Abstract
Background
Immune checkpoint inhibitors (ICIs) have revolutionised cancer treatment, but their use near the end of life in patients with advanced cancer is poorly documented. This study investigated the association between administration of ICI therapy in the last month of life and the duration of involvement of the palliative care (PC) team, among patients with advanced cancer who died in-hospital.
Methods
In a retrospective, multicentre study, we included all patients who died in 2018 of melanoma, head and neck carcinoma, non-small cell lung cancer or urothelial or renal cancer, in 2 teaching hospitals and one community hospital in France. The primary outcome was the association between ICI therapy in the last month of life and duration of involvement of the PC team in patient management.
Results
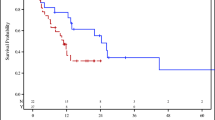
Among 350 patients included, 133 (38%) received anti-cancer treatment in the last month of life, including 71/133 (53%) who received ICIs. A total of 207 patients (59%) received palliative care, only 127 (36%) 30 days before death. There was a significant association between ongoing ICI therapy in the last month of life and shorter duration of PC management (p = 0.04). Receiving ICI therapy in the last month of life was associated with an increased risk of late PC initiation by multivariate regression analysis (hazard ratio 1.668; 95% CI 1.022–2.722).
Conclusion
ICI therapy is frequently used close to the end of life in patients with advanced cancer. Innovative new anti-cancer treatments should not delay PC referral. Improved collaboration between PC and oncological teams is needed to address this issue.


Similar content being viewed by others
Availability of data and materials
Our data are only available on request due to legal restrictions. Indeed, the data are the property of the University Hospital of Grenoble, France. To access our data, a written request must be addressed to our administration at the following email address: accueilrecherche@chu-grenoble.fr.
Code availability
Not applicable.
References
Vaddepally RK, Kharel P, Pandey R, Garje R, Chandra AB (2020) Review of indications of FDA-approved immune checkpoint inhibitors per NCCN guidelines with the level of evidence. Cancers (Basel) 12 https://doi.org/10.3390/cancers12030738.
Davis MP, Panikkar R (2018) Checkpoint inhibitors, palliative care, or hospice. Curr Oncol Rep 20:2. https://doi.org/10.1007/s11912-018-0659-0
Magee DE, Hird AE, Klaassen Z, Sridhar SS, Nam RK, Wallis CJD, Kulkarni GS (2020) Adverse event profile for immunotherapy agents compared with chemotherapy in solid organ tumors: a systematic review and meta-analysis of randomized clinical trials. Ann Oncol 31:50–60. https://doi.org/10.1016/j.annonc.2019.10.008
Temel JS, Greer JA, Muzikansky A, Gallagher ER, Admane S, Jackson VA, Dahlin CM, Blinderman CD, Jacobsen J, Pirl WF et al (2010) Early palliative care for patients with metastatic non-small-cell lung cancer. N Engl J Med 363:733–742. https://doi.org/10.1056/NEJMoa1000678
Vanbutsele G, Pardon K, Van Belle S, Surmont V, De Laat M, Colman R, Eecloo K, Cocquyt V, Geboes K, Deliens L (2018) Effect of early and systematic integration of palliative care in patients with advanced cancer: a randomised controlled trial. Lancet Oncol 19:394–404. https://doi.org/10.1016/S1470-2045(18)30060-3
Zimmermann C, Swami N, Krzyzanowska M, Hannon B, Leighl N, Oza A, Moore M, Rydall A, Rodin G, Tannock I et al (2014) Early palliative care for patients with advanced cancer: a cluster-randomised controlled trial. Lancet 383:1721–1730. https://doi.org/10.1016/S0140-6736(13)62416-2
Kaasa S, Loge JH (2018) Early integration of palliative care-new evidence and old questions. Lancet Oncol 19:280–281. https://doi.org/10.1016/S1470-2045(18)30061-5
Ferrell BR, Temel JS, Temin S, Alesi ER, Balboni TA, Basch EM, Firn JI, Paice JA, Peppercorn JM, Phillips T et al (2017) Integration of palliative care into standard oncology care: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol 35:96–112. https://doi.org/10.1200/JCO.2016.70.1474
Gidwani R, Joyce N, Kinosian B, Faricy-Anderson K, Levy C, Miller SC, Ersek M, Wagner T, Mor V (2016) Gap between recommendations and practice of palliative care and hospice in cancer patients. J Palliat Med 19:957–963. https://doi.org/10.1089/jpm.2015.0514
