Abstract
Purpose
Extensive data in White women have linked oral contraceptive use, tubal ligation, and parity to reduced risk of ovarian cancer; results on postmenopausal female hormone use are mixed. Few studies, all of which are case–control studies, have been undertaken among Black women. The aim of the present study was to prospectively assess associations of reproductive factors and exogenous hormones with ovarian cancer among Black women.
Methods
During follow-up from 1995 to 2013 in the Black Women’s Health Study, a prospective cohort study, 115 incident cases of ovarian cancer were identified. Cox proportional hazards models were used to calculate hazard ratios (HRs) and 95% confidence intervals (CIs) for the relation of the factors of interest to risk of ovarian cancer, with control for covariates.
Result
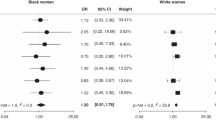
Oral contraceptive use was inversely associated with ovarian cancer risk: The HR for ≥10 years of use relative to <1 year was 0.50 (95% CI 0.30–0.98). For postmenopausal female hormone use, the HRs for ever use of estrogen with progestin and of estrogen alone were 1.37 (0.73–2.55) and 1.66 (0.90–3.07), respectively. The HRs for parity and tubal ligation were below 1.0, but were not statistically significant.
Conclusion
Overall, the findings indicate that the relation of reproductive factors and exogenous hormone use to risk of ovarian cancer is similar among Black and White women. The results on estrogen-only supplements and estrogen with progestin supplements add to evidence from Whites, indicating that use of hormone supplements may be associated with increased risk of ovarian cancer.
Similar content being viewed by others
References
Chumlea WC, Schubert CM, Roche AF et al (2003) Age at menarche and racial comparisons in US girls. Pediatrics 111:110–113
Martin JA, Osterman MJ, Centers for Disease C, Prevention (2013) Preterm births—United States, 2006 and 2010. MMWR Suppl. 62:136–138
Centers for Disease C, Prevention (2013) Progress in increasing breastfeeding and reducing racial/ethnic differences-United States, 2000–2008 births. MMWR Morb Mortal Wkly Rep 62:77–80
Daniels K, Mosher WD (2013) Contraceptive methods women have ever used: United States, 1982–2010. Natl Health Stat Report 62:1–15
Rice MS, Murphy MA, Tworoger SS (2012) Tubal ligation, hysterectomy and ovarian cancer: a meta-analysis. J Ovarian Res 5:13
McLemore MR, Miaskowski C, Aouizerat BE, Chen LM, Dodd MJ (2009) Epidemiological and genetic factors associated with ovarian cancer. Cancer Nurs. 32:281–288 quiz 9–90
Chowdhury R, Sinha B, Sankar MJ et al (2015) Breastfeeding and maternal health outcomes: a systematic review and meta-analysis. Acta Paediatr 104:96–113
Luan NN, Wu QJ, Gong TT, Vogtmann E, Wang YL, Lin B (2013) Breastfeeding and ovarian cancer risk: a meta-analysis of epidemiologic studies. Am J Clin Nutr 98:1020–1031
Wu AH, Pearce CL, Tseng CC, Pike MC (2015) African Americans and hispanics remain at lower risk of ovarian cancer than non-hispanic whites after considering nongenetic risk factors and oophorectomy rates. Cancer Epidemiol Biomark Prev 24:1094–1100
Terry KL, Karageorgi S, Shvetsov YB et al (2013) Genital powder use and risk of ovarian cancer: a pooled analysis of 8,525 cases and 9,859 controls. Cancer Prev Res (Phila) 6:811–821
Tsilidis KK, Allen NE, Key TJ et al (2011) Menopausal hormone therapy and risk of ovarian cancer in the European prospective investigation into cancer and nutrition. Cancer Causes Control 22:1075–1084
Lee AW, Ness RB, Roman LD et al (2016) Association between menopausal estrogen-only therapy and ovarian carcinoma risk. Obstet Gynecol 127:828–836
Trabert B, Wentzensen N, Yang HP et al (2012) Ovarian cancer and menopausal hormone therapy in the NIH-AARP diet and health study. Br J Cancer 107:1181–1187
John EM, Whittemore AS, Harris R, Itnyre J (1993) Characteristics relating to ovarian cancer risk: collaborative analysis of seven U.S. case–control studies. Epithelial ovarian cancer in black women. Collaborative Ovarian Cancer Group. J Natl Cancer Inst 85:142–147
Hoyo C, Berchuck A, Halabi S et al (2005) Anthropometric measurements and epithelial ovarian cancer risk in African–American and White women. Cancer Causes Control 16:955–963
Ness RB, Grisso JA, Klapper J, Vergona R (2000) Racial differences in ovarian cancer risk. J Natl Med Assoc 92:176–182
Moorman PG, Palmieri RT, Akushevich L, Berchuck A, Schildkraut JM (2009) Ovarian cancer risk factors in African-American and white women. Am J Epidemiol 170:598–606
Moorman PG, Alberg AJ, Bandera EV et al (2016) Reproductive factors and ovarian cancer risk in African-American women. Ann Epidemiol 26:654–662
