Abstract
Context
In France, cases of people self-reporting symptoms due to electromagnetic fields (EMF) or idiopathic environmental intolerance attributed to electromagnetic fields (IEI-EMF) have emerged over the past 10 years. Several self-help and action groups have claimed an increasing number of members. However, little is known about this population in France.
Aim
Our primary objective was to describe the reported symptoms and the sources that may induce these symptoms through a questionnaire-based study. Secondly, we discussed our results alongside those obtained from the existing literature and provide an overview of this physical condition.
Subjects and methods
From April to November 2014, a self-questionnaire survey was conducted in France. With 52 participants, the average age of respondents was 50 ± 11 years and the majority of participants at 79% were women.
Results
Our study results in the French population were consistent with findings in the literature conducted in other countries and also highlighted a number of emerging EMF sources such as wireless area networks, to be perceived as possible causes of symptoms.
Conclusions
Despite methodological differences, we summarized facts from previous comparable investigations. We also provided an overview of people claiming EMF effects and briefly discussed possible avenues of research.
Similar content being viewed by others
Introduction
Increasing use of electric appliances and wireless telecommunications devices may potentially lead to greater human exposure to electromagnetic fields. Some individuals experience adverse effects while using or being in the vicinity of devices and equipment emitting electromagnetic fields. This sensitivity to electromagnetic fields is a recent syndrome that is commonly known as electromagnetic hypersensitivity, a name given to it by Bergqvist and Vogel (1997). The phenomenon was first observed in 1980 in Norway and Sweden, where some workers claimed to have developed facial skin symptoms when working close to video display terminals (Knave et al. 1985). Electrohypersensitivity (EHS) syndrome is currently classified among the group of idiopathic environmental intolerances (IEI). An IEI is related to several environmental factors that are tolerated by the majority of individuals and for which the physiopathology is unclear. In 2006, the World Health Organization (WHO 2006) replaced the term “electromagnetic hypersensitivity” with “idiopathic environmental intolerance attributed to electromagnetic fields” (IEI-EMF). IEI-EMF manifestations include sleep disorders, headaches, fatigue, nervousness or distress and difficulty concentrating, skin symptoms or more localized symptoms affecting the ears, throat and eyes (Röösli et al. 2004). It is generally acknowledged that there is an overlap between the different symptoms of multiple chemical sensitivity (MCS), sick building syndrome (SBS) symptoms, amalgams-related symptoms, fibromyalgia (Kipen and Fiedler 2002) and environmental somatization syndrome (ESS) (Göthe et al. 1995). This cluster of syndromes including IEI-EMF is associated with odor and noise intolerance (Nordin et al. 2014).
The sources most often reported to have triggered IEI-EMF are mobile phones, cordless phones and power lines (Röösli et al. 2004; Eltiti et al. 2007), base stations, television, and public transportation (Kato and Johansson 2012), as well as personal computers (Hagström et al. 2013). A difference in symptom types according to the EMF source was found by Johansson et al. (2010).
The estimated prevalence of IEI-EMF varies from 1.5% in Sweden (Hillert et al. 2002) to 3.2% in California (Levallois et al. 2002), 3.5% in Austria (Schreier et al. 2006), 4% in the UK (Eltiti et al. 2007) and 13.3% in Taiwan (Meg Tseng et al. 2011). These differences are primarily dependent on the definition of IEI-EMF in the region. IEI-EMF prevalence is highest among women (Hillert et al. 2002).
Despite numerous double-blind experimental studies, there presently exists no validated demonstration of a direct association between the presentation of these symptoms and exposure to EMF (Rubin et al. 2011). Additionally, despite numerous propositions, a generally accepted mechanism of IEI-EMF is still lacking. Differences in physiological characteristics (baseline indices) between subjects reporting IEI-EMF and controls have been reported, suggesting a predisposition to sensitivity to physical stressors (Lyskov et al. 2001). One hypothesis of a genetic polymorphism pattern associated with IEI has been proposed by De Luca et al. (2014). Furthermore, a diagnosis of IEI-EMF remains difficult (Baliatsas et al. 2012) and most individuals who report suffering from IEI-EMF are self-diagnosed (Crasson 2005), with very few having been diagnosed by a physician.
The subject of IEI-EMF is controversial in France but has become a recurrent topic in recent media debates due to the public’s increasing concerns about the effects of EMF on health. Given the lack of studies available on the topic, we conducted a self-reporting survey involving people who suffer from IEI-EMF. The aim of this study was first to describe and characterize IEI-EMF more thoroughly in the French context by analyzing the reported symptoms of people suffering from this syndrome, as well as associated sources that individuals suffering from IEI-EMF believe are causing their symptoms. Secondly, we compared our results with those reported in the literature by previous studies.
Subjects and methods
Population
Information about the survey was first communicated to self-help group representatives for distribution to all members. In addition, people claiming to suffer from IEI-EMF and who heard about the survey were sent the questionnaire. The survey participants were all over the age of 22 and up to 80 years old and reported having developed at least one symptom, which they attributed to one or more sources of EMFs. They self-reported being “electrohypersensitive,” as no recognized medical procedure is in place for diagnosis of IEI-EMF.
