Abstract
Background and purpose
DSA (digital subtraction angiography) is the gold standard for measuring carotid artery stenosis (CS). Yet, the correlation between DSA and stenosis is not well documented.
Material and methods
We compared CS as measured by DSA to carotid artery specimens obtained from carotid endarterectomy surgery. Patients were divided into three groups according to NASCET criteria (North American Symptomatic Carotid Endarterectomy Trial): stenosis of 30–49% (mild), stenosis of 50–69% (moderate), and stenosis of 70–99% (severe).
Results
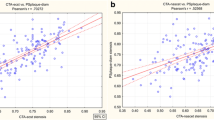
This prospective cohort study involved 644 patients. The mean stenosis in the mild stenosis group (n = 128 patients) was 54% ECST (European Carotid Surgery Trial), 40% NASCET, and 72% ESs (endarterectomy specimens). The mean absolute difference between ECST and NASCET was 14%. The mean stenosis in the moderate stenosis group (n = 347 patients) was 66% ECST, 60% NASCET, and 77% ES. The mean absolute difference between ECST and NASCET was 6%. The mean stenosis in the severe group (n = 169 patients) was 80% ECST, 76% NASCET, and 79% ES. No significant correlation coefficients were found between DSA and ES methods. In the mild group, the CC was 0.16 (ESCT) and 0.13 (NASCET); in the moderate group, the CC was 0.05 (ESCT) and 0.01 (NASCET); and in the severe group, the CC was 0.23 (ESCT) and 0.10 (NASCET). For all groups combined, CC was 0.22 for the ECST and 0.20 for the NASCET method.
Conclusion
The relationship between DSA and ES methods to measure CS is almost random. This lack of a relationship between the DSA and ES techniques questions the validity of current DSA-based guidelines.




Similar content being viewed by others
References
Aboyans V, Ricco JB, Bartelink MEL, Bjorck M, Brodmann M, Cohnert T, Collet JP, Czerny M, De Carlo M, Debusa S, Espinola-Klein C, Kahan T, Kownator S, Mazzolai L, Naylora AR, Roffi M, Rotherb J, Sprynger M, Tendera M, Tepe G, Venermoa M, Vlachopoulos C, Desormais I (2018) 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS). Rev Esp Cardiol 71:111. https://doi.org/10.1016/j.rec.2017.12.014
Alexandrov AV, Bladin CF, Maggisano R, Norris JW (1993) Measuring carotid stenosis. Time for a reappraisal. Stroke 24:1292–1296. https://doi.org/10.1161/01.str.24.9.1292
Anzalone N, Scomazzoni F, Castellano R, Strada L, Righi C, Politi LS, Kirchin MA, Chiesa R, Scotti G (2005) Carotid artery stenosis: intraindividual correlations of 3D time-of-flight MR angiography, contrast-enhanced MR angiography, conventional DSA, and rotational angiography for detection and grading. Radiology 236:204–213. https://doi.org/10.1148/radiol.2361032048
Boehme AK, Esenwa C, Elkind MS (2017) Stroke risk factors, genetics, and prevention. Circ Res 120:472–495. https://doi.org/10.1161/CIRCRESAHA.116.308398
Chappell FM, Wardlaw JM, Young GR, Gillard JH, Roditi GH, Yip B, Pell JP, Rothwell PM, Brown MM, Gough MJ, Randall MS (2009) Carotid artery stenosis: accuracy of noninvasive tests–individual patient data meta-analysis. Radiology 251:493–502. https://doi.org/10.1148/radiol.2512080284
Endarterectomy for asymptomatic carotid artery stenosis (1995) Executive Committee for the Asymptomatic Carotid Atherosclerosis Study. JAMA 273:1421–1428
Ferguson GG, Eliasziw M, Barr HW, Clagett GP, Barnes RW, Wallace MC, Taylor DW, Haynes RB, Finan JW, Hachinski VC, Barnett HJ (1999) The North American Symptomatic Carotid Endarterectomy Trial : surgical results in 1415 patients. Stroke 30:1751–1758
Isner JM, Kishel J, Kent KM, Ronan JA Jr, Ross AM, Roberts WC (1981) Accuracy of angiographic determination of left main coronary arterial narrowing. Angiographic–histologic correlative analysis in 28 patients. Circulation 63:1056–1064. https://doi.org/10.1161/01.cir.63.5.1056
Kashyap VS, Pavkov ML, Bishop PD, Nassoiy SP, Eagleton MJ, Clair DG, Ouriel K (2008) Angiography underestimates peripheral atherosclerosis: lumenography revisited. J Endovasc Ther : Off J Int Soc Endovasc Spec 15:117–125. https://doi.org/10.1583/07-2249R.1
Kernan WN, Ovbiagele B, Black HR, Bravata DM, Chimowitz MI, Ezekowitz MD, Fang MC, Fisher M, Furie KL, Heck DV, Johnston SC, Kasner SE, Kittner SJ, Mitchell PH, Rich MW, Richardson D, Schwamm LH, Wilson JA, American Heart Association Stroke Council CoC, Stroke Nursing CoCC, Council on Peripheral Vascular D (2014) Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 45:2160–2236. https://doi.org/10.1161/STR.0000000000000024
