Abstract
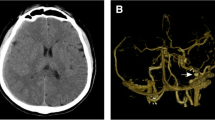
Here is reported a case of dural arteriovenous fistula (DAVF) formation following middle meningeal artery (MMA) embolization. A 64-year-old male patient was operated for a bilateral CSDH by burr-hole craniostomy. Prophylactic post-operative MMA embolization was performed with 300–500-μm calibrated microparticles. The patient was admitted 3 months later for a left CSDH recurrence. Digital subtraction angiography demonstrated formation of a superior sagittal sinus DAVF fed by both superficial temporal arteries. This case highlights the possible role of local tissue hypoxia as a significant component of DAVF pathogenesis. Moreover, it has potential implications for MMA embolization as a management strategy for CSDH.


Similar content being viewed by others
References
Shotar E, Meyblum L, Premat K et al (2020) Middle meningeal artery embolization reduces the post-operative recurrence rate of at-risk chronic subdural hematoma. J Neurointerventional Surg. https://doi.org/10.1136/neurintsurg-2020-016048
Piergallini L, Dargazanli C, Derraz I, Costalat V (2019) Immediate development of dural arteriovenous fistula after middle meningeal artery embolization: first angiographic demonstration. World Neurosurg. https://doi.org/10.1016/j.wneu.2019.04.246
Shotar E, Mathon B, Meyblum L, Lenck S, Premat K, Degos V, Sourour N-A, Clarençon F (2019) Letter to the Editor Regarding “Immediate Development of Dural Arteriovenous Fistula After Middle Meningeal Artery Embolization: First Angiographic Demonstration.” World Neurosurg 131:295–296
Gandhi D, Chen J, Pearl M, Huang J, Gemmete JJ, Kathuria S (2012) Intracranial dural arteriovenous fistulas: classification, imaging findings, and treatment. AJNR Am J Neuroradiol 33(6):1007–1013
Polster SP, Zeineddine HA, Baron J, Lee S-K, Awad IA (2018) Patients with cranial dural arteriovenous fistulas may benefit from expanded hypercoagulability and cancer screening. J Neurosurg 129(4):954–960
Tsai LK, Jeng JS, Liu HM, Wang HJ, Yip PK (2004) Intracranial dural arteriovenous fistulas with or without cerebral sinus thrombosis: analysis of 69 patients. J Neurol Neurosurg Psychiatry 75(11):1639–1641
Herman JM, Spetzler RF, Bederson JB, Kurbat JM, Zabramski JM (1995) Genesis of a dural arteriovenous malformation in a rat model. J Neurosurg 83(3):539–545
Lawton MT, Jacobowitz R, Spetzler RF (1997) Redefined role of angiogenesis in the pathogenesis of dural arteriovenous malformations. J Neurosurg 87(2):267–274
Wang S-S, Li C-H, Zhang X-J, Wang R-M (2014) Investigation of the mechanism of dural arteriovenous fistula formation induced by high intracranial venous pressure in a rabbit model. BMC Neurosci 15:101
Zhu Y, Lawton MT, Du R, Shwe Y, Chen Y, Shen F, Young WL, Yang G-Y (2006) Expression of hypoxia-inducible factor-1 and vascular endothelial growth factor in response to venous hypertension. Neurosurgery 59(3):687–696 discussion 687-696
Ishikawa T, Sato S, Sasaki T, Matsumoto M, Suzuki K, Itakura T, Kodama N, Hiraiwa K (2007) Histologic study of arteriovenous shunts in the normal dura mater adjacent to the transverse sinus. Surg Neurol 68(3):272–276 discussion 276
Mironov A (1994) Pathogenetical consideration of spontaneous dural arteriovenous fistulas (DAVFs). Acta Neurochir (Wien) 131(1–2):45–58
Waltham M, Burnand KG, Collins M, Smith A (2000) Vascular endothelial growth factor and basic fibroblast growth factor are found in resolving venous thrombi. J Vasc Surg 32(5):988–996
Tirakotai W, Bertalanffy H, Liu-Guan B, Farhoud A, Sure U (2005) Immunohistochemical study in dural arteriovenous fistulas and possible role of local hypoxia for the de novo formation of dural arteriovenous fistulas. Clin Neurol Neurosurg 107(6):455–460
