Abstract
Purpose
Postoperative morbidity remains common after esophagectomy. There are currently few tools that can be used to estimate the incidence of complications. This study aimed to create a novel scoring system for predicting postoperative morbidity.
Methods
A total of 365 patients who underwent elective esophagectomy with two- or three-field lymphadenectomy for esophageal cancer were retrospectively analyzed. Patients were divided into development (n = 250) and validation datasets (n = 115). A scoring system was established by specifying the expected morbidity incidence values for all independent predictors in the development dataset, after which, the reproducibility was confirmed in the validation dataset.
Results
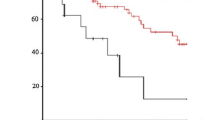
The incidence of any morbidity was 44.7 %. Male sex, severe emaciation (body mass index <18), a lower performance status (grade 1 or 2), operation ≥540 min and massive bleeding (blood loss/body weight ≥20) were independent predictors of postoperative morbidity. The total of all predictive scores was calculated. The incidence of any morbidity and of severe morbidity (Clavien–Dindo classification ≥IIIb) significantly correlated with the score after dividing the scores into three groups (≤8, 10 and 11 and ≥13). This finding was also confirmed in the validation dataset.
Conclusion
The current scoring system is considered to be useful for predicting postoperative morbidity after esophagectomy.


Similar content being viewed by others
References
Takemura M, Hori T, Fujiwara Y. Clinical outcomes and prognosis after thoracoscopic esophagectomy with two-field lymph node dissection for lower thoracic esophageal cancer. Anticancer Res. 2013;33:601–8.
Ferguson MK, Celauro AD, Prachand V. Assessment of a scoring system for predicting complications after esophagectomy. Dis Esophagus. 2011;24:510–5.
Valentí V, Hernández-Lizoain JL, Marínez-Regueira F, Bellver M, Rodríguez J, Díaz González JA, et al. Transthoracic oesophagectomy with lymphadenectomy in 100 oesophageal cancer patients: multidisciplinary approach. Clin Transl Oncol. 2011;13:899–903.
Dutta S, Al-Mrabt NM, Fullarton GM, Horgan PG, McMillan DC. A comparison of POSSUM and GPS models in the prediction of post-operative outcome in patients undergoing oesophago-gastric cancer resection. Ann Surg Oncol. 2011;18:2808–17.
Grotenhuis BA, van Hagen P, Reitsma JB, Lagarde SM, Wijnhoven BP, van Berge Henegouwen MI, et al. Validation of a nomogram predicting complications after esophagectomy for cancer. Ann Thorac Surg. 2010;90:920–5.
Dhungel B, Diggs BS, Hunter JG, Sheppard BC, Vetto JT, Dolan JP. Patient and peri-operative predictors of morbidity and mortality after esophagectomy: American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP), 2005–2008. J Gastrointest Surg. 2010;14:1492–501.
Wright CD, Kucharczuk JC, O’Brien SM, Grab JD, Allen MS. Predictors of major morbidity and mortality after esophagectomy for esophageal cancer: a society of thoracic surgeons general thoracic surgery database risk adjustment model. J Thorac Cardiovasc Surg. 2009;137:587–95.
Lagarde SM, Reitsma JB, Maris AK, van Berge Henegouwen MI, Busch OR, Obertop H, et al. Preoperative prediction of the occurrence and severity of complications after esophagectomy for cancer with use of a nomogram. Ann Thorac Surg. 2008;85:1938–45.
Thompson AM, Rapson T, Gilbert FJ, Park KG. Hospital volume does not influence long-term survival of patients undergoing surgery for oesophageal or gastric cancer. Br J Surg. 2007;94:578–84.
Merkow RP, Bilimoria KY, McCarter MD, Phillips JD, Decamp MM, Sherman KL, et al. Short-term outcomes after esophagectomy at 164 American College of Surgeons National Surgical Quality Improvement Program Hospitals: effect of operative approach and hospital-level variation. Arch Surg. 2012;147:1009–16.
Goldfaden D, Orringer MB, Appelman HD, Kalish R. Adenocarcinoma of the distal esophagus and gastric cardia. comparison of results of transhiatal esophagectomy and thoracoabdominal esophagogastrectomy. J Thorac Cardiovasc Surg. 1986;91:242–7.
Yoshida N, Watanabe M, Baba Y, Iwagami S, Ishimoto T, Iwatsuki M, et al. Risk factors for pulmonary complications after esophagectomy for esophageal cancer. Surg Today. 2014;44:526–32.
Zingg U, Smithers BM, Gotley DC, Smith G, Aly A, Clough A, et al. Factors associated with postoperative pulmonary morbidity after esophagectomy for cancer. Ann Surg Oncol. 2011;18:1460–8.
Hsu FM, Lee YC, Lee JM, Hsu CH, Lin CC, Tsai YC, et al. Association of clinical and dosimetric factors with postoperative pulmonary complications in esophageal cancer patients receiving intensity-modulated radiation therapy and concurrent chemotherapy followed by thoracic esophagectomy. Ann Surg Oncol. 2009;16:1669–77.
van Hagen P, Hulshof MC, van Lanschot JJ, Steyerberg EW, van Berge Henegouwen MI, Wijnhoven BP, et al. Preoperative chemoradiotherapy for esophageal or junctional cancer. N Engl J Med. 2012;366:2074–84.
Ando N, Kato H, Igaki H, Shinoda M, Ozawa S, Shimizu H, et al. A randomized trial comparing postoperative adjuvant chemotherapy with cisplatin and 5-fluorouracil versus preoperative chemotherapy for localized advanced squamous cell carcinoma of the thoracic esophagus (JCOG9907). Ann Surg Oncol. 2012;19:68–74.
