Takeuchi H, Mizuno T, Suzumura A (2005) Autocrine activation of microglia by tumor necrosis factor-alpha. J Neuroimmunol 162(1–2):89–96. https://doi.org/10.1016/j.jneuroim.2005.01.015
Kunugi H, Hori H, Adachi N, Numakawa T (2010) Interface between hypothalamic–pituitary–adrenal axis and brain-derived neurotrophic factor in depression. Psychiatry Clin Neurosci 64(5):447–459. https://doi.org/10.1111/j.1440-1819.2010.02135.x
Ledford H (2014) Medical research: if depression were cancer. Nature 515(7526):182–184. https://doi.org/10.1038/515182a
Lee BH, Kim H, Park SH, Kim YK (2007) Decreased plasma BDNF level in depressive patients. J Affect Disord 101(1–3):239–244. https://doi.org/10.1016/j.jad.2006.11.005
Lee JY, Lee HE, Kang SR, Choi HY, Ryu JH, Yune TY (2014) Fluoxetine inhibits transient global ischemia-induced hippocampal neuronal death and memory impairment by preventing blood-brain barrier disruption. Neuropharmacology 79:161–171. https://doi.org/10.1016/j.neuropharm.2013.11.011
Leng L, Zhuang K, Liu Z, Huang C, Gao Y, Chen G, Lin H, Hu Y, Wu D, Shi M, Xie W, Sun H, Shao Z, Li H, Zhang K, Mo W, Huang TY, Xue M, Yuan Z, Zhang X, Bu G, Xu H, Xu Q, Zhang J (2018) Menin deficiency leads to depressive-like behaviors in mice by modulating astrocyte-mediated neuroinflammation. Neuron 100(3):551-563.e557. https://doi.org/10.1016/j.neuron.2018.08.031
Li SH, Wang LT, Deng X, Jiao YN, Kong L, Fu M, Jia LQ, Yang JX, Ren L (2018) Electroacupuncture rescued the impairment of hippocampal neurons in perimenopausal depression rats via activating the CREB/BDNF pathway. Int J Pharmacol 14(2):164–178. https://doi.org/10.3923/ijp.2018.164.178
Li DY, Liu XY, Liu TM, Liu HT, Tong L, Jia SW, Wang YF (2020) Neurochemical regulation of the expression and function of glial fibrillary acidic protein in astrocytes. Glia 68(5):878–897. https://doi.org/10.1002/glia.23734
Liang Z, Wang X, Hao YL, Qiu L, Lou YY, Zhang YT, Ma D, Feng JC (2020) The multifaceted role of astrocyte connexin 43 in ischemic stroke through forming hemichannels and gap junctions. Front Neurol 11:703. https://doi.org/10.3389/fneur.2020.00703
Lin PY, Ma ZZ, Mahgoub M, Kavalali ET, Monteggia LM (2021) A synaptic locus for TrkB signaling underlying ketamine rapid antidepressant action. Cell Rep 36(7):109513. https://doi.org/10.1016/j.celrep.2021.109513
Liu XH, Gangoso E, Yi CJ, Jeanson T, Kandelman S, Mantz J, Giaume C (2016) General anesthetics have differential inhibitory effects on gap junction channels and hemichannels in astrocytes and neurons. Glia 64(4):524–536. https://doi.org/10.1002/glia.22946
Loebel A, Cucchiaro J, Silva R, Kroger H, Sarma K, Xu J, Calabrese JR (2014) Lurasidone as adjunctive therapy with lithium or valproate for the treatment of bipolar I depression: a randomized, double-blind, placebo-controlled study. Am J Psychiatry 171(2):169–177. https://doi.org/10.1176/appi.ajp.2013.13070985
Lommatzsch M, Hornych K, Zingler C, Schuff-Werner P, Hoppner J, Virchow JC (2006) Materna serum concentrations of BDNF and depression in the perinatal period. Psychoneuroendocrinology 31(3):388–394. https://doi.org/10.1016/j.psyneuen.2005.09.003
Lou YX, Li J, Wang ZZ, Xia CY, Chen NH (2018) Glucocorticoid receptor activation induces decrease of hippocampal astrocyte number in rats. Psychopharmacology (berlin) 235(9):2529–2540. https://doi.org/10.1007/s00213-018-4936-2