Questionnaires were sent out from April to November 2014 throughout France to participants’ domicile in the following regions: Aquitaine, Bretagne, Centre, Ile de France, Limousin, Lorraine, Nord-Pas-de Calais, Normandie, Pays de la Loire, Provence-Alpe-Côte d’Azur and Rhône Alpes. Completed questionnaires were returned to our laboratory at INERIS (Institut nationale de l’environnement et des risques industriels). People interested in participating had preliminary contact with a researcher prior to receiving the questionnaire and were given information such as the affiliation and funding of the study, as well as the its purpose. Self-administered questionnaires were sent electronically or by regular mail, accompanied by a cover letter that included the names and contact information of the researchers responsible for conducting the study. Reminders were sent as needed.
The questionnaire was based on survey questionnaires previously used in epidemiological studies (Crasson 2005; Eltiti et al. 2007) and further elaborated with members of a local self-help group (Collectif des électrosensibles de France). Some modifications were made to the terms used and additional explanations (such as definitions of terms) and detailed questions were added.
Questionnaire
The self-administered French questionnaire included biographical questions such as age, gender, educational status and professional activities. The second part contained questions about the frequency and severity of symptoms in a list of 62 categorized symptoms. A Likertscale for frequency varying from “never” to “very often” and severity varying from “not at all” to “a great deal” was presented. Categories of symptoms included headache, sensation of coldness and categories for specific organs, functions or systems: skin, sensitivity, sleep, neurovegetative, locomotor, visual and auditory, and cardiorespiratory. These categories were proposed by a previous study by Eltiti et al. (2007) and found suitable for the purpose of our survey as this classification system encompasses a large number of symptoms.
Proposed sources included different frequency ranges resulting from the use of electricity (extremely low frequency range) to a few kilohertz (computer, TV display) and those deriving from mobile communication and broadband techniques (radio and microwave frequencies). Twenty-two EMF sources that may potentially trigger symptoms such as the digital enhanced cordless telecommunication (DECT), or other cordless phones, as well as mobile phones, were proposed and presented in the form of a Likert scale. Wireless fidelity (Wi-Fi), a local area wireless technology that is widely used in France, was also among the proposed sources. Numerous electronic devices use Wi-Fi including domestic appliances and public appliances (hotspots). Wi-Fi uses 2.45 and 5.2 GHz radio waves. The respondents were able to report whether an EMF source was “not at all” or “significantly” linked to occurring symptoms.
In an open question, participants were also given the opportunity to report all health complaints attributed to EMF and the associated EMF sources. Proximity to various sources (antennas, online high voltage, etc.) and the use of different electromagnetic devices (mobile phone, DECT) were also recorded. The third part of the questionnaire involved the general medical status of participants, including their medical history and environmental nuisance status (such as sensitivity to noise, smells, lights or any other environmental intolerance). Participants were asked to respond ‘yes’ or ‘no’ to the presence of sleep disturbance.
The final part of the questionnaire included questions about measures taken by participants and the perceived efficiency of different tested treatments such as conventional medicine, complementary and alternative medicine (CAM) and specific actions. All participants provided written informed consent for participating in the study. The protocol including biological tests (Andrianome et al. 2016, 2017a, b) and the self-questionnaire was approved by the ethics committee of CPP Nord Ouest CHU Amiens, France (CPP, 2014/8).
Data were collected in Excel tables, processed and analyzed with GraphPad Prism version 5.00 for Windows (GraphPad Software, San Diego, CA) and expressed as mean ± SD or number with percentage in parentheses. Symptom prevalence according to gender or association membership (people gathered in groups as associations or self-help groups) was compared using multiple Pearson chi-square tests. The alpha error was corrected and a corrected p-value of p < 0.00081 was considered significant.
Results
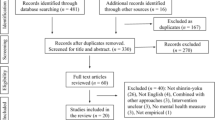
Questionnaires were sent to 84 individuals who had expressed an interest in the study and 52 (62%) were completed and returned. The remaining 32 were not returned and participants confirmed their non-participation for various reasons including the length of the questionnaire, a state of severe fatigue, or moving away from the area, as well as several other circumstances that prevented their participation. All returned questionnaires included usable datasets.
Among the respondents, 30 had registered themselves as electrohypersensitive at a French self-help group or other associations across France, while 22 did not belong to any type of association, but as members of the general population had been aware of the survey and reported at least one symptom that they attributed to one or multiple EMF sources. These participants were recruited through website advertising and word of mouth, as well as through blogs and online forums and newsgroups.
Respondents represented different regions across France: 50% were from Île de France (Paris area and its suburbs) and 50% were from other regions including Aquitaine, Bretagne, Centre, Limousin, Lorraine, Nord-Pas-de Calais, Normandie, Pays de la Loire, Provence-Alpe-Côte d’Azur and Rhône Alpes. The age and gender distribution of the participants are shown in Fig. 1. The ages of respondents varied from 22 to 80 years, with 83% of participants older than 40 and the average age being 50 (SD = 11).
The study population’s characteristics are presented in Table 1. Female respondents represented 79% of the study participants; 92% of participants had a high educational level (high-school graduation diploma or greater) and 62% took part in professional or educational activities. In terms of general health status, 6% (three women) reported a history of breast or skin cancer. Other respondents (8%) reported a medical diagnosis of Lyme’s disease (borreliosis), while 17% of respondents reported endocrine disorders (secondary amenorrhea, thyroid disorder or parathyroid disorder). One respondent reported having monoclonal gammopathy and 52% of participants reported the presence of sleep disorders.
