Abstract
Objective
We developed a detailed imaging phenotype of the cerebral complications in critically ill patients with infective endocarditis (IE) and determine whether any specific imaging pattern could impact prognostic information.
Methods
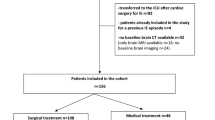
One hundred ninety-two patients admitted to the intensive care units of seven tertiary centers with severe, definite left IE and neurological complications were included. All underwent cerebral imaging few days after admission to define the types of lesions, their volumes, and their locations using voxel-based lesion-symptom mapping (VLSM). We employed uni- and multi-variate logistic regression analyses to explore the associations among imaging features and other prognostic variables and the 6-month modified Rankin Scale (mRS) score.
Results
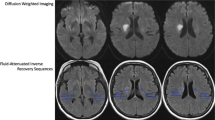
Ischemic lesions were the most common lesions (75%; mean volume, 15.3 ± 33 mL) followed by microbleeds (50%; mean number, 4 ± 7.5), subarachnoidal hemorrhages (20%), hemorrhagic strokes (16%; mean volume, 14.6 ± 21 mL), and hemorrhagic transformations (10%; mean volume, 5.6 ± 11 mL). The volume of hemorrhagic transformations, the severity of leukopathy, and the compromises of certain locations on the motor pathway from the VLSM were associated with a poor 6-month mRS score on univariate analyses. However, upon multivariate analyses, no such specific imaging pattern independently predicted the mRS; this was instead influenced principally by age (OR = 1.03 [1.004–1.06]) and cardiac surgery status (OR = 0.06 [0.02–0.16]) in the entire cohort, and by age (OR = 1.04 [1.01–1.08]) and Staphylococcus aureus status (OR = 2.86 [1.19–6.89]) in operated patients.
Conclusions
In a cohort of severely ill IE patients with neurological complications, no specific imaging pattern could be highlighted as a reliable predictor of prognosis.



Similar content being viewed by others
Data availability
The datasets used during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
Abbreviations
- ADC:
-
Apparent diffusion coefficient
- DWI:
-
Diffusion-weighted imaging
- ESC:
-
European Society of Cardiology
- FLAIR:
-
Fluid-attenuated inversion recovery
- ICE-COCA:
-
InfeCtious Endocarditis with Cerebral cOmplications: a Cohort from French reAnimations
- ICU:
-
Intensive care unit
- IE:
-
Infective endocarditis
- IIA:
-
Infectious intracranial aneurysm
- mRS:
-
Modified Rankin Scale
- SAH:
-
Subarachnoidal hemorrhage
- SOFA:
-
Sequential organ failure assessment
- VLSM:
-
Voxel-based lesion symptom mapping
References
Cahill TJ, Prendergast BD (2016) Infective endocarditis. Lancet 387(10021):882–893
Murdoch DR et al (2009) Clinical presentation, etiology, and outcome of infective endocarditis in the 21st century: the International Collaboration on Endocarditis-Prospective Cohort Study. Arch Intern Med 169(5):463–473
Habib G et al (2015) 2015 ESC Guidelines for the management of infective endocarditis: The Task Force for the Management of Infective Endocarditis of the European Society of Cardiology (ESC). Endorsed by: European Association for Cardio-Thoracic Surgery (EACTS), the European Association of Nuclear Medicine (EANM). Eur Heart J 36(44):3075–3128
Garcia-Cabrera E et al (2013) Neurological complications of infective endocarditis: risk factors, outcome, and impact of cardiac surgery: a multicenter observational study. Circulation 127(23):2272–2284
Sonneville R et al (2011) Neurologic complications and outcomes of infective endocarditis in critically ill patients: the ENDOcardite en REAnimation prospective multicenter study. Crit Care Med 39(6):1474–1481
Habib G et al (2019) Clinical presentation, aetiology and outcome of infective endocarditis. Results of the ESC-EORP EURO-ENDO (European infective endocarditis) registry: a prospective cohort study. Eur Heart J 40(39):3222–3232
Iung B et al (2013) Determinants of cerebral lesions in endocarditis on systematic cerebral magnetic resonance imaging: a prospective study. Stroke 44(11):3056–3062
Vogt G et al (2012) Initial lesion volume is an independent predictor of clinical stroke outcome at day 90: an analysis of the Virtual International Stroke Trials Archive (VISTA) database. Stroke 43(5):1266–1272
Broderick JP et al (1993) Volume of intracerebral hemorrhage. A powerful and easy-to-use predictor of 30-day mortality. Stroke 24(7):987–93
Wu O et al (2015) Role of acute lesion topography in initial ischemic stroke severity and long-term functional outcomes. Stroke 46(9):2438–2444
Appleton JP et al (2020) Imaging markers of small vessel disease and brain frailty, and outcomes in acute stroke. Neurology 94(5):e439–e452
Ryu WS et al (2017) Stroke outcomes are worse with larger leukoaraiosis volumes. Brain 140(1):158–170
Kang DH et al (2012) Early surgery versus conventional treatment for infective endocarditis. N Engl J Med 366(26):2466–2473
Wilbring M et al (2014) The impact of preoperative neurological events in patients suffering from native infective valve endocarditis. Interact Cardiovasc Thorac Surg 18(6):740–747