Maes M, Yirmyia R, Noraberg J, Brene S, Hibbeln J, Perini G, Kubera M, Bob P, Lerer B, Maj M (2009) The inflammatory & neurodegenerative (I&ND) hypothesis of depression: leads for future research and new drug developments in depression. Metab Brain Dis 24(1):27–53. https://doi.org/10.1007/s11011-008-9118-1
Mahmoud S, Gharagozloo M, Simard C, Amrani A, Gris D (2019) NLRX1 enhances glutamate uptake and inhibits glutamate release by astrocytes. Cells 8(5):400. https://doi.org/10.3390/cells8050400
Maturana CJ, Aguirre A, Sáez JC (2017) High glucocorticoid levels during gestation activate the inflammasome in hippocampal oligodendrocytes of the offspring. Dev Neurobiol 77(5):625–642. https://doi.org/10.1002/dneu.22409
Mazaud D, Capano A, Rouach N (2021) The many ways astroglial connexins regulate neurotransmission and behavior. Glia 69(11):2527–2545. https://doi.org/10.1002/glia.24040
Mechawar N, Savitz J (2016) Neuropathology of mood disorders: do we see the stigmata of inflammation? Transl Psychiatry 6(11):e946. https://doi.org/10.1038/tp.2016.212
Mesnil M, Defamie N, Naus C, Sarrouilhe D (2020) Brain disorders and chemical pollutants: a gap junction link? Biomolecules 11(1):51. https://doi.org/10.3390/biom11010051
Miguel-Hidalgo JJ (2022) Astroglia in the vulnerability to and maintenance of stress-mediated neuropathology and depression. Front Cell Neurosci 16:869779. https://doi.org/10.3389/fncel.2022.869779
Mitterauer BJ (2012) Ketamine may block NMDA receptors in astrocytes causing a rapid antidepressant effect. Front Synaptic Neurosci 4:8. https://doi.org/10.3389/fnsyn.2012.00008
Molofsky AV, Deneen B (2015) Astrocyte development: a guide for the perplexed. Glia 63(8):1320–1329. https://doi.org/10.1002/glia.22836
Morioka N, Suekama K, Zhang FF, Kajitani N, Hisaoka-Nakashima K, Takebayashi M, Nakata Y (2014) Amitriptyline up-regulates connexin 43-gap junction in rat cultured cortical astrocytes via activation of the p38 and c-Fos/AP-1 signalling pathway. Br J Pharmacol 171(11):2854–2867. https://doi.org/10.1111/bph.12614
Morioka N, Kondo S, Harada N, Takimoto T, Tokunaga N, Nakamura Y, Hisaoka-Nakashima K, Nakata Y (2021a) Downregulation of connexin 43 potentiates noradrenaline-induced expression of brain-derived neurotrophic factor in primary cultured cortical astrocytes. J Cell Physiol 236(10):6777–6792. https://doi.org/10.1002/jcp.30353
Morioka N, Kondo S, Takimoto T, Tokunaga N, Nakamura Y, Hisaoka-Nakashima K (2021b) Decreased connexin 43 expression in the hippocampus is related to the antidepressant effect of amitriptyline in neuropathic pain mice. Biochem Biophys Res Commun 566:141–147. https://doi.org/10.1016/j.bbrc.2021.06.020
Mostafavi H, Khaksarian M, Joghataei MT, Hassanzadeh G, Soleimani M, Eftekhari S, Soleimani M, Mousavizadeh K, Hadjighassem MR (2014) Fluoxetin upregulates connexin 43 expression in astrocyte. Basic Clin Neurosci 5(1):74–79
Musazzi L, Treccani G, Mallei A, Popoli M (2013) The action of antidepressants on the glutamate system: regulation of glutamate release and glutamate receptors. Biol Psychiatry 73(12):1180–1188. https://doi.org/10.1016/j.biopsych.2012.11.009
Nagy C, Suderman M, Yang J, Szyf M, Mechawar N, Ernst C, Turecki G (2015) Astrocytic abnormalities and global DNA methylation patterns in depression and suicide. Mol Psychiatry 20(3):320–328. https://doi.org/10.1038/mp.2014.21