Allergies and complaints related to environmental factors
The participants were asked to provide details about their allergies (Table 2). Food-induced allergies and intolerances included kiwi, apple, meat, milk and soy. Disturbances from various environmental factors in the home were assessed and the most disturbing environmental sources reported, in addition to electromagnetic fields, were cigarette smoke (37%), exhaust fumes (35%), stuffy air (37%), electrostatic discharges (35%), street odors (31%) low temperature (29%), and perfume (29%).
Symptoms attributed to EMF reported by respondents
Respondents were asked about the frequency of categorized symptoms in their daily lives. These are shown in Table 3.
For the 52 respondents, the most frequent symptoms were neurovegetative signs: fatigue, sleep disorders, exhaustion, difficulty concentrating and memory disorders, followed by head-related symptoms including headache, warmth or pain in the head, and tinnitus. Skin symptoms were less frequently reported. Generally, there was little difference in the frequencies of other symptoms (Table 3). There was no statistically significant difference between frequencies of occurrence for symptoms according to gender (male or female) at p = 0.99. According to volunteer origin (member or not a member of a self-help group) there was a statistical difference between the two groups (p < 0.0001).
Participants’ evaluation of symptom severity showed that the most intense symptoms (“quite a bit” to “a great deal”) were fatigue and exhaustion (73 and 64% respectively), sleep disorders (64%), headaches (52%) and tinnitus (52%), stress (48%), concentration difficulty (48%), sensitivity to noise (48%), anxiety (42%) and pressure in the ear (42%). Localized symptoms such as migraines, pain in the ear or hand tingling were intense for 37 to 40% of participants.
Participants were asked in an open question about the symptoms they experienced. A total of 77 different symptoms were reported, the individual number being 7 ± 5 per participant. One participant did not complete this part of the questionnaire. Figure 2 shows the 17 highest-reported symptoms, with headaches at the top of the list representing 59%, followed by neurovegetative symptoms (fatigue 35%, sleep disorders 31% and difficulty concentrating 26%). The following symptoms were also mentioned: anosmia, pain, pressure, buzzing, muscle stiffness, tension (each symptom by 10%); skin burning, blurred vision, burning eyes, oppression on diaphragm, depression (each symptom by 8%); sensation that the head is caught in a vise or heat (each symptom by 6%). New symptoms that were not mentioned in the questionnaire but mentioned by respondents included electrical sensations, buzzing and head vise. A sensation of discomfort when surrounded by EMF sources was also reported by 25% of the participants.
Sources
When presented with a list of 22 EMF sources, the most reported among those believed to be linked to symptoms were communication technologies, such as those presented in Fig. 3. In response to the open question, the most reported sources were also EMF associated with communication. Additionally, 46% of respondents were unable to cite a precise EMF source in their response (Fig. 4). Other sources were also mentioned: radiators, convectors, motor vehicles, radio antennas, metals, surveillance systems and underground cables. The average number of suspected sources was 5 ± 3 types per participant in the entire group.
Characteristics of IEI-EMF symptoms
The mean duration of IEI-EMF in the population sample was 8.5 years (SD = 8.4), with a minimum of 1 year and a maximum of 42 years. Among respondents, 75% reported having developed their sensitivity during the past 10 years. Respondents reported developing symptoms immediately when exposed to EMF sources (23%), after a few minutes (14%), after a few hours (11%) or after 1 day (4%) of exposure. Seven respondents (14%) reported different forms of onset depending on the source intensity, the location (city or country), their level of tiredness and the time of day (day or night). Among the respondents, 35% reported developing symptoms during a variable window following exposure (from a few minutes to 1 day after exposure to an EMF source).
According to 10% of respondents, the symptoms resolved spontaneously following the end of exposure to an EMF source. Other participants (10%) required a few minutes and 25% needed a few hours to recover. There was heterogeneity regarding the time of offset for 29% of respondents and this was dependent on the EMF source. Recovery was gradual, ranging from several hours to several days for 25% of the respondents.
Electromagnetic field exposure and intolerance history
The proximity to environmental EMF reported by participants is depicted in Table 4. Among participants, 67% reported proximity to a mobile phone antenna (37% at a distance of 50 m), while only 18% reported being near to high voltage lines. A proportion of 64% considered themselves to be in proximity to an electric line, transformer or railway.
First symptom appearance was linked to a particular event for 50% of the participants. These events included dental restoration, first use of a mobile phone and electrical appliance installation. One participant reported initial symptoms after traveling abroad and one following a car accident (Table 5).
Support and applied treatments
The self-reported questionnaire comprised a list of entities potentially approached by respondents and that could have assisted them. Among all respondents, 89% consulted a general practitioner, 73% a medical specialist, 71% an association, 52% an occupational physician, 37% local authorities, 23% a scientist and 21% contacted telephone operators. According to participants, the most satisfying entities were an association (70%), medical specialist (34%) and a scientist (33%). Only 15% of those who consulted a general practitioner were satisfied (Table 6).
