Abstract
Purpose
Although thymic epithelial tumors (TETs) are rare, their spinal metastases are even rarer, and they have only been described in a few case reports. The aim of the present study is to discuss the possible treatments and outcomes of patients with spinal metastasis from TETs.
Methods
Included in this retrospective study were 15 patients with metastasis of TETs who received either radical or debulking surgery plus radiochemotherapy as adjuvant therapy in our center between 2007 and 2017. Possible prognostic factors for progression-free survival (PFS) and overall survival (OS) were analyzed by log-rank analysis.
Results
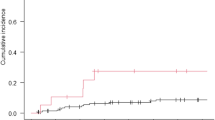
Our series comprised seven men and eight women, with a median age of 52 years. The period from the primary diagnosis to spinal metastasis varied from 0 to 16 months. The metastatic lesions were mainly located in the thoracic spine (n = 11; 73.3%), followed by the cervical and lumbar spine (n = 2; 13.3%, respectively). The median follow-up period was 28 months. Local tumor progression was detected in four patients (26.7%), and seven patients (46.7%) died of the disease during the follow-up period. Log-rank analysis indicated that radical resection was associated with longer PFS, whereas PFS, response to systemic chemotherapy and WHO B1–B2 were favorable factors of OS for patients with spinal metastatic TETs.
Conclusions
Radical surgery is associated with longer PFS, while PFS is associated with better OS. Postoperative radiotherapy seems to be a useful supplementary treatment after debulking surgery, and patients who respond to postoperative chemotherapy were demonstrated with greater OS. WHO type B3–C seemed to be an adverse factor for spinal metastasis from TETs.
Graphical abstract
These slides can be retrieved under Electronic Supplementary Material.




Similar content being viewed by others
References
Sadohara J, Fujimoto K, Müller NL et al (2006) Thymic epithelial tumors: comparison of CT and MR imaging findings of low-risk thymomas, high-risk thymomas, and thymic carcinomas. Eur J Radiol 60(1):70–79
Achey RL, Lee BS, Sundar S, Benzel EC, Krishnaney AA (2018) Rare thymoma metastases to the Spine: case reports and review of the literature. World Neurosurg 110:423–431
Suster S, Moran CA (2008) Histologic classification of thymoma: the World Health Organization and beyond. Hematol Oncol Clin North Am 22(3):381–392
Kondo K, Yoshizawa K, Tsuyuguchi M et al (2004) WHO histologic classification is a prognostic indicator in thymoma. Ann Thorac Surg 77(4):1183–1188
Vladislav T, Jain RK, Alvarez R et al (2012) Extrathoracic metastases of thymic origin: a review of 35 cases. Mod Pathol 25(3):370–377
Jee TK, Lee S-H, Kim HJ, Kim E-S, Eoh W (2014) Spinal metastasis of thymic carcinoma as a rare manifestation: a summary of 7 consecutive cases. Korean J Spine 11(3):157–161
Liu T, Qiu G, Tian Y (2011) Thymic carcinoma with primary spine metastasis. J Clin Neurosci 18(6):840–842
Hong B, Nakamura M, Hartmann C, Brandis A, Ganser A, Krauss JK (2013) Delayed distant spinal metastasis in thymomas. Spine (Phila Pa 1976) 38(26):E1709–E1713
Marotta N, Mancarella C, Colistra D, Landi A, Dugoni DE, Delfini R (2015) First description of cervical intradural thymoma metastasis. World J Clin Cases 3(11):946–950
Kim JY, Lee YS, Kang DH et al (2017) Epidural metastasis in malignant thymoma mimicking epidural abscess: case report and literature review. Korean J Spine 14(4):162–165
Low HM, Wong CF, H’ng MW (2016) Thymic carcinoma presenting with an unusual and delayed metastasis to the neural foramen, mimicking thoracic spinal radiculopathy. Med J Malays 71(6):368–369
Farin A, Aryan HE, Abshire BB (2005) Thymoma metastatic to the extradural spine. J Clin Neurosci 12(7):824–827