Colombet I, Montheil V, Durand JP, Gillaizeau F, Niarra R, Jaeger C, Alexandre J, Goldwasser F, Vinant P (2012) Effect of integrated palliative care on the quality of end-of-life care: retrospective analysis of 521 cancer patients. BMJ Support Palliat Care 2:239–247. https://doi.org/10.1136/bmjspcare-2011-000157
Vinant P, Joffin I, Serresse L, Grabar S, Jaulmes H, Daoud M, Abitbol G, Fouassier P, Triol I, Rostaing S et al (2017) Integration and activity of hospital-based palliative care consultation teams: the INSIGHT multicentric cohort study. BMC Palliat Care 16:36. https://doi.org/10.1186/s12904-017-0209-9
Barth C, Colombet I, Montheil V, Huillard O, Boudou-Rouquette P, Tlemsani C, Alexandre J, Goldwasser F, Vinant P (2020) First referral to an integrated onco-palliative care program: a retrospective analysis of its timing. BMC Palliat Care 19:31. https://doi.org/10.1186/s12904-020-0539-x
Gaertner J, Wolf J, Hallek M, Glossmann JP, Voltz R (2011) Standardizing integration of palliative care into comprehensive cancer therapy–a disease specific approach. Support Care Cancer 19:1037–1043. https://doi.org/10.1007/s00520-011-1131-y
Beernaert K, Deliens L, Pardon K, Van den Block L, Devroey D, Chambaere K, Cohen J (2015) What are physicians’ reasons for not referring people with life-limiting illnesses to specialist palliative care services? A nationwide survey. PLoS One 10:e0137251. https://doi.org/10.1371/journal.pone.0137251
Greer JA, Pirl WF, Jackson VA, Muzikansky A, Lennes IT, Heist RS, Gallagher ER, Temel JS (2012) Effect of early palliative care on chemotherapy use and end-of-life care in patients with metastatic non-small-cell lung cancer. J Clin Oncol 30:394–400. https://doi.org/10.1200/JCO.2011.35.7996
Wentlandt K, Krzyzanowska MK, Swami N, Rodin GM, Le LW, Zimmermann C (2012) Referral practices of oncologists to specialized palliative care. J Clin Oncol 30:4380–4386. https://doi.org/10.1200/JCO.2012.44.0248
Wu CC, Hsu TW, Chang CM, Lee CH, Huang CY, Lee CC (2016) Palliative chemotherapy affects aggressiveness of end-of-life care. Oncologist 21:771–777. https://doi.org/10.1634/theoncologist.2015-0445
Schulkes KJG, van Walree IC, van Elden LJR, van den Bos F, van Huis-Tanja L, Lammers JJ, Ten BokkelHuinink D, Hamaker ME (2018) Chemotherapy and healthcare utilisation near the end of life in patients with cancer. Eur J Cancer Care (Engl) 27:e12796. https://doi.org/10.1111/ecc.12796
Skov Benthien K, Adsersen M, Petersen MA, Soelberg Vadstrup E, Sjogren P, Groenvold M (2018) Is specialized palliative cancer care associated with use of antineoplastic treatment at the end of life? A population-based cohort study. Palliat Med 32:1509–1517. https://doi.org/10.1177/0269216318786393
Zdenkowski N, Cavenagh J, Ku YC, Bisquera A, Bonaventura A (2013) Administration of chemotherapy with palliative intent in the last 30 days of life: the balance between palliation and chemotherapy. Intern Med J 43:1191–1198. https://doi.org/10.1111/imj.12245
Colombet I, Bouleuc C, Piolot A, Vilfaillot A, Jaulmes H, Voisin-Saltiel S, Goldwasser F, Vinant P, group, E.s (2019) Multicentre analysis of intensity of care at the end-of-life in patients with advanced cancer, combining health administrative data with hospital records: variations in practice call for routine quality evaluation. BMC Palliat Care 18:35. https://doi.org/10.1186/s12904-019-0419-4
Monier PA, Chrusciel J, Ecarnot F, Bruera E, Sanchez S, Barbaret C (2020) Duration of palliative care involvement and cancer care aggressiveness near the end of life. BMJ Support Palliat Care. https://doi.org/10.1136/bmjspcare-2020-002641
Mullins MA, Ruterbusch JJ, Clarke P, Uppal S, Cote ML, Wallner LP (2021) Continuity of care and receipt of aggressive end of life care among women dying of ovarian cancer. Gynecol Oncol 162:148–153. https://doi.org/10.1016/j.ygyno.2021.04.024
Urvay S, Civelek B, Ozaslan E, Surel AA (2021) Chemotherapy at the End of Life. J Palliat Care 36:73–77. https://doi.org/10.1177/0825859720946505
Melac AT, Lesuffleur T, Bousquet PJ, Fagot-Campagna A, Gastaldi-Menager C, Tuppin P (2020) Cancer and end of life: the management provided during the year and the month preceding death in 2015 and causes of death in France. Support Care Cancer 28:3877–3887. https://doi.org/10.1007/s00520-019-05188-z
Haukland EC, von Plessen C, Nieder C, Vonen B (2020) Adverse events in deceased hospitalised cancer patients as a measure of quality and safety in end-of-life cancer care. BMC Palliat Care 19:76. https://doi.org/10.1186/s12904-020-00579-0
