Abstract
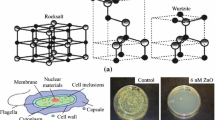
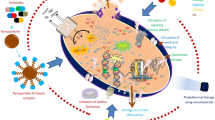
Rapidly growing mycobacteria (RGM) are pathogens that belong to the mycobacteriaceae family and responsible for causing mycobacterioses, which are infections of opportunistic nature and with increasing incidence rates in the world population. This work evaluated the use of six water-soluble cationic porphyrins as photosensitizers for the antimicrobial photodynamic therapy (aPDT) of four RGM strains: Mycolicibacterium fortuitum, Mycolicibacterium smeagmatis, Mycobacteroides abscessus subs. Abscessus, and Mycobacteroides abscessus subsp. massiliense. Experiments were conducted with an adequate concentration of photosensitizer under white-light irradiation conditions over 90 min and the results showed that porphyrins 1 and 2 (M = 2H or ZnII ion) were the most effective and significantly reduced the concentration of viable mycobacteria. The present work shows the result is dependent on the metal-center ion coordinated in the cationic porphyrin core. Moreover, we showed by atomic force microscopy (AFM) the possible membrane photodamage caused by reactive oxygen species and analyzed the morphology and adhesive force properties. Tetra-positively charged and water-soluble metalloporphyrins may be promising antimycobacterial aPDT agents with potential applications in medical clinical cases and bioremediation.





Similar content being viewed by others
Abbreviations
- MIC:
-
Minimum inhibitory concentration
- ROS:
-
Reactive oxygen species
- RGM:
-
Rapidly growing mycobacteria
- PS:
-
Photosensitizers
- aPDT:
-
Antimicrobial photodynamic therapy
- AFM:
-
Atomic force microscopy
- EFM:
-
Electrostatic force microscopy
- LJ:
-
Löwenstein-Jensen
- AA:
-
Ascorbic acid
- Man:
-
Mannitol
- KI:
-
Potassium iodide
- TTC:
-
2,3,5-Triphenyltetrazolium chloride
- M. fortuitum :
-
Mycolicibacterium fortuitum
- M. abscessus :
-
Mycobacteroides abscessus subs. abscessus
- M. massiliense :
-
Mycobacteroides abscessus subsp. massiliense
- M. smeagmatis :
-
Mycolicibacterium smeagmatis
References
Agertt VA, Bonez PC, Rossi GG, Flores VC, Siqueira FS, Mizdal CR, Marques LL, De Oliveira GM, Campos MMA (2016) Identification of antimicrobial activity among new sulfonamide metal complexes for combating rapidly growing mycobacteria. Biometals. https://doi.org/10.1007/s10534-016-9951-3
Almeida J, Tomé JPC, Neves MGPMS, Tomé AC, Cavaleiro JAS, Cunha A et al (2014) Photodynamic inactivation of multidrug-resistant bacteria in hospital wastewaters: influence of residual antibiotics. Photochem Photobiol Sci 13:626–633. https://doi.org/10.1039/c3pp50195g
Alves E, Faustino MAF, Tome JPC, Neves MGPMS, Tomé AC, Cavaleiro JAS et al (2011) Photodynamic antimicrobial chemotherapy in aquaculture: photoinactivation studies of Vibrio fischeri. PLoS ONE 6:e20970–e20979. https://doi.org/10.1371/journal.pone.0020970
Arredondo-Espinoza EU, López-Cortina ST, Ramírez-Cabrera MA, Balderas-Rentería I (2016) Synthesis and photodynamic activity of unsymmetrical A3B tetraarylporphyrins functionalized with l-glutamate and their Zn(II) and Cu(II) metal complex derivatives. Biomed Pharmacother 82:327–336. https://doi.org/10.1016/j.biopha.2016.05.010
Aung TT, Yam JKH, Lin S, Salleh SM, Givskov M, Liu S et al (2016) Biofilms of pathogenic nontuberculous mycobacteria targeted by new therapeutic approaches. Antimicrob Agents Chemother 60:24–35. https://doi.org/10.1128/AAC.01509-15
Bartolomeu M, Rocha S, Cunha Â, Neves MG, Faustino MA, Almeida A (2016) Effect photodynamic therapy on the virulence factors of Staphylococcus aureus. Front Microbiol 7:267–278. https://doi.org/10.3389/fmicb.2016.00267
