Abstract
Objectives
This cross-sectional study investigated the factors associated with weight gain ≥ 10 kg after 20 years of age in the general Japanese population, with a focus on the number of teeth.
Materials and methods
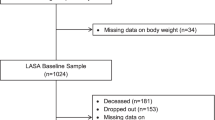
We included individuals aged ≥ 40 years from Yamagata prefecture, Japan from 2017–2021. A postal survey was conducted using a self-administered questionnaire; 5,940 participants were included in the final analysis. The questionnaire included items on lifestyle factors, medical history, physical and mental conditions, oral health, and dietary intake. A multivariate logistic regression analysis was used to identify independent associations between weight gain ≥ 10 kg after 20 years of age and various parameters; adjusted odds ratios (ORs) and 95% confidence intervals (CIs) were estimated.
Results
Less than 20 teeth, male sex, drinking habit frequency, eating very fast or fast, and a higher frequency of eating-away-from-home were significant factors associated with weight gain ≥ 10 kg after 20 years of age; individuals with < 20 versus > 20 teeth exhibited a 1.35-fold higher OR (95% CI 1.15–1.59; p < 0.01).
Conclusions
Our results suggest that having < 20 teeth may affect weight gain ≥ 10 kg after 20 years of age. However, owing to the cross-sectional study design, causality could not be determined. Therefore, maintaining healthy lifestyle behaviors to avoid tooth loss may also affect weight gain ≥ 10 kg after 20 years of age.
Clinical relevance
Having < 20 teeth has the potential to affect long-term weight gain after 20 years of age.
Similar content being viewed by others
Data availability
Data cannot be shared for privacy or ethical reasons but are available from the corresponding author on reasonable request after permission of the ethics committee of Yamagata University.
References
Paoli A (2014) Ketogenic diet for obesity: Friend or foe? Int J Environ Res Public Health 11:2092–2107. https://doi.org/10.3390/ijerph110202092
Ortega FB, Lavie CJ, Blair SN (2016) Obesity and cardiovascular disease. Circ Res 118:1752–1770. https://doi.org/10.1161/CIRCRESAHA.115.306883
Rajadhyaksha A, Sarate N, Raghorte N, Ingawale S (2022) A clinical profile of patients with hyperuricemia and the relationship between hyperuricemia and metabolic syndrome: A cross-sectional study at a tertiary hospital in the Indian population. J Assoc Physicians India 70:11–12. https://doi.org/10.0102/japi.2022.05
Iwashita M, Hayashi M, Nishimura Y, Yamashita A (2021) The link between periodontal inflammation and obesity. Curr Oral Health Rep 8:76–83. https://doi.org/10.1007/s40496-021-00296-4
Dhurandhar NV, Petersen KS, Webster C (2021) Key causes and contributors of obesity: A perspective. Nurs Clin North Am 56:449–464. https://doi.org/10.1016/j.cnur.2021.07.007
Kim D, Ahn BI (2020) Eating out and consumers’ health: Evidence on obesity and balanced nutrition intakes. Int J Environ Res Public Health 17:586. https://doi.org/10.3390/ijerph17020586
Zhao P, Xu A, Leung WK (2022) Obesity, bone loss, and periodontitis: The interlink. Biomolecules 12:865. https://doi.org/10.3390/biom12070865
Nascimento GG, Leite FR, Conceição DA, Ferrúa CP, Singh A, Demarco FF (2016) Is there a relationship between obesity and tooth loss and edentulism? A systematic review and meta-analysis. Obes Rev 17:587–598. https://doi.org/10.1111/obr.12418
Ikebe K, Matsuda K, Kagawa R, Enoki K, Yoshida M, Maeda Y, Nokubi T (2011) Association of masticatory performance with age, gender, number of teeth, occlusal force and salivary flow in Japanese older adults: Is ageing a risk factor for masticatory dysfunction? Arch Oral Biol 56:991–996. https://doi.org/10.1016/j.archoralbio.2011.03.019