Nagy C, Torres-Platas SG, Mechawar N, Turecki G (2017) Repression of astrocytic connexins in cortical and subcortical brain regions and prefrontal enrichment of H3K9me3 in depression and suicide. Int J Neuropsychopharmacol 20(1):50–57. https://doi.org/10.1093/ijnp/pyw071
Navinés R, Oriolo G, Horrillo I, Cavero M, Aouizerate B, Schaefer M, Capuron L, Meana JJ, Martin-Santos R (2022) High S100B levels predict antidepressant response in patients with major depression even when considering inflammatory and metabolic markers. Int J Neuropsychopharmacol 25(6):468–478. https://doi.org/10.1093/ijnp/pyac016
Neumeister A, Wood S, Bonne O, Nugent AC, Luckenbaugh DA, Young T, Bain EE, Charney DS, Drevets WC (2005) Reduced hippocampal volume in unmedicated, remitted patients with major depression versus control subjects. Biol Psychiatry 57(8):935–937. https://doi.org/10.1016/j.biopsych.2005.01.016
Norden DM, Fenn AM, Dugan A, Godbout JP (2014) TGFβ produced by IL-10 redirected astrocytes attenuates microglial activation. Glia 62(6):881–895. https://doi.org/10.1002/glia.22647
O’leary LA, Mechawar N (2021) Implication of cerebral astrocytes in major depression: a review of fine neuroanatomical evidence in humans. Glia 69(9):2077–2099. https://doi.org/10.1002/glia.23994
O’leary LA, Davoli MA, Belliveau C, Tanti A, Ma JC, Farmer WT, Turecki G, Murai KK, Mechawar N (2020) Characterization of vimentin-immunoreactive astrocytes in the human brain. Front Neuroanat 14:31. https://doi.org/10.3389/fnana.2020.00031
Okada M, Fukuyama K, Shiroyama T, Murata M (2020) A working hypothesis regarding identical pathomechanisms between clinical efficacy and adverse reaction of clozapine via the activation of connexin 43. Int J Mol Sci 21(19):7019. https://doi.org/10.3390/ijms21197019
Okada M, Oka T, Nakamoto M, Fukuyama K, Shiroyama T (2021) Astroglial connexin 43 as a potential target for a mood stabiliser. Int J Mol Sci 22(1):339. https://doi.org/10.3390/ijms22010339
Orellana JA, Moraga-Amaro R, Díaz-Galarce R, Rojas S, Maturana CJ, Stehberg J, Sáez JC (2015) Restraint stress increases hemichannel activity in hippocampal glial cells and neurons. Front Cell Neurosci 9:102. https://doi.org/10.3389/fncel.2015.00102
Pál B (2018) Involvement of extrasynaptic glutamate in physiological and pathophysiological changes of neuronal excitability. Cell Mol Life Sci 75(16):2917–2949. https://doi.org/10.1007/s00018-018-2837-5
Peng L, Verkhratsky A, Gu L, Li BM (2015) Targeting astrocytes in major depression. Expert Rev Neurother 15(11):1299–1306. https://doi.org/10.1586/14737175.2015.1095094
Pisu MG, Garau A, Boero G, Biggio F, Pibiri V, Dore R, Locci V, Paci E, Porcu P, Serra M (2016) Sex differences in the outcome of juvenile social isolation on HPA axis function in rats. Neuroscience 320:172–182. https://doi.org/10.1016/j.neuroscience.2016.02.009
Pogoda K, Kameritsch P, Retamal MA, Vega JL (2016) Regulation of gap junction channels and hemichannels by phosphorylation and redox changes: a revision. BMC Cell Biol 17 Suppl 1(Suppl 1):11. https://doi.org/10.1186/s12860-016-0099-3
Politynska B, Pokorska O, Wojtukiewicz AM, Sawicka M, Mysliwiec M, Honn KV, Tucker SC, Wojtukiewicz MZ (2022) Is depression the missing link between inflammatory mediators and cancer? Pharmacol Ther 240:108293. https://doi.org/10.1016/j.pharmthera.2022.108293