A Likert-scale concerning the measures taken was completed as part of the questionnaire. Of the 52 responses, the most effective actions were measures of avoidance such as participants keeping themselves away from EMF sources (89%), disconnecting all EMF sources (81%) and removing EMF sources where possible (79%; Table 7). Additionally, in their daily lives, 60% of participants declared limiting their use of mobile phones. The median time spent on mobile phones talking or texting was 5 min/day (range from 0 to 120 min) with a mean of 15.8 ± 26 min. Wireless networks were avoided and not used by 73% of respondents. Most of them (92%) used computers with a plasma screen or cathodic screen at home or at work. Protection devices such as special fabrics and a baldachin were effective for 57% of participants used them; 67% took vitamin supplements and 56% took medication, but these were declared helpful only for 35% and 40% respectively.
Discussion
This is the first questionnaire-based study conducted involving people self-reporting symptoms attributed to EMF in France. The present survey confirmed the presence of people self-diagnosing IEI-EMF syndrome in France. When self-reporting IEI-EMF, participants responded “yes” to the question: “Do you consider yourself as electrohypersensitive?”. Furthermore, participants self-reporting IEI-EMF were also given the opportunity to attribute symptoms to a source in an open question. Since the extent of this physical condition is unknown in France, one of our goals was to identify and describe IEI-EMF sufferers. While associations and Internet groups have recently increased in number and visibility worldwide, IEI-EMF remains unclear. Despite the fact that causality has not been established in Finland, IEI-EMF sufferers self-report that shielding and alternative therapies are more effective than psychotherapy and medication, which are the officially recommended treatments (Hagström et al. 2013). Several reviews concluded the absence of effects of short-term exposure to EMF (Kwon and Hämäläinen 2011; Röösli et al. 2010; Röösli and Hug 2011; Rubin et al. 2006, 2010) but controversies regarding the long-term effects of EMF on health, and more specifically on cancer, remain current and debated. This maintains and confirms the necessity for conducting further studies on the topic. On the other hand, the official French Agency for Food, Environmental and Occupational Health and Safety (ANSES) has, along with scientific expert groups, issued a report in which it is concluded that some biological effects have been observed as the result of exposure to EMF. However, it is impossible to conclude that the observed biological effects are generators of adverse health effects (ANSES, collective expert report, 2013). Most recent studies that address people’s complaints about EMF in France date back to 2002 and aim to evaluate the health of people living near mobile base stations (Santini et al. 2002). One ongoing clinical research hospital program was initiated in 2012 and relates to people presenting IEI-EMF across France (Assistance Publique, Hôpitaux de Paris et al. 2012).
Our study included self-reported IEI-EMF from several French regions and the study group comprised both volunteers registered at self-help groups and those who were not. We received 52 questionnaires, which can be considered a relatively low number, but it is comparable to those reported in other surveys in terms of population size (Kato and Johansson 2012). However, it can also be speculated that the prevalence of self-reported IEI-EMFs is low in France. Additionally, our study took place within a limited time frame of 8 months. The low response may to some extent be attributed to a discrepancy between our goals and the expectations of the self-reporting sensitive population. Indeed, people self-reporting IEI-EMF actively seek out concrete solutions. It also appears that the length of the questionnaire may have contributed to the low participation rate. Our questionnaire structure may be improved for future studies. Likewise, a larger epidemiological study will be necessary to evaluate the estimated prevalence of IEI-EMF in France. To further examine IEI-EMF characteristics, a large number of observational and experimental studies have been performed.
When comparing our results with existing literature (surveys), we noted that volunteers were selected from self-help groups, from the general population or from both. While some studies, such as our investigation, focused on IEI-EMF cases only (Kato and Johansson 2012; Hagström et al. 2013), others compared groups with IEI-EMF to healthy individuals (Röösli et al. 2004; van Dongen et al. 2014; Johansson et al. 2010), while some addressed populations reporting general environmental sensitivity (GES) (Baliatsas et al. 2014). In some studies, individuals with IEI-EMF were compared with people complaining about general mobile phone disturbances only (Johansson et al. 2010) or with people reporting non-specific physical symptoms, but who did not consider themselves as electrohypersensitive (Rubin et al. 2008). The presence of a comparative group is informative for the identification of potential associated factors or links with other environmental illnesses or diseases.
Presently, there is no generally accepted definition for this syndrome (Baliatsas et al. 2012). For a classification of IEI-EMF cases, most studies use a common criterion that was also used in our survey. IEI-EMF was self-reported by complainants and IEI-EMF accepted being categorized as an IEI-EMF sufferer. Baliatsas et al. (2014) defined IEI-EMF cases as volunteers who responded “quite agree” to “agree” to a sensitivity to mobile phone base stations, communication systems devices and electrical devices. Using this combination of criteria, these authors (Baliatsas et al. 2014) defined IEI-EMF cases but not the volunteers themselves. It is important to emphasize that the selection criteria used since the beginning of research on IEI-EMF has been the self-testimony of symptom appearance related to EMF exposure.
