Abstract
Background
The relationship between gastroesophageal reflux disease (GERD) and constipation has not yet been examined in Japan. We herein analyzed the use of laxatives by GERD and non-GERD patients to clarify the relationship between GERD and constipation.
Methods
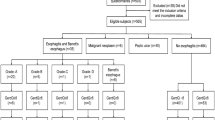
This was a retrospective observational study designed to examine the use of laxatives by GERD and non-GERD patients. A total of 118 patients (mean age 69.7 years, 50 males) with reflux esophagitis (RE) and non-erosive reflux disease (NERD) who received maintenance acid-suppressive therapy for more than 1 year were included in the GERD group (83 RE patients, 35NERD patients). Similarly, 61 patients (mean age 69.4 years, 28 males) who received regular acid-suppressive therapy for reasons other than GERD were included in the non-GERD group. We also investigated demographic factors associated with the onset of GERD, including body mass index (BMI), age, and sex.
Results
The frequency of laxative use was significantly higher in the GERD group (38.1%) than in the non-GERD group (21.3%). No significant differences were observed in dose frequencies between the groups. The type of laxative used also did not significantly differ between the groups. Furthermore, no significant differences were noted in sex, age, or BMI between the groups.
Conclusions
The use of laxatives was significantly more common in GERD patients than in non-GERD patients. The present results suggest that a relationship exists between GERD and constipation.

Similar content being viewed by others
References
Iwakiri K, Kinoshita Y, Habu Y, et al. Evidence-based clinical practice guidelines for gastroesophageal reflux disease 2015. J Gastroenterol. 2016;51:751–67.
Locke GR 3rd, Zinsmeister AR, Fett SL, et al. Overlap of gastrointestinal symptom complexes in a US community. Neurogastroenterol Motil. 2005;17:29–34.
Miwa H, Nakajima K, Yamaguchi K, et al. Generation of dyspeptic symptoms by direct acid infusion into the stomach of healthy Japanese subjects. Aliment Pharmacol Ther. 2007;26:257–64.
Lee KJ, Vos R, Janssens J, et al. Influence of duodenal acidification on the sensorimotor function of the proximal stomach in humans. Am J Physiol Gastrointest Liver Physiol. 2004;2086:G278–G284284.
Lacy BE, Mearin F, Chang L, et al. Bowel disorders. Gastroenterology. 2016;150:1393–407.
Furukawa N, Iwakiri R, Koyama T, et al. Proportion of reflux esophagitis in 6010 Japanese adults: prospective evaluation by endoscopy. J Gastroenterol. 1999;34:441–4.
Choung RS, Locke GR 3rd, Schleck CD, et al. Cumulative incidence of chronic constipation: a population-based study 1988–2003. Aliment Pharmacol Ther. 2007;26:1521–8.
Lee J, Anggiansah A, Anggiansah R, et al. Effects of age on the gastroesophageal junction, esophageal motility, and reflux disease. Clin Gastroenterol Hepatol. 2007;5:1392–8.
Madsen JL, Graff J. Effects of ageing on gastrointestinal motor function. Age Ageing. 2004;33:154–9.
Gunji T, Sato H, Iijima K, et al. Risk factors for erosive esophagitis: a cross-sectional study of a large number of Japanese males. J Gastroenterol. 2011;46:448–55.
Mizuta A, Adachi K, Furuta K, et al. Different sex-related influences of eating habits on the prevalence of reflux esophagitis in Japanese. J Gastroenterol Hepatol. 2011;26:1060–4.
Mittal RK, Holloway RH, Penagini R, et al. Transient lower esophageal sphincter relaxation. Gastroenterology. 1995;109:601–10.
Iwakiri K, Kawami N, Sano H, et al. Mechanisms of excessive esophageal acid exposure in patients with reflux esophagitis. Dig Dis Sci. 2009;54:1686–92.
Iwakiri K, Hayashi Y, Kotoyori M, et al. Transient lower esophageal sphincter relaxations (TLESRs) are the major mechanism of gastroesophageal reflux but are not the cause of reflux disease. Dig Dis Sci. 2005;50:1072–7.
Holloway RH, Hongo M, Berger K, et al. Gastric distention: a mechanism for postprandial reflux. Gastroenterology. 1985;89:779–84.
Wyman JB, Dent J, Heddle R, et al. Control of belching by the lower oesophageal sphincter. Gut. 1990;31:639–46.
Holloway RH, Lyrenas E, Ireland A, et al. Effect of intraduodenal fat on lower oesophageal sphincter function and gastro-oesophageal reflux. Gut. 1997;40:449–53.
Boulant J, Fioramonti J, Dapoigny M, et al. Cholecystokinin and nitric oxide in transient lower esophageal sphincter relaxation to gastric distention in dogs. Gastroenterology. 1994;107:1059–66.
Wu JC, Mui LM, Cheung CM, et al. Obesity is associated with increased transient lower esophageal sphincter relaxation. Gastroenterology. 2007;132:883–9.
Lembo A, Camilleri M. Chronic constipation. N Engl J Med. 2003;349:1360–8.
Acknowledgements
The authors thank Ms. Satoko Nishimura for her administrative assistance.
Author information
Authors and Affiliations
Contributions
EM: protocol design, data acquisition and analysis, and writing of the manuscript. MK: data acquisition and analysis. TT: data acquisition and analysis. YH: data acquisition. SH: data acquisition. NK: data acquisition. TK: data acquisition. AT: data acquisition. MK: data acquisition. KI: protocol design, data acquisition and analysis, and writing of the manuscript.
Corresponding author
Ethics declarations
Ethical Statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions.
Conflict of interest
Katsuhiko Iwakiri received lecture fees from Takeda Pharmaceutical Co., Ltd., Otsuka Pharmaceutical Co., Ltd., EA Pharma Co., Ltd., and Mochida Pharmaceutical Co., Ltd. The remaining authors declare that they have no conflicts of interest.
Informed consent
Informed consent or substitute for it was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Momma, E., Koeda, M., Tanabe, T. et al. Relationship between gastroesophageal reflux disease (GERD) and constipation: laxative use is common in GERD patients. Esophagus 18, 152–155 (2021). https://doi.org/10.1007/s10388-020-00770-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10388-020-00770-5