Zheng Y, Manson JE, Yuan C, Liang MH, Grodstein F, Stampfer MJ, Willett WC, Hu FB (2017) Associations of weight gain from early to middle adulthood with major health outcomes later in life. JAMA 318:255–269. https://doi.org/10.1001/jama.2017.7092
Takebe N, Tanno K, Ohmomo H, Hangai M, Oda T, Hasegawa Y, Takanashi N, Sasaki R, Shimizu A, Sasaki A, Sakata K, Sasaki M, Ishigaki Y (2021) Weight gain after 20 years of age is associated with unfavorable lifestyle and increased prevalence of metabolic disorders. Diabetes Metab Syndr Obes 14:2065–2075. https://doi.org/10.2147/DMSO.S300250
Chei CL, Iso H, Yamagishi K, Inoue M, Tsugane S (2008) Body mass index and weight change since 20 years of age and risk of coronary heart disease among Japanese: The Japan Public Health Center-Based Study. Int J Obes (Lond) 32:144–151. https://doi.org/10.1038/sj.ijo.0803686
Shimazu M, Koyama W, Hamada K, Irie A, Manzoji T, Watabe H, Tsuchiya A (2021) Investigation of medical examinee for men under 40 years of age [in Japanese]. Ningen Dock 35:739–747
Watanabe SHY, Yagi K (2020) Visceral obesity with normal waist circumference is associated with lifestyle and arterioscleotic risk factors: Benefits of visceral fat area measurement by abdominal bioimpedance method. Ningen Dock 35:8
Okutsu S, Kato Y, Funakoshi S, Maeda T, Yoshimura C, Kawazoe M, Satoh A, Yokota S, Tada K, Takahashi K, Ito K, Yasuno T, Fujii H, Mukoubara S, Nakashima H, Kawanami D, Masutani K, Arima H, Nabeshima S (2021) Effects of weight gain after 20 years of age and incidence of hyper-low-density lipoprotein cholesterolemia: The Iki epidemiological study of atherosclerosis and chronic kidney disease (ISSA-CKD). J Clin Med 10:3098. https://doi.org/10.3390/jcm10143098
Rohrmann S, Steinbrecher A, Linseisen J, Hermann S, May A, Luan J, Ekelund U, Overvad K, Tjønneland A, Halkjær J, Fagherazzi G, Boutron-Ruault MC, Clavel-Chapelon F, Agnoli C, Tumino R, Masala G, Mattiello A, Ricceri F, Travier N, Amiano P, Ardanaz E, Chirlaque MD, Sanchez MJ, Rodríguez L, Nilsson LM, Johansson I, Hedblad B, Rosvall M, Lund E, Braaten T, Naska A, Orfanos P, Trichopoulou A, van den Berg S, Bueno-de-Mesquita HB, Bergmann MM, Steffen A, Kaaks R, Teucher B, Wareham NJ, Khaw KT, Crowe FL, Illner AK, Slimani N, Gallo V, Mouw T, Norat T, Peeters PH (2012) The association of education with long-term weight change in the EPIC-PANACEA cohort. Eur J Clin Nutr 66:957–963. https://doi.org/10.1038/ejcn.2012.55
Pan A, Malik VS, Hao T, Willett WC, Mozaffarian D, Hu FB (2013) Changes in water and beverage intake and long-term weight changes: Results from three prospective cohort studies. Int J Obes (Lond) 37:1378–1385. https://doi.org/10.1038/ijo.2012.225
Toyoshima H, Masuoka N, Hashimoto S, Otsuka R, Sasaki S, Tamakoshi K, Yatsuya H (2009) Effect of the interaction between mental stress and eating pattern on body mass index gain in healthy Japanese male workers. J Epidemiol 19:88–93. https://doi.org/10.2188/jea.je20080066
Yang J, Zhang C, Chavarro JE, Rich-Edwards JW, Wang M, Fawzi WW, Manson JE, Lee IM, Hu FB, Tobias DK (2022) Lifestyle changes and long-term weight gain in women with and without a history of gestational diabetes mellitus: A prospective study of 54,062 women in the nurses’ health Study II. Diabetes Care 45:348–356. https://doi.org/10.2337/dc21-1692
Chao AM, Wadden TA, Ashare RL, Loughead J, Schmidt HD (2019) Tobacco smoking, eating behaviors, and body weight: A review. Curr Addict Rep 6:191–199. https://doi.org/10.1007/s40429-019-00253-3
Auerbach BJ, Littman AJ, Krieger J, Young BA, Larson J, Tinker L, Neuhouser ML (2018) Association of 100% fruit juice consumption and 3-year weight change among postmenopausal women in the in the Women’s Health Initiative. Prev Med 109:8–10. https://doi.org/10.1016/j.ypmed.2018.01.004