Basso G, Cargnelutti JF, Oliveira AL, Acunha TV, Weiblen R, Flores EF et al (2019) Photodynamic inactivation of selected bovine viruses by isomeric cationic tetra-platinated porphyrins. Porphyrins Phthalocyanines 23:1041–1046. https://doi.org/10.1142/S1088424619500767
Batinić-Haberle I, Rebouças JS, Spasojević I (2010) Superoxide dismutase mimics: chemistry, pharmacology, and therapeutic potential. Antioxid Redox Sign 13:877–918. https://doi.org/10.1016/j.redox.2019.101139
Benov L, Batinić-Haberle I, Spasojević I, Fridovich I (2002) Isomeric N-alkylpyridylporphyrins and their Zn(II) complexes: inactive as SOD mimics but powerful photosensitizers. Arch Biochem Biophys 402:159–165. https://doi.org/10.1016/S0003-9861(02)00062-0
Brown-Elliott BA, Wallace RJ Jr, Crist CJ, Mann L, Wilson RW (2002) Comparison of in vitro activities of gatifloxacin and ciprofloxacin against four taxa of rapidly growing mycobacteria. Antimicrob Agents Chemother 46:3283–3285. https://doi.org/10.1128/aac.46.10.3283-3285.2002
Carmello JC, Alves F, Basso FG, Costa CAS, Tedesco AC, Lucas Primo F et al (2019) Antimicrobial photodynamic therapy reduces adhesion capacity and biofilm formation of Candida albicans from induced oral candidiasis in mice. Photodiagn Photodyn Ther 27:402–407. https://doi.org/10.1016/j.pdpdt.2019.06.010
Costa-Silve M, César A, Nuno PG, Azavedo F (2018) Mycobacterium abscessus infection in a spa worker. Acta Dermatovenerol Alp Pannonica Adriat 27:159–160. https://doi.org/10.15570/actaapa.2018.33
Couto GK, Pacheco BS, Borba VM, Junior JCR, Oliveira TL, Segatto NV et al (2020) Tetra-cationic platinum(II) porphyrins like a candidate photosensitizers to bind, selective and drug delivery for metastatic melanoma. J Photochem Photobiol B Biol 202:111725–111737. https://doi.org/10.1016/j.jphotobiol.2019.111725
da Silveira CH, Vieceli V, Clerici DJ, Santos RCV, Iglesias BA (2020) Investigation of isomeric tetra-cationic porphyrin activity with peripheral [Pd(bpy)Cl]+ units by antimicrobial photodynamic therapy. Photodiag Photodyn Ther 31:101920. https://doi.org/10.1016/j.pdpdt.2020.101920
Donlan RM, Costerton JW (2002) Biofilms: survival mechanisms of clinically relevant microorganisms. Clin Microbiol Rev 15:167–193. https://doi.org/10.15190/d.2019.13
Esteban J, Navas E (2018) Treatment of infections caused by nontuberculous mycobacteria. Enferm Infecc Microbiol Clin 36(9):586–592. https://doi.org/10.1016/j.eimc.2017.10.008
Ethirajan M, Chen P, Ohulchanskyy TY, Goswami LN, Gupta A, Srivatsan A et al (2013) Regioselective synthesis and photophysical and electrochemical studies of 20-substituted cyanine dye-purpurinimide conjugates: Incorporation of Ni II into the conjugate enhances its tumor-uptake and fluorescence-imaging ability. Chem Eur 19:6670–6684. https://doi.org/10.1002/chem.201203867
Flores VC, Siqueira FS, Mizdal CR, Bonez PC, Agertt VA, Stefanello ST et al (2016) Antibiofilm effect of antimicrobials used in the therapy of mycobacteriosis. Microb Pathog 99:229–235. https://doi.org/10.1016/j.micpath.2016.08.017
Follmann HDM, Martins AF, Gerola AP, Burgo TAL, Nakamura CV, Rubira AF et al (2012) Antiadhesive and antibacterial multilayer films via layer-by-layer assembly of TMC/heparin complexes. Biomacromol 13:3711–3722. https://doi.org/10.1021/bm3011962
Forbes BY, Hall GS, Miller MB, Novak S, Rowlinson MC, Salfinger M et al (2018) Practice guidelines for clinical microbiology laboratories: mycobacteria. Clin Microbiol Rev 31:e00038. https://doi.org/10.1128/CMR.00038-17
Gong N, Tan Y, Li M, Lu W, Lei X (2016) ALA-PDT combined with antibiotics for the treatment of multiple skin abscesses caused by Mycobacterium fortuitum. Photodiagn Photodyn Ther 15:70–72. https://doi.org/10.1016/j.pdpdt.2016.05.009
Gupta RS, Lo B, Son J (2018) Phylogenomics and comparative genomic studies robustly support division of the genus Mycobacterium into an emended genus Mycobacterium and four novel genera. Front Microbiol 9:67. https://doi.org/10.3389/fmicb.2018.00067
