Abstract
Background
To clarify the clinical as well as pathological outcomes in Japanese women with germline pathogenic BRCA1/2 variants who underwent risk-reducing salpingo-oophorectomy (RRSO).
Methods
This prospective study examined the rate of occult cancer and primary peritoneal cancer after RRSO at our institution in the period from 2011 to 2020. Clinical records of genetically confirmed patients with germline pathogenic BRCA1/2 variants who desired to undergo RRSO were reviewed. Specimens obtained during RRSO were pathologically diagnosed as per SEE-FIM protocol. All the participants underwent magnetic resonance imaging (MRI) about 1 month preoperatively.
Results
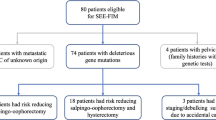
One hundred and seventeen women underwent RRSO during this period. Of these, the numbers of women with germline pathogenic BRCA1 and BRCA2 variants were 72 and 45, respectively. The mean observational time after RRSO was 35.8 months. Despite negative preoperative screening results, three (2.6%) serous tubal intraepithelial carcinoma and three (2.6%) invasive carcinomas were identified. Of the three invasive carcinomas cases, two were International Federation of Gynecology and Obstetrics (FIGO) stage I primary fallopian tube cancer, and the third case was double cancer (ovarian cancer and fallopian tube cancer) with FIGO stage IC3.
Conclusions
The rate of occult neoplasms was similar to those reported by studies performed in other countries. Although women with occult cancer were diagnosed with FIGO stage I, the MRI performed 1 month preoperatively did not show any such malignant findings. Thus, RRSO is the only promising method that can improve the prognosis in women with germline pathogenic BRCA1/2 variants.




Similar content being viewed by others
References
Chen S, Parmigiani G (2007) Meta-analysis of BRCA1 and BRCA2 penetrance. J Clin Oncol 25:1329–1333
Chen J, Bae E, Zhang L et al (2020) Penetrance of breast and ovarian cancer in women who carry a BRCA1/2 mutation and do not use risk-reducing salpingo-oophorectomy: an updated meta-analysis. JNCI Cancer Spectr. https://doi.org/10.1093/jncics/pkaa029
Alsop K, Fereday S, Meldrum C et al (2012) BRCA mutation frequency and patterns of treatment response in BRCA mutation-positive women with ovarian cancer: a report from the Australian Ovarian Cancer Study Group. J Clin Oncol 30:2654–2663
Enomoto T, Aoki D, Hattori K et al (2019) The first Japanese nationwide multicenter study of BRCA mutation testing in ovarian cancer: CHARacterizing the cross-sectionaL approach to Ovarian cancer genetic Testing of BRCA (CHARLOTTE). Int J Gynecol Cancer 29:1043–1049
McLaughlin JR, Rosen B, Moody J et al (2013) Long-term ovarian cancer survival associated with mutation in BRCA1 or BRCA2. J Natl Cancer Inst 105:141–148
Biglia N, Sgandurra P, Bounous VE et al (2016) Ovarian cancer in BRCA1 and BRCA2 gene mutation carriers: analysis of prognostic factors and survival. Ecancermedicalscience 10:639. https://doi.org/10.3332/ecancer.2016.639.eCollection2016
Kim SI, Lee M, Kim HS et al (2019) Effect of BRCA mutational status on survival outcome in advanced-stage high-grade serous ovarian cancer. J Ovarian Res 12:40. https://doi.org/10.1186/s13048-019-0511-7
Kotsopoulos J, Rosen B, Fan I et al (2016) Ten-year survival after epithelial ovarian cancer is not associated with BRCA mutation status. Gynecol Oncol 140:42–47
Olivier RI, Lubsen-Brandsma MA, Verhoef S et al (2006) CA125 and transvaginal ultrasound monitoring in high-risk women cannot prevent the diagnosis of advanced ovarian cancer. Gynecol Oncol 100:20–26
Stirling D, Evans DG, Pichert G et al (2005) Screening for familial ovarian cancer: failure of current protocols to detect ovarian cancer at an early stage according to the international federation of gynecology and obstetrics system. J Clin Oncol 23:5586–5596
