Abstract
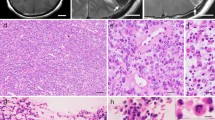
We report an intramedullary spinal tumor consisting of an ependymoma and a hemangioblastoma (HB). A 37-year-old woman presented with progressive bilateral lower limb sensory and motor deficits. Magnetic resonance imaging showed a single intramedullary mass in the thoracic cord (T4–T6 level). Clinically, the patient had no von Hippel–Lindau disease and neurofibromatosis type 2. Metastatic carcinomas including renal cell carcinoma were altogether negative. Complete surgical resection was performed. Histologically, the tumor consisted of a mixed ependymoma and HB. Tumor cells of ependymoma displayed a rather uniform appearance with round to oval nuclei having salt-and-pepper-like chromatin, forming perivascular pseudorosette structures with radially arranged, tapering cell processes extending to intratumoral blood vessels. Stromal cells of HB had vacuolated or homogeneously eosinophilic cytoplasm and variable sized hyperchromatic nuclei within a background of capillaries. Immunohistochemically, tumor cells of ependymoma were strongly positive for glial fibrillary acidic protein (GFAP), focally positive for epithelial membrane antigen (EMA) and D2-40 in a dot-like or ring-like pattern. Stromal cells of HB showed immunoreactivity for S100, vimentin, inhibin-α, D2-40, EMA and cytokeratins (CK: AE1/AE3, CK19). A review of the literature, in conjunction with the present case, shows that ependymomas and HBs may have a close relationship with each other.



Similar content being viewed by others
References
Nakamura M, Ishii K, Watanabe K, Tsuji T, Takaishi H, Matsumoto M, Toyama Y, Chiba K (2008) Surgical treatment of intramedullary spinal cord tumors: prognosis and complications. Spinal Cord 46:282–286
Garcés-Ambrossi GL, McGirt MJ, Mehta VA, Sciubba DM, Witham TF, Bydon A, Wolinksy JP, Jallo GI, Gokaslan ZL (2009) Factors associated with progression-free survival and long-term neurological outcome after resection of intramedullary spinal cord tumors: analysis of 101 consecutive cases. J Neurosurg Spine 11:591–599
Bansal S, Ailawadhi P, Suri A, Kale SS, Sarat Chandra P, Singh M, Kumar R, Sharma BS, Mahapatra AK, Sharma MC, Sarkar C, Bithal P, Dash HH, Gaikwad S, Mishra NK (2013) Ten years’ experience in the management of spinal intramedullary tumors in a single institution. J Clin Neurosci 20:292–298
Roonprapunt C, Silvera VM, Setton A, Freed D, Epstein FJ, Jallo GI (2001) Surgical management of isolated hemangioblastomas of the spinal cord. Neurosurgery 49:321–328
Park CH, Lee CH, Hyun SJ, Jahng TA, Kim HJ, Kim KJ (2012) Surgical outcome of spinal cord hemangioblastomas. J Korean Neurosurg Soc 52:221–227
Serban D, Exergian F (2013) Intramedullary hemangioblastoma—local experience of a tertiary clinic. Chirurgia (Bucur) 108:325–330
Hagel C, Stemmer-Rachamimov AO, Bornemann A, Schuhmann M, Nagel C, Huson S, Evans DG, Plotkin S, Matthies C, Kluwe L, Mautner VF (2012) Clinical presentation, immunohistochemistry and electron microscopy indicate neurofibromatosis type 2-associated gliomas to be spinal ependymomas. Neuropathology 32:611–616
McLendon RE, Wiestler OD, Kros JM, Korshunov A, Ng HK (2007) Ependymoma. In: Louis DN, Ohgaki H, Wiestler OD, Cavenee WK (eds) WHO classification of tumours of the central nervous system, 4th edn. IARC, Lyon, pp 74–78
