Abstract
Background
Serum osmolality levels are measured to determine acid–base and electrolyte imbalance in serum. In cases where measurement is not possible, the serum osmolality value can be calculated by various calculation methods. In this study, we compared the Worthley osmolality calculation method which is used most frequently mentioned in literature and the measurements made with vapor pressure osmometer used in our laboratory. We compared whether there was a difference between the results obtained by measurement and calculation method in different age groups.
Methods
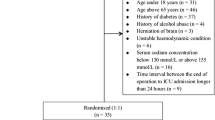
221 serum samples of patients who were admitted to the Eskişehir Osmangazi University Hospital Biochemistry Laboratory between December 2016 and May 2018 were included in this study. Glucose, blood urea nitrogen and sodium values were recorded to determine the calculated osmolality values of the patients.
Results
There was a statistically significant difference between the measured osmolality values and the calculated osmolality values of the patients (p < 0.001). When compared according to age groups, there was a significant difference between calculated osmolality values (p = 0.006), but there was no difference in measured osmolality values (p = 0.787) in different age groups. It has been observed that this difference in the calculated osmolality values between the age groups is derived from the adult group (18–65, p < 0.001).
Conclusion
Our results showed that it is not reliable to calculate serum osmolality values, especially in the adult age group. According to our results the calculated osmolality values are higher than our measured osmolality values.

Similar content being viewed by others
References
Rasouli M. Basic concepts and practical equations on osmolality: biochemical approach. Clin Biochem. 2016;49(12):936–41.
Knepper MA, Kwon TH, Nielsen S. Molecular physiology of water balance. N Engl J Med. 2015;372:1349–58.
Braun MM, Barstow CH, Pyzocha NJ. Diagnosis and management of sodium disorders: hyponatremia and hypernatremia. Am Fam Physician. 2015;91(5):299–307.
Faria DK, Mendes ME, Sumita NM. The measurement of serum osmolality and its application to clinical practice and laboratory: literature review. J Bras Patol Med Lab. 2017;53(1):38–45.
Arora A. The ‘gap’ in the ‘plasma osmolar gap’. BMJ Case Rep. 2013. https://doi.org/10.1136/bcr-2013-200250.
Wu AH, Yang HS, Thoren K. Biological variation of the osmolality and the osmolal gap. Clin Biochem. 2014;47(15):130–1.
Kruse JA, Cadnapaphornchai P. The serum osmole gap. J Crit Care. 1994;9(3):185–97.
Wrenn KD. Osmolality. Ann Intern Med. 1991;114:337–8.
Gennari FJ. Serum osmolality, uses and limitations. N Engl J Med. 1984;310:102–5.
Purssell RA, Lynd LD, Koga YT. The use of the osmole gap as a screening test for the presence of exogenous substances. Toxicol Rev. 2004;23:189–202.
Krasowski MD, Wilcoxon RM, Miron J. A retrospective analysis of glycol and toxic alcohol ingestion: utility of anion and osmolal gaps. BMC Clin Pathol. 2012;12:1.
Fazekas AS, Funk GC, Klobassa DS, Rüther H, Ziegler I, Zander R, Semmelrock HJ. Evaluation of 36 formulas for calculating plasma osmolality. Intensive Care Med. 2013;39(2):302–8.
Mccrow J, et al. Salt in the desert: a comparison of clinical versus serum-calculated osmolality determination of dehydration. Healthy Aging Res. 2016. https://doi.org/10.12715/har.2016.5.12.
Thomas DR, Cote TR, Lawhorne L, Levenson SA, Rubenstein LZ, Smith DA, et al. Understanding clinical dehydration and its treatment. J Am Med Directors Assoc. 2008;9(5):292–301.
Hooper L, Abdelhamid A, Ali A, Bunn DK, Jennings A, John WG, et al. Diagnostic accuracy of calculated serum osmolarity to predict dehydration in older people: adding value to pathology laboratory reports. BMJ Open. 2015;5(10):e008846.
