Abstract
Background
The use of prostheses in inguinal hernia repair reduces the incidence of recurrence. Quality of life and pain after hernia repair are largely correlated with the technique and type of prosthesis.
Aims of study
To evaluate the 2-year incidence of recurrence and pain for two types of hernioplasty, Lichtenstein repair and laparoscopy (totally extraperitoneal approach or TEP), and two types of mesh, polypropylene mesh and beta-d-glucan-coated mesh (Glucamesh).
Patients
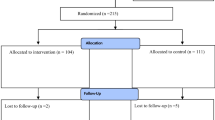
A total of 410 consecutive patients of mean age 54 years (18–84) underwent repair of inguinal hernias, 96 (23%) of which were bilateral and 56 (13%) recurrent. A total of 273 (66.5%) patients underwent Lichtenstein repair: 215 (78.7%) with polypropylene mesh, 58 (21.3%) with Glucamesh; 137 patients underwent laparoscopy: 80 (58.4%) with polypropylene mesh, 57 (41.6%) with Glucamesh. In each group, the populations were comparable and the techniques utilized were identical.
Methods
The patients were followed-up for at least 2 years, after which the incidence of recurrence was determined, and chronic pain was assessed by means of a visual analog scale and a validated questionnaire.
Results
A total of 349 patients (85.1%) were reassessed, 117 of whom had undergone laparoscopy and 232 Lichtenstein repair. There were ten recurrences (2.8%), and incidence which was independent of the technique (laparoscopy 1.7% vs. Lichtenstein 3.4%) (ns) and the type of prosthesis (Glucamesh 1.9% vs. polypropylene 2.4%) (ns). Chronic pain was noted in 69 patients (19.7%) and severe pain in 11 (3.1%). The incidence of chronic pain was the same for the two techniques: laparoscopy 17.9% vs. Lichtenstein 20.7% (ns). The same was true for severe pain: laparoscopy 3.4% vs Lichtenstein 3% (ns). The incidence of chronic pain was closely correlated with the type of prosthesis utilized: Glucamesh 4.8% vs. polypropylene 26.5% (P = 0.02), irrespective of the technique. The same was true for severe pain (0.9 vs. 4%) (P = 0.02).
Conclusion
The utilization of beta-d-glucan-coated mesh did not involve more recurrence and was accompanied by a significant decrease in chronic pain at 2 years, independent of the technique. After 2 years, the results of hernia repair show that the choice of prosthesis was more determinant than choice of technique.
Similar content being viewed by others
References
EU Hernia Trialist Collaboration (2000) Mesh compared with non-mesh methods on open groin hernia repair. Systematic review of randomized controlled trial. Br J Surg 87:854–859
Bay Nielsen M, Perkins FM, Kehlet H for the Danish Data Base (2001) Pain and functional impairment one year after inguinal herniorraphy: a national questionnaire study. Ann Surg 233(1):1–7
Callesen T, Kehlet H (1997) Post-herniorrhaphy pain. Anesthesiology 87:1219–1230
Cunningham J, Temple WJ, Mitchell P (1996) Cooperative hernia study. Pain in the post-repair patient. Ann Surg 224:598–602
Gillion JF, Fagniez PL (1999) Chronic pain and cutaneous sensory changes after inguinal hernia repair: comparison between open and laparoscopic techniques. Hernia 3:75–80
Kumar S, Wilson RG, Nixon SJ, MacIintyre MC (2002) Chronic pain after laparoscopic and open mesh repair of groin hernia. Br J Surg 89:1476–1479
Post S, Weiss B, Willer M, Neufang T, Lorenz D (2004) Randomized clinical trial of lightweight composite mesh for Lichtenstein inguinal hernia. Br J Surg 91:44–48
American Society of Anesthesiology (ASA) (2006) ASA Physical Status Classification System. http://www.asahq.org/clinical/physicalstatus.htm
