Abstract
Background
Minimally invasive spine surgery (MISS) has been increasingly advocated during the last decade with new studies being reported every year. Minimally invasive spine procedures, such as minimally invasive transforaminal interbody fusion (MI-TLIF), have been introduced to reduce approach-related muscle trauma, to minimise blood loss, and to achieve faster wound healing, quicker ambulation and earlier patient discharge.
Methods
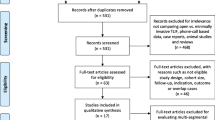
The aim of this article was to give a comprehensive review of the available English literature comparing open TLIF with MI-TLIF techniques published or available online between 1990 and 2014 as identified by an electronic database search on http://www.ncbi.nlm.nih.gov/pubmed. Fourteen relevant studies comparing MI-TLIF and open TLIF cohorts could be identified.
Results and conclusion
MI-TLIF seems to be a valid alternative to open TLIF. Both methods yield good clinical results with similar improvements of Oswestry Disability Index (ODI) and visual analogue scale (VAS) on follow-up. There seems to be no significant differences in clinical outcome and fusion rates on comparison. These results are consistent throughout all reported studies in this review. The most pronounced benefits of MI-TLIF are a significant reduction of blood loss, shorter lengths of hospital stay (LOHS) and lower surgical site infection rates. On the downside, MI-TLIF seems to be associated with significantly higher intraoperative radiation doses, a shallow learning curve, at least in the beginning, longer operating times and potentially more frequent implant failures/cage displacements and revision surgeries.


Similar content being viewed by others
References
Adogwa O, Johnson K, Min ET, Issar N, Carr KR, Huang K, Cheng J (2012) Extent of intraoperative muscle dissection does not affect long-term outcomes after minimally invasive surgery versus open-transforaminal lumbar interbody fusion surgery: A prospective longitudinal cohort study. Surg Neurol Int 3:S355–S361
Adogwa O, Parker SL, Bydon A, Cheng J, McGirt MJ (2011) Comparative effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion: 2-year assessment of narcotic use, return to work, disability, and quality of life. J Spinal Disord Tech 24:479–484
Authors on behalf of I, Stewart FA, Akleyev AV, Hauer-Jensen M, Hendry JH, Kleiman NJ, Macvittie TJ, Aleman BM, Edgar AB, Mabuchi K, Muirhead CR, Shore RE, Wallace WH (2012) ICRP publication 118: ICRP statement on tissue reactions and early and late effects of radiation in normal tissues and organs—threshold doses for tissue reactions in a radiation protection context. Ann ICRP 41:1–322
Beringer WF, Mobasser JP (2006) Unilateral pedicle screw instrumentation for minimally invasive transforaminal lumbar interbody fusion. Neurosurg Focus 20:E4
Brodano GB, Martikos K, Lolli F, Gasbarrini A, Cioni A, Bandiera S, Di Silvestre M, Boriani S, Greggi T (2013) Transforaminal lumbar interbody fusion in degenerative disc disease and spondylolisthesis grade I: minimally invasive versus open surgery. J Spinal Disord Tech 33(3):269–275
Cheng JS, Park P, Le H, Reisner L, Chou D, Mummaneni PV (2013) Short-term and long-term outcomes of minimally invasive and open transforaminal lumbar interbody fusions: is there a difference? Neurosurg Focus 35:E6
Cloward RB (1952) The treatment of ruptured lumbar intervertebral disc by vertebral body fusion. III Method of use of banked bone. Ann Surg 136:987–992
Cloward RB (1981) Spondylolisthesis: treatment by laminectomy and posterior interbody fusion. Clin Orthop Relat Res 154:74–82
Dhall SS, Wang MY, Mummaneni PV (2008) Clinical and radiographic comparison of mini-open transforaminal lumbar interbody fusion with open transforaminal lumbar interbody fusion in 42 patients with long-term follow-up. J Neurosurg Spine 9:560–565
Eckman WW, Hester L, McMillen M (2014) Same-day discharge after minimally invasive transforaminal lumbar interbody fusion: a series of 808 cases. Clin Orthop Relat Res 472:1806–1812
Fan S, Hu Z, Zhao F, Zhao X, Huang Y, Fang X (2010) Multifidus muscle changes and clinical effects of one-level posterior lumbar interbody fusion: minimally invasive procedure versus conventional open approach. Eur Spine J 19:316–324
Foley KT, Holly LT, Schwender JD (2003) Minimally invasive lumbar fusion. Spine 28:S26–S35
Gejo R, Kawaguchi Y, Kondoh T, Tabuchi E, Matsui H, Torii K, Ono T, Kimura T (2000) Magnetic resonance imaging and histologic evidence of postoperative back muscle injury in rats. Spine 25:941–946