Kawano N, Yasui Y, Utsuki S, Oka H, Fujii K, Yamashina S (2004) Light microscopic demonstration of the microlumen of ependymoma: a study of the usefulness of antigen retrieval for epithelial membrane antigen (EMA) immunostaining. Brain Tumor Pathol 21:17–21
Hasselblatt M, Paulus W (2003) Sensitivity and specificity of epithelial membrane antigen staining patterns in ependymomas. Acta Neuropathol 106:385–388
Ishizawa K, Komori T, Shimada S, Hirose T (2009) Podoplanin is a potential marker for the diagnosis of ependymoma: a comparative study with epithelial membrane antigen (EMA). Clin Neuropathol 28:373–378
Aldape KD, Plate KH, Vortmeyer AO, Zagzag D, Neumann HPH (2007) Haemangioblastoma. In: Louis DN, Ohgaki H, Wiestler OD, Cavenee WK (eds) WHO classification of tumours of the central nervous system, 4th edn. IARC, Lyon, pp 184–186
Ishizawa K, Komori T, Hirose T (2005) Stromal cells in hemangioblastoma: neuroectodermal differentiation and morphological similarities to ependymoma. Pathol Int 55:377–385
Hasselblatt M, Jeibmann A, Gerss J, Behrens C, Rama B, Wassmann H, Paulus W (2005) Cellular and reticular variants of haemangioblastoma revisited: a clinicopathologic study of 88 cases. Neuropathol Appl Neurobiol 31:618–622
Weinbreck N, Marie B, Bressenot A, Montagne K, Joud A, Baumann C, Klein O, Vignaud JM (2008) Immunohistochemical markers to distinguish between hemangioblastoma and metastatic clear-cell renal cell carcinoma in the brain: utility of aquaporin1 combined with cytokeratin AE1/AE3 immunostaining. Am J Surg Pathol 32:1051–1059
Jung SM, Kuo TT (2005) Immunoreactivity of CD10 and inhibin alpha in differentiating hemangioblastoma of central nervous system from metastatic clear cell renal cell carcinoma. Mod Pathol 18:788–794
Lach B, Gregor A, Rippstein P, Omulecka A (1999) Angiogenic histogenesis of stromal cells in hemangioblastoma: ultrastructural and immunohistochemical study. Ultrastruct Pathol 23:299–310
Gouldesbrough DR, Bell JE, Gordon A (1988) Use of immunohistochemical methods in the differential diagnosis between primary cerebellar haemangioblastoma and metastatic renal carcinoma. J Clin Pathol 41(8):861–865
Brown DF, Gazdar AF, White CL 3rd, Yashima K, Shay JW, Rushing EJ (1997) Human telomerase RNA expression and MIB-1 (Ki-67) proliferation index distinguish hemangioblastomas from metastatic renal cell carcinomas. J Neuropathol Exp Neurol 56:1349–1355
Kawano N, Yagishita S, Komatsu K, Suwa T, Oka H, Utsuki S, Fujii K (1999) Cerebellar clear cell ependymoma mimicking hemangioblastoma: its clinical and pathological features. Surg Neurol 51:281–287
Bonnin JM, Peña CE, Rubinstein LJ (1983) Mixed capillary hemangioblastoma and glioma. A redefinition of the “angioglioma”. J Neuropathol Exp Neurol 42:504–516
Adams SA, Hilton DA (2002) Recurrent haemangioblastoma with glial differentiation. Neuropathol Appl Neurobiol 28:142–146
Yang QX, Li Y, Tian XY, Liao B, Jiang XZ, Li Z (2012) Bilateral cerebellar epithelioid hemangioblastoma with possible ependymal differentiation in a patient with von Hippel–Lindau disease. Neuropathology 32:662–667
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cheng, HX., Chu, SG., Xu, QW. et al. A spinal tumor showing mixed features of ependymoma and hemangioblastoma: a case report and literature review. Brain Tumor Pathol 32, 112–118 (2015). https://doi.org/10.1007/s10014-014-0208-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10014-014-0208-y