Guterres KB, Rossi GG, Menezes LB, Anraku de Campos MM, Iglesias BA (2019) Preliminary evaluation of the positively and negatively charge effects of tetra-substituted porphyrins on photoinactivation of rapidly growing mycobacteria. Tuberculosis 117:45–51. https://doi.org/10.1016/j.tube.2019.06.001
Huang Q, Pan Z, Wang P, Chen Z, Zhang X, Xu H (2006) Zinc(II) and copper(II) complexes of beta-substituted hydroxylporphyrins as tumor photosensitizers. Bioorg Med Chem Lett 16(11):3030–3033. https://doi.org/10.1016/j.bmcl.2005.02.094
Jeong SH, Kim SY, Huh HJ, Ki CS, Lee NY, Kang CI et al (2017) Mycobacteriological characteristics and treatment outcomes in extrapulmonary Mycobacterium abscessus complex infections. Int J Infect Dis 60:49–56. https://doi.org/10.1016/j.ijid.2017.05.007
Kasperbauer SH, De Groote MA (2015) The treatment of rapidly growing mycobacterial infections. Clin Chest Med 36:67–78. https://doi.org/10.1016/j.ccm.2014.10.004
Kuhn BL, Paveglio GC, Silvestri S, Muller EI, Enders MSP, Martins MAP, Zanatta N, Bonacorso HG, Radke C, Frizzo CP (2019) TiO2 nanoparticles coated with deep eutectic solvents: characterization and effect on photodegradation of organic dyes. New J Chem 43:1415–1423. https://doi.org/10.1039/C8NJ05957H
Langa K, Mosinger J, Wagnerová DM (2004) Photophysical properties of porphyrinoid sensitizers non-covalently bound to host molecules; models for photodynamic therapy. Coord Chem Rev 248:321–350. https://doi.org/10.1016/j.ccr.2004.02.004
Lopes LQS, Ramos AP, Copetti PM, Acunha TV, Iglesias BA, Vianna Santos RC et al (2019) Antimicrobial activity and safety applications of meso-tetra(4-pyridyl)platinum(II) porphyrin. Microb Pathog 28:47–54. https://doi.org/10.1016/j.micpath.2018.12.038
MacDonald IJ, Dougherty TJ (2001) Basic principles of photodynamic therapy. J Porphyrins Phthalocyan 5:105–129. https://doi.org/10.1002/jpp.328
Mah N, Perez-Iratxeta C, Andrade-Navarro MA (2010) Outer membrane pore protein prediction in mycobacteria using genomic comparison. Microbiology 156:2506–2515. https://doi.org/10.1099/mic.0.040089-0
Mahmoudi H, Pourhajibagher M, Alikhani MY, Bahador A (2019) The effect of antimicrobial photodynamic therapy on the expression of biofilm associated genes in Staphylococcus aureus strains isolated from wound infections in burn patients. Photodiagn Photodyn Ther 25:406–413. https://doi.org/10.1016/j.pdpdt.2019.01.028
Merchat M, Spikes JD, Bertoloni G, Jori G (1996) Studies on the mechanism of bacteria photosensitization by meso-substituted cationic porphyrins. J Photochem Photobiol B 35:149–157. https://doi.org/10.1016/s1011-1344(96)07321-6
Moore JE, Kruijshaar ME, Ormerod LP, Drobniewski F, Abubakar I (2010) Increasing reports of non-tuberculous mycobacteria in England, Wales and Northern Ireland, 1995–2006. BMC Public Health 10:612–621. https://doi.org/10.1186/1471-2458-10-612
Mosti G, Picerni P, Licau M, Mattaliano V (2018) Photodynamic therapy in infected venous and mixed leg ulcers: a pilot experience. J Wound Care 27:816–821. https://doi.org/10.12968/jowc.2018.27.12.816
Mougari F, Guglielmetti L, Raskine L, Sermet-Gaudelus I, Veziris N, Cambau E (2016) Infections caused by Mycobacterium abscessus: epidemiology, diagnostic tools and treatment. Expert Rev Anti-Infect Ther 14:1139–1154. https://doi.org/10.1080/14787210.2016.1238304
O’Riordan K, Sharlin DS, Gross J, Chang S, Errabelli D, Akilov OE et al (2006) Photoinactivation of Mycobacteria in vitro and in a new murine model of localized Mycobacterium bovis BCG-induced granulomatous infection. Antimicrob Agents Chemother 50:1828–1834. https://doi.org/10.1128/AAC.50.5.1828-1834.2006