Gejo R, Matsui H, Kawaguchi Y, Ishihara H, Tsuji H (1999) Serial changes in trunk muscle performance after posterior lumbar surgery. Spine 24:1023–1028
Gu G, Zhang H, Fan G, He S, Cai X, Shen X, Guan X, Zhou X (2014) Comparison of minimally invasive versus open transforaminal lumbar interbody fusion in two-level degenerative lumbar disease. Int Orthop 38:817–824
Gurr KR, McAfee PC (1988) Cotrel-Dubousset instrumentation in adults. A preliminary report. Spine 13:510–520
Habib A, Smith ZA, Lawton CD, Fessler RG (2012) Minimally invasive transforaminal lumbar interbody fusion: a perspective on current evidence and clinical knowledge. Minim Invasive Surg 2012:657342
Harms JG, Jeszenszky D (1998) [The posterior, fenestrations, lumbar fusion in unilateral transforaminal technology]. Oper Orthop Traumatol 10:90–102
Hubbe U, Sircar R, Scheiwe C, Scholz C, Kogias E, Kruger MT, Volz F, Klingler JH (2015) Surgeon, staff, and patient radiation exposure in minimally invasive transforaminal lumbar interbody fusion: impact of 3D fluoroscopy-based navigation partially replacing conventional fluoroscopy: study protocol for a randomized controlled trial. Trials 16:142
Humphreys SC, Hodges SD, Patwardhan AG, Eck JC, Murphy RB, Covington LA (2001) Comparison of posterior and transforaminal approaches to lumbar interbody fusion. Spine 26:567–571
Isaacs RE, Podichetty VK, Santiago P, Sandhu FA, Spears J, Kelly K, Rice L, Fessler RG (2005) Minimally invasive microendoscopy-assisted transforaminal lumbar interbody fusion with instrumentation. J Neurosurg Spine 3:98–105
Jang JS, Lee SH (2005) Minimally invasive transforaminal lumbar interbody fusion with ipsilateral pedicle screw and contralateral facet screw fixation. J Neurosurg Spine 3:218–223
Karikari IO, Isaacs RE (2010) Minimally invasive transforaminal lumbar interbody fusion: a review of techniques and outcomes. Spine 35:S294–301
Kawaguchi Y, Matsui H, Tsuji H (1996) Back muscle injury after posterior lumbar spine surgery. A histologic and enzymatic analysis. Spine 21:941–944
Lau D, Khan A, Terman SW, Yee T, La Marca F, Park P (2013) Comparison of perioperative outcomes following open versus minimally invasive transforaminal lumbar interbody fusion in obese patients. Neurosurg Focus 35:E10
Lau D, Lee JG, Han SJ, Lu DC, Chou D (2011) Complications and perioperative factors associated with learning the technique of minimally invasive transforaminal lumbar interbody fusion (TLIF). J Clin Neurosci 18:624–627
Lee DY, Jung TG, Lee SH (2008) Single-level instrumented mini-open transforaminal lumbar interbody fusion in elderly patients. J Neurosurg Spine 9:137–144
Lee KH, Yeo W, Soeharno H, Yue WM (2014) Learning curve of a complex surgical technique: minimally invasive transforaminal lumbar interbody fusion (MIS TLIF). J Spinal Disord Tech 27:E234–240
Lo WL, Lin CM, Yeh YS, Su YK, Tseng YY, Yang ST, Lin JW (2015) Comparing miniopen and minimally invasive transforaminal interbody fusion in single-level lumbar degeneration. Biomed Res Int 2015:168384
McGirt MJ, Parker SL, Lerner J, Engelhart L, Knight T, Wang MY (2011) Comparative analysis of perioperative surgical site infection after minimally invasive versus open posterior/transforaminal lumbar interbody fusion: analysis of hospital billing and discharge data from 5170 patients. J Neurosurg Spine 14:771–778
Mummaneni PV, Rodts GE Jr (2005) The mini-open transforaminal lumbar interbody fusion. Neurosurgery 57:256–261, discussion 256–261
Ozgur BM, Yoo K, Rodriguez G, Taylor WR (2005) Minimally-invasive technique for transforaminal lumbar interbody fusion (TLIF). Eur Spine J 14:887–894
Park P, Foley KT (2008) Minimally invasive transforaminal lumbar interbody fusion with reduction of spondylolisthesis: technique and outcomes after a minimum of 2 years’ follow-up. Neurosurg Focus 25:E16
Parker SL, Adogwa O, Witham TF, Aaronson OS, Cheng J, McGirt MJ (2011) Post-operative infection after minimally invasive versus open transforaminal lumbar interbody fusion (TLIF): literature review and cost analysis. Minimally Invasive Neurosurg 54:33–37
Peng CW, Yue WM, Poh SY, Yeo W, Tan SB (2009) Clinical and radiological outcomes of minimally invasive versus open transforaminal lumbar interbody fusion. Spine 34:1385–1389
Rodriguez-Vela J, Lobo-Escolar A, Joven E, Munoz-Marin J, Herrera A, Velilla J (2013) Clinical outcomes of minimally invasive versus open approach for one-level transforaminal lumbar interbody fusion at the 3- to 4-year follow-up. Eur Spine J 22:2857–2863
