Abstract
Purpose
The purpose of our meta-analyses is to find the most appropriate surgical technique treating lumbar degenerative disc disease (DDD). Spinal fusion is the conventional treatment for lumbar DDD. Total disc replacement (TDR) has been developed to avoid negative effects of fusions by preserving functionality. To our knowledge, there is no evaluation comparing meta-analytically the clinical results of three different surgical techniques with same inclusion and exclusion criteria for treating DDD.
Methods
The surgical techniques TDR, anterior lumbar interbody fusion (ALIF) and circumferential fusion (CFF) are pairwise meta-analytically compared. Primary outcomes are pain measured by the Visual Analogue Scale (VAS) and function measured by the Oswestry Disability Index (ODI). Secondary outcomes are the mean number of complications per case (MNOC) at surgery and follow-up and the overall MNOC.
Results
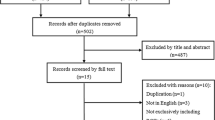
In our systematic search, we found finally six prospective studies with the minimum follow-up of two years: four randomized controlled trials and two cohort studies. In VAS and ODI, TDR is proved to be superior to ALIF and CCF (p < 0.05), whereat ALIF is more effective than CFF without statistical significance. CFF presents the best result in complications with the lowest overall MNOC (0.1), followed by TDR (1.2) and ALIF (1.5).
Conclusion
According to our meta-analyses, we regard TDR to be the most appropriate surgical technique treating DDD, followed by ALIF. Further studies with a longer follow-up are needed using the same methodical approach to strengthen the VAS and ODI results and to explain the discrepant result to complications.







Similar content being viewed by others
References
Ehrlich GE (2003) Low back pain. Bull World Health Organ 81:671–676
Bai D-Y, Liang L, Zhang B-B, Zhu T, Zhang H-J, Yuan Z-G, Chen Y-F (2019) Total disc replacement versus fusion for lumbar degenerative diseases—a meta-analysis of randomized controlled trials. Medicine 98:1–11
Formica M, Divano S, Cavagnaro L, Basso M, Zanirato A, Formica C, Felli L (2017) Lumbar total disc arthroplasty: outdated or here to stay procedure? A systematic review of current literature. J Orthop Traumatol 18:197–215
Sumpio BE (2008) Technique of Anterior Exposure of the Lumbar Spine. In: Yue JJ, Bertagnoli R, McAfee PC, An HS (eds) Motion Preservation Surgery of the Spine—advanced techniques and controversies. Saunders Elsevier Inc., Philadelphia, pp 141–147
Geisler H (2015) Charité Artificial Disc. In: Kim DH, Sengupta DK, Cammisa FP, Yoon DH, Fessler RG (eds) Dynamic Reconstruction of the Spine, 2nd edn. Thieme, New York, pp 313–333
Madan SS, Boeree NR (2003) Comparison of instrumented anterior interbody fusion with instrumented circumferential lumbar fusion. Eur Spine J 12:567–575
Sasso R, Foulk DM, Hahn M (2008) Prospective, randomized trial of metal-on-metal artificial lumbar disc replacement: initial results for treatment of discogenic pain. Spine 33:123–131
Rao MJ, Cao SS (2014) Artificial total disc replacement versus fusion for lumbar degenerative disc disease: a meta-analysis of randomized controlled trials. Arch Orthop Trauma Surg 134:149–158
Wei J, Song Y, Sun L, Lv C (2013) Comparison of artificial total disc replacement versus fusion for lumbar degenerative disc disease: a meta-analysis of randomized controlled trials. Int Orthop 37:1315–1325
Fairbank JCT, Pynsent PB (2000) The Oswestry disability index. Spine 25:2940–2953
Lang SAJ (2017) What is the best surgery for lumbar degenerative disc disease and chronic low back pain? A meta-analysis comparing circumferential fusion, anterior stand alone fusion and TDR in relation to pain, function and complications. https://spinefoundation.info/medaba/studyprotocols?u=7
Büttner-Janz K (2013) User advice of the Meta-analyses-DataBase of the Büttner-Janz Spinefoundation. https://spinefoundation.info/en/meta-analyses-database
