Abstract
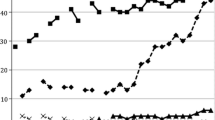
To examine the association between demographic characteristics and long-term smoking trajectory group membership among HIV-seropositive and HIV-seronegative men who have sex with men (MSM). A cohort of 6552 MSM from the Multicenter AIDS Cohort Study were asked detailed information about their smoking history since their last follow-up. Group-based trajectory modeling was used to examine smoking behavior and identify trajectory group membership. Because participants enrolled after 2001 were more likely to be younger, HIV-seronegative, non-Hispanic black, and have a high school diploma or less, we also assessed time of enrollment in our analysis. Participants were grouped into 4 distinct smoking trajectory groups: persistent nonsmoker (n = 3737 [55.9 %]), persistent light smoker (n = 663 [11.0 %]), heavy smoker to nonsmoker (n = 531 [10.0 %]), and persistent heavy smoker (n = 1604 [23.1 %]). Compared with persistent nonsmokers, persistent heavy smokers were associated with being enrolled in 2001 and later (adjusted odds ratio [aOR] 2.35; 95 % CI 2.12–2.58), having a high school diploma or less (aOR 3.22; 95 % CI 3.05–3.39), and being HIV-seropositive (aOR 1.17; 95 % CI 1.01–1.34). These associations were statistically significant across all trajectory groups for time of enrollment and education but not for HIV serostatus. The overall decrease of smoking as shown by our trajectory groups is consistent with the national trend. Characteristics associated with smoking group trajectory membership should be considered in the development of targeted smoking cessation interventions among MSM and people living with HIV.

Similar content being viewed by others
References
Mdodo R, et al. Cigarette smoking prevalence among adults with HIV compared with the general adult population in the United States: cross-sectional surveys. Ann Intern Med. 2015;162(5):335–44.
Crothers K, et al. Impact of cigarette smoking on mortality in HIV-positive and HIV-negative veterans. AIDS Educ Prev. 2009;21(3 Suppl):40–53.
Lifson AR, Lando HA. Smoking and HIV: prevalence, health risks, and cessation strategies. Curr HIV/AIDS Rep. 2012;9(3):223–30.
Lifson AR, et al. Smoking-related health risks among persons with HIV in the strategies for management of antiretroviral therapy clinical trial. Am J Public Health. 2010;100(10):1896–903.
Tesoriero JM, et al. Smoking among HIV positive New Yorkers: prevalence, frequency, and opportunities for cessation. AIDS Behav. 2010;14(4):824–35.
Pacek LR, Harrell PT, Martins SS. Cigarette smoking and drug use among a nationally representative sample of HIV-positive individuals. Am J Addict. 2014;23(6):582–90.
Benard A, et al. Tobacco addiction and HIV infection: toward the implementation of cessation programs. ANRS CO3 Aquitaine Cohort. AIDS Patient Care STDS. 2007;21(7):458–68.
Royce RA, Winkelstein W Jr. HIV infection, cigarette smoking and CD4 + T-lymphocyte counts: preliminary results from the San Francisco Men’s Health Study. AIDS. 1990;4(4):327–33.
Stall RD, et al. Cigarette smoking among gay and bisexual men. Am J Public Health. 1999;89(12):1875–8.
Reynolds NR. Cigarette smoking and HIV: more evidence for action. AIDS Educ Prev. 2009;21(3 Suppl):106–21.
Agaku I, King B, Dube S. Current cigarette smoking among adults-United States, 2005–2012. MMWR Mortal Mortal Wkly Rep. 2014;63:29–34.
Justice AC. HIV and aging: time for a new paradigm. Curr HIV/AIDS Rep. 2010;7(2):69–76.
Barbaro G, et al. An open-label, prospective, observational study of the incidence of coronary artery disease in patients with HIV infection receiving highly active antiretroviral therapy. Clin Ther. 2003;25(9):2405–18.
Friis-Moller N, et al. Combination antiretroviral therapy and the risk of myocardial infarction. N Engl J Med. 2003;349(21):1993–2003.
Petoumenos K, et al. Rates of cardiovascular disease following smoking cessation in patients with HIV infection: results from the D:A: D study(*). HIV Med. 2011;12(7):412–21.
Kaslow RA, et al. Infection with the human immunodeficiency virus: clinical manifestations and their relationship to immune deficiency. A report from the Multicenter AIDS Cohort Study. Ann Intern Med. 1987;107(4):474–80.
Dudley J, et al. The Multicenter AIDS Cohort Study: retention after 9 1/2 years. Am J Epidemiol. 1995;142(3):323–30.
Akhtar-Khaleel WZ, et al. Trends and predictors of cigarette smoking among HIV seropositive and seronegative men: the Multicenter AIDS Cohort Study. AIDS Behav. 2015. doi:10.1007/s10461-015-1099-6.
Cook RL, et al. Alcohol consumption trajectory patterns in adult women with HIV infection. AIDS Behav. 2013;17(5):1705–12.
Lim SH, et al. Changes in stimulant drug use over time in the MACS: evidence for resilience against stimulant drug use among men who have sex with men. AIDS Behav. 2012;16(1):151–8.
Hedeker D, Gibbons R. Longitudinal data analysis. Hoboken: Wiley; 2006.
Nagin D. Group-based modeling of development. Cambridge: Harvard University Press; 2005.