El Reda D, Ström P, Sandin S, Oh JK, Adami HO, Löf M, Weiderpass E (2017) Determinants of long-term weight change among middle-aged Swedish women. Obesity (Silver Spring) 25:476–485. https://doi.org/10.1002/oby.21745
Konttinen H, van Strien T, Männistö S, Jousilahti P, Haukkala A (2019) Depression, emotional eating and long-term weight changes: A population-based prospective study. Int J Behav Nutr Phys Act 16:28. https://doi.org/10.1186/s12966-019-0791-8
Ogilvie RP, Patel SR (2017) The epidemiology of sleep and obesity. Sleep Health 3:383–388. https://doi.org/10.1016/j.sleh.2017.07.013
Gesteiro E, García-Carro A, Aparicio-Ugarriza R, González-Gross M (2022) Eating out of home: Influence on nutrition, health, and policies: A scoping review. Nutrients 14:1265. https://doi.org/10.3390/nu14061265
Lara M, Sisa I, Yepez MC (2019) Breakfast skipping, nutritional status, and physical activity in a middle-aged Latin American population: A population-based study from Ecuador. Nutr Hosp 36:1123–1132. https://doi.org/10.20960/nh.02393
Konieczna J, Romaguera D, Pereira V, Fiol M, Razquin C, Estruch R, Asensio EM, Babio N, Fitó M, Gómez-Gracia E, Ros E, Lapetra J, Arós F, Serra-Majem L, Pintó X, Toledo E, Sorlí JV, Bulló M, Schröder H, Martínez-González MA (2019) Longitudinal association of changes in diet with changes in body weight and waist circumference in subjects at high cardiovascular risk: The PREDIMED trial. Int J Behav Nutr Phys Act 16:139. https://doi.org/10.1186/s12966-019-0893-3
Bes-Rastrollo M, Basterra-Gortari FJ, Sánchez-Villegas A, Marti A, Martínez JA, Martínez-González MA (2010) A prospective study of eating away-from-home meals and weight gain in a Mediterranean population: The SUN (Seguimiento Universidad de Navarra) cohort. Public Health Nutr 13:1356–1363. https://doi.org/10.1017/S1368980009992783
Ueno M, Yanagisawa T, Shinada K, Ohara S, Kawaguchi Y (2008) Masticatory ability and functional tooth units in Japanese adults. J Oral Rehabil 35:337–344. https://doi.org/10.1111/j.1365-2842.2008.01847.x
Tatematsu M, Mori T, Kawaguchi T, Takeuchi K, Hattori M, Morita I, Nakagaki H, Kato K, Murakami T, Tuboi S, Hayashizaki J, Murakami H, Yamamoto M, Ito Y (2004) Masticatory performance in 80-year-old individuals. Gerodontology 21:112–119. https://doi.org/10.1111/j.1741-2358.2004.00018.x
Hsu KJ, Yen YY, Lan SJ, Wu YM, Chen CM, Lee HE (2011) Relationship between remaining teeth and self-rated chewing ability among population aged 45 years or older in Kaohsiung City, Taiwan. Kaohsiung J Med Sci 27:457–465. https://doi.org/10.1016/j.kjms.2011.06.006
Wakai K, Naito M, Naito T, Kojima M, Nakagaki H, Umemura O, Yokota M, Hanada N, Kawamura T (2010) Tooth loss and intakes of nutrients and foods: A nationwide survey of Japanese dentists. Community Dent Oral Epidemiol 38:43–49. https://doi.org/10.1111/j.1600-0528.2009.00512.x
Shen J, Qian S, Huang L, Tao Y, Chen H, Deng K, Yang F, Zong G, Zheng Y, Wang X, Tonetti M, Yuan C (2023) Association of the number of natural teeth with dietary diversity and nutritional status in older adults: A cross-sectional study in China. J Clin Periodontol 50:242–251. https://doi.org/10.1111/jcpe.13728
Kotsakis GA, Chrepa V, Shivappa N, Wirth M, Hebert J, Koyanagi A, Tyrovolas S (2018) Diet-borne systemic inflammation is associated with prevalent tooth loss. Clin Nutr 37:1306–1312. https://doi.org/10.1016/j.clnu.2017.06.001
Zhu Y, Hollis JH (2014) Increasing the number of chews before swallowing reduces meal size in normal-weight, overweight, and obese adults. J Acad Nutr Diet 114:926–931. https://doi.org/10.1016/j.jand.2013.08.020
