Abstract
Introduction
Resistance training (RT) is well tolerated and has shown promise for decreasing fatigue. However, the effects of RT have never been examined in primary Sjogren’s syndrome (pSS).
Objective
To assess the feasibility, effectiveness, and safety of a resistance exercise program on fatigue in patients with pSS.
Methods
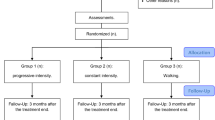
This is a parallel, single-blind randomized trial. Women aged 18 years or older, diagnosed with pSS according to the American-European criteria, were included. We randomized 59 participants to a resistance training group (RT) or a control group (CG). Participants in the RT group performed a 16-week resistance exercise program. The sessions consisted of three sets of resistance exercises (10 repetitions each) at 60 to 80% of 1 repetition maximum, designed to improve whole-body strength. The participants in the CG received their usual pharmacological treatment and instructions regarding disease control, pain management, sleep hygiene, and activities of daily living. To compare intergroup and intragroup variability, a one-factor repeated-measures analysis of variance (ANOVA) was used.
Results
RT effectively improved fatigue, pain, functional capacity, emotional aspects, vitality, and subjective perception of disease activity by the patient. No between-group differences were found in the ESSPRI mental score, ESSDAI, SF-36-Physical Aspects, SF-36-General Health, SF-36-Social aspects, and SF-36-Mental Health after the training period.
Conclusion
An RT program was safe and effective in improving fatigue, pain, functional capacity, emotional aspects, vitality, and subjective perception of disease activity by the patient in women with pSS.
Key Points • This is the first study to evaluate the effects of a resistance training program on fatigue in patients with primary Sjogren’s syndrome. • A resistance training program was shown to be effective in improving fatigue in patients with primary Sjogren’s syndrome. • A resistance training program is well-tolerated, has good compliance, and is not associated with serious adverse effects in patients with primary Sjogren’s syndrome. |

Similar content being viewed by others
References
Qin B, Wang J, Yang Z, Yang M, Ma N, Huang F et al (2015) Epidemiology of primary Sjögren’s syndrome: a systematic review and meta-analysis. Ann Rheum Dis 74(11):1983–1989
Mandl T, Jørgensen TS, Skougaard M, Olsson P, Kristensen L-E (2017) Work disability in newly diagnosed patients with primary Sjögren syndrome. J Rheumatol 44(2):209–215 Available from: http://www.jrheum.org/lookup/doi/10.3899/jrheum.160932
Wang S-Q, Zhang L-W, Wei P, Hua H (2017) Is hydroxychloroquine effective in treating primary Sjogren’s syndrome: a systematic review and meta-analysis. BMC Musculoskelet Disord 18(1):186
Hartkamp A, Geenen R, Godaert GLR, Bootsma H, Kruize AA, Bijlsma JWJ et al (2008) Effect of dehydroepiandrosterone administration on fatigue, well-being, and functioning in women with primary Sjogren syndrome: a randomised controlled trial. Ann Rheum Dis 67(1):91–97 Available from: http://ard.bmj.com/cgi/doi/10.1136/ard.2007.071563
Price EJ, Rigby SP, Clancy U, Venables PJ (1998) A double blind placebo controlled trial of azathioprine in the treatment of primary Sjogren’s syndrome. J Rheumatol 25(5):896–899
van Woerkom JM, Kruize AA, Geenen R, van Roon EN, Goldschmeding R, Verstappen SMM et al (2007) Safety and efficacy of leflunomide in primary Sjogren’s syndrome: a phase II pilot study. Ann Rheum Dis 66(8):1026–1032
Mariette X, Ravaud P, Steinfeld S, Baron G, Goetz J, Hachulla E et al (2004) Inefficacy of infliximab in primary Sjögren’s syndrome: results of the randomized, controlled Trial of Remicade in Primary Sjögren’s Syndrome (TRIPSS). Arthritis Rheum 50(4):1270–1276