Several studies in the literature also introduce subscales from validated questionnaires. Questionnaires used included the Coping Inventory for Stressful Situations (CISS) to evaluate stress, the Four-Dimensional Symptom Questionnaire (4DSQ) for somatic symptoms, the Groningen Sleep Quality Scale (GSQS) for sleep quality, the Modern Health Worries (MHWs), Karolinska Scales of Personality (KSP) for personality assessment and the Symptoms and Perception (SaP) scale. Baliatsas et al. (2014) evaluated EMF exposure using self-reported symptoms and electro-medical records. A strong limitation of surveys in general is their cross-sectional design; however, by using information from medical records, more data on the general history of patients can be obtained. Wherever possible, such a method should be used to complete surveys studies.
Our results have another point in common with the literature, namely the overwhelming evidence that the proportion of those with IEI-EMF is predominantly female (up to 95%). Thirteen studies among 16 we reviewed showed that the proportion of women respondents is above 50%, which is in accordance with our findings. Whether the gender of sufferers might account for triggering symptoms in IEI-EMF subjects remains unclear. The mean age of participants was roughly 50, and the predominance of middle-aged individuals may indicate a special mechanism, such as the cumulative effect of exposure in earlier periods of life, or simply vulnerability at this particular age.
Due to the large number of terms used, some authors restricted the number of proposed symptoms (Röösli et al. 2004) by gathering them under common terms. A small number of studies assessed the frequency or severity of symptoms. Additionally, some studies differentiated between EMF sources. As a result of these different assessment methods, comparisons between studies present some challenges. However, it is still possible to say that symptoms such as fatigue, headache and sleep disorders remained predominant among the most frequently reported symptoms, followed by concentration difficulty, stress and anxiety, whereas skin dryness, sore joints and musculoskeletal symptoms were less common. Researchers used different methods to determine the frequency of symptoms, e.g. symptoms developing at least once a week (Röösli et al. 2004; Johansson et al. 2010), symptoms related or unrelated to an acute phase (Hagström et al. 2013) or generally reported symptoms. Knave et al. (1985) reported symptoms of sensitivity focused on local manifestations such as eye or skin-related symptoms. Such manifestations are currently integrated in the categories of neurovegetative and head-related symptoms. Furthermore, in our survey, the use of new terms for describing some symptoms such as “electrical sensation” or “buzzing” and “head vise” are not mentioned in earlier studies.
The relatively high number of symptoms attributed to EMF contributes to the complexity of IEI-EMF. In fact, many of these symptoms were presented by healthy individuals in their daily lives (e.g. headache and sleep disorders) or were found alongside other diseases such as inflammatory and chronic diseases (Dahmen et al. 2009; Eltiti et al. 2009; Hillert et al. 2001), or in other IEI such as multiple chemical sensitivity. For this reason, it is useful to create a comparative group in order to evaluate differences in the frequency or severity of symptoms. Eltiti and colleagues suggested identifying IEI-EMF cases according to the severity and frequency of symptoms (Eltiti et al. 2007) by using a threshold score.
Another important aspect assessed in various questionnaires was the identification of EMF sources triggering symptoms. Studies once again differed to some degree with regard to symptom assessment. Sources can be summarized into groups of communication techniques, electrical appliances and/or EMF associated with transportation, which supposes a wide range of EMF frequencies. Among the most recurrent associated sources, mobile phones, base stations, cordless phones and power lines remain constantly cited. Other electrical appliances such as transformers, televisions and personal computers are also reported. IEI-EMF sufferers also identified several light sources as triggering symptoms, including low voltage light and energy saving lamps. We noted in our study the appearance of new sources, such as a wireless networks (Wi-Fi) and Bluetooth. It seems that sources related to wireless technology and associated with symptoms of IEI-EMF will increase alongside the continuous development of wireless technologies.
In order to evaluate the relationship between EMF exposure and symptoms, questions assessing direct associations between EMF and sources need to be better developed. Likewise, few studies have correlated the use of EMF-emitting sources and people suffering from IEI-EMF. In our study, we evaluated both sources and the association between sources and symptoms. Curiously, we noted that some cited sources are not actually sources of exposure, which means that either some participants were not aware of what source emits EMF or not, or that the symptoms they attribute to these sources have other origins that need to be identified.
Other key points of comparison
Only two studies, including our survey, report the latency of symptoms; this aspect may serve as a clue for determining the mechanism that triggers symptom appearance. Despite the majority of IEI-EMF sufferers reacting rapidly (immediately to within a few minutes), almost half of them in both our study and Röösli’s surveys (2004, 2010) reported developing symptoms after at least 1 h, indicating a lengthy onset time. Additionally, these results may indicate that EMF symptoms may occur after either an acute or long-term exposure to EMF. Recent studies have questioned whether a distinction should be made between patients reporting symptoms after short-term exposure and patients experiencing symptoms after longer-term exposure to EMF sources (Baliatsas et al. 2012). Furthermore, as proposed by the same author, it is not yet known whether a subdivision exists between sources (source specific sensitivities). This question cannot be answered in the current study, due to the multiple EMF sources reported.