Shivapathasundram G, Sammons V, Bazina R (2016) Metastatic thymoma presenting as spontaneous epidural lumbar haematoma. Eur Spine J 25(Suppl 1):33–37
Frankel HL, Hancock DO, Hyslop G et al (1969) The value of postural reduction in the initial management of closed injuries of the spine with paraplegia and tetraplegia: I. Paraplegia 7(3):179–192
Oken MM, Creech RH, Tormey DC et al (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Boriani S, Weinstein JN, Biagini R (1997) Primary bone tumors of the spine: terminology and surgical staging. Spine (Phila Pa 1976) 22(9):1036–1044
Tomita K, Kawahara N, Kobayashi T, Yoshida A, Murakami H, Akamaru T (2001) Surgical strategy for spinal metastases. Spine (Phila Pa 1976) 26(3):298–306
Aoude A, Fortin M, Aldebeyan S, Ouellet J, Amiot LP, Weber MH, Jarzem P (2018) The revised Tokuhashi score; analysis of parameters and assessment of its accuracy in determining survival in patients afflicted with spinal metastasis. Eur Spine J 27(4):835–840
Versteeg AL, Verlaan JJ, Sahgal A et al (2016) The spinal instability neoplastic score: impact on oncologic decision-making. Spine Phila Pa (1976) 41(Suppl 20):S231–S237
Venuta F, Rendina EA, Longo F et al (2003) Long-term outcome after multimodality treatment for stage III thymic tumors. Ann Thorac Surg 76(6):1866–1872
Mou H, Liao Q, Hou X, Chen T, Zhu Y (2018) Clinical characteristics, risk factors, and outcomes after adjuvant radiotherapy for patients with thymoma in the United States: analysis of the surveillance, epidemiology, and end results (SEER) registry (1988–2013). Int J Radiat Biol 94(5):495–502
Lim Yu Jin, Song Changhoon, Kim Jae-Sung (2017) Improved survival with postoperative radiotherapy in thymic carcinoma: a propensity-matched analysis of surveillance, epidemiology, and end results (SEER) database. Lung Cancer 108(2017):161–167
Shin DY, Kim DW, Keam B et al (2014) The presence of extrathoracic metastasis is more prognostic of survival than Masaoka stage (IVa/IVb) in metastatic thymic epithelial tumor.—A retrospective cohort study. Lung Cancer 85(2):320–325
Jia Qi, Yin Huabin, Yang Jian et al (2018) Treatment and outcome of metastatic paraganglioma of the spine. Eur Spine J 2018(27):859–867
Kondo Kazuya, Monden Yasumasa (2003) Therapy for thymic epithelial tumors: a clinical study of 1,320 patients from Japan. Ann Thorac Surg 2003(76):878–885
Cassidy JT, Baker JF, Lenehan B (2018) The role of prognostic scoring systems in assessing surgical candidacy for patients with vertebral metastasis: a narrative review. Glob Spine J 8(6):638–651
Valente M, Schinzari G, Ricciotti A, Barone C (2007) Role of chemotherapy in malignant thymoma. Ann Ital Chir 2007(78):377–380
Loehrer PJ Sr, Jiroutek M, Aisner S et al (2001) Combined etoposide, ifosfamide, and cisplatin in the treatment of patients with advanced thymoma and thymic carcinoma: an intergroup trial. Cancer 2001(91):2010–2015
Giaccone G, Wilmink H, Paul MA, van der Valk P (2006) Systemic treatment of malignant thymoma A decade experience at a single institution. Am J Clin Oncol 29(4):336–344
Funding
This work was supported by grants from National Key Research and Development Program of China (2016YFC0902100).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The author(s) declare that they have no conflicts of interest.
Ethical standards
This research was approved by the hospital ethics committee of the hospital, and written informed consent was obtained from patients or their legal guardians.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jia, Q., Yang, J., Hu, J. et al. Treatments and outcomes of spinal metastasis from thymic epithelial tumors: 10-year experience with 15 patients in a single center. Eur Spine J 28, 1520–1528 (2019). https://doi.org/10.1007/s00586-019-05982-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-05982-7