Oliveira VA, Iglesias BA, Auras BL, Neves A, Terenzi H (2017) Photoactive meso-tetra(4-pyridyl)porphyrin-tetrakis-[chloro(2,2´bipyridine)platinum(II) derivatives recognize and cleave DNA upon irradiation. Dalton Trans 46:1660–1669. https://doi.org/10.1039/c6dt04634g
Pavani C, Uchoa AF, Oliveira CS, Iamamoto Y, Baptista MS (2009) Effect of zinc insertion and hydrophobicity on the membrane interactions and PDT activity of porphyrin photosensitizers. Photochem Photobiol Sci 8:233–240. https://doi.org/10.1039/b810313e
Pérez-Laguna V, Gilaberte Y, Millán-Lou MI, Agut M, Nonell S, Rezusta A et al (2019) A combination of photodynamic therapy and antimicrobial compounds to treat skin and mucosal infections: a systematic review. Photochem Photobiol Sci 18(5):1020–1029. https://doi.org/10.1039/c8pp00534f
Philips RC, Hoyer PE, White SM, Tinkey KT, Loeffelholz M, Andersen CR et al (2019) Cutaneous nontuberculous mycobacteria infections: a retrospective case series of 78 patients from the Texas Gulf Coast region. J Am Acad Dermatol 81:730–739. https://doi.org/10.1016/j.jaad.2019.04.022
Prochnow C, Venturini AB, Guilardi LF, Pereira GKR, Burgo TAL, Bottino MC et al (2018) Hydrofluoric acid concentrations: Effect on the cyclic load-to-failure of machined lithium disilicate restorations. Dent Mater 34:e255–e263. https://doi.org/10.1016/j.dental.2018.06.028
Rezende CA, Lee LT, Galembeck F (2009) Surface mechanical properties of thin polymer films investigated by AFM in pulsed force mode. Langmuir 25:9938–9946. https://doi.org/10.1021/la9010949
Ries AS, Cargnelutti JF, Basso G, Acunha TV, Iglesias BA, Flores EF, Weiblen R (2020) Water-soluble tetra-cationic porphyrins display virucidal activity against Bovine adenovirus and Bovine alphaherpesvirus 1. Photodiag Photodyn Ther 31:101947. https://doi.org/10.1016/j.pdpdt.2020.101947
Rosa LP, da Silva FC, Vieira RL, Tanajura BR, Gusmão AGS, Oliveira JM et al (2017) Application of photodynamic therapy, laser therapy, and a cellulose membrane for calcaneal pressure ulcer treatment in a diabetic patient: a case report. Photodiagn Photodyn Ther 19:235–238. https://doi.org/10.1016/j.pdpdt.2017.06.011
Rossi GG, Guterres KB, Bonez PC, Gundel SS, Aggertt VA, Siqueira FS, Ourique AF, Wagnerd R, Klein B, Santos RCV, Campos MMA (2017) Antibiofilm activity of nanoemulsions of Cymbopogon flexuosus against rapidly growing mycobacteria. Microb Pathog 113:335–341. https://doi.org/10.1016/j.micpath.2017.11.002
Rossi GG, Guterres KB, da Silveira CH, Moreira KS, Burgo TAL, Iglesias BA, de Campos MMA (2020) Peripheral tetra-cationic Pt(II) porphyrins photo-inactivating rapidly growing mycobacteria: First application in mycobacteriology. Microb Pathog 148:104455. https://doi.org/10.1016/j.micpath.2020.104455
Sander MA, Isaac-Renton JL, Tyrrell GJ (2018) Cutaneous nontuberculous mycobacterial infections in Alberta, Canada: an epidemiologic study and review. J Cutan Med Surg 22:479–483. https://doi.org/10.1177/1203475418776945
Sepehrnia N, Bachmann J, Ali M, Afyuni M, Andreas M (2018) Modeling Escherichia coli and Rhodococcus erythropolis transport through wettable and water repellent porous media. Colloids Surf B 172:280–287. https://doi.org/10.1016/j.colsurfb.2018.08.044
Shih MH, Huang FC (2011) Effects of photodynamic therapy on rapidly growing nontuberculous mycobacteria keratitis. Invest Ophthalmol Vis Sci 52:223–229. https://doi.org/10.1167/iovs.10-5593
Shleeva MO, Savitsky AP, Nikitushkin VD, Solovyev ID, Kazachkina NI, Perevarov VV et al (2019) Photoinactivation of dormant Mycobacterium smegmatis due to its endogenous porphyrins. Appl Microbiol Biotechnol 103:9687–9695. https://doi.org/10.1007/s00253-019-10197-3
Siqueira FS, Rossi GG, Machado AK, Alves CFS, Flores VC, Somavilla VD et al (2018) Sulfamethoxazole derivatives complexed with metals: a new alternative against biofilms of rapidly growing mycobacteria. Biofouling 34(1–19):57. https://doi.org/10.1080/08927014.2018.1514497