Mayberg MR, Wilson SE, Yatsu F, Weiss DG, Messina L, Hershey LA, Colling C, Eskridge J, Deykin D, Winn HR (1991) Carotid endarterectomy and prevention of cerebral ischemia in symptomatic carotid stenosis. Veterans Affairs Cooperative Studies Program 309 Trialist Group. JAMA 266:3289–3294
Naylor AR, Ricco JB (2018) Response to “Re: Management of Atherosclerotic Carotid and Vertebral Artery Disease: 2017 Clinical Practice Guidelines of the European Society for Vascular Surgery (ESVS).” Eur J Vasc Endovasc Surg : Off J Eur Soc Vasc Surg 55:902. https://doi.org/10.1016/j.ejvs.2018.03.023
Netuka D, Belsan T, Broulikova K, Mandys V, Charvat F, Malik J, Coufalova L, Bradac O, Ostry S, Benes V (2016) Detection of carotid artery stenosis using histological specimens: a comparison of CT angiography, magnetic resonance angiography, digital subtraction angiography and Doppler ultrasonography. Acta Neurochir 158:1505–1514. https://doi.org/10.1007/s00701-016-2842-0
Patel SG, Collie DA, Wardlaw JM, Lewis SC, Wright AR, Gibson RJ, Sellar RJ (2002) Outcome, observer reliability, and patient preferences if CTA, MRA, or Doppler ultrasound were used, individually or together, instead of digital subtraction angiography before carotid endarterectomy. J Neurol Neurosurg Psychiatry 73:21–28. https://doi.org/10.1136/jnnp.73.1.21
Schenk EA, Bond MG, Aretz TH, Angelo JN, Choi HY, Rynalski T, Gustafson NF, Berson AS, Ricotta JJ, Goodison MW et al (1988) Multicenter validation study of real-time ultrasonography, arteriography, and pathology: pathologic evaluation of carotid endarterectomy specimens. Stroke 19:289–296
Wardlaw JM, Chappell FM, Best JJ, Wartolowska K, Berry E, Research NHS, Development Health Technology Assessment Carotid Stenosis Imaging G (2006) Non-invasive imaging compared with intra-arterial angiography in the diagnosis of symptomatic carotid stenosis: a meta-analysis. Lancet 367:1503–1512. https://doi.org/10.1016/S0140-6736(06)68650-9
Randomised trial of endarterectomy for recently symptomatic carotid stenosis: final results of the MRC European Carotid Surgery Trial (ECST) (1998). Lancet 351:1379–1387
Funding
The study was supported by Grant No. NV19-04–00270.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The study complied with the Helsinki Declaration of 1975 (as revised in 2004 and 2008). Ethics approval was obtained from the local institutional review board. All patients provided written informed consent.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Comments
This manuscript shows us, eloquently, that endarterectomy specimens in these authors’ series do not correlate well with DSA measurement findings in CEA patients. It is important work from an experienced and outstanding center, and worthy of our consideration.
The clinical relevance is less compelling now, since as the authors state, MRA, CTA or even DUS (the latter admittedly double-corroborated) have for the most part replaced DSA in their practice.
So we are at first dismayed that something we have believed in for so long may not have been as accurate as we had believed. But we must consider this. The major CEA cooperative trials have shown a benefit for surgery in properly selected cases, always measured with the gold standard of DSA. So even if DSA does not correlate well with ES, evaluation by DSA is still a valid method to improve stroke outcomes in patients. In other words, although DSA might not have been what it seemed, it still worked. Patients have been helped and strokes have been prevented by surgery that was planned with DSA data.
Now I might suggest that this outstanding group keep track of their ongoing ES specimens and compare them to MRA, CTA, or even DUS findings. We will look forward to seeing that data also.
Christopher M. Loftus
Philadelphia, PA, USA
This article is part of the Topical Collection on Vascular Neurosurgery—Ischemia
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Svoboda, N., Bradac, O., Mandys, V. et al. Diagnostic accuracy of DSA in carotid artery stenosis: a comparison between stenosis measured on carotid endarterectomy specimens and DSA in 644 cases. Acta Neurochir 164, 3197–3202 (2022). https://doi.org/10.1007/s00701-022-05332-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05332-5