Abstract
Objective
The purpose of this study is to retrospectively explore the utilization of coralline hydroxyapatite in maxillary sinus augmentation.
Method
One hundred and eighteen cases of sinus lift with coralline hydroxyapatite (CHA) were included in this study. In detail, simultaneous implantation was conducted in 78 patients (174 implants) and delayed implantation was done in 40 cases (82 implants) around 6 months after bone transplantation. The clinical features and X-ray radiographs after operation were analyzed to evaluate osseointegration procedures according to a planned medical follow-up. In the delayed group, around 6 months, a bone biopsy was taken just during implant placement in order to evaluate the new formed bone from a histological and histomorphometrical point of view. A further 6 months later, abutment connection was performed, and the patients received prosthetic restoration of the missing teeth.
Result
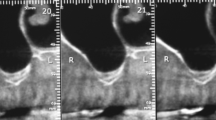
Clinically, the incisions healed well. No abnormal reactions were found during follow-up period. All the 174 simultaneous implants were successful after 1–5 years of medical review; Out of 82 delayed implants, 3 were found to be loose. Histologically, all the specimens showed signs of active remodeling, and all the tissues had a large amount of osteocyte at sixth month after sinus augmentation. New bone formed dramatically. Radiologically, the density of CHA gradually reduced since the beginning of the third month, and CHA may be completely resolved at about fifth year.
Conclusion
CHA is proven an ideal bone graft material for its reliable clinical results and favorable histocompatibility in the treatment of sinus atrophy or other kinds of insufficient bone volume in this region. Moreover, CHA’s signal application can achieve desired clinical effect.
Clinical relevance
This study shows the clinic application of CHA in maxillary sinus augmentation. Compared with popular mixture of autogenous bone and grafting materials, our results show CHA’s signal application can achieve ideal osseointegration interface and satisfying clinic effect.





Similar content being viewed by others
References
Tatum OH (1986) Maxillary and sinus implant reconstruction. Dent Clin North Am 30:207–229
Tatum OH Jr, Lebowitz MS, Tatum CA et al (1993) Sinus augmentation: rationale, development, long-term results. N Y State Dent J 59:43–48
Raghoebar GM et al (1997) Bone grafting of the floor of the maxillary sinus for placement of endosseous implants. J Oral Maxillofac Surg 35:119–125
Furst G, Gruber R, Tangl S et al (2003) Sinus grafting with autogenous plateletrich plasma and bovine hydroxyapatite. A histomorphometric study in minipigs. Clin Oral Implants Res 14:500–508
Block MS, Kent JN (1993) Maxillary sinus grafting for totally and partially edentulous patients. J Am Dent Assoc 124:139–143
Contar CM, Sarot JR, Bordini J Jr, Galvão GH, Nicolau GV, Machado MA (2009) Maxillary ridge augmentation with fresh-frozen bone allografts. J Oral Maxillofac Surg 67:1280–1285
Cosci F, Luccioli M (2000) A new sinus lift technique in conjunction with placement of 256 implants: a 6-year retrospective study. Implant Dent 9:363–368
Tong DC, Rioux K, Drangsholt M et al (1998) A review of survival rates for implants placed in grafted maxillary sinuses using meta-analysis. Int J Oral Maxillofac Implants 12:175–182
Jensen OT, Greer R (1992) Immediate placement of osseointegrated implant into the maxillary sinus augmented with mineralized cancellous allograft and Gore-Tex. Second-stage surgical and histological findings. In: Laney WR, Tolman D (eds) Tissue integration in oral, orthopedic and maxillofacial reconstruction Quintessence, Chicago, pp 321–333
Boo JS, Yamada Y, Okazaki Y, Hibino Y, Okada K, Hata K-I, Yoshikawa T, Sugiura Y, Ueda M (2002) Tissue-engineered bone using mesenchymal stem cells and a biodegradable scaffold. J Craniofac Surg 13:231–239
Tawil G, Mawla M (2001) Sinus floor elevation using a bovine bone mineral (Bio-Oss) with or without the concomitant use of bilayered collagen barrier (Bio-Guide): a clinical report of immediate and delayed implant placement. Int J Oral Maxillofac Implants 16:713–721
Becker W, Becker BE, Polizzi G et al (1994) Autogenous bone grafting of bone defects adjacent to implants placed into immediate extraction sockets in patients: a prospective study. Int J Oral Maxillofac Implants 9:389–396
van den Bergh JP, ten Bruggenkate CM, Krekeler G, Tuinzing DB (1998) Sinus floor elevation and grafting with autogenous iliac crest bone. Clin Oral Implants Res 9:429–435
Hallman M, Sennerby L, Zetterqvist L, Lundgren S (2005) A 3-year prospective follow-up study of implant-supported fixed prostheses in patients subjected to maxillary sinus floor augmentation with an 80:20 mixture of deproteinized bovine bone and autogenous bone. Clinical, radiographic and resonance frequency analysis. Int J Oral Maxillofac Surg 34:273–280
Marchetti C, Pieri F, Trasarti S et al (2007) Impact of implants surface and grafting protocol on clinical outcomes of endosseous implants. Int J Oral Maxillofac Implants 22:399–407