Quesseveur G, David DJ, Gaillard MC, Pla P, Wu MV, Nguyen HT, Nicolas V, Auregan G, David I, Dranovsky A, Hantraye P, Hen R, Gardier AM, Déglon N, Guiard BP (2013) BDNF overexpression in mouse hippocampal astrocytes promotes local neurogenesis and elicits anxiolytic-like activities. Transl Psychiatry 3:e253. https://doi.org/10.1038/tp.2013.30
Quesseveur G, Portal B, Basile JA, Ezan P, Mathou A, Halley H, Leloup C, Fioramonti X, Déglon N, Giaume C, Rampon C, Guiard BP (2015) Attenuated levels of hippocampal connexin 43 and its phosphorylation correlate with antidepressant- and anxiolytic-like activities in mice. Front Cell Neurosci 9:490. https://doi.org/10.3389/fncel.2015.00490
Rahimian R, Belliveau C, Chen R, Mechawar N (2022) Microglial inflammatory-metabolic pathways and their potential therapeutic implication in major depressive disorder. Front Psychiatry 13:871997. https://doi.org/10.3389/fpsyt.2022.871997
Rajkowska G, Stockmeier CA (2013) Astrocyte pathology in major depressive disorder: insights from human postmortem brain tissue. Curr Drug Targets 14(11):1225–1236. https://doi.org/10.2174/13894501113149990156
Ren Q, Wang ZZ, Chu SF, Xia CY, Chen NH (2018) Gap junction channels as potential targets for the treatment of major depressive disorder. Psychopharmacology 235(1):1–12. https://doi.org/10.1007/s00213-017-4782-7
Retamal MA, Froger N, Palacios-Prado N, Ezan P, Sáez PJ, Sáez JC, Giaume C (2007) Cx43 hemichannels and gap junction channels in astrocytes are regulated oppositely by proinflammatory cytokines released from activated microglia. J Neurosci 27(50):13781–13792. https://doi.org/10.1523/jneurosci.2042-07.2007
Rogóż Z, Kamińska K, Pańczyszyn-Trzewik P, Sowa-Kućma M (2017) Repeated co-treatment with antidepressants and risperidone increases BDNF mRNA and protein levels in rats. Pharmacol Rep 69(5):885–893. https://doi.org/10.1016/j.pharep.2017.02.022
Rouach N, Glowinski J, Giaume C (2000) Activity-dependent neuronal control of gap-junctional communication in astrocytes. J Cell Biol 149(7):1513–1526. https://doi.org/10.1083/jcb.149.7.1513
Rouach N, Calvo CF, Glowinski J, Giaume C (2002) Brain macrophages inhibit gap junctional communication and downregulate connexin 43 expression in cultured astrocytes. Eur J Neurosci 15(2):403–407. https://doi.org/10.1046/j.0953-816x.2001.01868.x
Rouach N, Koulakoff A, Giaume C (2004) Neurons set the tone of gap junctional communication in astrocytic networks. Neurochem Int 45(2–3):265–272. https://doi.org/10.1016/j.neuint.2003.07.004
Sáez JC, Leybaert L (2014) Hunting for connexin hemichannels. FEBS Lett 588(8):1205–1211. https://doi.org/10.1016/j.febslet.2014.03.004
Sáez JC, Berthoud VM, Branes MC, Martinez AD, Beyer EC (2003) Plasma membrane channels formed by connexins: their regulation and functions. Physiol Rev 83(4):1359–1400. https://doi.org/10.1152/physrev.00007.2003
Saggini A, Tripodi D, Maccauro G, Castellani ML, Anogeianaki A, Tete S, Felaco P, De Lutiis MA, Galzio R, Fulcheri M, Theoharides TC, Caraffa A, Antinolfi P, Felaco M, Conti F, Neri G, Pandolfi F, Toniato E, Shaik-Dasthagirisaheb YB (2011) Tumor necrosis factor-alpha and mast cells revisited study. Eur J Inflamm 9(1):17–22. https://doi.org/10.1177/1721727x1100900103
