Abstract
The central question of nephron-sparing surgery in unilateral non-syndromic Wilms tumour sits at a crossroads between surgery, oncology, and nephrology. There has been a significant paradigm shift in paediatric oncology towards reducing toxicity and addressing long-term treatment-related sequalae amongst childhood cancer survivors. After paediatric nephrectomy and 30–50 years of follow-up, 40% of patients will have chronic kidney disease, including 22% with hypertension and 23% with albuminuria. It is difficult to predict which patients will progress to develop hypertension, reduced glomerular filtration rate, albuminuria, and a higher cardiovascular risk. For these reasons, nephron-sparing surgery when it is technically feasible must be considered. To decrease the incidence of positive surgical margins (viable tumour present at a resection margin), incomplete lymph node sampling, and complications, these procedures should be performed at specialist and experienced reference centres. Based on the impacts of individual treatment pathways, survivors of childhood WT need to be followed through adulthood for early detection of chronic kidney disease, hypertension, and prevention of cardiovascular events.
Similar content being viewed by others
Introduction
Survivors of childhood cancer remain at risk of reduced life expectancy and morbidity due to treatment-related effects [1]. In 2016, The Renal Tumour Study Group of the International Society of Paediatric Oncology developed a protocol that established new pathways in diagnosis and treatment of children with renal tumours, to continue the iterative process of collaboration and research. This was termed the UMBRELLA protocol and one of its goals was to decrease acute toxicity and long-term treatment-related sequelae [2]. The chosen surgical strategy plays an important role in preserving functional kidney and reducing morbidity through the selective utilization of nephron-sparing surgery (NSS) [3]. To preserve kidney function, NSS was established in children with bilateral Wilms tumours (WT), or unilateral WT with a syndrome predisposing to metachronous Wilms tumours. However, in the recent UMBRELLA protocol, NSS has become an acceptable treatment option in non-syndromic unilateral WT when certain criteria are met [2]. Adoption of NSS has been slow [3] due to concern around surgical complications, and positive surgical margins necessitating additional therapy [4].
The principles that have established the application of NSS in children include a physiological rationale for its use, consistent case selection, maintenance of the oncological principles of surgery, and surgery that is performed in a high-volume centre by an experienced team. These themes will subsequently be discussed in detail. The goal of this review was to determine a rationale for the adoption of NSS in a wider context and to specify the conditions, extended indications, technical considerations, and expected outcomes.
Rationale for a broader application of nephron-sparing surgery
The goal of NSS is to safely preserve as much functioning and draining renal parenchyma as possible while maintaining an excellent oncological outcome. To determine the rationale for this, the consequences of total nephrectomy (TN) on kidney function, and the associated cardiovascular morbidity, must be established. The evolution of kidney function with age and the consequences of TN in children or adults can be illustrated by studying various situations. The definition of kidney injury and classification of chronic kidney disease are based on the glomerular filtration rate (GFR) and albuminuria, as standardized by the KDIGO CKD work group [5, 6]. Furthermore, when eGFR is reported, it should be accompanied by the endogenous filtration marker, assay method, and estimating equation. In this consensus statement, criteria and severity for albuminuria and proteinuria are also precisely defined.
The physiology of kidney function and the aging kidney
GFR is low at birth and reaches adult levels at the end of the second year of life [7]. It is stable at around 120 ml/min/1.73 m2 until the fourth decade, after which time it slowly declines by 8 ml/min/1.73 m2 per decade [8]. This decline relates to reduced renal mass, glomerular sclerosis, and reduced glomerular capillary flow. There is wide anatomical variation in the total glomerular number, between as little as 200,0000 and nearly 2 million [9, 10]. The number of nephrons present at birth relates to the fetal milieu and genetic factors. Of the many aspects involved, birth weight has been the most widely studied and there is a linear relationship between nephrons at birth and birth weight (260,000 nephrons per kg) [11]. However, it is noted that there is a huge variation around the line of association. Interestingly, the importance of birth weight holds for pre-term infants with appropriate weight for age, or term infants who are small for gestational age [12].
The decline of GFR with age is often undetected because of concomitant decrease in muscular mass [13], notwithstanding that creatinine is not a pure marker of glomerular filtration (it is secreted and reabsorbed by kidney tubules) [14]. Cystatin C is produced by all nucleated cells, is freely filtered by glomeruli and not reabsorbed, and the filtration rate appears unaffected by severe illness [15]. Ultimately, when an accurate GFR assessment is needed a measured GFR should be used [16, 17].
