Abstract
Purpose
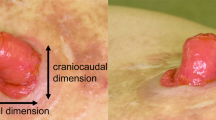
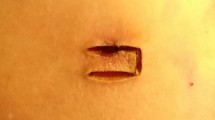
Peristomal skin disorders (PSDs) are common stoma-related complications. However, there is no standard method for the evaluation of PSDs, and the true incidence is unclear. There are also no reports on risk factors for severe PSDs. Therefore, this study was performed to analyze the incidence of PSD in temporary loop stoma based on the DET score and ABCD-stoma score and to determine the risk factors for all and severe PSDs.
Methods
A retrospective analysis of patient and surgical characteristics was carried out in 333 consecutive cases of stoma creation with loop ileostomy or colostomy performed at our hospital from January 2014 to December 2016.
Results
PSDs were diagnosed in 262 patients (78.7%), including 79 (23.7%) and 71 (21.3%) that were defined as severe based on DET and ABCD-stoma scores, respectively. Multivariate analyses showed that parastomal hernia was an independent risk factor for severe PSD defined by DET score and that adjuvant chemotherapy was an independent risk factor for severe PSD defined by the ABCD-stoma score.
Conclusions
Severe PSDs are associated with parastomal hernia when diagnosed by the DET score and with adjuvant chemotherapy when diagnosed by the ABCD-stoma score.
Similar content being viewed by others
References
Penna M, Hompes R, Arnold S, Wynn G, Austin R, Warusavitarne J, et al. Transanal total mesorectal excision: international registry results of the first 720 cases. Ann Surg. 2017;266:111–7.
Celerier B, Denost Q, Van Geluwe B, Pontallier A, Rullier E. The risk of definitive stoma formation at 10 years after low and ultralow anterior resection for rectal cancer. Colorectal Dis. 2016;18:59–66.
Yokota M, Ito M, Nishizawa Y, Kobayashi A, Saito N. the impact of anastomotic leakage on anal function following intersphincteric resection. World J Surg. 2017;41:2168–77.
Peeters KC, Tollenaar RA, Marijnen CA, Klein Kranenbarg E, Steup WH, Wiggers T, et al. Risk factors for anastomotic failure after total mesorectal excision of rectal cancer. Br J Surg. 2005;92:211–6.
Phatak UR, Kao LS, You YN, Rodriguez-Bigas MA, Skibber JM, Feig BW, et al. Impact of ileostomy-related complications on the multidisciplinary treatment of rectal cancer. Ann Surg Oncol. 2014;21:507–12.
Matthiessen P, Hallböök O, Rutegård J, Simert G, Sjödahl R. Defunctioning stoma reduces symptomatic anastomotic leakage after low anterior resection of the rectum for cancer: a randomized multicenter trial. Ann Surg. 2007;246:207–14.
Miyo M, Takemasa I, Ikeda M, Tujie M, Hasegawa J, Ohue M, et al. The influence of specific technical maneuvers utilized in the creation of diverting loop-ileostomies on stoma-related morbidity. Surg Today. 2017;47:940–50.
Szewczyk MT, Majewska G, Cabral MV, Hölzel-Piontek K. The effects of using a moldable skin barrier on peristomal skin condition in persons with an ostomy: results of a prospective, observational, multinational study. Ostomy Wound Manag. 2014;60:16–26.
Boland J, Brooks D. Topical application of a beclometasone steroid inhaler for treatment of stoma inflammation. Palliat Med. 2012;26:1055–6.
Pittman J, Rawl SM, Schmidt CM, Grant M, Ko CY, Wendel C, et al. Demographic and clinical factors related to ostomy complications and quality of life in veterans with an ostomy. J Wound Ostomy Cont Nurs. 2008;35:493–503.
Chambers SK, Meng X, Youl P, Aitken J, Dunn J, Baade P. A five-year prospective study of quality of life after colorectal cancer. Qual Life Res. 2012;21:1551–644.
Taneja C, Netsch D, Rolstad BS, Inglese G, Lamerato L, Oster G. Clinical and economic burden of peristomal skin complications in patients with recent ostomies. J Wound Ostomy Contin Nurs. 2017;44:350–7.
Jemec GB, Martins L, Claessens I, Ayello EA, Hansen AS, Poulsen LH, et al. Assessing peristomal skin changes in ostomy patients: validation of the Ostomy Skin Tool. Br J Dermatol. 2011;164:330–5.
Shabbir J, Britton DC. Stoma complications: a literature overview. Colorectal Dis. 2010;12:958–64.
Martins L, Ayello EA, Claessens I, Steen Hansen A, Hentze Poulsen L, Sibbald RG, et al. The ostomy skin tool: tracking peristomal skin changes. Br J Nurs. 2010;19:932–4.