Yoshioka D et al (2012) Impact of early surgical treatment on postoperative neurologic outcome for active infective endocarditis complicated by cerebral infarction. Ann Thorac Surg 94(2):489–95; discussion 496
Fazekas F et al (1987) MR signal abnormalities at 1.5 T in Alzheimer’s dementia and normal aging. AJR Am J Roentgenol 149(2):351–6
Rudilosso S et al (2017) Evaluation of white matter hypodensities on computed tomography in stroke patients using the Fazekas score. Clin Imaging 46:24–27
Greenberg SM et al (2009) Cerebral microbleeds: a guide to detection and interpretation. Lancet Neurol 8(2):165–174
Bates E et al (2003) Voxel-based lesion-symptom mapping. Nat Neurosci 6(5):448–450
Rorden C, Karnath HO, Bonilha L (2007) Improving lesion-symptom mapping. J Cogn Neurosci 19(7):1081–1088
Tzourio-Mazoyer N et al (2002) Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. Neuroimage 15(1):273–289
Munsch F et al (2016) Stroke location is an independent predictor of cognitive outcome. Stroke 47(1):66–73
Janssen PM et al (2010) Comparison of telephone and face-to-face assessment of the modified Rankin Scale. Cerebrovasc Dis 29(2):137–139
Broderick JP, Adeoye O, Elm J (2017) Evolution of the modified Rankin Scale and its use in future stroke trials. Stroke 48(7):2007–2012
Hess A et al (2013) Brain MRI findings in neurologically asymptomatic patients with infective endocarditis. AJNR Am J Neuroradiol 34(8):1579–1584
Goulenok T et al (2013) Infective endocarditis with symptomatic cerebral complications: contribution of cerebral magnetic resonance imaging. Cerebrovasc Dis 35(4):327–336
Kidwell CS et al (2004) Comparison of MRI and CT for detection of acute intracerebral hemorrhage. JAMA 292(15):1823–1830
Di Salvo G et al (2001) Echocardiography predicts embolic events in infective endocarditis. J Am Coll Cardiol 37(4):1069–1076
Johnston KC et al (2007) Validation of an acute ischemic stroke model: does diffusion-weighted imaging lesion volume offer a clinically significant improvement in prediction of outcome? Stroke 38(6):1820–1825
Cheng B et al (2014) Influence of stroke infarct location on functional outcome measured by the modified rankin scale. Stroke 45(6):1695–1702
Duval X et al (2010) Effect of early cerebral magnetic resonance imaging on clinical decisions in infective endocarditis: a prospective study. Ann Intern Med 152(8):497–504, W175
Author information
Authors and Affiliations
Consortia
Contributions
T. T. and A. B. designed the study. Y. O. G., A. G., and H. F. collected the data. Y. O. G., H. F., and T. T. wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Retrospective database construction was approved by our local ethics committee (approval no. CE-SRLF-15–54) and the national data protection authority (declaration no. 2082557 v0) and complied with all dictates of the European Union General Data Protection Regulation in terms of protection of personal health data and personal information.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Pr. Boyer and Pr. Tourdias jointly directed this work and share co-senior authorship.
A complete list of ICE-COCA investigators can be found in the Appendix at the end of the manuscript.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Expanded materials and methods
Supplemental tables I and II
Appendix
Appendix
The ICE-COCA research investigators:
Bordeaux University Hospital: Pr. BOYER Alexandre, Pr. GRUSON Didier and Dr. GROS Alexandre, Service de Médecine Intensive Réanimation, Pr. COSTE Pierre and Dr. SEGUY Benjamin, Soins intensifs de cardiologie, Hôpital Cardiologique du Haut-Lévêque, Pr. TOURDIAS Thomas and Dr. GUETTARD Yves-Olivier, Service de Neuroradiologie.
Clermont-Ferrand University Hospital: Dr. SOUWEINE Bertrand and Dr. COUPEZ Elisabeth, Médecine intensive et réanimation.
Lille University Hospital: Pr. PREAU Sébastien, Pr. NSEIR Saad and Dr. TOUSSAINT Aurélia, Réanimation médicale, Dr. OUTTERYCK Olivier, service de neuroradiologie.
Nantes University Hospital: Pr. REIGNIER Jean and Dr. MAREST Delphine, Service d’Anesthésie-Réanimation.
Poitiers University Hospital: Pr. ROBERT René and Dr. COUDROY Rémi, Médecine Intensive Réanimation.
Rennes University Hospital: Dr. MARTINS Raphaël, Cardiologie et maladies vasculaires, and Dr. URIEN Jean Marie, service de cardiologie, groupe hospitalier Bretagne sud.
Toulouse University Hospital: Dr. PORTE Lydie, Département de maladies infectieuses; Dr. LAVIE-BADIE Yoan, Dr. ROBIN Guillaume and Dr. CHARBONNIER Gaëtan, Centre expert de la valve, fédération de cardiologie; Dr. SARTON Benjamine and Pr. SILVA Stein, Réanimation polyvalente adultes.
Rights and permissions
About this article
Cite this article
Guettard, YO., Gros, A., Fukutomi, H. et al. Brain imaging determinants of functional prognosis after severe endocarditis: a multicenter observational study. Neurol Sci 43, 3759–3768 (2022). https://doi.org/10.1007/s10072-021-05789-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05789-9