Abstract
Alcohol abuse can influence sexual risk behavior; however, its measurement is not straightforward. This study compared self-reported alcohol use, via the AUDIT and CAGE, with levels of phosphatidylethanol (Peth), a phospholipid biomarker that forms with chronic, heavy drinking, among high-risk MSM and TW in Lima, Peru. Chi square, Fisher’s exact, Wilcoxon ranksum tests compared the instruments. Receiver operating curves determined sensitivity and specificity of the self-reported measures. Among 69 MSM and 17 TW, PEth was positive for 86% (95% CI 77–93%) of participants, while 67% reported binge-drinking in the last 2 weeks. The AUDIT classified 25% as hazardous drinkers while CAGE identified 6% as problem drinkers. Self-reported binge drinking was more sensitive than the AUDIT for PEth positivity (71% vs. 27%, p = 0.022). Among high-risk MSM and TW in Lima, validated, self-report measures of alcohol abuse underestimated biological measures. Further research correlating bio-markers and self-reported alcohol abuse measures is needed.

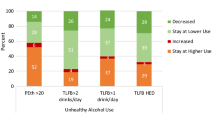
Image credit: United States Drug Testing Laboratories, Inc
Similar content being viewed by others
References
Cook RL, Clark DB. Is there an association between alcohol consumption and sexually transmitted diseases? A systematic review. Sex Transm Dis. 2005;32(3):156–64.
Fisher JC, Bang H, Kapiga SH. The association between HIV infection and alcohol use: a systematic review and meta-analysis of African studies. Sex Transm Dis. 2007;34(11):856–63. doi:10.1097/OLQ.0b013e318067b4fd.
Kalichman SC, et al. Alcohol use and sexual risks for HIV/AIDS in sub-Saharan Africa: systematic review of empirical findings. Prev Sci. 2007;8(2):141–51. doi:10.1007/s11121-006-0061-2.
Vagenas P, et al. A systematic review of alcohol use and sexual risk-taking in latin America. Pan Am J Public Health. 2013;34(4):267–74.
Chersich MF, et al. Enhancing global control of alcohol to reduce unsafe sex and HIV in sub-Saharan Africa. Glob Health. 2009;5:16. doi:10.1186/1744-8603-5-16.
Herrera MC, et al. Impact of alcohol use on sexual behavior among men who have sex with men and transgender women in Lima, Peru. Drug Alcohol Depend. 2016;161:147–54. doi:10.1016/j.drugalcdep.2016.01.030.
Ludford KT, et al. Screening for drug and alcohol use disorders and their association with HIV-related sexual risk behaviors among men who have sex with men in Peru. PLoS ONE. 2013;8(8):e69966. doi:10.1371/journal.pone.0069966.
Deiss RG, et al. Problem drinking is associated with increased prevalence of sexual risk behaviors among men who have sex with men (MSM) in Lima, Peru. Drug Alcohol Depend. 2013;132(1):134–9. doi:10.1016/j.drugalcdep.2013.01.011.
Vagenas P, et al. Being unaware of being HIV-infected is associated with alcohol use disorders and high-risk sexual behaviors among men who have sex with men in Peru. AIDS Behav. 2014;18(1):120–7. doi:10.1007/s10461-013-0504-2.
Schneider M, et al. Alcohol consumption and HIV/AIDS: the neglected interface. Addiction. 2012;107(8):1369–71. doi:10.1111/j.1360-0443.2012.03824.x.
Antiretroviral treatment as prevention (TasP) of HIV and TB. Programmatic update, AVAC. http://www.avac.org/resource/antiretroviral-treatment-prevention-tasp-hiv-and-tb-programmatic-update. Accessed 28 Dec 2015.
Hendershot CS, et al. Alcohol use and antiretroviral adherence: review and meta-analysis. J Acquir Immune Defic Syndr. 1999;52(2):180–202. doi:10.1097/QAI.0b013e3181b18b6e.
Ferro EG, et al. Alcohol use disorders negatively influence antiretroviral medication adherence among men who have sex with men in Peru. AIDS Care. 2015;27(1):93–104. doi:10.1080/09540121.2014.963013.
Azar MM, et al. A systematic review of the impact of alcohol use disorders on HIV treatment outcomes, adherence to antiretroviral therapy and health care utilization. Drug Alcohol Depend. 2010;112(3):178–93. doi:10.1016/j.drugalcdep.2010.06.014.
Hahn JA, Samet JH. Alcohol and HIV disease progression: weighing the evidence. Curr HIV/AIDS Rep. 2010;7(4):226–33. doi:10.1007/s11904-010-0060-6.
Bagby GJ, et al. Alcohol and HIV effects on the immune system. Alcohol Res. 2015;37(2):287–97.