Amid PK, Lichtenstein IL (1998) Long-term results and presentation of data of the Lichtenstein open tension-free hernioplasty. Hernia 2:89–94
Barrat C, Seriser F, Arnoud R, Trouette P, Champault G (2004) Inguinal hernia repair with beta glucan-coated mesh: prospective multicenter study (115 cases). Preliminary results. Hernia 8:33–38
Lau H, Patel NF, Yuen K, Lee F (2003) Prevalence and severity of chronic groin pain after endoscopic extraperitoneal hernioplasty. Surg Endosc 17:1620–1623
Wrigland WW, Van Den Tol MP, Luijendijih RW, Hop WCP, Busschbacht JJV, de Lange DCD, Van Geldere D, Rottier AB, Vegt PA, Ijzermans JNM, Jeekel J (2002) Randomized trial of non-mesh versus mesh repair of primary inguinal hernia. Br J Surg 89(3):293–297
Poobalan AS, Bruce J, King PM, Chambers WA, Krukowski ZH, Smith WCS (2001) Chronic pain and quality of life following open inguinal hernia. Br J Surg 88:1122–1126
Silen W (2002) Chronic pain and quality of life following open inguinal hernia repair. Br J Surg 89:123
Arvidson D, Berndsen FM, Larsson LG, Leijonmarck CE, Rimback G, Rudberg C, Smedberg S, Spangen L, Montgomery A (2005) Randomized clinical trial comparing 5-year recurrence rate after laparoscopic versus shouldice repaire of primary inguinal hernia. Br J Surg 92:1085–1091
Wara P, Bay Nielsen M, Jul P, Bendix J, Kehlet H (2005) Prospective nationwide analysis of laparoscopic versus Lichtenstein repair of inguinal hernia. Br J Surg 92:1277–1281
Lozano DD, Noordenbos J, Hansbrough JF (2002) The use of glucan II in the treatment of donor sites. J Burn Care Rehabil Suppl 23(2):S81
Abel G, Czop JK (1992) Stimulation of human monocyte beta-glucan receptors by glucan particles induces production of TNF-alpha and IL-1 beta. Int J Immunopharmacol 14:1363–1373
De Fellipe Jr J, Da Rocha e Silva Jr M, Maicel FM, Soares A Mendes NF (1993) Infection prevention in patient with severe multiple trauma with the immunomodulator beta 1-3 polyglucose (glucan). Surg Gynecol Obstet 177:383–388
Estrada A, Yun CH, Van Kessel A, Li B, Hunta S (1987) Immunomodulatory activities of oat beta-glucan in vitro and in vivo. Microbiol Immunol 41(12):991–998
Champault G, Barrat C (2005) Inguinal hernia repair with beta glucan-coated mesh: results at two-year follow up. Hernia 9:125–130
Langenbach MR, Schmidt J, Zirngilbl H (2003) Comparison of biomaterials in the early post operative period. Polypropylene meshes in laparoscopic inguinal hernia repair. Surg Endosc 17:1104–1105
Barrat C, Surlin V, Polliand C, Matthyssens L, Champault G (2005) Place des prothèses dans les cures de hernies inguinales. J Coelio Chir 53:30–33
Conze J, Kingsnorth AN, Flament JB, Simmermacker P, Arlt G, Langer C, Shippers E, Hartley A, Schlumpelick V (2005) Randomized clinical trial comparing lightweight composite mesh with polyester or polypropylene mesh for incisional hernia repair. Br J Surg 92:1488–1493
Cobb WS, Kercher KW, Heniford TB (2005) The argument for lightweight polypropylene mesh in hernia repair. Surg Inn 12:63–69
Bringman S, Wollert S, Osterberg J, Smedberg S, Granlund H, Heikkinen TJ (2006) Three-year results of a randomized clinical trial of lightweight or standard polypropylene mesh in Lichtenstein repair of primary inguinal hernia. Br J Surg 93:1056–1059
Khan LR, Kumar S, Nixon SJ (2006) Early results for new lightweight mesh in laparoscopic totally extraperitoneal inguinal hernia repair. Hernia 10:303–308
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Champault, G., Bernard, C., Rizk, N. et al. Inguinal hernia repair: the choice of prosthesis outweighs that of technique. Hernia 11, 125–128 (2007). https://doi.org/10.1007/s10029-006-0179-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-006-0179-y