Reduction of GFR with age is of growing importance as life expectancy in developed countries has increased significantly, and kidney failure carries a significant health burden. The diminishing function of the aging kidney is also affected by common co-morbidities (hypertension, nephrotoxic medications, diabetes, and metabolic syndrome). For these reasons, the mean eGFR in the general population over 70 years of age is less than 60 ml/min/1.73 m2 [13]. A reduction of GFR (< 45 ml/min/1.73 m2) in adults over 60 years of age doubles all-cause mortality and also has a significant impact on cardiovascular mortality [18]. This notion of the aging kidney is critical when we interpret the consequences of TN in paediatric patients. It underscores that even 20–30 years of follow-up is insufficient to determine the consequences of total nephrectomy.
Single kidney (congenital or acquired) in children
In 1981, Brenner postulated that hyperfiltration in remnant nephrons following renal ablation contributes to progressive kidney dysfunction after studying rats [19]. Decreased functional kidney reserve leads to increased intraglomerular pressure and hyperfiltration. These physiological alterations may exacerbate any co-existent predisposition to glomerular pathology, whether genetic or acquired. Judicious and pro-active management of risk factors in patients with acquired single kidney (ASK) may slow the progression to chronic kidney disease [14].
Congenital and acquired causes of single kidney have distinct consequences. Nephrogenesis continues up to 36 weeks’ gestation and this allows an opportunity for physiological compensation in situations where there is a congenital single functioning kidney [20]. This phenomenon could explain why cases of congenital single kidney (CSK) may have a superior functional profile, although this has been variably found in comparative studies (Table 1). However, children with both CSK and ASK do show compensatory hypertrophy regardless of aetiology [21], and it may be this adaptive (or maladaptive) response to reduced kidney reserve is more age and stage dependent rather than related to aetiology per se. Furthermore, a higher GFR within the first decade in children with a single kidney needs to be interpreted with caution, as this may represent a higher degree of hyperfiltration and herald a worst prognosis, rather than reflect better kidney function.
A review of adults following childhood TN (for oncological and non-oncological indications) revealed that after > 30 years follow-up: 40% had kidney dysfunction (eGFR < 90 ml/min/1.73 m2), 22% had hypertension, and 23% had albuminuria. After 50 years of follow-up 88% of patients had an eGFR between 46 and 86 ml/min/1.73 m2 [27]. These results must be put in the context of a heterogenous group, with 30 years of follow-up and historical regimens of both adjuvant chemotherapy and radiotherapy. Nonetheless, nephrectomy performed for non-oncological indications had similarly poor outcomes (kidney dysfunction 38%, hypertension 26%, albuminuria 33%) after >30 years of follow-up. Care pathways and recommended follow-up have been developed for this population in response to the risks outlined [20, 22, 27, 28].
Living kidney donors
Although the effects of nephrectomy in childhood and adulthood are quite distinct from an experimental perspective [29], living kidney donors represent a valuable model to understand the evolution of kidney function after TN, being generally healthy and well-studied adults. However, it must be noted that living kidney donors have a higher incidence of developing metabolic syndrome than matched controls [30]. This may partially explain their long-term cardiovascular morbidity, but GFR has been identified as an independent cardiovascular risk factor in this group [31]. Another major limitation of extrapolating outcomes from this group, over and above the differences between donor nephrectomy and ASK in childhood, are the requirement for at least 10 years of follow-up to allow some meaningful application.
A study of nearly 4000 living donors with a mean follow-up of 17 years illustrated some of the expected dysfunction in ASK. Proteinuria was detected in 6%, eGFR < 60 ml/min/1.73 m2 in 36%, and 2.5% had an eGFR < 30 ml/min1.73 m2 or kidney failure (KF). The cumulative incidence of kidney failure was 1.3 per 1000 donors at 15 years, 7.7 per 1000 donors at 30 years, and 8.8 per 1000 donors at 40 years [32]. These figures must be interpreted with some care. The risk of kidney failure is elevated in related donors, which may be due to ill-defined genetic factors, or more comprehensive and long-term study of related donors (unrelated donation was rare before the 1980s) [32, 33].
Another North American study of over 70,000 kidney donors reported the cumulative incidence of kidney failure at 15-years post-donation. This ranged from 1.1 per 1000 donors to 3.3 per 1000 donors. This was related to eGFR six months post-donation, but importantly the pre-donation eGFR was not predictive of post-donation kidney function [34].