Bornstein MM, Chappuis V, VonArx T et al (2008) Performance of dental implants after staged sinus floor elevation (SFE) procedures: 5 year results of a prospective study in partially edentulous patients. Clin Oral Implants Res 19:1034–1043
Chiapasco M, Zaniboni M, Rimondini L (2008) Dental implants placed in grafted maxillary sinuses: a retrospective analysis of clinical outcome according to the initial clinical situation and a proposal of defect classification. Clin Oral Implants Res 19:416–428
Mazor Z, Peleq M, Garq AK et al (2007) The use of hydroxyapatite bone cement for sinus floor augmentation with simultaneous implant placement in the atrophic maxilla. A report of 10 cases. J Periodontol 71:1187–1194
Yukna RA (1994) Clinical evaluation of coralline calcium carbonate as bone replacement graft material in human periodontal osseous defects. J Periodontol 65:177–185
Pollick S, Shors EC, Holmes RE et al (1995) Bone formation and implant degradation of coralline porous ceramics placed in bone and ectopic sites. J Oral Maxillofac Surg 53:915–922
Roudier M, Bouchon C, Rouvillain JL et al (1995) The resorption of bone-implanted corals varies with porosity but also with the host reaction. J Biomed Mater Res 29(8):909–915
Byrd HS, Hobar PC, Shewmake K (1993) Augmentation of the craniofacial skeleton with porous hydroxyapatite granules. Plast Reconstr Surg 91:15–22, discussion 23–16
Rosen HM, McFarland MM (1990) The biological behavior of hydroxyapatite implanted into the maxillofacial skeleton. Plast Reconstr Surg 85:718–723
Waite PD, Matukas VJ (1986) Zygomatic augmentation with hydroxylapatite: a preliminary report. J Oral Maxillofac Surg 44:349–352
Pjetursson BE, Tan WC, Zwahlen M, Lang NP (2008) A systematic review of the success of sinus floor elevation and survival of implant inserted in combination with sinus floor elevation. J Clin Periodontol 35(Suppl):216–240
Jensen OT (1990) Allogenic bone or hydroxylapatite for the sinus lift procedure? J Oral Maxillofac Surg 48:771–776
Garg AK, Quinones CR (1997) Augmentation of the maxillary sinus: a surgical technique. Pract Periodontics Aesthet Dent 9:211–219
Aghaloo TL, Moy PK (2007) Which hard tissue augmentation techniques are the most successful in furnishing bony support for implant placement? Int J Oral Maxillofac Implants 22(Suppl):49–70
Raghoebar GM, Brouwer TJ, Reintsema H, Van Oort RP (1993) Augmentation of the maxillary sinus floor with autogenous bone for the placement of endosseous implants: a preliminary report. J Oral Maxillofac Surg 51:1198–1203
Nkenke E, Stelzle F (2009) Clinical outcomes of sinus floor augmentation for implant placement using autogenous bone or bone substitutes: a systematic review. Clin Oral Impl Res 20:124–133
Becker W, Schenk R, Higuchi K et al (1995) Variations in bone regeneration adjacent to implants augmented with barrier membranes alone or with demineralized freeze-dried bone or autologous grafts in dogs. Int J Oral Maxillofac Implants 10:143–154
Piattelli A, Scarano A, Corigliano M et al (1996) Comparison of bone regeneration with the use of mineralized and demineralized freeze-dried bone allografts: a histological and histochemical study in man. Biomaterials 17:1127–1131
Gomes KU, Carlini JL, Biron C, Rapoport A, Dedivitis RA (2008) Use of allogeneic bone graft in maxillary reconstruction for installation of dental implants. J Oral Maxillofac Surg 66:2335–2338
Yaremchuk MJ (2003) Facial skeletal reconstruction using porous polyethylene implants. Plast Reconstr Surg 111:1818–1827
Haas R, Donath K, Födinger M, Watzek G (1998) Bovine hydroxyapatite for maxillary sinus grafting: comparative histomorphometric findings in sheep. Clin Oral Implants Res 9:107–116
Hürzeler MB, Quinones CR, Kirsch A, Gloker C, Schüpbach P, Strub JR, Caffesse RG (1997) Maxillary sinus augmentation using different grafting materials and dental implants in monkeys. Part I. Evaluation of anorganic bovine-derived bone matrix. Clin Oral Implants Res 8:476–486
Rodoni LR, Glauser R, Hämmerle CH (2005) Implants in the posterior maxilla: a comparative clinical and radiologic study. Int J Oral Maxillofac Implants 20:231–237
Mangano C, Scarano A, Lezzi G et al (2006) Maxillary sinus augmentation using an engineered porous hydroxyappatite: a clinical, histological and transmission electron microscopy study in man. J Oral Implantol 22:122–131
Ethics
The study was approved by the Ethics Committee of Guanghua School of Stomatology, Sun Yat-sen University.
Conflict of interest
There is no conflict of interest. This paper was financially supported by grant A2008225 of the Medical Research Foundation Program of Guangdong Province and grant 2008B030301087 of Science and Technology Plan Program of Guangdong Province Department of Science and Technology.
Author information
Authors and Affiliations
Corresponding author
Additional information
Authors Zhi-Bin Luo and Qing-Bin Zhang contributed equally to this paper.
Rights and permissions
About this article
Cite this article
Luo, ZB., Zhang, QB., Zhang, ZQ. et al. Performance of coralline hydroxyapatite in sinus floor augmentation: a retrospective study. Clin Oral Invest 17, 2003–2010 (2013). https://doi.org/10.1007/s00784-013-0922-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-013-0922-6