Bafford AC, Irani JL. Management and complications of stomas. Surg Clin N Am. 2013;93:145–66.
Pace U, Rega D, Scala D, Montesarchio L, Delrio P. Skin bridge loop ileostomy: technical details. Tech Coloproctol. 2014;18:855–6.
Dziki Ł, Mik M, Trzciński R, Buczyński J, Darnikowska J, Spychalski M, et al. Evaluation of the early results of a loop stoma with a plastic rod in comparison to a loop stoma made with a skin bridge. Pol Przegl Chir. 2015;87:31–4.
Ostomy Guidelines Task Force, Goldberg M, Aukett LK, Carmel J, Fellows J, Folkedahl B, et al. Management of the patient with a fecal ostomy: best practice guideline for clinicians. J Wound Ostomy Contin Nurs. 2010;37:596–8.
Hendren S, Hammond K, Glasgow SC, Perry WB, Buie WD, Steele SR, et al. Clinical practice guidelines for ostomy surgery. Dis Colon Rectum. 2015;58:375–87.
Cressey BD, Belum VR, Scheinman P, Silvestri D, McEntee N, Livingston V, et al. Stoma care products represent a common and previously underreported source of peristomal contact dermatitis. Contact Dermat. 2017;76:27–33.
Colwell JC, Pittman J, Raizman R, Salvadalena G. A randomized controlled trial determining variances in ostomy skin conditions and the economic impact (ADVOCATE Trial). J Wound Ostomy Contin Nurs. 2018;45:37–42.
Meisner S, Lehur PA, Moran B, Martins L, Jemec GB. Peristomal skin complications are common, expensive, and difficult to manage: a population based cost modeling study. PLoS O ne. 2012;7:e37813.
Oliphant R, Czerniewski A, Robertson I, McNulty C, Waterston A, Macdonald A. The effect of adjuvant chemotherapy on stoma-related complications after surgery for colorectal cancer: a retrospective analysis. J Wound Ostomy Contin Nurs. 2015;42:494–8.
Rolstad BS, Erwin-Toth PL. Peristomal skin complications: prevention and management. Ostomy Wound Manag. 2004;50:68–77.
Almutairi D, LeBlanc K, Alavi A. Peristomal skin complications: what dermatologists need to know. Int J Dermatol. 2018;57:257–64.
Aquina CT, Iannuzzi JC, Probst CP, Kelly KN, Noyes K, Fleming FJ, et al. Parastomal hernia: a growing problem with new solutions. Dig Surg. 2014;31:366–76.
Kye BH, Kim HJ, Kim JG, Cho HM. Is it safe the reversal of a diverting stoma during adjuvant chemotherapy in elderly rectal cancer patients? Int J Surg. 2014;12:1337–411.
Erwin-Toth P, Stricker LJ, Rijswijk LV. Wound wise: peristomal skin complications. Am J Nurs. 2010;110:43–8.
de Gramont A, Figer A, Seymour M, Homerin M, Hmissi A, Cassidy J, et al. Leucovorin and fluorouracil with or without oxaliplatin as first-line treatment in advanced colorectal cancer. J Clin Oncol. 2000;18:2938–47.
Kokotis P, Schmelz M, Kostouros E, Karandreas N, Dimopoulos MA. Oxaliplatin-induced neuropathy: a long-term clinical and neurophysiologic follow-up study. Clin Colorectal Cancer. 2016;15:e133–e140140.
Lou Y, Wang Q, Zheng J, Hu H, Liu L, Hong D, et al. Possible pathways of capecitabine-induced hand-foot syndrome. Chem Res Toxicol. 2016;29:1591–601.
Konya C, Sanada H, Sugama J, Okuwa M, Kamatani Y, Nakagami G, et al. Skin injuries caused by medical adhesive tape in older people and associated factors. J Clin Nurs. 2010;19:1236–42.
Iizaka S, Asada M, Koyanagi H, Sasaki S, Naito A, Konya C, et al. The reliability and validity of color indicators using digital image analysis of peristomal skin photographs: results of a preliminary prospective clinical study. Ostomy Wound Manag. 2014;60:12–29.
Funding
The authors have no conflicts of interest regarding the financial aspects of the work in this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest with regard to this study.
Ethical approval
All procedures involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shiraishi, T., Nishizawa, Y., Nakajima, M. et al. Risk factors for the incidence and severity of peristomal skin disorders defined using two scoring systems. Surg Today 50, 284–291 (2020). https://doi.org/10.1007/s00595-019-01876-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-019-01876-9