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Berg S, Tullberg T, Branth B, Olerud C, Tropp H (2009) Total disc replacement compared to lumbar fusion: a randomized controlled trial with a 2-year follow up. Eur Spine J 18:1512–1519
Blumenthal S, McAfee PC, Guyer RD, Hochschuler SH, Geisler FH, Holt RT, Garcia R, Regan JJ, Ohnmeiss DD (2005) A prospective, randomized, multicenter Food and Drug Administration investigational device exemptions study of lumbar total disc replacement with the CHARITE artificial disc versus lumbar fusion: part I: evaluation of clinical outcomes. Spine 30:1565–1575
Geisler FH, Blumenthal SL, Guyer RD, McAfee PC, Regan JJ, Johnson JP, Mullin B (2004) Neurological complications of lumbar artificial disc replacement and comparison of clinical results with those related to lumbar arthrodesis in the literature: results of a multicenter, prospective, randomized investigational device exemption study of Charité intervertebral disc. invited submission from the joint section meeting on disorders of the spine and peripheral nerves, march 2004. J Neurosurg 1(2):143–154
Guyer RD, McAfee PC, Hochschuler SH, Blumenthal SL, Fedder IL, Ohnmeiss DD, Cunningham BW (2004) Prospective randomized study of the Charité artificial disc: data from two investigational centers. Spine J 4:S252–S259
Gornet MF, Burkus JK, Dryer RF, Peloza JH (2011) Lumbar disc arthroplasty with Maverick disc versus stand-alone Interbody fusion: a prospective, randomized, controlled, multicenter investigational device exemption trial. Spine 36:E1600–E1611
Delamarter R, Zigler JE, Balderston RA, Cammisa FP, Goldstein JA, Spivak JM (2011) Prospective, randomized, multicenter Food and Drug Administration investigational device exemption study of the ProDisc-L total disc replacement compared with circumferential arthrodesis for the treatment of two-level lumbar degenerative disc disease. J Bone Joint Surg Am 93:705–715
Zigler J, Delamarter R, Spivak JM et al (2007) Results of the prospective, randomized, multicenter Food and Drug Administration investigational device exemption study of the ProDisc-L total disc replacement versus circumferential fusion for the treatment of 1-level degenerative disc disease. Spine 32:1155–1162
Strube P, Hoff E, Hartwig T, Perka CF, Gross C, Putzier M (2012) Stand-alone anterior versus anteroposterior lumbar interbody single-level fusion after a mean follow-up of 41 months. J Spinal Disord Tech 25:362–369
Gornet MF, Burkus JK, Dryer RF, Peloza JH, Schranck FW, Copay AG (2019) Lumbar disc arthroplasty versus anterior lumbar interbody fusion: 5-year outcomes for patients in the Maverick disc investigational device exemption study. J Neurosurg Spine 17:1–10
Guyer RD, McAfee PC, Banco RJ et al (2009) Prospective, randomized, multicenter Food and Drug Administration investigational device exemption study of lumbar total disc replacement with the CHARITÉ artificial disc versus lumbar fusion: five-year follow-up. Spine J 9:374–386
Zigler JE, Delamarter RB (2012) Five-year results of the prospective, randomized, multicenter, Food and Drug Administration investigational device exemption study of the ProDisc-L total disc replacement versus circumferential arthrodesis for the treatment of single-level degenerative disc disease. J Neurosurg Spine 17:493–501
Ding F, Jia Z, Zhao Z, Xie L, Gao X, Ma D, Liu M (2017) Total disc replacement versus fusion for lumbar degenerative disc disease: a systematic review of overlapping meta-analyses. Eur Spine J 26:806–815
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lang, S.A.J., Bohn, T., Barleben, L. et al. Advanced meta-analyses comparing the three surgical techniques total disc replacement, anterior stand-alone fusion and circumferential fusion regarding pain, function and complications up to 3 years to treat lumbar degenerative disc disease. Eur Spine J 30, 3688–3701 (2021). https://doi.org/10.1007/s00586-021-06784-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-06784-6