Specific factors affecting kidney function in cases of Wilms tumour
Treatment effects from chemotherapy and radiotherapy on kidney function are an important additional consideration in this population. A cohort of children (n = 75) treated for non-syndromic WT with TN alone (not requiring nephrotoxic chemotherapy or radiotherapy) have illuminated this point. With a mean follow-up of 20 years, 21% had an eGFR of < 90 ml/min/1.73 m2; and no patient had an eGFR of < 60 ml/min/1.73 m2. The authors concluded in this specific population the risk of developing significant long-term kidney dysfunction was low [35]. However, the consequences of mild kidney impairment in later adulthood remain unclear.
A smaller (n = 37) but prospective German study had a longer mean follow-up of 25 years. Of note, in this population of children treated for WT, 60% received radiotherapy (predominantly flank/abdominal), and 14% nephrotoxic chemotherapy (cyclophosphamide and/or carboplatin). They found 27% of patients had an eGFR between 60 and 90 ml/min/1.73 m2, and 3% had an GFR < 60 ml/min/1.73 m2. Hypertension was present in 41% of patients. The results when compared with previous studies (in terms of kidney function and hypertension) are likely explained by the extended follow-up and impact of adjuvant treatment [36].
A Dutch study recently reported the outcomes of 31 WT survivors with 15 years of follow-up. The rates of hypertension were 26% and 4% of patients had an eGFR < 60 ml/min/1.73 m2 [37]. And even more recently a French childhood survivor cancer study reported outcomes of 5498 survivors and 42,118 person-years of follow-up. They reported that children who underwent nephrectomy and required ifosfamide (> 60 g/m2) had an extremely high risk of hospitalisation for renal causes [38]. From these studies, there is a proportion of patients treated for WT following TN who will have chronic kidney disease and/or hypertension. However, the relative renal impact of surgery, radiotherapy, and nephrotoxic chemotherapy needs to be more clearly delineated [16]. Furthermore, until WT1 genetic screening is uniformly applied, it is difficult to identify if there is a sub-group of children with poor outcomes who are incorrectly classified as non-syndromic [39].
A large prospective childhood cancer survivor study reported kidney outcomes in children with unilateral non-syndromic WT stratified by treatments received (n = 2008) [40]. Compared to their siblings, WT survivors experienced a ten-fold increased in the rate of kidney failure (2.4% 35-year cumulative incidence) [40]. The addition of abdominal radiotherapy doubled the relative risk of kidney failure to 20-fold [40]. Although this was a North American study, there was no survivor group that underwent nephrectomy alone. Once long-term follow-up for this group becomes available for comparison, it will further clarify the consequences of adjuvant treatments on long-term outcomes.
In the UMBRELLA protocol, post-operative local or flank radiotherapy is indicated in children with unilateral WT with:
-
1.
Intermediate-risk histology and stage III disease (lymph node positivity, R1 or R2 resection, e.g. microscopic or macroscopic residual disease, or tumour rupture)
-
2.
High-risk histology stage II disease (except blastemal subtypes)
-
3.
High-risk histology stage III disease (all histological subtypes)
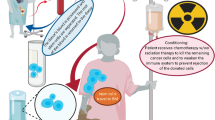
It must be emphasised that many aspects of this decision can only be confirmed post-operatively following histological review (e.g. histological risk group, lymph node positivity, tumour at resection margins). Dosing depends on many individual and disease factors, but the protocol stipulates that the dose to the whole kidney should not exceed 12 Gy when NSS is performed, even if there is high-risk histology. The anticipated use of radiotherapy is used as an argument against NSS when there is a high suspicion of lymph node involvement because the effects of radiotherapy are said to counterbalance any benefit of nephron capital linked to NSS (extension to adjacent organs being a contra-indication of NSS per se). However, radiotherapy-associated kidney injury is a very slow process (particularly in association with the protocolised reduction in radiotherapy dose) and is imprecisely defined (but includes hypertension [41, 42] and functional effects). Therefore, although circumstances that may mandate radiotherapy should be considered in decision-making around performing NSS, a rationale for it remains so long as the oncological principles of surgery can be maintained (further discussed under “Nephron-sparing surgery” and illustrated in Fig. 2).
Cardiovascular morbidity and mortality
Long-term studies of WT survivors demonstrate significant cardiovascular morbidity and mortality into adulthood [43]. A recent study from the Childhood Cancer Survivor Study (of which 7–9% had WT) confirmed that life expectancy has improved amongst adult survivors of childhood cancer. The gap for life expectancy (compared with individuals without a history of childhood cancer) was 25% for those diagnosed in 1970–1979, 19% for those diagnosed in 1980–1989, and 14% for those diagnosed in 1990–1999 [1].