van Nagell JR Jr, Miller RW, DeSimone CP et al (2011) Long-term survival of women with epithelial ovarian cancer detected by ultrasonographic screening. Obstet Gynecol 118:1212–1221
Domchek SM, Friebel TM, Singer CF et al (2010) Association of risk-reducing surgery in BRCA1 or BRCA2 mutation carriers with cancer risk and mortality. JAMA 304:967–975
Rebbeck TR, Kauff ND, Domchek SM (2009) Meta-analysis of risk reduction estimates associated with risk-reducing salpingo-oophorectomy in BRCA1 or BRCA2 mutation carriers. J Natl Cancer Inst 21:80–87
Finch AP, Lubinski J, Moller P et al (2014) Impact of oophorectomy on cancer incidence and mortality in women with a BRCA1 or BRCA2 mutation. J Clin Oncol 32:1547–1553
Lee Y, Medeiros F, Kindelberger D et al (2006) Advances in the recognition of tubal intraepithelial carcinoma: applications to cancer screening and the pathogenesis of ovarian cancer. Adv Anat Pathol 13:1–7
Nomura H, Sekine M, Yokoyama S et al (2019) Clinical background and outcomes of risk-reducing salpingo-oophorectomy fir hereditary breast and ovarian cancers in Japan. Int J Clin Oncol 24:1105–1110
National Comprehensive Cancer Network (NCCN) clinical practice guidelines in oncology. Geneic/Familyial High-Risk Assessment: Breast, Ovarian, and Pancreatic. Version 1.2022. https://www.nccn.org/professionals/physician_gls/pdf/genetics_bop.pdf. Accessed 11 Jan 2021
Garcia C, Wendt J, Lyon L et al (2014) Risk management options elected by women after testing positive for a BRCA mutation. Gynecol Oncol 32:428–433
Lee YJ, Lee SW, Kim KR et al (2017) Pathologic findings at risk-reducing salpingo-oophorectomy (RRSO) in germline BRCA mutation carriers with breast cancer: significance of bilateral RRSO at the optimal age in germline BRCA mutation carriers. J Gynecol Oncol 28:e3. https://doi.org/10.3802/jgo.2017.28.e3
Shigehiro M, Kita M, Takeuchi S et al (2016) Study on the psychosocial aspects of risk-reducing salpingo-oophorectomy (RRSO) in BRCA1/2 mutation carriers in Japan: a preliminary report. Jpn J Clin Oncol 46:254–259
Kobayashi Y, Hirasawa A, Chiyoda T et al (2021) Retrospective evaluation of risk-reducing salpingo-oophorectomy for BRCA1/2 pathogenic variant carriers among a cohort study in a single institution. Jpn J Clin Oncol 51:213–217
Arai M, Yokoyama S, Watanabe C et al (2018) Genetic and clinical characteristics in Japanese hereditary breast and ovarian cancer: first report after establishment of HBOC registration system in Japan. J Hum Genet 64:447–457
Sherman ME, Piedmonte M, Mai PL et al (2014) Pathologic findings at risk-reducing salpingo-oophorectomy: primary results from gynecologic oncology group trial GOG-0199. J Clin Oncol 32:3275–3283
Powel CB, Chen LM, McLennan J et al (2011) Risk-reducing salpingo-oophorectomy (RRSO) in BRCA mutation carriers: experience with a consecutive series of 111 patients using a standardized surgical-pathological protocol. Int J Gynecol Cancer 21:846–851
Shu CA, Pike MC, Jotwani AR et al (2016) Uterine cancer after risk-reducing salpingo-oophorectomy without hysterectomy in women with BRCA mutations. JAMA Oncol 2:1134–1140
Laitman Y, Michaelson-Cohen R, Levi E et al (2019) Uterine cancer in Jewish Israeli BRCA1/2 mutation carriers. Cancer 125:698–703
Acknowledgements
We thank Dr, Masami Arai, Dr. Reiko Yoshida, Keika Kaneko, Hiromi Arakawa, Eri Habano, Mizuho Kita and Yuumi Ashihara for their cooperation for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no disclosures for this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Nomura, H., Ikki, A., Fusegi, A. et al. Clinical and pathological outcomes of risk-reducing salpingo-oophorectomy for Japanese women with hereditary breast and ovarian cancer. Int J Clin Oncol 26, 2331–2337 (2021). https://doi.org/10.1007/s10147-021-02020-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-021-02020-9