Shwarz G. Estimating the dimension of a model. Ann Stat. 1978;9(2):461–4.
Audrain-McGovern J, et al. Identifying and characterizing adolescent smoking trajectories. Cancer Epidemiol Biomarkers Prev. 2004;13(12):2023–34.
Bernat DH, et al. Adolescent smoking trajectories: results from a population-based cohort study. J Adolesc Health. 2008;43(4):334–40.
Hampson SE, et al. Smoking trajectories across high school: sensation seeking and hookah use. Nicotine Tob Res. 2013;15(8):1400–8.
Lessov-Schlaggar CN, et al. Adolescent smoking trajectories and nicotine dependence. Nicotine Tob Res. 2008;10:341–51.
Greenwood GL, et al. Tobacco use and cessation among a household-based sample of US urban men who have sex with men. Am J Public Health. 2005;95:145–51.
Herrick AL, et al. Adversity and syndemic production among men participating in the multicenter AIDS cohort study: a life-course approach. Am J Public Health. 2013;103(1):79–85.
Kurtz SP, et al. Resilience, syndemic factors, and serosorting behaviors among HIV-positive and HIV-negative substance-using MSM. AIDS Educ Prev. 2012;24(3):193–205.
Stall R, Friedman M, Catania J. Interacting epidemics and gay men’s health: a theory of syndemic production among urban gay men. In: Unequal opportunity: health disparities affecting gay and bisexual men in the United States. New York: Oxford University Press; 2008.
Fergus S, Zimmerman MA. Adolescent resilience: a framework for understanding healthy development in the face of risk. Annu Rev Public Health. 2005;26:399–419.
Rabkin JG, et al. Resilience in adversity among long-term survivors of AIDS. Hosp Community Psychiatry. 1993;44(2):162–7.
Mills TC, et al. Distress and depression in men who have sex with men: the Urban Men’s Health Study. Am J Psychiatry. 2004;161(2):278–85.
Stall R, et al. Alcohol use, drug use and alcohol-related problems among men who have sex with men: the Urban Men’s Health Study. Addiction. 2001;96(11):1589–601.
Herrick AL, et al. Resilience as an untapped resource in behavioral intervention design for gay men. AIDS Behav. 2011;15(Suppl 1):S25–9.
Kent M, Davis M. The emergence of capacity-building programs and models of resilience. Handbook of adult resilience. New York: Guilford Press; 2010. p. 427–49.
Acknowledgments
Data in this manuscript were collected by the Multicenter AIDS Cohort Study (MACS) with centers at Baltimore (U01-AI35042): The Johns Hopkins University Bloomberg School of Public Health: Joseph B. Margolick (PI), Barbara Crain, Adrian Dobs, Homayoon Farzadegan, Joel Gallant, Lisette Johnson-Hill, Cynthia Munro, Michael W. Plankey, Ned Sacktor, James Shepard, Chloe Thio; Chicago (U01-AI35039): Feinberg School of Medicine, Northwestern University, and Cook County Bureau of Health Services: Steven M. Wolinsky (PI), John P. Phair, Sheila Badri, Maurice O’Gorman, David Ostrow, Frank Palella, Ann Ragin; Los Angeles(U01-AI35040): University of California, UCLA Schools of Public Health and Medicine: Roger Detels (PI), Otoniel Martínez-Maza (Co-P I), Aaron Aronow, Robert Bolan, Elizabeth Breen, Anthony Butch, Beth Jamieson, Eric N. Miller, John Oishi, Harry Vinters, Dorothy Wiley, Mallory Witt, Otto Yang, Stephen Young, Zuo Feng Zhang; Pittsburgh (U01-AI35041): University of Pittsburgh, Graduate School of Public Health: Charles R. Rinaldo (PI), Lawrence A. Kingsley (Co-PI), James T. Becker, Ross D. Cranston, Jeremy J. Martinson, John W. Mellors, Anthony J. Silvestre, Ronald D. Stall; and the Data Coordinating Center (UM1-AI35043): The Johns Hopkins University Bloomberg School of Public Health: Lisa P. Jacobson (PI), Alvaro Munoz (Co-PI), Alison, Abraham, Keri Althoff, Christopher Cox, Jennifer Deal, Gypsyamber D’Souza, Priya Duggal, Janet Schollenberger, Eric C. Seaberg, Sol Su, Pamela Surkan. The MACS is funded primarily by the National Institute of Allergy and Infectious Diseases (NIAID), with additional co-funding from the National Cancer Institute (NCI). Targeted supplemental funding for specific projects was also provided by the National Heart, Lung, and Blood Institute (NHLBI), and the National Institute on Deafness and Communication Disorders (NIDCD). MACS data collection is also supported by UL1-TR000424 (JHU CTSA). Website located at http://www.statepi.jhsph.edu/macs/macs.html. The contents of this publication are solely the responsibility of the authors and do not represent the official views of the National Institutes of Health (NIH).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Akhtar-Khaleel, W.Z., Cook, R.L., Shoptaw, S. et al. Long-Term Cigarette Smoking Trajectories Among HIV-Seropositive and Seronegative MSM in the Multicenter AIDS Cohort Study. AIDS Behav 20, 1713–1721 (2016). https://doi.org/10.1007/s10461-016-1343-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-016-1343-8