Sarrouilhe D, Dejean C, Mesnil M (2017) Connexin43-and pannexin-based channels in neuroinflammation and cerebral neuropathies. Front Mol Neurosci 10:320. https://doi.org/10.3389/fnmol.2017.00320
Sarrouilhe D, Defamie N, Mesnil M (2021) Is the exposome involved in brain disorders through the serotoninergic system? Biomedicines 9(10):1351. https://doi.org/10.3390/biomedicines9101351
Schroeder M, Krebs MO, Bleich S, Frieling H (2010) Epigenetics and depression: current challenges and new therapeutic options. Curr Opin Psychiatry 23(6):588–592. https://doi.org/10.1097/YCO.0b013e32833d16c1
Schroeter ML, Sacher J, Steiner J, Schoenknecht P, Mueller K (2013) Serum S100B represents a new biomarker for mood disorders. Curr Drug Targets 14(11):1237–1248. https://doi.org/10.2174/13894501113149990014
Severs NJ, Coppen SR, Dupont E, Yeh HI, Ko YS, Matsushita T (2004) Gap junction alterations in human cardiac disease. Cardiovasc Res 62(2):368–377. https://doi.org/10.1016/j.cardiores.2003.12.007
Shu Y, Zhu C, Zeng M, Zhan Q, Hu ZP, Wu XM (2019) The protective effect of carbenoxolone on gap junction damage in the hippocampal CA1 area of a temporal lobe epilepsy rat model. Ann Transl Med 7(22):624. https://doi.org/10.21037/atm.2019.11.04
Skaper SD (2017) Impact of inflammation on the blood-neural barrier and blood-nerve interface: from review to therapeutic preview. Int Rev Neurobiol 137:29–45. https://doi.org/10.1016/bs.irn.2017.08.004
Son H, Baek JH, Go BS, Jung DH, Sontakke SB, Chung HJ, Lee DH, Roh GS, Kang SS, Cho GJ, Choi WS, Lee DK, Kim HJ (2018) Glutamine has antidepressive effects through increments of glutamate and glutamine levels and glutamatergic activity in the medial prefrontal cortex. Neuropharmacology 143:143–152. https://doi.org/10.1016/j.neuropharm.2018.09.040
Stamatovic SM, Johnson AM, Keep RF, Andjelkovic AV (2016) Junctional proteins of the blood–brain barrier: new insights into function and dysfunction. Tissue Barriers 4(1):e1154641. https://doi.org/10.1080/21688370.2016.1154641
Stehberg J, Moraga-Amaro R, Salazar C, Becerra A, Echeverria C, Orellana JA, Bultynck G, Ponsaerts R, Leybaert L, Simon F, Saez JC, Retamal MA (2012) Release of gliotransmitters through astroglial connexin 43 hemichannels is necessary for fear memory consolidation in the basolateral amygdala. FASEB J 26(9):3649–3657. https://doi.org/10.1096/fj.11-198416
Stenovec M (2021) Ketamine alters functional plasticity of astroglia: an Implication for antidepressant effect. Life-Basel 11(6):573. https://doi.org/10.3390/life11060573
Sun JD, Liu Y, Yuan YH, Li J, Chen NH (2012) Gap junction dysfunction in the prefrontal cortex induces depressive-like behaviors in rats. Neuropsychopharmacology 37(5):1305–1320. https://doi.org/10.1038/npp.2011.319
Takeuchi H, Jin S, Wang J, Zhang G, Kawanokuchi J, Kuno R, Sonobe Y, Mizuno T, Suzumura A (2006) Tumor necrosis factor-alpha induces neurotoxicity via glutamate release from hemichannels of activated microglia in an autocrine manner. J Biol Chem 281(30):21362–21368. https://doi.org/10.1074/jbc.M600504200
Tao S, Jia M, Qiu T (2019) Expression and role of CaMKII and Cx43 in a rat model of post-stroke depression. Exp Ther Med 18(3):2153–2159. https://doi.org/10.3892/etm.2019.7782
