Abstract
Goals
The objective of this study was to determine utility of prophylactic anti-coagulation in cancer patients hospitalised for palliative care in a specialised centre.
Materials and methods
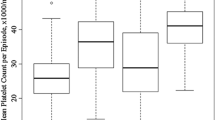
Prospective 1:1 open randomised study was designed. Twenty patients aged 55 to 88 years with advanced cancer and an estimated life expectancy of less than 6 months were assigned to either receive treatment with 2,850/3,800 U (<70/>70 kg) of daily subcutaneous nadroparin or no treatment. Suspicion of venous thrombo-embolism (deep vein thrombosis and pulmonary embolism) was confirmed by echo-Doppler examination of the lower limbs and/or by spiral computed tomography scan of the lungs. Bleeding episodes were recorded. Platelet count was measured on days 7 and 14. Survival time from study entry was determined.
Main results
One venous thrombo-embolism and one major bleeding occurred in the group receiving nadroparin, whereas two minor bleedings occurred in the control group. At 3 months, nine of ten participants had died in the control group vs five of ten in the group receiving nadroparin (P = 0.141). Five participants could be discharged home (P = 0.141).
Conclusions
Decision to administer prophylactic nadroparin in hospitalised cancer patients under palliative care remains a challenge. Better mobility score at admission and the likelihood to be discharged home may be useful for practical purposes. The observation of a potential influence of prophylactic nadroparin on survival deserves further studies.



Similar content being viewed by others
References
Agrawal M, Danis M (2002) End-of-life care for terminally ill participants in clinical research. J Palliat Med 5:729–737
Baron JA, Gridley G, Weiderpass E, Nyren O, Linet M (1998) Venous thromboembolism and cancer. Lancet 351:1077–1080
Bruera E, Neumann CM (1998) Management of specific symptom complexes in patients receiving palliative care. Can Med Assoc J 158:1717–1726
Bruera E, Miller L, McCallion J, Macmillan J et al (1992) Cognitive failure in patients with terminal cancer: a prospective study. J Pain Symptom Manage 7:192–195
Casarett DJ, Karlawish JHT (2000) Are special ethical guidelines needed for palliative care research? J Pain Symptom Manage 20:130–139
Deitcher SR, Gomes MP (2004) The risk of venous thromboembolic disease associated with adjuvant hormone therapy for breast carcinoma: a systematic review. Cancer 101:439–449
Federal Office of Statistics (Switzerland). http://www.bfs.admin.ch/
Folstein MF, Folstein SE, Mc Hugh PR (1975) Mini-Mental state. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Goodnough LT, Saito H, Manni A, Jones PK, Pearson OH (1984) Increased incidence of thromboembolism in stage IV breast cancer patients treated with a five-drug chemotherapy regimen. A study of 159 patients. Cancer 54:1264–1268
Gouin-Thibaut I, Samama MM (2000) Venous thrombosis and cancer. Ann Biol Clin (Paris) 58:675–682
Hawryluck L (2004) People at the end of life are a vulnerable research population. Clin Oncol 16:225–226
Jacobs LG (2003) Prophylactic anticoagulation for venous thromboembolic disease in geriatric patients. J Am Geriatr Soc 51:1472–1478
Jilma B, Kamath S, Lip GYH (2003) Antithrombotic therapy in special circumstances. II-in children, thrombophilia, and miscellanaous conditions. Br Med J 326:93–96
Johnson MJ, Sherry K (1997) How do palliative physicians manage venous thromboembolism? Palliat Med 11:462–468
Kakkar AK, Levine MN, Kadziola Z et al (2004) Low molecular weight heparin, therapy with dalteparin, and survival in advanced cancer: The Fragmin Advanced malignancy Outcome Study (FAMOUS). J Clin Oncol 22:1944–1948
Keith RA, Granger CV, Hamilton BB, Sherwin FS (1987) The functional independence measure: a new tool for rehabilitation. Adv Clin Rehabil 1:6–18
Klerk CPW, Smorenburg SM, Otten HM et al (2005) The effect of low molecular weight heparin on survival in patients with advanced malignancy. J Clin Oncol 23:2130–2135
Koedoot CG, de Haan RJ, Stiggelbout AM et al (2003) Palliative chemotherapy or best supportive care? A prospective study explaining patients’ preference and choice. Br J Cancer 89:2219–2226
Lee AYY (2003) Epidemiology and management of venous thromboembolism in patients with cancer. Thromb Res 110:167–172
Leizorovicz A, Cohen AT, Turpie AGG et al (2004) Randomized, placebo-controlled trial of dalteparin for the prevention of venous thromboembolism in acutely ill medical patients. Circulation 110:874–879
Mazzocato C, Sweeney C, Bruera E (2001) Clinical research in palliative care: choice of trial design. Palliat Med 15:261–264
Merminod T, Zulian GB (2007) Venous thromboembolism in cancer patients under palliative care: retrospective study with lessons to the future. Supportive Palliative Cancer Care J (in press)
Pautex S, Moynier K, Weber C, Zulian GB (2002) L’évaluation des symptômes en oncologie palliative. Méd Hyg 60:1313–1317
Samama MM, Cohen AT, Darmon JY et al (1999) A comparaison of enoxaparin with placebo for the prevention of venous thromboembolism in acutely ill medical patients. New Eng J Med 341:793–800
Saphner T, Tormey DC, Gray R (1991) Venous and arterial thrombosis in patients who received adjuvant therapy for breast cancer. J Clin Oncol 9:286–294
Trousseau A (1865) Phlegmasia Alba Dolens. Clinique médicale de l’Hôtel Dieu de Paris, vol 3. The New Sydenham Society, London, p 94
Wilson CB, Lambert HE, Scott RD (1987) Subclavian and axillary vein thrombosis following radiotherapy for carcinoma of the breast. Clin Radiol 38:95–96
World Heath Organization. http://www.who.int/cancer/palliative/definition/en/
Yancik R (2005) Population aging and cancer: a cross-national concern. Cancer 11:437–441
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Weber, C., Merminod, T., Herrmann, F.R. et al. Prophylactic anti-coagulation in cancer palliative care: a prospective randomised study. Support Care Cancer 16, 847–852 (2008). https://doi.org/10.1007/s00520-007-0339-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-007-0339-3