Abstract
Objectives
Surgery-first orthognathic surgery is rarely used in class III asymmetry due to concerns of reduced skeletal stability from unstable surgical occlusion. This study aimed to evaluate if skeletal stability after surgery-first orthognathic surgery is related to virtual surgical occlusal contact or surgical change.
Materials and methods
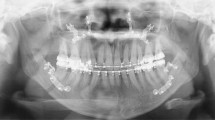
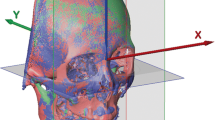
We studied 58 adults with class III asymmetry, consecutively corrected by Le Fort I osteotomy and bilateral sagittal split osteotomy using a surgery-first approach. Dental casts were manually set to measure virtual surgical occlusal contact including contact distribution, contact number, and contact area. Cone-beam computed tomography taken before treatment, 1-week post-surgery, and after treatment was used to measure surgical change and post-surgical stability of the maxilla and mandible in translation (left/right, posterior/anterior, superior/inferior) and rotation (pitch, roll, yaw). The relationship between skeletal stability and surgical occlusal contact or surgical change was evaluated with correlation analysis.
Results
Significant instability was found in the mandible but not in the maxilla. No correlation was found between the maxillary or mandibular stability and surgical occlusal contact (all p > 0.01). However, a significant correlation was found between the maxillary (roll and yaw) or mandibular (shift, roll and pitch) stability and its surgical change (all p < 0.001).
Conclusions
In correction of class III asymmetry with surgery-first bimaxillary surgery, the skeletal stability is not related to the virtual surgical occlusal contact, but surgical skeletal change.
Clinical relevance
Planned over-correction is a reasonable option for correction of severe shift or roll mandibular asymmetry in bimaxillary surgery for class III deformity.






Similar content being viewed by others
References
Samman N, Tong AC, Cheung DL, Tideman H (1992) Analysis of 300 dentofacial deformities in Hong Kong. Int J Adult Orthodon Orthognath Surg 7:181–185
Cheong YW, Lo LJ (2011) Facial asymmetry: etiology, evaluation, and management. Chang Gung Med J 34:341–351
Proffit WR, White RP, Sarver DM (2003) Contemporary treatment of dentofacial deformity. Mosby, Inc., St. Louis, MO
Jeong WS, Lee JY, Choi JW (2017) Large-scale study of long- term anteroposterior stability in a surgery-first orthognathic approach without presurgical orthodontic treatment. J Craniofac Surg 28(8):2016–2020
Belusic Gobic M, Kralj M, Harmicar D, Cerovic R, Mady Maricic B, Spal S (2021) Dentofacial deformity and orthognathic surgery: influence on self-esteem and aspects of quality of life. J Craniomaxillofac Surg 49(4):277–281
Di Palma E, Gasparini G, Pelo S, Tartaglia GM, Sforzaet C (2010) Activities of masticatory muscles in patients before orthognathic surgery. J Craniofac Surg 21:724–726
Diaz PM, Garcia RG, Gias LN, Aguirre-Jaime A, Pérez JS, de la Plata MM, Navarro EV, Gonzalez FJ (2010) Time used for orthodontic surgical treatment of dentofacial deformities in white patients. J Oral Maxillofac Surg 68(1):88–92
Hosseinzadeh Nik T, Gholamrezaei E, Keshvad MA (2019) Facial asymmetry correction: from conventional orthognathic treatment to surgery-first approach. J Dent Res Dent Clin Dent Prospects 13(4):311–320
Huang CS, Hsu SS, Chen YR (2014) Systematic review of the surgery-first approach in orthognathic surgery. Biomed J 37(4):184–190
Gabardo M, Zielak J, Tórtora G, Gerber J, Meger M, Rebellato N, Küchlera K, Scariot R (2019) Impact of orthognathic surgery on quality of life: predisposing clinical and genetic factors. J Craniomaxillofac Surg 47(8):1285–1291
Liao YF, Chiu YT, Huang CS, Ko EW, Chen YR (2010) Presurgical orthodontics versus no presurgical orthodontics: treatment outcome of surgical-orthodontic correction for skeletal Class III open bite. Plast Reconstr Surg 126:2074–2083
Liou EJ, Chen PH, Wang YC, Yu CC, Huang CS, Chen YR (2011) Surgery-first accelerated orthognathic surgery: postoperative rapid orthodontic tooth movement. J Oral Maxillofac Surg 69(3):781–785
Mah DH, Kim SG, Oh JS, You JS, Jung SY, Kim WG, Yu KH (2017) Comparative study of postoperative stability between conventional orthognathic surgery and a surgery-first orthognathic approach after bilateral sagittal split ramus osteotomy for skeletal class III correction. J Korean Assoc Oral Maxillofac Surg 43:23–28