Tao XD, Liu ZR, Zhang YQ, Zhang XH (2021) Connexin 43 hemichannels contribute to working memory and excitatory synaptic transmission of pyramidal neurons in the prefrontal cortex of rats. Life Sci 286:120049. https://doi.org/10.1016/j.lfs.2021.120049
Tarasov VV, Svistunov AA, Chubarev VN, Sologova SS, Mukhortova P, Levushkin D, Somasundaram SG, Kirkland CE, Bachurin SO, Aliev G (2019) Alterations of astrocytes in the context of schizophrenic dementia. Front Pharmacol 10:1612. https://doi.org/10.3389/fphar.2019.01612
Tokunaga N, Takimoto T, Nakamura Y, Hisaoka-Nakashima K, Morioka N (2022) Downregulation of connexin 43 potentiates amitriptyline-induced brain-derived neurotrophic factor expression in primary astrocytes through lysophosphatidic acid receptor(1/3), Src, and extracellular signal-regulated kinase. Eur J Pharmacol 925:174986. https://doi.org/10.1016/j.ejphar.2022.174986
Torres-Platas SG, Nagy C, Wakid M, Turecki G, Mechawar N (2016) Glial fibrillary acidic protein is differentially expressed across cortical and subcortical regions in healthy brains and downregulated in the thalamus and caudate nucleus of depressed suicides. Mol Psychiatry 21(4):509–515. https://doi.org/10.1038/mp.2015.65
Touchant M, Labonte B (2022) Sex-specific brain transcriptional signatures in human MDD and their correlates in mouse models of depression. Front Behav Neurosci 16:845491. https://doi.org/10.3389/fnbeh.2022.845491
Turkheimer FE, Althubaity N, Schubert J, Nettis MA, Cousins O, Dima D, Mondelli V, Bullmore ET, Pariante C, Veronese M (2021) Increased serum peripheral C-reactive protein is associated with reduced brain barriers permeability of TSPO radioligands in healthy volunteers and depressed patients: implications for inflammation and depression. Brain Behav Immun 91:487–497. https://doi.org/10.1016/j.bbi.2020.10.025
Uchida S, Yamagata H, Seki T, Watanabe Y (2018) Epigenetic mechanisms of major depression: targeting neuronal plasticity. Psychiatry Clin Neurosci 72(4):212–227. https://doi.org/10.1111/pcn.12621
Wang Q, Jie W, Liu JH, Yang JM, Gao TM (2017) An astroglial basis of major depressive disorder? An overview. Glia 65(8):1227–1250. https://doi.org/10.1002/glia.23143
Wang BL, Chen XQ, Zhou TT, Wang XY (2018a) Antidepressant-like effects of embelin and its possible mechanisms of action in chronic unpredictable stress-induced mice. Neurol Res 40(8):666–676. https://doi.org/10.1080/01616412.2018.1460705
Wang Y, Xie L, Gao C, Zhai L, Zhang N, Guo L (2018b) Astrocytes activation contributes to the antidepressant-like effect of ketamine but not scopolamine. Pharmacol Biochem Behav 170:1–8. https://doi.org/10.1016/j.pbb.2018.05.001
Wang Y, Ni J, Zhai LY, Gao C, Xie LM, Zhao L, Yin XX (2019) Inhibition of activated astrocyte ameliorates lipopolysaccharide-induced depressive-like behaviors. J Affect Disord 242:52–59. https://doi.org/10.1016/j.jad.2018.08.015
Wang Y, Su Y, Yu G, Wang X, Chen X, Yu B, Cheng Y, Li R, Sáez JC, Yi C, Xiao L, Niu J (2021a) Reduced oligodendrocyte precursor cell impairs astrocytic development in early life stress. Adv Sci (weinh) 8(16):e2101181. https://doi.org/10.1002/advs.202101181
Wang YT, Wang XL, Feng ST, Chen NH, Wang ZZ, Zhang Y (2021b) Novel rapid-acting glutamatergic modulators: targeting the synaptic plasticity in depression. Pharmacol Res 171:105761. https://doi.org/10.1016/j.phrs.2021.105761
