Abstract
Objective
Decompressive hinge craniotomy (DHC) is an alternative treatment option to decompressive craniectomy (DC) for elevated intracranial pressure (ICP). The aim of this study was to characterize the difference in pressure–volume relationship between DHC and DC.
Methods
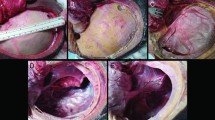
We compared the intracranial pressure–volume relationship in a human cadaver model following either DHC, DC, or fixing of the bone plate by titanium clamps. We inserted an intracranial expandable device in two human cadaver specimens, performed either DHC, DC, or bone plate fixation, and gradually increased the intracranial volume while measuring ICP. Following DHC, we also performed CT-scans at pre-defined intervals.
Results
Before ICP exceeded a threshold of 20 mmHg, a fixed bone plate tolerated an increase of 130 ml of intracranial volume, while DHC and DC allowed an increase of 190 ml and 290 ml, respectively. CT-derived calculations following DHC determined that the increase in intracranial volume at ICP 22 mmHg was 65 ml, the maximal increase of intracranial volume was 84 ml, the maximal bone displacement was 21 mm, and the bone plate volume to be 82 ml. Manual stress test of the hinged bone plate did not allow misalignment or intracranial displacement of the bone plate.
Conclusion
DHC increases the intracranial volume by up to 84 ml and allows for approximately 60 ml increase of intracranial volume before ICP exceeds 20 mmHg. This indicates, when comparing with results from previous studies of herniation volumes, that DHC will be sufficient in many patients with head injury or cerebral infarction with treatment refractory intracranial hypertension.




Similar content being viewed by others
References
Abode-Iyamah KO, Stoner KE, Close LN, DeVries Watson NA, Flouty OE, Grosland NM, Howard MA 3rd (2018) Volume of brain herniation after decompressive craniectomy in patients with traumatic brain injury. World Neurosurg 118:e414–e421
Adeleye AO (2016) Clinical and radiologic outcome of a less invasive, low-cost surgical technique of osteoplastic decompressive craniectomy. J Neurol Surgery, Part A Cent Eur Neurosurg. https://doi.org/10.1055/s-0035-1566115
Brasil S, Solla DJF, Nogueira R de C, Jacobsen Teixeira M, Malbouisson LMS, Paiva WS (2021) Intracranial compliance assessed by intracranial pressure pulse waveform. Brain Sci. https://doi.org/10.3390/brainsci11080971
Gutman MJ, How E, Withers T (2017) The floating anchored craniotomy. Surg Neurol Int. https://doi.org/10.4103/sni.sni_460_16
Kano T, Kurosaki S, Wada H (2012) Retrospective analysis of hinge technique for head trauma or stroke. Neurol Med Chir (Tokyo). https://doi.org/10.2176/nmc.52.816
Kenning TJ, Gandhi RH, German JW (2009) A comparison of hinge craniotomy and decompressive craniectomy for the treatment of malignant intracranial hypertension: early clinical and radiographic analysis. Neurosurg Focus. https://doi.org/10.3171/2009.4.FOCUS0960
Kenning TJ, Gooch MR, Gandhi RH, Shaikh MP, Boulos AS, German JW (2012) Cranial decompression for the treatment of malignant intracranial hypertension after ischemic cerebral infarction: decompressive craniectomy and hinge craniotomy. J Neurosurg 116(6):1289–1298
Khanna R (2017) Dynamic decompressive craniotomy with a novel reversibly expandable plate. J Neurol Surgery, Part A Cent Eur Neurosurg. https://doi.org/10.1055/s-0036-1594013
Khanna R, Ferrara L, Khanna S (2019) Biomechanics of a novel reversibly expandable dynamic craniotomy bone flap fixation plate. J Neurosurg. https://doi.org/10.3171/2018.8.JNS172614
Layard Horsfall H, Mohan M, Devi BI et al (2019) Hinge/floating craniotomy as an alternative technique for cerebral decompression: a scoping review. Neurosurg Rev. https://doi.org/10.1007/s10143-019-01180-7
Li X, Von Holst H, Kleiven S (2013) Decompressive craniectomy causes a significant strain increase in axonal fiber tracts. J Clin Neurosci. https://doi.org/10.1016/j.jocn.2012.04.019
Lilja-Cyron A, Andresen M, Kelsen J, Andreasen TH, Fugleholm K, Juhler M (2019) Long-term effect of decompressive craniectomy on intracranial pressure and possible implications for intracranial fluid movements. Neurosurgery. https://doi.org/10.1093/neuros/nyz049
Raposio E (2018) Scalp expansion: surgical considerations and possible future directions. Indian J Plast Surg Off Publ Assoc Plast Surg India 51(1):84–88
Raposio E, Cella A, Barabino P, Santi P (1999) Ineffectiveness of acute scalp expansion. Plast Reconstr Surg 103(6):1645–1649
Sauvigny T, Göttsche J, Czorlich P, Vettorazzi E, Westphal M, Regelsberger J (2018) Intracranial pressure in patients undergoing decompressive craniectomy: new perspective on thresholds. J Neurosurg 128(3):819–827
Stoner KE, Abode-Iyamah KO, Grosland NM, Howard MA (2016) Volume of brain herniation in patients with ischemic stroke after decompressive craniectomy. World Neurosurg. https://doi.org/10.1016/j.wneu.2016.08.095
Wilhelmi BJ, Blackwell SJ, Mancoll JS, Phillips LG (1998) Creep vs. stretch: a review of the viscoelastic properties of skin. Ann Plast Surg 41(2):215–219
Zanaty M, Chalouhi N, Starke RM et al (2015) Complications following cranioplasty: incidence and predictors in 348 cases. J Neurosurg. https://doi.org/10.3171/2014.9.JNS14405
Acknowledgements
We thank professor of clinical anatomy Jørgen Tranum-Jensen and laboratory chief technician Johnny Grandt, Institute of Cellular and Molecular Medicine, for invaluable help with cadaver specimens and technical support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This study was conducted with human cadaver specimens donated from consenting Danish adults with their intention of participating in medical science following their natural death. All patients and data are anonymous and the study is exempted from approval from the Danish Ethics Committee.
Competing interests
The authors declare no conflict of interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Neurosurgical intensive care
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Søndergaard, C.B., Villa, C., Jacobsen, C. et al. The intracranial pressure–volume relationship following decompressive hinge craniotomy compared to decompressive craniectomy—a human cadaver study. Acta Neurochir 165, 271–277 (2023). https://doi.org/10.1007/s00701-022-05409-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05409-1