Nelson S, Bagby GJ. Alcohol and HIV infection. Trans Am Clin Climatol Assoc. 2011;122:244–53.
Pandrea I, et al. Alcohol’s role in HIV transmission and disease progression. Alcohol Res Health. 2010;33(3):203–18.
Lotfipour S, et al. Increased detection of alcohol consumption and at-risk drinking with computerized alcohol screening. J Emerg Med. 2013;44(4):861–6. doi:10.1016/j.jemermed.2012.09.038.
Brown S-E, et al. Men who have sex with men in Peru: acceptability of medication-assisted therapy for treating alcohol use disorders. Am J Men’s Health. 2015;. doi:10.1177/1557988315576775.
Karno M, Granholm E, Lin A. Factor structure of the alcohol use disorders identification test (AUDIT) in a mental health clinic sample. J Stud Alcohol. 2015;. doi:10.15288/jsa.2000.61.751.
Reinert DF, Allen JP. The alcohol use disorders identification test (AUDIT): a review of recent research. Alcohol Clin Exp Res. 2002;26(2):272–9.
Isaksson A, et al. Phosphatidylethanol in blood (B-PEth): a marker for alcohol use and abuse. Drug Test Anal. 2011;3(4):195–200. doi:10.1002/dta.278.
Bajunirwe F, et al. Comparison of self-reported alcohol consumption to phosphatidylethanol measurement among HIV-infected patients initiating antiretroviral treatment in southwestern Uganda. PLoS ONE. 2014;9(12):e113152. doi:10.1371/journal.pone.0113152.
Asiimwe SB, et al. Comparison of traditional and novel self-report measures to an alcohol biomarker for quantifying alcohol consumption among HIV-infected adults in sub-Saharan Africa. Alcohol Clin Exp Res. 2015;39(8):1518–27. doi:10.1111/acer.12781.
Viel G, et al. Phosphatidylethanol in blood as a marker of chronic alcohol use: a systematic review and meta-analysis. Int J Mol Sci. 2012;13(11):14788–812. doi:10.3390/ijms131114788.
Deiss RG, et al. Characterizing the syphilis epidemic among men who have sex with men in lima, peru to identify new treatment and control strategies. BMC Infect Dis. 2013;13:426. doi:10.1186/1471-2334-13-426.
Saunders JB, et al. Development of the alcohol use disorders identification test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption–II. Addiction. 1993;88(6):791–804.
Bradley KA, et al. AUDIT-C as a brief screen for alcohol misuse in primary care. Alcohol Clin Exp Res. 2007;31(7):1208–17. doi:10.1111/j.1530-0277.2007.00403.x.
Ewing JA. Detecting alcoholism. The CAGE questionnaire. JAMA. 1984;252(14):1905–7.
Drinking Levels Defined| National Institute on Alcohol Abuse and Alcoholism (NIAAA). https://www.niaaa.nih.gov/alcohol-health/overview-alcohol-consumption/moderate-binge-drinking. Accessed 7 Apr 2017.
Bakhireva LN, et al. The validity of phosphatidylethanol in dried blood spots of newborns for the identification of prenatal alcohol exposure. Alcohol Clin Exp Res. 2014;38(4):1078–85. doi:10.1111/acer.12349.
Stewart SH, et al. Phosphatidylethanol and alcohol consumption in reproductive age women. Alcohol Clin Exp Res. 2010;34(3):488–92. doi:10.1111/j.1530-0277.2009.01113.x.
Hahn JA, et al. Phosphatidylethanol (PEth) as a biomarker of alcohol consumption in HIV positives in sub-Saharan Africa. Alcohol Clin Exp Res. 2012;36(5):854–62. doi:10.1111/j.1530-0277.2011.01669.x.
Stewart SH, et al. Validation of blood phosphatidylethanol as an alcohol consumption biomarker in patients with chronic liver disease. Alcohol Clin Exp Res. 2014;38(6):1706–11. doi:10.1111/acer.12442.
Alvy LM, et al. Depression is associated with sexual risk among men who have sex with men, but is mediated by cognitive escape and self-efficacy. AIDS Behav. 2011;15(6):1171–9. doi:10.1007/s10461-010-9678-z.
Ruiz-Grosso P, et al. Validation of the spanish center for epidemiological studies depression and Zung self-rating depression scales: a comparative validation study. PLoS ONE. 2012;7(10):e45413. doi:10.1371/journal.pone.0045413.
Clark JL, et al. Sampling methodologies for epidemiologic surveillance of men who have sex with men and transgender women in latin America: an empiric comparison of convenience sampling, time space sampling, and respondent driven sampling. AIDS Behav. 2014;18(12):2338–48. doi:10.1007/s10461-013-0680-0.