Himmlova L, Goldmann T, Ihde S, Konvickova S (2007) Time analysis of hard and soft bolus processing. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 151:327–332. https://doi.org/10.5507/bp.2007.056
Wing RR (1999) Physical activity in the treatment of the adulthood overweight and obesity: Current evidence and research issues. Med Sci Sports Exerc 31:S547–S552. https://doi.org/10.1097/00005768-199911001-00010
Telleria-Aramburu N, Arroyo-Izaga M (2022) Risk factors of overweight/obesity-related lifestyles in university students: Results from the EHU12/24 study. Br J Nutr 127:914–926. https://doi.org/10.1017/S0007114521001483
Almohamad M, Krall Kaye E, Mofleh D, Spartano NL (2022) The association of sedentary behaviour and physical activity with periodontal disease in NHANES 2011–2012. J Clin Periodontol 49:758–767. https://doi.org/10.1111/jcpe.13669
Muniz FWMG, Pola NM, Silva CFE, Silva FGD, Casarin M (2021) Are periodontal diseases associated with sleep duration or sleep quality? A systematic review. Arch Oral Biol 129:105184. https://doi.org/10.1016/j.archoralbio.2021.105184
Kotronia E, Brown H, Papacosta AO, Lennon LT, Weyant RJ, Whincup PH, Wannamethee SG, Ramsay SE (2021) Poor oral health and the association with diet quality and intake in older people in two studies in the UK and USA. Br J Nutr 126:118–130. https://doi.org/10.1017/S0007114521000180
Martinon P, Fraticelli L, Giboreau A, Dussart C, Bourgeois D, Carrouel F (2021) Nutrition as a key modifiable factor for periodontitis and main chronic diseases. J Clin Med 10:197. https://doi.org/10.3390/jcm10020197
Hwang SY, Jang JH, Park JE (2022) Association between healthy lifestyle (diet quality, physical activity, normal body weight) and periodontal diseases in Korean adults. Int J Environ Res Public Health 19:3871. https://doi.org/10.3390/ijerph19073871
Suzuki S, Sugihara N, Kamijo H, Morita M, Kawato T, Tsuneishi M, Kobayashi K, Hasuike Y, Sato T (2022) Reasons for tooth extractions in Japan: The second nationwide survey. Int Dent J 72:366–372. https://doi.org/10.1016/j.identj.2021.05.008
Otsuka R, Tamakoshi K, Yatsuya H, Murata C, Sekiya A, Wada K, Zhang HM, Matsushita K, Sugiura K, Takefuji S, OuYang P, Nagasawa N, Kondo T, Sasaki S, Toyoshima H (2006) Eating fast leads to obesity: Findings based on self-administered questionnaires among middle-aged Japanese men and women. J Epidemiol 16:117–124. https://doi.org/10.2188/jea.16.117
van den Boer JHW, Kranendonk J, van de Wiel A, Feskens EJM, Geelen A, Mars M (2017) Self-reported eating rate is associated with weight status in a Dutch population: A validation study and a cross-sectional study. Int J Behav Nutr Phys Act 14:121. https://doi.org/10.1186/s12966-017-0580-1
Fagerberg P, Charmandari E, Diou C, Heimeier R, Karavidopoulou Y, Kassari P, Koukoula E, Lekka I, Maglaveras N, Maramis C, Pagkalos I, Papapanagiotou V, Riviou K, Sarafis I, Tragomalou A, Ioakimidis I (2021) Fast eating is associated with increased BMI among high-school students. Nutrients 13:880. https://doi.org/10.3390/nu13030880
Wei X, Yu D, Ju L, Cheng X, Zhao L (2021) Analysis of the correlation between eating away from home and BMI in adults 18 years and older in China: Data from the CNNHS 2015. Nutrients 14:146. https://doi.org/10.3390/nu14010146
Ueno M, Shimazu T, Sawada N, Tsugane S, Kawaguchi Y (2018) Validity of self-reported tooth counts and masticatory status study of a Japanese adult population. J Oral Rehabil 45:393–398. https://doi.org/10.1111/joor.12615
Høvik H, Kolberg M, Gjøra L, Nymoen LC, Skudutyte-Rysstad R, Hove LH, Sun YQ, Fagerhaug TN (2022) The validity of self-reported number of teeth and edentulousness among Norwegian older adults, the HUNT Study. BMC Oral Health 22:82. https://doi.org/10.1186/s12903-022-02116-2