Schizas C, Tzinieris N, Tsiridis E, Kosmopoulos V (2009) Minimally invasive versus open transforaminal lumbar interbody fusion: evaluating initial experience. Int Orthop 33:1683–1688
Schwender JD, Holly LT, Rouben DP, Foley KT (2005) Minimally invasive transforaminal lumbar interbody fusion (TLIF): technical feasibility and initial results. J Spinal Disord Tech 18(Suppl):S1–S6
Shunwu F, Xing Z, Fengdong Z, Xiangqian F (2010) Minimally invasive transforaminal lumbar interbody fusion for the treatment of degenerative lumbar diseases. Spine 35:1615–1620
Sihvonen T, Herno A, Paljarvi L, Airaksinen O, Partanen J, Tapaninaho A (1993) Local denervation atrophy of paraspinal muscles in postoperative failed back syndrome. Spine 18:575–581
Stevens KJ, Spenciner DB, Griffiths KL, Kim KD, Zwienenberg-Lee M, Alamin T, Bammer R (2006) Comparison of minimally invasive and conventional open posterolateral lumbar fusion using magnetic resonance imaging and retraction pressure studies. J Spinal Disord Tech 19:77–86
Terman SW, Yee TJ, Lau D, Khan AA, La Marca F, Park P (2014) Minimally invasive versus open transforaminal lumbar interbody fusion: comparison of clinical outcomes among obese patients. J Neurosurg Spine 20:644–652
Vialle R, Court C, Khouri N, Olivier E, Miladi L, Tassin JL, Defives T, Dubousset J (2005) Anatomical study of the paraspinal approach to the lumbar spine. Eur Spine J 14:366–371
Villard J, Ryang YM, Demetriades AK, Reinke A, Behr M, Preuss A, Meyer B, Ringel F (2014) Radiation exposure to the surgeon and the patient during posterior lumbar spinal instrumentation: a prospective randomized comparison of navigated versus non-navigated freehand techniques. Spine 39:1004–1009
Villavicencio AT, Burneikiene S, Roeca CM, Nelson EL, Mason A (2010) Minimally invasive versus open transforaminal lumbar interbody fusion. Surg Neurol Int 1:12
Wang J, Zhou Y (2014) Perioperative complications related to minimally invasive transforaminal lumbar fusion: evaluation of 204 operations on lumbar instability at single center. Spine J 14:2078–2084
Wang J, Zhou Y, Feng Zhang Z, Qing Li C, Jie Zheng W, Liu J (2014) Comparison of the clinical outcome in overweight or obese patients after minimally invasive versus open transforaminal lumbar interbody fusion. J Spinal Disord Tech 27:202–206
Wang J, Zhou Y, Zhang ZF, Li CQ, Zheng WJ, Liu J (2010) Comparison of one-level minimally invasive and open transforaminal lumbar interbody fusion in degenerative and isthmic spondylolisthesis grades 1 and 2. Eur Spine J 19:1780–1784
Wang J, Zhou Y, Zhang ZF, Li CQ, Zheng WJ, Liu J (2011) Minimally invasive or open transforaminal lumbar interbody fusion as revision surgery for patients previously treated by open discectomy and decompression of the lumbar spine. Eur Spine J 20:623–628
Wang L, Wang Y, Li Z, Yu B, Li Y (2014) Unilateral versus bilateral pedicle screw fixation of minimally invasive transforaminal lumbar interbody fusion (MIS-TLIF): a meta-analysis of randomized controlled trials. BMC Surg 14:87
Wiltse LL, Bateman JG, Hutchinson RH, Nelson WE (1968) The paraspinal sacrospinalis-splitting approach to the lumbar spine. J Bone Joint Surg Am 50:919–926
Wiltse LL, Spencer CW (1988) New uses and refinements of the paraspinal approach to the lumbar spine. Spine 13:696–706
Yarascavitch BA, Chuback JE, Almenawer SA, Reddy K, Bhandari M (2012) Levels of evidence in the neurosurgical literature: more tribulations than trials. Neurosurgery 71:1131–1137, discussion 1137–1138
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
B.M.—consulting: DepuySynthes, Brainlab, Medtronic, Ulrich, Spineart, Reliviant; received funding from: DepuySynthes, Brainlab, Medtronic, Ulrich, Reliviant; Royalties/Patent: Ulrich, Spineart.
J.G.—consulting: BrainLab.
All other authors certify that they have no affiliations with or involvement in any organisation or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study formal consent is not required.
This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Vazan, M., Gempt, J., Meyer, B. et al. Minimally invasive transforaminal lumbar interbody fusion versus open transforaminal lumbar interbody fusion: a technical description and review of the literature. Acta Neurochir 159, 1137–1146 (2017). https://doi.org/10.1007/s00701-017-3078-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-017-3078-3