Siroy A, Mailaender C, Harder D, Koerber S, Wolschendorf F, Danilchanka O et al (2008) Rv1698 of Mycobacterium tuberculosis represents a new class of channel-forming outer membrane proteins. J Biol Chem 283:17827–17837. https://doi.org/10.1074/jbc.M800866200
Sun Y, Ogawa R, Xiao BH, Feng YX, Wu Y, Chen LH et al (2019) Antimicrobial photodynamic therapy in skin wound healing: a systematic review of animal studies. Int Wound J. https://doi.org/10.1111/iwj.13269
Sung N, Back S, Jung JH, Kim K-H, Kim J-K, Lee JH, Ra Y, Yang HC, Lim C, Cho S, Kim K, Jheon S (2013) Inactivation of multidrug resistant (MDR)—and extensively drug resistant (XDR)—Mycobacterium tuberculosis by photodynamic therapy. Photodiagn Photodyn Ther 10:694–702. https://doi.org/10.1016/j.pdpdt.2013.09.001
Tasso TT, Tsubone TM, Baptista MS, Mattiazzi LM, Acunha TV, Iglesias BA (2017) Isomeric effect on the properties of tetraplatinated porphyrins showing optimized phototoxicity for photodynamic therapy. Dalton Trans 46:11037–11045. https://doi.org/10.1039/c7dt01205e
Tovmasyan A, Weitner T, Sheng H, Lu M, Rajic Z, Warner DS et al (2013) Differential coordination demands in Fe versus Mn water-soluble cationic metalloporphyrins translate into remarkably different aqueous redox chemistry and biology. Inorg Chem 52:5677–5691. https://doi.org/10.1021/ic3012519
Wang SH, Pancholi P (2014) Mycobacterial skin and soft tissue infection. Curr Infect Dis Rep 16:438–452. https://doi.org/10.1007/s11908-014-0438-5
Wentworth AB, Drage LA, Wengenack NL, Wilson JW, Lohse CM (2013) Increased Incidence of cutaneous nontuberculous mycobacterial infection, 1980 to 2009: a population-based study. Mayo Clin Proc 88:38–45. https://doi.org/10.1016/j.mayocp.2012.06.029
Wildner LM, Nogueira CL, Souza BS, Senna SG, da Silva RM, Bazzo ML (2011) Micobactérias: Epidemiologia E Diagnóstico. Rev Patol Trop 40:207–229
Woods GL, Brown-Elliott B, Conville PS, Desmond EP, Hall GS, Lin G et al (2011) Susceptibility testing of mycobacteria, nocardiae, and other aerobic actinomycetes; approved standard, 2nd edn. Clinical and Laboratory Standards Institute, Wayne
Yang SC, Hsueh PR, Lai HC, Teng LJ, Huang LM, Chen JM et al (2003) High prevalence of antimicrobial resistance in rapidly growing mycobacteria in Taiwan. Antimicrob Agents Chemother 47:1958–1962. https://doi.org/10.1128/aac.47.6.1958-1962.2003
Acknowledgements
This study was financed by CNPq, CAPES, and FAPERGS. Bernardo A. Iglesias thanks Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq – Brazil; Universal process 409150/2018-5 and PG-2018 grants process 304711/2018-7) and Marli Matiko Anraku de Campos thanks Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq—Brazil; Grants 404541/2016-0). Thiago A. L. Burgo thanks to MCTIC/CNPq (465452/2014-0), FAPESP (2014/50906-9) and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior—Brasil (CAPES)—Finance Code 001 through INCT/INOMAT (National Institute for Complex Functional Materials) and MCT/Finep/CT-Infra 02/2010.
Author information
Authors and Affiliations
Contributions
KBG, GGR, and KM conceived and designed the study. KBG, GGR, and KM conducted experiments. BAI contributed to porphyrin synthesis. KBG, GGR, and KM analyzed the data. BAI, MMAC, and TALB wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This article does not contain any studies with human participants or animals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guterres, K.B., Rossi, G.G., de Campos, M.M.k.A. et al. Metal center ion effects on photoinactivating rapidly growing mycobacteria using water-soluble tetra-cationic porphyrins. Biometals 33, 269–282 (2020). https://doi.org/10.1007/s10534-020-00251-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-020-00251-3