Margozzini P, Berríos R, Cantarutti C, Veliz C, Ortuno D (2019) Validity of the self-reported number of teeth in Chilean adults. BMC Oral Health 19:99. https://doi.org/10.1186/s12903-019-0794-5
Tegelberg P, Saxlin T, Tervonen T, Knuuttila M, Jokelainen J, Auvinen J, Ylöstalo P (2021) Association of long-term obesity and weight gain with periodontal pocketing: Results of the Northern Finland Birth Cohort 1966 study. J Clin Periodontol 48:1344–1355. https://doi.org/10.1111/jcpe.13524
Ladeira LLC, Nascimento GG, Leite FRM, Alves-Costa S, Barbosa JMA, Alves CMC, Thomaz EBAF, Batista RFL, Ribeiro CCC (2023) Obesity, insulin resistance, caries, and periodontitis: Syndemic framework. Nutrients 15:3512. https://doi.org/10.3390/nu15163512
Ueno M, Shimazu T, Sawada N, Tsugane S, Kawaguchi, (2020) Validity of self-reported periodontitis in Japanese adults: The Japan Public Health Center-Based Prospective Study for the Next-Generation Oral Health Study. Asia Pac J Public Health 32:346–353. https://doi.org/10.1177/1010539520944721
Yland JJ, Wesselink AK, Lash TL, Fox MP (2022) Misconceptions about the direction of bias from nondifferential misclassification. Am J Epidemiol 191:1485–1495. https://doi.org/10.1093/aje/kwac035
Dahl AK, Reynolds CA (2013) Accuracy of recalled body weight–a study with 20-years of follow-up. Obesity (Silver Spring) 21:1293–1298. https://doi.org/10.1002/oby.20299
Dahl AK, Hassing LB, Fransson EI, Pedersen NL (2010) Agreement between self-reported and measured height, weight and body mass index in old age–a longitudinal study with 20 years of follow-up. Age Ageing 39:445–451. https://doi.org/10.1093/ageing/afq038
Lawlor DA, Bedford C, Taylor M, Ebrahim S (2002) Agreement between measured and self-reported weight in older women. Results from the British Women’s Heart and Health Study. Age Ageing 31:169–174. https://doi.org/10.1093/ageing/31.3.169
Acknowledgements
We thank Editage for their English language editing service.
Funding
This work was supported by a grant-in-aid from the 21st Century Center of Excellence and the Global Center of Excellence Program of the Japan Society for the Promotion of Science.
Author information
Authors and Affiliations
Contributions
Conceptualization: [Shigeo Ishikawa],[Tsuneo Konta], and [Mitsuyoshi Iino];Methodology: [Shigeo Ishikawa] and [Tsuneo Konta]; Formal analysis and investigation: [Shigeo Ishikawa], [Tsuneo Konta], [Shinji Susa], [Kenichi Ishizawa], [Naohiko Makino], and [Yoshiyuki Ueno]; Writing—original draft preparation: [Shigeo Ishikawa]; Writing—review and editing:[Tsuneo Konta], [Shinji Susa], [Kenichi Ishizawa],[Naohiko Makino],[Yoshiyuki Ueno],[Naoki Okuyama], and [Mitsuyoshi Iino]; Supervision: [Shinji Susa], [Kenichi Ishizawa],[Naohiko Makino],[Yoshiyuki Ueno].
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
All procedures performed in this study involving human partifcipants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the Ethics Committee of Yamagata University (No. 2022–135).
Consent to participate
Informed consent was obtained from all participants in the original cohort study. In this study, the participants were given an option to opt out online. None of the patients declined to participate.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ishikawa, S., Konta, T., Susa, S. et al. Association of health behaviors, dietary habits, and oral health with weight gain after 20 years of age in community-dwelling Japanese individuals aged 40 years and older: a cross-sectional study. Clin Oral Invest 27, 7345–7358 (2023). https://doi.org/10.1007/s00784-023-05325-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-023-05325-3