Wang YT, Zhang NN, Liu LJ, Jiang H, Hu D, Wang ZZ, Chen NH, Zhang Y (2022) Glutamatergic receptor and neuroplasticity in depression: implications for ketamine and rapastinel as the rapid-acting antidepressants. Biochem Biophys Res Commun 594:46–56. https://doi.org/10.1016/j.bbrc.2022.01.024
Wei Y, Xiao L, Fan WH, Zou J, Yang H, Liu B, Ye Y, Wen D, Liao LC (2022) Astrocyte activation, but not microglia, is associated with the experimental mouse model of schizophrenia induced by chronic ketamine. J Mol Neurosci 72(9):1902–1915. https://doi.org/10.1007/s12031-022-02046-2
Wu LY, Yu XL, Feng LY (2015) Connexin 43 stabilizes astrocytes in a stroke-like milieu to facilitate neuronal recovery. Acta Pharmacol Sin 36(8):928–938. https://doi.org/10.1038/aps.2015.39
Wu SS, Yin YY, Du LF (2022) Blood–brain barrier dysfunction in the pathogenesis of major depressive disorder. Cell Mol Neurobiol 42(8):2571–2591. https://doi.org/10.1007/s10571-021-01153-9
Xia CY, Chu SF, Zhang S, Gao Y, Ren Q, Lou YX, Luo P, Tian MT, Wang ZQ, Du GH, Tomioka Y, Yamakuni T, Zhang Y, Wang ZZ, Chen NH (2017) Ginsenoside Rg1 alleviates corticosterone-induced dysfunction of gap junctions in astrocytes. J Ethnopharmacol 208:207–213. https://doi.org/10.1016/j.jep.2017.06.031
Xia CY, Wang ZZ, Yamakuni T, Chen NH (2018a) A novel mechanism of depression: role for connexins. Eur Neuropsychopharmacol 28(4):483–498. https://doi.org/10.1016/j.euroneuro.2018.01.009
Xia CY, Wang ZZ, Zhang Z, Chen J, Wang YY, Lou YX, Gao Y, Luo P, Ren Q, Du GH, Chen NH (2018b) Corticosterone impairs gap junctions in the prefrontal cortical and hippocampal astrocytes via different mechanisms. Neuropharmacology 131:20–30. https://doi.org/10.1016/j.neuropharm.2017.12.003
Xia CY, Wang ZZ, Wang HQ, Ren SY, Lou YX, Jin C, Qu TG, Feng ST, Zhang Y, Chu SF, Chen NH (2020) Connexin 43: a novel ginsenoside Rg1-sensitive target in a rat model of depression. Neuropharmacology 170:108041. https://doi.org/10.1016/j.neuropharm.2020.108041
Xiao Q, Xu XR, Tu J (2020) Chronic optogenetic manipulation of basolateral amygdala astrocytes rescues stress-induced anxiety. Biochem Biophys Res Commun 533(4):657–664. https://doi.org/10.1016/j.bbrc.2020.09.106
Yang KL, Zhou Y, Zhou LQ, Yan FM, Guan L, Liu HM, Liu W (2020a) Synaptic plasticity after focal cerebral ischemia was attenuated by Gap26 but enhanced by GAP-134. Front Neurol 11:888. https://doi.org/10.3389/fneur.2020.00888
Yang T, Nie Z, Shu H, Kuang Y, Chen X, Cheng J, Yu S, Liu H (2020b) The role of BDNF on neural plasticity in depression. Front Cell Neurosci 14:82. https://doi.org/10.3389/fncel.2020.00082
Zeb S, Ye H, Liu Y, Du HP, Guo Y, Zhu YM, Ni Y, Zhang HL, Xu Y (2023) Necroptotic kinases are involved in the reduction of depression-induced astrocytes and fluoxetine’s inhibitory effects on necroptotic kinases. Front Pharmacol 13:1060954. https://doi.org/10.3389/fphar.2022.1060954
Zhang JC, Yao W, Hashimoto K (2016) Brain-derived neurotrophic factor (BDNF)-TrkB signaling in inflammation-related depression and potential therapeutic targets. Curr Neuropharmacol 14(7):721–731. https://doi.org/10.2174/1570159x14666160119094646
Zhang YP, Wang HY, Zhang C, Liu BP, Peng ZL, Li YY, Liu FM, Song C (2018) Mifepristone attenuates depression-like changes induced by chronic central administration of interleukin-1β in rats. Behav Brain Res 347:436–445. https://doi.org/10.1016/j.bbr.2018.03.033
