Abstract
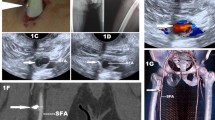
To assess the sensitivity of detecting the most commonly encountered foreign bodies in Emergency Radiology using all imaging modalities (conventional radiography, computed tomography, ultrasound, and magnetic resonance imaging). The following materials were inserted into a pig-leg phantom and imaged using conventional radiography, computed tomography, ultrasound, and magnetic resonance imaging: Plastics #1, 2, 3, 5, and compostable plastic; dry and wet wood, aluminum, gravel, glass (tinted and non-tinted), and Salmon and Halibut fish bones. The visibility of plastic is variable on both conventional radiography and computed tomography, depending on composition, but all types of plastic are well visualized on ultrasound. Wood is most easily identified and localized on both computed tomography and ultrasound, is only faintly visible on conventional radiography, and is not well visualized on magnetic resonance imaging. Gravel, glass, and aluminum are well visualized on all modalities, with the exception of magnetic resonance imaging, where there is significant artifact surrounding the foreign body. Fish bones (Halibut and Salmon) are well visualized on conventional radiography, computed tomography, and ultrasound. Conventional radiography and computed tomography are great modalities for detecting foreign bodies of various compositions. Computed tomography is particularly useful at localizing the foreign body and determining its relationship to surrounding structures and its depth of involvement. All foreign bodies are visualized on ultrasound if the location is known and the foreign body is in the plane of the transducer. Magnetic resonance imaging is not helpful in detecting foreign bodies.








Similar content being viewed by others
References
Ariz C, Horton KM, Fishman EK (2004) 3D CT evaluation of retained foreign bodies. Emerg Radiol 11(2):95–99
Braham R, Said M, Jerbi Ommezine S, Gannouni A (2005) Foreign bodies in the soft tissues. The interest of sonography. Presse Med 34(3):256
Callegari L, Leonardi A, Bini A, Sabato C, Nicotera P, Spano E et al (2009) Ultrasound-guided removal of foreign bodies: personal experience. Eur Radiol 19(5):1273–1279
Peterson JJ, Bancroft LW, Kransdorf MJ (2002) Wooden foreign bodies: imaging appearance. AJR Am J Roentgenol 178(3):557–562
Teltzrow T, Hallermann C, Muller S, Schwipper V (2006) Foreign body-induced angiosarcoma 60 years after a shell splinter injury. Mund-, Kiefer- und Gesichtschirurgie MKG 10(6):415–418
Dumarey A, De Maeseneer M, Ernst C (2004) Large wooden foreign body in the hand: recognition of occult fragments with ultrasound. Emerg Radiol 10(6):337–339
Valente JH, Lemke T, Ridlen M, Ritter D, Clyne B, Reinert SE (2005) Aluminum foreign bodies: do they show up on X-ray? Emerg Radiol 12(1–2):30–33
Ho VT, McGuckin JF Jr, Smergel EM (1996) Intraorbital wooden foreign body: CT and MR appearance. AJNR Am J Neuroradiol 17(1):134–136
Yamashita K, Noguchi T, Mihara F, Yoshiura T, Togao O, Yoshikawa H et al (2007) An intraorbital wooden foreign body: description of a case and a variety of CT appearances. Emerg Radiol 14(1):41–43
de Santana Santos T, Avelar RL, Melo AR, de Moraes HH, Dourado E (2011) Current approach in the management of patients with foreign bodies in the maxillofacial region. J Oral Maxillofac Surg: Off J Am Assoc Oral Maxillofac Surg 69(9):2376–2382
Specht CS, Varga JH, Jalali MM, Edelstein JP (1992) Orbitocranial wooden foreign body diagnosed by magnetic resonance imaging. Dry wood can be isodense with air and orbital fat by computed tomography. Surv Ophthalmol 36(5):341–344
SPI Resin Identification Code—guide to correct use: Society of the Plastics Industry, Plastics Industry Trade Association; 2014 [updated 2014; cited 2015 1/15/15]. Available from: http://www.plasticsindustry.org/AboutPlastics/content.cfm?ItemNumber=823
Halverson M, Servaes S (2013) Foreign bodies: radiopaque compared to what? Pediatr Radiol 43(9):1103–1107
Maizlin ZV, Vos PM, Lee A, Syed NS, Anaspure RS, Mah JY et al (2012) Stone foreign body—radiographic and CT appearance. Emerg Radiol 19(4):317–322
Weiss CR, Fishman EK (2005) Multidetector 3D CT of pulmonary embolism of a peripheral intravenous line. Emerg Radiol 11(4):247–249
Khalil PN, Huber-Wagner S, Regauer M, Thun H, Kanz KG, Mutschler W (2010) Identification and removal of subcutaneous foreign bodies. MMW Fortschritte der Medizin 152(10):38–40
Conflict of interest
The authors have no conflicts of interest or financial relationships to disclose related to the presented material.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ingraham, C.R., Mannelli, L., Robinson, J.D. et al. Radiology of foreign bodies: how do we image them?. Emerg Radiol 22, 425–430 (2015). https://doi.org/10.1007/s10140-015-1294-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-015-1294-9