Uranishi R, Nakase H, Sakaki T (1999) Expression of angiogenic growth factors in dural arteriovenous fistula. J Neurosurg 91(5):781–786
Friede RL, Schachenmayr W (1978) The origin of subdural neomembranes. II. Fine structural of neomembranes. Am J Pathol 92(1):69–84
Pouvelle A, Pouliquen G, Premat K, Chougar L, Lenck S, Degos V, Sourour N-A, Mathon B, Clarençon F, Shotar E (2020) Larger middle meningeal arteries on computed tomography angiography in patients with chronic subdural hematomas as compared to matched controls. J Neurotrauma. https://doi.org/10.1089/neu.2020.7168
Yamashima T, Yamamoto S, Friede RL (1983) The role of endothelial gap junctions in the enlargement of chronic subdural hematomas. J Neurosurg 59(2):298–303
Clarençon F, Di Maria F, Gabrieli J, Carpentier A, Pistochi S, Bartolini B, Zeghal C, Chiras J, Sourour N-A (2016) Double-lumen balloon for Onyx® embolization via extracranial arteries in transverse sigmoid dural arteriovenous fistulas: initial experience. Acta Neurochir (Wien) 158(10):1917–1923
Tirakotai W, Benes L, Kappus C, Sure U, Farhoud A, Bien S, Bertalanffy H (2007) Surgical management of dural arteriovenous fistulas with transosseous arterial feeders involving the jugular bulb. Neurosurg Rev 30(1):40–48 discussion 48-49
Clarençon F, Shotar E, Pouvelle A, Mouyal S, Lenck S, Premat K, Cornu P, Sourour N-A (2020) Direct puncture of the superficial temporal artery for ethylene vinyl alcohol embolization of a type 3 arteriovenous fistula with a dual lumen balloon. J Neurointerventional Surg. https://doi.org/10.1136/neurintsurg-2020-016351
Kerber CW, Newton TH (1973) The macro and microvasculature of the dura mater. Neuroradiology 6(4):175–179
Borden JA, Wu JK, Shucart WA (1995) A proposed classification for spinal and cranial dural arteriovenous fistulous malformations and implications for treatment. J Neurosurg 82(2):166–179
Cognard C, Gobin YP, Pierot L, Bailly AL, Houdart E, Casasco A, Chiras J, Merland JJ (1995) Cerebral dural arteriovenous fistulas: clinical and angiographic correlation with a revised classification of venous drainage. Radiology 194(3):671–680
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Patient consent
The next of kin/guardian has consented to the submission of the case report to the journal.
Additional information
Comments
The authors report an interesting observation of a formation of a DAVF secondary to MMA embolization for treatment of a CSDH. This case deserves attention for two reasons:
1) Although not proven, local tissue hypoxia appears here the most likely explanation for the formation of the DAVF and may contribute to our general understanding of the pathogenesis in these lesions.
2) The potential development of a dural AV shunt following a benign procedure such as MMA embolization is, if observed more frequently, not trivial for the management of CSDH patients. More time and data should tell whether or not these aspects will gain clinical relevance. Systematic FU imaging in these patients should possibly be considered as small dural AV shunts can be clinically silent.
Goetz Benndorf,
Denmark
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Vascular Neurosurgery
Rights and permissions
About this article
Cite this article
Shotar, E., Premat, K., Barberis, E. et al. Dural arteriovenous fistula formation following bilateral middle meningeal artery embolization for the treatment of a chronic subdural hematoma: a case report. Acta Neurochir 163, 1069–1073 (2021). https://doi.org/10.1007/s00701-020-04696-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-020-04696-w