Linderkamp O, et al. Estimation and prediction of blood volume in infants and children. Eur J Pediatr. 1977;125(4):227–34.
EFSA Panel On Dietetic Products, Nutrition, and Allergies (NDA). Scientific opinion on dietary reference values for water. EFSA J. 2010;8(3):1459.
United Nations, Department of Economic and Social Affairs, Population Division. World population prospects: the 2017 revision, key findings and advance tables. Working Paper No. ESA/P/WP/248. 2017.
Morley JE. Nutrition in older adults: dehydration, hypernatremia, and hyponatremia. Clin Geriatric Med. 2015;31(Issue 3):389–99.
Dorwart WV, Chalmers L. Comparison of methods for calculating serum osmolality from chemical concentrations, and prognostic value of such calculation. Clin Chem. 1975;21:190–4.
Bhagat CI, Garcia-Webb P, Fletcher E, Beilby JP. Calculated vs. measured plasma osmolality revisited. Clin Chem. 1984;30:1703–5.
Worthley LI, Guerin M, Pain RW. For calculating osmolality, the simplest formula is the best. Anesth Intensive Care. 1987;15:199–202.
Rasouli M, Kalantari KR. Comparison of methods for calculating serum osmolality: multivariate linear regression analysis. Clin Chem Lab Med. 2005;43:635–40.
Khajuria A, Krahn J. Osmolality revisited-deriving and validating the best formula for calculated osmolality. Clin Biochem. 2005;38:514–9.
Martín-Calderón JL, Bustos F, Tuesta-Reina LR, Varona JM, Caballero L, Solano F. Choice of the best equation for plasma osmolality calculation: comparison of fourteen formulae. Clin Biochem. 2015;48:529–33.
Siervo M, Bunn D, Prado CM, Hooper L. Accuracy of prediction equations for serum osmolarity in frail older people with and without diabetes. Am J Clin Nutr. 2014;100:867–76.
Scott MG, LeGrys VA, Hood JH. Electrolytes and blood gases. In: Burtis CA, Ashwood ER, Bruns DE, editors. Tietz textbook of clinical chemistry andmolecular diagnosis. 5th ed. Philadelphia: WB Saunders; 2012. p. 807–49.
Siperstein MD. Diabetic ketoacidosis and hyperosmolar coma. Endo Metabol Clin N Am. 1995;21:415–32.
Thornton SN. Thirst and hydration: physiology and consequences of dysfunction. Physiol Behav. 2010;100(1):15–21.
Bardis CN, et al. Mild hypohydration decreases cycling performance in the heat. Med Sci Sports Exerc. 2013;45(9):1782–9.
Kavouras SA, et al. Validation of a urine color scale for assessment of urine osmolality in healthy children. Eur J Nutr. 2016;55(3):907–15.
Manz F, Wentz A. 24-h hydration status: parameters, epidemiology and recommendations. Eur J Clin Nutr. 2003;57(S2):S10.
Stookey JD, et al. What is the cell hydration status of healthy children in the USA? Preliminary data on urine osmolality and water intake. Public health nutrition. 2012;15(11):2148–56.
Perrier E, et al. Hydration biomarkers in free-living adults with different levels of habitual fluid consumption. Br J Nutr. 2013;109(9):1678–87.
Perrier E, et al. Circadian variation and responsiveness of hydration biomarkers to changes in daily water intake. Eur J Appl Physiol. 2013;113(8):2143–51.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no conflict of interest exists.
Ethics standard
This study was approved by Eskişehir Osmangazi University Non-Interventional Ethics Committee (Decision number: 2019/25).
Informed consent
Informed consent was not required because of the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kar, E., Kocatürk, E., Küskü Kiraz, Z. et al. Comparison of measured and calculated osmolality levels. Clin Exp Nephrol 24, 444–449 (2020). https://doi.org/10.1007/s10157-020-01848-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-020-01848-1