Riaz F, Gan G, Li F, Davidoff AJ, Adelson KB, Presley CJ, Adamson BJ, Shaw P, Parikh RB, Mamtani R et al (2020) Adoption of immune checkpoint inhibitors and patterns of care at the end of life. JCO Oncol Pract 16:e1355–e1370. https://doi.org/10.1200/OP.20.00010
Temel JS, Shaw AT, Greer JA (2016) Challenge of prognostic uncertainty in the modern era of cancer therapeutics. J Clin Oncol 34:3605–3608. https://doi.org/10.1200/JCO.2016.67.8573
Beaussant Y, Mathieu-Nicot F, Pazart L, Tournigand C, Daneault S, Cretin E, Godard-Marceau A, Chassagne A, Trimaille H, Bouleuc C et al (2015) Is shared decision-making vanishing at the end-of-life? A descriptive and qualitative study of advanced cancer patients’ involvement in specific therapies decision-making. BMC Palliat Care 14:61. https://doi.org/10.1186/s12904-015-0057-4
Brom L, Onwuteaka-Philipsen BD, Widdershoven GA, Pasman HR (2016) Mechanisms that contribute to the tendency to continue chemotherapy in patients with advanced cancer. Qualitative observations in the clinical setting. Support Care Cancer 24:1317–1325. https://doi.org/10.1007/s00520-015-2910-7
Rietjens JAC, Sudore RL, Connolly M, van Delden JJ, Drickamer MA, Droger M, van der Heide A, Heyland DK, Houttekier D, Janssen DJA et al (2017) Definition and recommendations for advance care planning: an international consensus supported by the European Association for Palliative Care. Lancet Oncol 18:e543–e551. https://doi.org/10.1016/S1470-2045(17)30582-X
Glisch C, Hagiwara Y, Gilbertson-White S, Gao Y, Lyckholm L (2020) Immune checkpoint inhibitor use near the end of life is associated with poor performance status, lower hospice enrollment, and dying in the hospital. Am J Hosp Palliat Care 37:179–184. https://doi.org/10.1177/1049909119862785
Petrillo LA, El-Jawahri A, Nipp RD, Lichtenstein MRL, Durbin SM, Reynolds KL, Greer JA, Temel JS, Gainor JF (2020) Performance status and end-of-life care among adults with non-small cell lung cancer receiving immune checkpoint inhibitors. Cancer 126:2288–2295. https://doi.org/10.1002/cncr.32782
Murakami N, Tanabe K, Morita T, Kadoya S, Shimada M, Ishiguro K, Endo N, Sawada K, Fujikawa Y, Takashima R et al (2015) Going back to home to die: does it make a difference to patient survival? BMC Palliat Care 14:7. https://doi.org/10.1186/s12904-015-0003-5
Hamano J, Yamaguchi T, Maeda I, Suga A, Hisanaga T, Ishihara T, Iwashita T, Kaneishi K, Kawagoe S, Kuriyama T et al (2016) Multicenter cohort study on the survival time of cancer patients dying at home or in a hospital: does place matter? Cancer 122:1453–1460. https://doi.org/10.1002/cncr.29844
Bourgeois H, Grude F, Solal-Celigny P, Dupuis O, Voog E, Ganem G, Denis F, Zinger M, Juhel-Voog L, Lafond C et al (2017) Clinical validation of a prognostic tool in a population of outpatients treated for incurable cancer undergoing anticancer therapy: PRONOPALL study. Ann Oncol 28:1612–1617. https://doi.org/10.1093/annonc/mdx172
LeBlanc TW, Temel JS, Helft PR (2018) “How much time do I have?”: communicating prognosis in the era of exceptional responders. Am Soc Clin Oncol Educ Book 38:787–794. https://doi.org/10.1200/EDBK_201211
Simmons CPL, McMillan DC, McWilliams K, Sande TA, Fearon KC, Tuck S, Fallon MT, Laird BJ (2017) Prognostic tools in patients with advanced cancer: a systematic review. J Pain Symptom Manage 53:962.e910-970.e910. https://doi.org/10.1016/j.jpainsymman.2016.12.330
Author information
Authors and Affiliations
Contributions
Study concept: JA, CB.
Study design: JA, CB, SS, IC, MF.
Data acquisition: JA, CB, BB, SS, LH.
Data analysis and interpretation: SS, JC, JA, CB, EB.
Statistical analysis: SS, JC.
Manuscript preparation: JA, CB, FE, SS, IC, RHD, GE, EB, MF.
Providing language help: FE, EB.
Corresponding author
Ethics declarations
Ethics approval
Since the study was wholly observational and used only anonymized data (patient names were not recorded), neither ethics approval nor a specific written informed consent from participants was required under French law as a retrospective database study.
Consent to participate
See the “Ethics approval” section.
Consent for publication
See the “Ethics approval” section.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Auclair, J., Sanchez, S., Chrusciel, J. et al. Duration of palliative care involvement and immunotherapy treatment near the end of life among patients with cancer who died in-hospital. Support Care Cancer 30, 4997–5006 (2022). https://doi.org/10.1007/s00520-022-06901-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-022-06901-1