The risk of adverse health outcomes was well defined by a large cohort of WT survivors (n = 1441) in the British Cancer Survivor Study [43]. Cumulative risk of death increased from 5.4% at 30 years from diagnosis, to 22.7% at 50 years from diagnosis. Three-quarters of excess deaths beyond 30 years were attributable to second primary malignancies (50%) and cardiac diseases (25%). Radiotherapy exposure was a risk factor for both outcomes [43].
The same group confirmed that survivors of childhood cancer experienced three times the number of cardiac deaths compared to the general population. Of all the primary tumour types included, WT survivors were found to have the greatest risk of ischemic heart disease. This was attributed to hypertension and having a solitary kidney, as cardiac radiotherapy exposure in these survivors would be anticipated to be less than the comparator tumour groups (e.g. Hodgkin lymphoma) [44]. Childhood cancer survivors are not immune to the host of cardiovascular risk factors that plague the general population: obesity, diabetes mellitus, smoking, positive family history of myocardial infarction/stroke, arterial hypertension, and dyslipidaemia; in fact they experience higher rates of the latter two [45]. In children surviving renal tumours, heart failure in particular leads to a 15-fold increase in hospitalisation compared to the general population [46]. Although this should be interpreted in the context of historical cohorts, nonetheless these studies illustrate the importance of minimising the long-term cardiovascular impacts of treatment in children with renal tumours.
Nephron-sparing surgery
Conditions for NSS
Three conditions are necessary to develop NSS.
-
Expertise: As NSS will represent no more than 15% of WT (including bilateral and syndromic WT), it is imperative to identify a few reference centres to concentrate expertise in each country (depending on population size). In adult urology, outcomes of robot-assisted partial nephrectomy closely relate to centre volume [47]. Low-volume centres were defined as those that performed less than 20 cases per year, and high volume 45–70 cases per year. Positive surgical margins (26% vs. 17%), length of stay (6 days vs. 4.7 days), warm ischaemia time (20 min vs. 15 min), operative time 181 min vs. 150 min), and major complications (12% vs. 4%) all improved significantly with higher centre volume [47]. In paediatrics, such cases are discussed at a regional multidisciplinary meeting at diagnosis. Definitive evaluation is performed at the reference centre following neoadjuvant chemotherapy. This expertise is necessary to maintain an excellent oncological outcome decreasing the risk of surgical up-staging and complications.
-
Neo-adjuvant chemotherapy: The efficacy of neo-adjuvant chemotherapy is well documented in terms of reduction in tumour size and prevention of tumour rupture. Intra-operative tumour rupture may be reported by the surgeon or pathologist. It is defined by the presence of viable tumour cells at the surface of the specimen (beyond the tumour pseudocapsule). Primary nephrectomy carries a 9.7% rate of intra-operative tumour spill [48], versus 2.8% following neoadjuvant chemotherapy [49]. In a review of 75 patients with WT, NSS was feasible in 3% at diagnosis, which increased to 15% following neo-adjuvant chemotherapy [50].
-
Imaging techniques: : A precise understanding of the relationship of the tumour with segmental renal vessels, major calyces, and the renal pelvis is critical to confirm the indication and determine the technique. Spatial understanding of these structures can now be appreciated with 3D reconstructions/printing based on CT scan images [51, 52] (Fig. 1). These provide a more intuitive anatomical assessment between the relationship of the tumour, arteries, veins, and collecting system, helping paediatric oncology surgeons in decision-making regarding NSS [52]. Furthermore, adult studies of partial nephrectomy confirm that inclusion of 3D virtual models: improves post-operative kidney function [53], and results in fewer collecting system injuries [54], and less transfusion requirement [54]. Intraoperative US can also be employed to visualize the critical relationships of the tumour and to aid in determining resection margins [55].
To allow accurate assessment of the impact of NSS, functional studies (DMSA scan) should be performed six months post-operatively. The UMBRELLA protocol also allows for a DMSA scan pre-operatively to clarify the anticipated contribution of spared renal tissue where this is equivocal.