Tachimori Y, Kanamori N, Uemura N, Hokamura N, Igaki H, Kato H. Salvage esophagectomy after high-dose chemoradiotherapy for esophageal squamous cell carcinoma. J Thorac Cardiovasc Surg. 2009;137:49–54.
Blank S, Stange A, Sisic L, Roth W, Grenacher L, Sterzing F, et al. Preoperative therapy of esophagogastric cancer: the problem of nonresponding patients. Langenbecks Arch Surg. 2013;398:211–20.
Noble F, Curtis N, Harris S, Kelly JJ, Bailey IS, Byrne JP, et al. Risk assessment using a novel score to predict anastomotic leak and major complications after oesophageal resection. J Gastrointest Surg. 2012;16:1083–95.
Yoshida N, Watanabe M, Baba Y, Iwagami S, Ishimoto T, Iwatsuki M, et al. Estimation of physiologic ability and surgical stress (E-PASS) can assess short-term outcome after esophagectomy for esophageal cancer. Esophagus. 2013;10:86–94.
Edge SB, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A. AJCC cancer staging manual. 7th ed. New York: Springer; 2009.
Society of Thoracic Surgeons. Risk-adjusted morbidity and mortality for esophagectomy for cancer. 2013. http://www.sts.org/quality-research-patient-safety/quality/quality-performance-measures. (Accessed 29 Dec 2013).
National Cancer Institute. Common Terminology Criteria for Adverse Events (CTCAE). United States Department of Health and Human Services. 2010. http://evs.nci.nih.gov/ftp1/CTCAE/CTCAE_4.03_2010-06-14_QuickReference_5x7.pdf#search=‘http%3A%2F%2Fevs.nci.nih.gov%2Fftp1%2FCTCAE%2F+CTCAE_4.03_20100614_QuickReference_5x7.pdf. (Accessed 29 Dec 2013).
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Findlay JM, Gillies RS, Millo J, Sgromo B, Marshall RE, Maynard ND. Enhanced recovery for esophagectomy: a systematic review and evidence-based guidelines. Ann Surg. 2014;259(3):413–31
Bakhos CT, Fabian T, Oyasiji TO, Gautam S, Gangadharan SP, Kent MS, et al. Impact of the surgical technique on pulmonary morbidity after esophagectomy. Ann Thorac Surg. 2012;93:221–6.
Schieman C, Wigle DA, Deschamps C, Nichols Iii FC, Cassivi SD, Shen KR, et al. Patterns of operative mortality following esophagectomy. Dis Esophagus. 2012;25:645–51.
Paul DJ, Jamieson GG, Watson DI, Devitt PG, Game PA. Perioperative risk analysis for acute respiratory distress syndrome after elective oesophagectomy. ANZ J Surg. 2011;81:700–6.
Rodgers M, Jobe BA, O’Rourke RW, Sheppard B, Diggs B, Hunter JG. Case volume as a predictor of inpatient mortality after esophagectomy. Arch Surg. 2007;142:829–39.
Grotenhuis BA, Wijnhoven BP, Grüne F, van Bommel J, Tilanus HW, van Lanschot JJ. Preoperative risk assessment and prevention of complications in patients with esophageal cancer. J Surg Oncol. 2010;101:270–8.
Sunpaweravong S, Ruangsin S, Laohawiriyakamol S, Mahattanobon S, Geater A. Prediction of major postoperative complications and survival for locally advanced esophageal carcinoma patients. Asian J Surg. 2012;35:104–9.
Schweigert M, Solymosi N, Dubecz A, Stadlhuber RJ, Ofner D, Stein HJ. Current outcome of esophagectomy in the very elderly: experience of a german high-volume center. Am Surg. 2013;79:754–63.
Morita M, Otsu H, Kawano H, Kumashiro R, Taketani K, Kimura Y, et al. Advances in esophageal surgery in elderly patients with thoracic esophageal cancer. Anticancer Res. 2013;33:1641–7.
Law S, Wong KH, Kwok KF, Chu KM, Wong J. Predictive factors for postoperative pulmonary complications and mortality after esophagectomy for cancer. Ann Surg. 2004;240:791–800.
Nakamura M, Iwahashi M, Nakamori M, Ishida K, Naka T, Iida T, et al. An analysis of the factors contributing to a reduction in the incidence of pulmonary complications following an esophagectomy for esophageal cancer. Langenbecks Arch Surg. 2008;393:127–33.
Hidaka H, Hotokezaka M, Nakashima S, Uchiyama S, Maehara N, Chijiiwa K. Sex difference in survival of patients treated by surgical resection for esophageal cancer. World J Surg. 2007;31:1982–7.
Morita M, Otsu H, Kawano H, Kasagi Y, Kimura Y, Saeki H, et al. Gender differences in prognosis after esophagectomy for esophageal cancer. Surg Today. 2014;44:505–12.
Koide N, Kitazawa M, Komatsu D, Suzuki A, Miyagawa S. Gender differences in clinicopathological features and outcomes of esophageal cancer patients treated surgically. Esophagus. 2011;8:107–12.
Bohanes P, Yang D, Chhibar RS, Labonte MJ, Winder T, Ning Y, et al. Influence of sex on the survival of patients with esophageal cancer. J Clin Oncol. 2012;30:2265–72.
Conflict of Interest
Naoya Yoshida and co-authors have no conflicts of interest to declare in association with this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yoshida, N., Baba, Y., Watanabe, M. et al. An original scoring system for predicting postoperative morbidity after esophagectomy for esophageal cancer. Surg Today 45, 346–354 (2015). https://doi.org/10.1007/s00595-014-0958-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-014-0958-5