Schildkraut JM, Alberg AJ, Bandera EV et al (2014) A multi-center population-based case–control study of ovarian cancer in African-American women: the African American Cancer Epidemiology Study (AACES). BMC Cancer 14:688
Rosenberg L, Adams-Campbell L, Palmer JR (1995) The Black Women’s Health Study: a follow-up study for causes and preventions of illness. J Am Med Womens Assoc 50:56–58
Rosenberg L, Palmer JR, Rao RS, Adams-Campbell LL (1999) Risk factors for coronary heart disease in African American women. Am J Epidemiol 150:904–909
NCHS (2013) National Death Index user’s guide. In: National Center for Health Statistics CfDCaP, U.S. Department of Health and Human Services, ed. Hyattsville, MD
Chen VW, Ruiz B, Killeen JL, Cote TR, Wu XC, Correa CN (2003) Pathology and classification of ovarian tumors. Cancer 97:2631–2642
Rosen DG, Yang G, Liu G et al (2009) Ovarian cancer: pathology, biology, and disease models. Front Biosci (Landmark Ed) 14:2089–2102
Carter-Nolan PL, Adams-Campbell LL, Makambi K, Lewis S, Palmer JR, Rosenberg L (2006) Validation of physical activity instruments: Black Women’s Health Study. Ethn Dis 16:943–947
Therneau TM (1996) Extending the Cox Model. Technical Report Series: Section of Biostatistics. Rochester, MN: Mayo Clinic. pp 1–63
Collaborative Group on Epidemiological Studies of Ovarian Cancer, Beral V, Doll R, Hermon C, Peto R, Reeves G (2008) Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45 epidemiological studies including 23,257 women with ovarian cancer and 87,303 controls. Lancet 371:303–314
Collaborative Group On Epidemiological Studies Of Ovarian Cancer, Beral V, Gaitskell K et al (2015) Menopausal hormone use and ovarian cancer risk: individual participant meta-analysis of 52 epidemiological studies. Lancet 385:1835–1842
Rice MS, Hankinson SE, Tworoger SS (2014) Tubal ligation, hysterectomy, unilateral oophorectomy, and risk of ovarian cancer in the Nurses’ Health Studies. Fertil Steril 102(192–8):e3
Rice MS, Murphy MA, Vitonis AF et al (2013) Tubal ligation, hysterectomy and epithelial ovarian cancer in the New England Case–Control Study. Int J Cancer 133:2415–2421
Gaitskell K, Green J, Pirie K, Reeves G, Beral V, Million Women Study C (2016) Tubal ligation and ovarian cancer risk in a large cohort: substantial variation by histological type. Int J Cancer 138:1076–1084
Ness RB, Grisso JA, Klapper J et al (2000) Risk of ovarian cancer in relation to estrogen and progestin dose and use characteristics of oral contraceptives. SHARE Study Group. Steroid Hormones and Reproductions. Am J Epidemiol 152:233–241
Schildkraut JM, Calingaert B, Marchbanks PA, Moorman PG, Rodriguez GC (2002) Impact of progestin and estrogen potency in oral contraceptives on ovarian cancer risk. J Natl Cancer Inst 94:32–38
Quirk JT, Natarajan N (2005) Ovarian cancer incidence in the United States 1992–1999. Gynecol Oncol 97:519–523
Gershenson DM (2013) The life and times of low-grade serous carcinoma of the ovary. Am Soc Clin Oncol Educ Book 33:e195–e199
Sieh W, Salvador S, McGuire V et al (2013) Tubal ligation and risk of ovarian cancer subtypes: a pooled analysis of case–control studies. Int J Epidemiol 42:579–589
Fortner RT, Ose J, Merritt MA et al (2015) Reproductive and hormone-related risk factors for epithelial ovarian cancer by histologic pathways, invasiveness and histologic subtypes: results from the EPIC cohort. Int J Cancer 137:1196–1208
Gaitskell K, Green J, Pirie K, Reeves G, Beral V (2014) Parity and ovarian cancer in the Million Women Study: variation by histological subtype. J Epidemiol Community Health 68:A15–A16
Acknowledgments
This research was supported by the National Cancer Institute of the National Institutes of Health (R01CA058420, UM1CA164974) and does not necessarily represent the views of the National Cancer Institute or the National Institutes of Health. Data on ovarian cancer cases were obtained from 24 state cancer registries (Arizona, California, Colorado, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, New Jersey, New York, North Carolina, Oklahoma, Pennsylvania, South Carolina, Tennessee, Texas, and Virginia), and these results do not necessarily represent their views. The authors gratefully acknowledge the BWHS participants and staff.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Bethea, T.N., Palmer, J.R., Adams-Campbell, L.L. et al. A prospective study of reproductive factors and exogenous hormone use in relation to ovarian cancer risk among Black women. Cancer Causes Control 28, 385–391 (2017). https://doi.org/10.1007/s10552-016-0840-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-016-0840-4