Concerning the management of symptoms by IEI-EMF sufferers, data collected in previous studies showed that hypersensitive individuals had undertaken several treatments to minimize symptoms. The majority of sufferers consulted a medical doctor or a medical specialist. However, the absence of a diagnosis and a lack of evidence regarding causality, as well as the lack of a known mechanism, saw solutions other than official treatments being sought out by IEI-EMF individuals. Participants physically avoided EMF sources, for example, by using shielding equipment. They used CAM and nutrition supplements such as vitamins or anti-oxidants. Some researchers have also suggested the use of cognitive behavioral therapy as a more available and effective treatment (Rubin et al. 2006). However, according to survey results, only a very low proportion of individuals with IEI-EMF reported psychotherapy as efficient or helpful (Hagström et al. 2013).
In terms of efficacy, avoidance of EMF is a more efficient approach to protection according to the respondents. This includes avoidance of EMF linked to electricity (Röösli et al. 2004), all indoor sources (Hagström et al. 2013) or simply disconnecting EMF sources or using EMF shielding. When other commonly cited sources, e.g. wireless networks, Bluetooth, mobile phones and DECT, were being employed for personal use, they could easily be avoided. Sources originating from other people nearby or neighbors, or mobile telephony base station antennas, were more difficult to avoid, except by moving away from them. As is known, the EMF decreases rapidly with distance from the source, where exposure levels generally become low, well below 1 V/m. Although highly satisfying for hypersensitive people, such actions are penalizing and drastic, and are incompatible with their current lifestyle. On the other hand, according to EHS testimonies, the economic aspects of some measures (e.g. shielding installation and moving house) are not affordable for all sufferers. The use of CAM has been found to be efficient for the alleviation of IEI-EMF symptoms. Some authors emphasize that anti-oxidants can potentially improve the health and physical condition of IEI-EMF sufferers. In the case of France, CAM is widely used by the population; in 2002, 49% of French citizens used a complementary alternative medicine at least once for curative intent or for improving their well-being (WHO 2002). Users of CAM were primarily women. The large-scale adoption of CAM may be explained by its availability and popularity.
In addition, some of the surveys analyzed also investigated different aspects of IEI-EMF. By using specific questionnaires, studies have explored personal characteristics (Johansson et al. 2010) and comorbidities (Baliatsas et al. 2014; Rubin et al. 2008; Kjellqvist et al. 2016). Nordin et al. (2014) evaluated the link between IEI-EMF and other IEI, while Palmquist et al.’s (2014) evaluation included environmental factors, stress-related factors, stress related to modern concerns and health risk perception. Previous studies also investigated the relationship between IEI-EMF and allergies. These aspects were not examined in our survey; however, all these findings contribute to a better comprehension of IEI-EMF. In view of the results of these studies, a multidisciplinary approach is necessary to provide for the adequate management of IEI-EMF. At the same time, research on IEI-EMF should pay more attention to these additional factors and their influence in the development of IEI-EMF.
More generally, in view of all the available research on IEI-EMF including surveys and experimental studies, a number of rare studies characterize the basal physiology or biology of IEI-EMF cases in the absence of EMF exposure. A greater number of studies have focused on exposure to EMF and concluded the absence of a causal link between exposure and biological/physiological parameters (Rubin et al. 2011). These studies are crucial for finding a link between exposure and IEI-EMF; however, characterization of IEI-EMF can also add invaluable information for better understanding of this condition. In fact, we can hypothesize that subjects suffering from IEI-EMF have distinct physiological or biological basal characteristics. One study among the limited literature is that of Lyskov et al. (2001), which investigated the neurophysiological characteristics of IEI-EMF patients by examining physiological functions and reactivity. In response to various tests, IEI-EMF individuals tend to have distinct responses compared with a control group. Biological aspects may be the needed tool for first evaluating the differences between sensitive and non-sensitive individuals. Similar approaches should be investigated in forthcoming studies. Additionally, biological analysis will confirm or invalidate the existence of possible subgroups of IEI-EMF: sufferers with symptoms after short-term exposure to EMF vs. sufferers with symptoms after long-term exposure to EMF (Baliatsas et al. 2012), and people attributing symptoms to mobile phones vs. people attributing symptoms to multiple sources (Johansson et al. 2010), for example. Cases with possible alternative diagnoses could also be identified. Such biological markers will be useful for researchers and clinicians (Andrianome et al. 2017a, b).
Conclusion
Our study provided an overview of the French IEI-EMF population and was compared to previous IEI-EMF surveys in the literature. Though our study was limited by its small sample size, its demographic data were in accordance with previous studies. It was important to highlight the presence of methodological differences between surveys. Methodological factors that were most commonly inconsistent across studies included symptoms and source assessments. Hence, it is challenging to compare results pertaining to symptoms and sources. However, data were quite complementary when employed to assess various aspects of IEI-EMF. Symptoms and self-descriptions can be used in the first step of identification; these could then be completed using other methods such as electro-medical records or journal records concerning electromagnetic field use in daily life. Secondly, in order to identify the physiological mechanisms underlying IEI-EMF, studies need to focus on biological identification, using markers to capture symptoms. Additional research is needed in this area, as current knowledge is insufficient for understanding the syndrome. Further research may wish to employ a standardized questionnaire to assess IEI-EMF and investigate potential biological markers.
Change history
30 January 2018
The journal had been advised to revise the title so that Clarivate Analytics can try to count the citations more accurately. There’s been confusion due to the existence of another journal with the same name.