Zhang XM, Wang LZ, He B, Xiang YK, Fan LX, Wang Q, Tao L (2019) The gap junction inhibitor INI-0602 attenuates mechanical allodynia and depression-like behaviors induced by spared nerve injury in rats. NeuroReport 30(5):369–377. https://doi.org/10.1097/wnr.0000000000001209
Zhang Y, Lu W, Wang Z, Zhang R, Xie Y, Guo S, Jiao L, Hong Y, Di Z, Wang G, Aa J (2020) Reduced neuronal cAMP in the nucleus accumbens damages blood–brain barrier integrity and promotes stress vulnerability. Biol Psychiatry 87(6):526–537. https://doi.org/10.1016/j.biopsych.2019.09.027
Zhang XL, Alnafisah RS, Hamoud ARA, Shukla R, Wen ZX, Mccullumsmith RE, O’donovan SM (2021) Role of astrocytes in major neuropsychiatric disorders. Neurochem Res 46(10):2715–2730. https://doi.org/10.1007/s11064-020-03212-x
Zhang NN, Zhang Y, Wang ZZ, Chen NH (2022a) Connexin 43: insights into candidate pathological mechanisms of depression and its implications in antidepressant therapy. Acta Pharmacol Sin 43(10):2448–2461. https://doi.org/10.1038/s41401-022-00861-2
Zhang YP, Li YY, Zhang C, Li YJ, Liu BP, Zhang Y, Lin JD, Song C (2022b) Interleukin-10 attenuates behavioral, immune and neurotrophin changes induced by chronic central administration of interleukin-1β in rats. NeuroImmunoModulation 29(4):380–390. https://doi.org/10.1159/000521710
Zhang NN, Jiang H, Wang HQ, Wang YT, Peng Y, Liu YB, Xia CY, Yan X, Chu SF, Zhang Y, Wang ZZ, Chen NH (2023) Novel antidepressant mechanism of ginsenoside Rg1 in regulating the dysfunction of the glutamatergic system in astrocytes. Int J Mol Sci 24(1):575. https://doi.org/10.3390/ijms24010575
Zhao Y, Lin Z, Chen L, Ouyang L, Gu L, Chen F, Zhang Q (2018) Hippocampal astrocyte atrophy in a mouse depression model induced by corticosterone is reversed by fluoxetine instead of benzodiazepine diazepam. Prog Neuropsychopharmacol Biol Psychiatry 83:99–109. https://doi.org/10.1016/j.pnpbp.2018.01.011
Zheng QL, Zhu HY, Xu X, Chu SF, Cui LY, Dong YX, Liu YJ, Zhan JH, Wang ZZ, Chen NH (2021) Korean red ginseng alleviate depressive disorder by improving astrocyte gap junction function. J Ethnopharmacol 281:114466. https://doi.org/10.1016/j.jep.2021.114466
Zhou SY, Chen R, She YL, Liu XJ, Zhao H, Li C, Jia YB (2022) A new perspective on depression and neuroinflammation: non-coding RNA. J Psychiatr Res 148:293–306. https://doi.org/10.1016/j.jpsychires.2022.02.007
Funding
This study was supported by National Natural Science Foundation of China (Grant Nos. 82274127 and 82104644).
Author information
Authors and Affiliations
Contributions
LL: Investigation, Methodology, Writing—original draft. Y-TW: Investigation; DH: Investigation; CG: Investigation; YZ: Conceptualization, Methodology, Supervision, Writing—review & editing.
Corresponding author
Ethics declarations
Competing interests
The authors have no competing interests to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lei, L., Wang, YT., Hu, D. et al. Astroglial Connexin 43-Mediated Gap Junctions and Hemichannels: Potential Antidepressant Mechanisms and the Link to Neuroinflammation. Cell Mol Neurobiol 43, 4023–4040 (2023). https://doi.org/10.1007/s10571-023-01426-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-023-01426-5