Bowman SJ, Everett CC, O’Dwyer JL, Emery P, Pitzalis C, Ng W-F et al (2017) Randomized controlled trial of rituximab and cost-effectiveness analysis in treating fatigue and oral dryness in primary Sjogren’s syndrome. Arthritis Rheumatol (Hoboken, NJ) 69(7):1440–1450
Price EJ, Rauz S, Tappuni AR, Sutcliffe N, Hackett KL, Barone F et al (2017) The British Society for Rheumatology guideline for the management of adults with primary Sjögren’s Syndrome. Rheumatology (Oxford) 56(10):1828
Strömbeck BE, Theander E, Jacobsson LTH (2007) Effects of exercise on aerobic capacity and fatigue in women with primary Sjogren’s syndrome. Rheumatology (Oxford) 46(5):868–871
Miyamoto ST, Valim V, Carletti L, Ng W-F, Perez AJ, Lendrem DW et al (2019) Supervised walking improves cardiorespiratory fitness, exercise tolerance, and fatigue in women with primary Sjögren’s syndrome: a randomized-controlled trial. Rheumatol Int 39(2):227–238
Andrade A, de Azevedo Klumb Steffens R, Sieczkowska SM, Peyré Tartaruga LA, Torres Vilarino G (2018) A systematic review of the effects of strength training in patients with fibromyalgia: clinical outcomes and design considerations. Adv Rheumatol (London, England) 58(1):36
Schmidt ME, Wiskemann J, Armbrust P, Schneeweiss A, Ulrich CM, Steindorf K (2015) Effects of resistance exercise on fatigue and quality of life in breast cancer patients undergoing adjuvant chemotherapy: a randomized controlled trial. Int J Cancer 137(2):471–480
Dodd KJ, Taylor NF, Shields N, Prasad D, McDonald E, Gillon A (2011) Progressive resistance training did not improve walking but can improve muscle performance, quality of life and fatigue in adults with multiple sclerosis: a randomized controlled trial. Mult Scler 17(11):1362–1374
Vitali C, Bombardieri S, Jonsson R, Moutsopoulos HM, Alexander EL, Carsons SE et al (2002) Classification criteria for Sjögren’s syndrome: a revised version of the European criteria proposed by the American-European Consensus Group. Ann Rheum Dis 61(6):554–558
Miyamoto ST, Paganotti MA, Serrano ÉV, Giovelli RA, Valim V (2015) Assessment of fatigue and dryness in primary Sjögren’s syndrome: Brazilian version of “Profile of Fatigue and Discomfort - Sicca Symptoms Inventory (short form) (PROFAD-SSI-SF)”. Rev Bras Reumatol 55(2):113–122
Webster K, Cella D, Yost K (2003) The Functional Assessment of Chronic Illness Therapy (FACIT) measurement system: properties, applications, and interpretation. Health Qual Life Outcomes 1:79
Seror R, Ravaud P, Mariette X, Bootsma H, Theander E, Hansen A et al (2011) EULAR Sjogren’s Syndrome Patient Reported Index (ESSPRI): development of a consensus patient index for primary Sjogren’s syndrome. Ann Rheum Dis 70(6):968–972
Ware JEJ (2000) SF-36 health survey update. Spine (Phila Pa 1976) 25(24):3130–3139
Pinto ACPN, Piva SR, da Silva Vieira AG, Gomes SGCN, Rocha AP, Tavares DRB et al (2021) Transcranial direct current stimulation for fatigue in patients with Sjogren’s syndrome: a randomized, double-blind pilot study. Brain Stimul 14(1):141–151
Grote M, Maihöfer C, Weigl M, Davies-Knorr P, Belka C (2018) Progressive resistance training in cachectic head and neck cancer patients undergoing radiotherapy: a randomized controlled pilot feasibility trial. Radiat Oncol 13(1):215
Mengshoel AM, Norheim KB, Omdal R (2014) Primary Sjögren’s syndrome: fatigue is an ever-present, fluctuating, and uncontrollable lack of energy. Arthritis Care Res 66(8):1227–1232
Stack RJ, Southworth S, Fisher BA, Barone F, Buckley CD, Rauz S et al (2017) A qualitative exploration of physical, mental and ocular fatigue in patients with primary Sjögren’s Syndrome. PLoS One 12(10):1–11
Godaert GLR, Hartkamp A, Geenen R, Garssen A, Kruize AA, Bijlsma JWJ et al (2002) Fatigue in daily life in patients with primary Sjögren’s syndrome and systemic lupus erythematosus. Ann N Y Acad Sci 966:320–326
Thorn L, Hucklebridge F, Evans P, Clow A (2009) The cortisol awakening response, seasonality, stress and arousal: a study of trait and state influences. Psychoneuroendocrinology. 34(3):299–306