References
Andrianome S, Hugueville L, de Seze R, Hanot-Roy M, Blazy K, Gamez C, Selmaoui B (2016) Disturbed sleep in individuals with idiopathic environmental intolerance attributed to electromagnetic fields (IEI-EMF): melatonin assessment as a biological marker. Bioelectromagnetics. https://doi.org/10.1002/bem.21965
Andrianome S, Gobert J, Hugueville L, Stéphan-Blanchard E, Telliez F, Selmaoui B (2017a) An assessment of the autonomic nervous system in the electrohypersensitive population: a heart rate variability and skin conductance study. J Appl Physiol (1985). https://doi.org/10.1152/japplphysiol.00229.2017
Andrianome S, Hugueville L, de Seze R, Selmaoui B (2017b) Increasing levels of saliva alpha amylase in electrohypersensitive (EHS) patients. Int J Radiat Biol 93(8):841–848. https://doi.org/10.1080/09553002.2017.1325971
Assistance Publique, Hôpitaux de Paris, Anses – Agence nationale de sécurité sanitaire de l’alimentation, de l’environnement et du travail (Anses), Institut National de l’Environnement Industriel et des Risques (INERIS) (2012) Evaluation of a specialized therapeutic care of patients presenting an idiopathic environmental intolerance attributed to electromagnetic fields. National Library of Medicine, Bethesda, MD. Available from: http://clinicaltrials.gov/show/NCT01854801. Accessed 20 April 2017
Avis de l’Anses Rapport d’expertise collective Radiofréquences et santé Mise à jour de l’expertise (2013) Available at: https://www.anses.fr/fr/system/files/AP2011sa0150Ra.pdf. Accessed 8 Jan 2016
Baliatsas C, Van Kamp I, Lebret E, Rubin G (2012) Idiopathic environmental intolerance attributed to electromagnetic fields (IEI-EMF): a systematic review of identifying criteria. BMC Public Health 12:643
Baliatsas C, van Kamp I, Hooiveld M, Yzermans J, Lebret E (2014) Comparing non-specific physical symptoms in environmentally sensitive patients: prevalence, duration, functional status and illness behavior. J Psychosom Res 76:405–413
Bergqvist U, Vogel E (1997) Possible health implication of subjective symptoms and electromagnetic fields. A report by a European group of experts for the European Commission. National Institute for Working Life, Solna , Sweden
Crasson M (2005) L’hypersensibilité à l’électricité: une approche multidisciplinaire pour un problème multifactoriel. Revue de la littérature. Rev Européenne Psychologie Appliquée/Eurp Rev Appl Psycho 55:51–67
Dahmen N, Ghezel-Ahmadi D, Engel A (2009) Blood laboratory findings in patients suffering from self-perceived electromagnetic hypersensitivity (EHS). Bioelectromagnetics 30(4):299–306
De Luca C, Thai JCS, Raskovic D, Cesareo E, Caccamo D, Trukhanov A, Korkina L (2014) Metabolic and genetic screening of electromagnetic hypersensitive subjects as a feasible tool for diagnostics and intervention. Mediat Inflamm 2014:924184. Available at: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4000647/pdf/MI2014-924184.pdf. Accessed 11 January 2016
Eltiti S, Wallace D, Zougkou K, Russo R, Joseph S, Rasor P, Fox E (2007) Development and evaluation of the electromagnetic hypersensitivity questionnaire. Bioelectromagnetics 28:137–151
Eltiti S, Wallace D, Ridgewell A, Zougkou K, Russo R, Sepulveda F, Fox E (2009) Short-term exposure to mobile phone base station signals does not affect cognitive functioning or physiological measures in individuals who report sensitivity to electromagnetic fields and controls. Bioelectromagnetics 30(7):556–563
Göthe C, Molin C, Nilsson C (1995) The environmental somatization syndrome. Psychosomatics 36:1–11
Hagström M, Auranen J, Ekman R (2013) Electromagnetic hypersensitive Finns: symptoms, perceived sources and treatments—a questionnaire study. Pathophysiology 20:117–122
Hillert L, Kolmodin-Hedman B, Eneroth P, Arnetz BB (2001) The effect of supplementary antioxidant therapy in patients who report hypersensitivity to electricity: a randomized controlled trial. Med Gen Med 3(2):11
Hillert L, Berglind N, Arnetz BB, Bellander T (2002) Prevalence of self-reported hypersensitivity to electric or magnetic fields in a population-based questionnaire survey. Scand J Work Environ Health 28:33–41
Johansson A, Nordin S, Heiden M, Sandström M (2010) Symptoms, personality traits, and stress in people with mobile phone-related symptoms and electromagnetic hypersensitivity. J Psychosom Res 68:37–45
Kato Y, Johansson O (2012) Reported functional impairments of electrohypersensitive Japanese: a questionnaire survey. Pathophysiology 19:95–100
Kipen HM, Fiedler N (2002) Environmental factors in medically unexplained symptoms and related syndromes: the evidence and the challenge. Environ Health Perspect 110(Suppl 4):597–599
Kjellqvist A, Palmquist E, Nordin S (2016) Psychological symptoms and health-related quality of life in idiopathic environmental intolerance attributed to electromagnetic fields. J Psychosom Res 84:8–12
Knave BG, Wibom RI, Voss M, Hedström LD, Bergqvist UO (1985) Work with video display terminals among office employees. I. subjective symptoms and discomfort. Scand J Work Environ Health 11:457–466