Song HS, Choi SH, Cha JY, Lee KJ, Yu HS (2017) Comparison of changes in the transverse dental axis between patients with skeletal class III malocclusion and facial asymmetry treated by orthognathic surgery with and without presurgical orthodontic treatment. Korean J Orthod 47(4):256–267
Liao YF, Lo SH (2018) Surgical occlusion setup in correction of skeletal Class III deformity using surgery-first approach: guidelines, characteristics and accuracy. Sci Rep 8:11673
Liao YF, Chen YF, Yao CF, Chen YA, Chen YR (2019) Long-term outcomes of bimaxillary surgery for treatment of asymmetric skeletal Class III deformity using surgery-first approach. Clin Oral Investig 23:1685–1693
Lin HH, Chang HW, Wang CH, Kim SG, Lo LJ (2015) Three-dimensional computer-assisted orthognathic surgery: experience of 37 patients. Ann Plast Surg 74:S118–S126
Lo SH, Chen YA, Yao CF, Liao YF, Chen YR (2019) Is skeletal stability after bimaxillary surgery for skeletal class III deformity related to surgical occlusal contact? Int J Oral Maxillofac Surg 48:1329–1336
Lin CL, Chen YA, Yao CF, Chang CS, Liao YF, Chen YR (2021) Comparative stability and outcomes of two surgical approaches for correction of class III asymmetry with lip or occlusal cant. Clin Oral Investig 25:5449–5462
Kim HJ, Hong M, Park HS (2019) Analysis of dental compensation in patients with facial asymmetry using cone-beam computed tomography. Am J Orthod Dentofacial Orthop 156(4):493–501
Liou EJ, Chen PH, Wang YC, Yu CC, Huang CS, Chen YR (2011) Surgery-first accelerated orthognathic surgery: orthodontic guidelines and setup for model surgery. J Oral Maxillofac Surg 69:771–780
Huang CS, Chen YR (2015) Orthodontic principles and guidelines for the surgery-first approach to orthognathic surgery. Int J Oral Maxillofac Surg 44:1457–1462
Yu HB, Mao LX, Wang XD, Fang B, Shen SG (2015) The surgery-first approach in orthognathic surgery: a retrospective study of 50 cases. Int J Oral Maxillofac Surg 44:1463–1467
Liao YF, Chen YA, Chen YC, Chen YR (2020) Outcomes of conventional versus virtual surgical planning of orthognathic surgery using surgery-first approach for class III asymmetry. Clin Oral Investig 24:1509–1516
Hernandez-Alfaro F, Guijarro-Martinez R, Peiro-Guijarro MA (2014) Surgery first in orthognathic surgery: what have we learned? A comprehensive workflow based on 45 consecutive cases. J Oral Maxillofac Surg 72:376–390
Baek SH, Ahn HW, Kwon YH, Choi JY (2010) Surgery-first approach in skeletal class III malocclusion treated with 2-jaw surgery: evaluation of surgical movement and postoperative orthodontic treatment. J Craniofac Surg 21(2):332–338
Choi JW, Park H, Kwon SM, Lee JY (2021) Surgery-first orthognathic approach for the correction of facial asymmetry. J Craniomaxillofac Surg 49(6):435–442
de Villa GH, Huang CS, Chen PK, Chen YR (2005) Bilateral sagittal split osteotomy for correction of mandibular prognathism: long-term results. J Oral Maxillofac Surg 63:1584–1592
Damstra J, Fourie Z, Ren Y (2013) Evaluation and comparison of postero-anterior cephalograms and cone-beam computed tomography images for the detection of mandibular asymmetry. Eur J Orthod 35(1):45–50
Gaber RM, Shaheen E, Falter B, Araya S, Politis C, Swennen GRJ, Jacobs R (2017) A systematic review to uncover a universal protocol for accuracy assessment of 3-dimensional virtually planned orthognathic surgery. J Oral Maxillofac Surg 75:2430–2440
Liebregts J, Baan F, de Koning M, Ongkosuwito E, Berge S, Maal T, Xi T (2017) Achievability of 3D planned bimaxillary osteotomies: maxilla-first versus mandible-first surgery. Sci Rep 7:9314
Muramatsu A, Nawa H, Kimura M et al (2008) Reproducibility of maxillofacial anatomic landmarks on 3-dimensional computed tomographic images determined with the 95% confidence ellipse method. Angle Orthod 78:396–402
Funding
The work was supported by the Chang Gung Memorial Hospital, Taiwan (CMRPG5K0181) and the Ministry of Science and Technology, Taiwan (MOST 108–2314-B-182–010).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in the study were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all participants.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liao, YF., Atipatyakul, P., Chen, YH. et al. Skeletal stability after bimaxillary surgery with surgery-first approach for class III asymmetry is not related to virtual surgical occlusal contact. Clin Oral Invest 26, 4935–4945 (2022). https://doi.org/10.1007/s00784-022-04462-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04462-5