Konda K, et al. (2015) Factors associated with high incident HIV in a high-risk cohort in Lima, Peru. IAS, Vancouver, July 2015.
Michaud JM, Johnson SM, Ellen J. Comparison of sex partner meeting venues and residences of syphilis cases in Baltimore. Sex Transm Dis. 2004;31(4):239–42.
Grov C, et al. Exploring the venue’s role in risky sexual behavior among gay and bisexual men: an event-level analysis from a national online survey in the U.S. Arch Sex Behav. 2013;42(2):291–302. doi:10.1007/s10508-011-9854-x.
Thiede H, et al. Determinants of recent HIV infection among seattle-area men who have sex with men. Am J Public Health. 2009;99(Suppl 1):S157–64. doi:10.2105/AJPH.2006.098582.
Jain J, et al. Comparison of phosphatidylethanol results to self-reported alcohol consumption among young injection drug users. Alcohol Alcohol. 2014;49(5):520–4. doi:10.1093/alcalc/agu037.
Francis JM, et al. Comparison of self-reported alcohol use with the alcohol biomarker phosphatidylethanol among young people in northern Tanzania. Drug Alcohol Depend. 2015;156:289–96. doi:10.1016/j.drugalcdep.2015.09.027.
Monteiro MG, et al. AUDIT : the alcohol use disorders identification test : guidelines for use in primary health care. 2001. http://www.who.int/iris/handle/10665/67205.
Bradley KA, et al. Screening for problem drinking: comparison of CAGE and AUDIT. J Gen Intern Med. 1998;13(6):379–88. doi:10.1046/j.1525-1497.1998.00118.x.
Kechagias S, et al. Phosphatidylethanol compared with other blood tests as a biomarker of moderate alcohol consumption in healthy volunteers: a prospective randomized study. Alcohol Alcohol. 2015;50(4):399–406. doi:10.1093/alcalc/agv038.
Bush K, Kivlahan DR, McDonell MB, Fihn SD, Bradley KA. The AUDIT alcohol consumption questions (AUDIT-C): an effective brief screening test for problem drinking. Ambulatory care quality improvement project (ACQUIP). Alcohol use disorders identification test. Arch Intern Med. 1998;158(16):1789–95.
Brawner BM, et al. The black man’s country club. Fam Community Health. 2013;36(2):109–18. doi:10.1097/FCH.0b013e318282b2b5.
Fritz KE, et al. The association between alcohol use, sexual risk behavior, and HIV infection among men attending beerhalls in Harare, Zimbabwe. AIDS Behav. 2002;6(3):221–8. doi:10.1023/A:1019887707474.
Kalichman SC, et al. HIV/AIDS risks among men and women who drink at informal alcohol serving establishments (Shebeens) in Cape Town, South Africa. Prev Sci. 2008;9(1):55–62. doi:10.1007/s11121-008-0085-x.
Daskalakis D, et al. Implementation of HIV testing at 2 New York City bathhouses: from pilot to clinical service. Clin Infect Dis. 2009;48(11):1609–16. doi:10.1086/598979.
Kalichman SC, et al. Randomized trial of a community-based alcohol-related HIV risk-reduction intervention for men and women in cape town south Africa. Ann Behav Med. 2008;36(3):270–9. doi:10.1007/s12160-008-9067-2.
Glanz K, Bishop DB. The role of behavioral science theory in development and implementation of public health interventions. Annu Rev Public Health. 2010;31(1):399–418. doi:10.1146/annurev.publhealth.012809.103604.
Acknowledgements
The authors would like to thank all study participants and staff for their contributions to this study. This study was partially funded by a seed grant from the UCLA AIDS Institute. We would also like to thank Jina Lee and Helen Houldsworth of the UCLA AIDS Institute for her assistance with study funding and obligations. Finally, we would like to thank Meghan Burke and Joseph Jones of the United States Drug Testing Laboratory for their assistance in obtaining and interpreting phosphatidylethanol test assays.
Funding
This research was funded by the UCLA Center for AIDS Research #AI028697 and by NIH 1R01AI099727 and NIH/NIMH R25MH087222.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study. The institutional review board of the Universidad Peruana Cayetano Heredia approved the study.
Rights and permissions
About this article
Cite this article
Herrera, M.C., Konda, K.A., Leon, S.R. et al. Do Subjective Alcohol Screening Tools Correlate with Biomarkers Among High-Risk Transgender Women and Men Who Have Sex with Men in Lima, Peru?. AIDS Behav 21 (Suppl 2), 253–261 (2017). https://doi.org/10.1007/s10461-017-1933-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-017-1933-0