Kwon MS, Hämäläinen H (2011) Effects of mobile phone electromagnetic fields: critical evaluation of behavioral and neurophysiological studies. Bioelectromagnetics 32:253–272
Levallois P, Neutra R, Lee G, Hristova L (2002) Study of self-reported hypersensitivity to electromagnetic fields in California. Environ Health Perspect 110(Suppl 4):619–623
Lyskov E, Sandström M, Hansson Mild K (2001) Neurophysiological study of patients with perceived “electrical hypersensitivity”. Int J Psychophysiol 42:233–241
Meg Tseng M-C, Lin Y-P, Cheng T-J (2011) Prevalence and psychiatric comorbidity of self-reported electromagnetic field sensitivity in Taiwan: a population-based study. J Formos Med Assoc 110:634–641
Nordin S, Neely G, Olsson D, Sandström M (2014) Odor and noise intolerance in persons with self-reported electromagnetic hypersensitivity. Int J Environ Res Public Health 11:8794–8805
Palmquist E, Claeson A-S, Neely G, Stenberg B, Nordin S (2014) Overlap in prevalence between various types of environmental intolerance. Int J Hyg Environ Health 217:427–434
Röösli M, Hug K (2011) Wireless communication fields and non-specific symptoms of ill health: a literature review. Wien Med Wochenschr 1946 161:240–250
Röösli M, Moser M, Baldinini Y, Meier M, Braun-Fahrländer C (2004) Symptoms of ill health ascribed to electromagnetic field exposure: a questionnaire survey. Int J Hyg Environ Health 207:141–150
Röösli M, Frei P, Mohler E, Hug K (2010) Systematic review on the health effects of exposure to radiofrequency electromagnetic fields from mobile phone base stations. Bull World Health Organ 88:887–896F
Rubin GJ, Das Munshi J, Wessely S (2006) A systematic review of treatments for electromagnetic hypersensitivity. Psychother Psychosom 75:12–18
Rubin GJ, Cleare AJ, Wessely S (2008) Psychological factors associated with self-reported sensitivity to mobile phones. J Psychosom Res 64:1–9-12
Rubin GJ, Nieto-Hernandez R, Wessely S (2010) Idiopathic environmental intolerance attributed to electromagnetic fields (formerly “electromagnetic hypersensitivity”): an updated systematic review of provocation studies. Bioelectromagnetics 31:1–11
Rubin GJ, Hillert L, Nieto-Hernandez R, van Rongen E, Oftedal G (2011) Do people with idiopathic environmental intolerance attributed to electromagnetic fields display physiological effects when exposed to electromagnetic fields? A systematic review of provocation studies. Bioelectromagnetics 32:593–609
Santini R, Santini P, Danze JM, Le Ruz P, Seigne M (2002) Investigation on the health of people living near mobile telephone relay stations: incidence according to distance and sex (in French). Pathol Biol (Paris) 50(6):369–373. Erratum in: Pathol Biol (Paris). 50(10):621
Schreier N, Huss A, Röösli M (2006) The prevalence of symptoms attributed to electromagnetic field exposure: a cross-sectional representative survey in Switzerland. Soz Praventivmed 51:202–209
van Dongen D, Smid T, Timmermans DRM (2014) Symptom attribution and risk perception in individuals with idiopathic environmental intolerance to electromagnetic fields and in the general population. Perspect Public Health 134:160–168
WHO (2006) Hansson Mild K, Repacholi M, van Deventer, Ravazzani P (Eds) Electromagnetic hypersensitivity. Proceedings from an international workshop on EMF Hypersensitivity, Prague, Czech Republic, Oct 27, 2004. WHO Library Cataloguing-in-Publication Data, WHO, Geneva
WHO Program on Traditional Medicine (2002) WHO traditional medicine strategy 2002–2005. World Health Organization, Geneva. Available from http://apps.who.int/iris/handle/10665/67163. Accessed 8 December 2015
Acknowledgements
The authors wish to warmly thank all the respondents for their participation, the members of French self-help and action groups, as well as the association representatives for sharing and communicating about the research, and the representatives of the “Collectif des Electrosensibles de France” for their invaluable assistance.
Funding
This work was fully funded by the French Agency for Food, Environmental and Occupational Health & Safety (ANSES); grant number: SENSI-RF EST-2013-002.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The protocol was approved by the ethics committee of the CPP Nord Ouest CHU Amiens, France (CPP, 2014/8).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
All authors declare have no conflict of interest.
Additional information
The original version of this article was revised: Due to the existence of another journal with the same name, the Publisher has added a subtitle, “From Theory to Practice.” Effective as of January 2018, the new title of this Journal is Journal of Public Health: From Theory to Practice.
Rights and permissions
About this article
Cite this article
Andrianome, S., De Seze, R., Braun, A. et al. Descriptive self-reporting survey of people with idiopathic environmental intolerance attributed to electromagnetic fields (IEI-EMF): similarities and comparisons with previous studies. J Public Health (Berl.) 26, 461–473 (2018). https://doi.org/10.1007/s10389-017-0886-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-017-0886-0