Mavragani CP, Fragoulis GE, Moutsopoulos HM (2012) Endocrine alterations in primary Sjogren’s syndrome: an overview. J Autoimmun 39(4):354–358. Available from: https://doi.org/10.1016/j.jaut.2012.05.011
Harboe E, Tjensvoll AB, Vefring HK, Gøransson LG, Kvaløy JT, Omdal R (2009) Fatigue in primary Sjögren’s syndrome--a link to sickness behaviour in animals? Brain Behav Immun 23(8):1104–1108
Bårdsen K, Brede C, Kvivik I, Kvaløy JT, Jonsdottir K, Tjensvoll AB et al (2019) Interleukin-1-related activity and hypocretin-1 in cerebrospinal fluid contribute to fatigue in primary Sjögren’s syndrome. J Neuroinflammation 16(1):102
D’Elia HF, Bjurman C, Rehnberg E, Kvist G, Konttinen YT (2009) Interleukin 6 and its soluble receptor in a central role at the neuroimmunoendocrine interface in Sjögren syndrome: an explanatory interventional study. Ann Rheum Dis 68(2):285–286
Zheng L, Zhang Z, Yu C, Tu L, Zhong L, Yang C (2009) Association between IFN-alpha and primary Sjogren’s syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 107(1):e12–e18
Nicklas BJ, Brinkley TE (2009) Exercise training as a treatment for chronic inflammation in the elderly. Exerc Sport Sci Rev 37(4):165–170
Walsh NP, Gleeson M, Shephard RJ, Gleeson M, Woods JA, Bishop NC et al (2011) Position statement. Part one: immune function and exercise. Exerc Immunol Rev 17:6–63
Pereira Nunes Pinto AC, Natour J, de Moura Castro CH, Eloi M, Lombardi Junior I (2017) Acute effect of a resistance exercise session on markers of cartilage breakdown and inflammation in women with rheumatoid arthritis. Int J Rheum Dis 20(11):1704–1713. https://doi.org/10.1111/1756-185X.13204
Sieczkowska SM, Smaira FI, Mazzolani BC, Gualano B, Roschel H, Peçanha T (2021) Efficacy of home-based physical activity interventions in patients with autoimmune rheumatic diseases: a systematic review and meta-analysis. Semin Arthritis Rheum 51(3):576–587
Sveaas SH, Smedslund G, Hagen KB, Dagfinrud H (2017) Effect of cardiorespiratory and strength exercises on disease activity in patients with inflammatory rheumatic diseases: a systematic review and meta-analysis. Br J Sports Med 51(14):1065–1072
Perandini LA, de Sá-Pinto AL, Roschel H, Benatti FB, Lima FR, Bonfá E et al (2012) Exercise as a therapeutic tool to counteract inflammation and clinical symptoms in autoimmune rheumatic diseases. Autoimmun Rev 12(2):218–224
Baillet A, Vaillant M, Guinot M, Juvin R, Gaudin P (2012) Efficacy of resistance exercises in rheumatoid arthritis: meta-analysis of randomized controlled trials. Rheumatology (Oxford) 51(3):519–527
Kao VP, Wen H-J, Pan Y-J, Pai C-S, Tsai S-T, Su K-Y (2021) Combined aerobic and resistance training improves physical and executive functions in women with systemic lupus erythematosus. Lupus. 30(6):946–955
Shehata M, Schwarzmeier JD, Hilgarth M, Demirtas D, Richter D, Hubmann R et al (2006) Effect of combined spa-exercise therapy on circulating TGF-beta1 levels in patients with ankylosing spondylitis. Wien Klin Wochenschr 118(9–10):266–272
Alexanderson H, Dastmalchi M, Esbjörnsson-Liljedahl M, Opava CH, Lundberg IE (2007) Benefits of intensive resistance training in patients with chronic polymyositis or dermatomyositis. Arthritis Rheum 57(5):768–777
Nader GA, Dastmalchi M, Alexanderson H, Grundtman C, Gernapudi R, Esbjörnsson M et al (2010) A longitudinal, integrated, clinical, histological and mRNA profiling study of resistance exercise in myositis. Mol Med 16(11–12):455–464
Funding
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior-Brasil (CAPES)–Finance Code 001.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dardin, L.P., Garcia, A.B.A., Minali, P.A. et al. The effects of resistance training in patients with primary Sjogren’s syndrome. Clin Rheumatol 41, 1145–1152 (2022). https://doi.org/10.1007/s10067-021-05977-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-021-05977-0