Indications
From a surgical perspective, the possibility of NSS should be at the forefront of the surgeons’ mind following neoadjuvant chemotherapy for WT. However, from the International Society of Paediatric Oncology WT trial 2001 (published in 2014), NSS was only employed in 3% of cases (whereas based on the literature one would have expected 5–10% of cases to be eligible for NSS) [3]. When reviewing participating Children’s Oncology Study group centres broadly (in the context of very low-risk and small tumours), only 8% of cases were deemed possible based on pre-treatment imaging [56]. There is an intrinsic challenge in developing treatment protocols that are to be applied in a variety of geographic locations and co-operative centres. The post-operative pathological specimen review suggests NSS may be applied in 25% of children with unilateral WT following neoadjuvant chemotherapy [57]; nonetheless, even large-volume single centres only report application as possible in 4–9% [35]. The reason for this discrepancy has not been clarified.
In the UMBRELLA protocol, conditions for NSS in unilateral non-syndromic WT were established (see Fig. 2). In a feasibility study of 75 unscreened unilateral non-syndromic WT, a blinded review of pre-operative CT scans utilizing the above criteria yielded 6% of patients were potentially amenable to NSS. The necessity to preserve greater than two-thirds of renal parenchyma is somewhat arbitrary, and details of how exactly this is to be calculated are not provided in the protocol. If this number is adjusted to 50%, NSS could be applied to 9% of patients, and if more than one-third of renal parenchyma is to be preserved 15% of patients may undergo NSS [50]. Although the ability to preserve functional renal parenchyma is an important consideration, we believe the relationship of the tumour to critical hilar structures is paramount.
In a small but detailed study of NSS in unilateral WT, an excellent functional recovery was observed in patients with > 40% preserved volume, with the preserved kidney demonstrating catch-up growth and function on DMSA scans during adolescence [58].
A further questionable criterion is initial tumour volume (< 300 mL) [2]. This is rationalized in the protocol by the fact that lymph node positivity is the exception rather than the rule in small tumours (5.5%) [59]. Both major study groups have confirmed that tumour volume correlates with lymph node positivity [60, 61]. A smaller tumour < 4 cm is also likely to be associated with a more benign eventual pathological diagnosis [62].
Lymph node positivity would necessitate radiotherapy as previously discussed, whose long-term impact on the remaining renal parenchyma remains ill-defined (further discussed under “Specific factors affecting kidney function in cases of Wilms tumour”). The effectiveness of lymph node sampling in the context of NSS has been questioned by a SEER (Surveillance, Epidemiology and End Results) database study. This study indicated that regional lymphadenectomy was omitted much more frequently when NSS was performed as opposed to TN (56% vs. 16%, p < 0.001) [63]. This is not because of technical limitations, but rather a surgical misconception or omission when performing NSS, and should be improved in the future.
Technical aspects
In unilateral non-syndromic WT, partial nephrectomy with a rim of normal parenchyma has been advocated by surgeons, pathologists [61], and in protocols [2], in an effort to decrease the risk of incomplete resection. This is a concept that is useful to prevent positive surgical margins, although the recommended margin of normal parenchyma has not been clarified. However, there are some circumstances where this rule may be excessive. In a polar exophytic tumour where the rim of normal parenchyma is thin, following neoadjuvant chemotherapy a pseudocapsule usually forms. If there is no rupture of the lesion at this point, and the surgical margins are clear otherwise, NSS may be considered safe. Laparoscopic-assisted open procedures [64] and robotic-assisted laparoscopic [65] partial nephrectomy have both been described with success. It should be emphasised however that NSS utilising a transperitoneal minimally invasive approach is not recommended because of the risk of massive spillage if margins are not secured, made worse by insufflation, and necessitating whole abdominal irradiation.
Regardless of the approach and depending on tumour localization, it can be necessary to temporarily clamp the renal artery, which can be safely done for up to 30 min [66]. Other authors advocate for a “zero-ischemia” approach, avoiding any major vessel clamping [58, 64]. Even complex closure of the collecting system can be safely performed without utilizing a JJ stent [67], which has the benefit of not interfering with ureteric peristalsis [68]. Lymph node sampling is then performed in the hilar, ipsilateral paraaortic, and caval nodes [69], with the intention of obtaining at least seven lymph nodes [2].
Complications
The largest and most comprehensive report comparing the complication profiles of NSS vs. TN suggested a higher rate of complications associated with NSS (36.4% vs. 13%). Prolonged urinary leak (persisting > 5 days following surgery) was the most common complication and the only complication with a statistically significant difference between groups (16% vs. 0%, p = 0.003) [67]. It must be noted that the majority of NSS in this study was done in the context of bilateral WT which is by nature more complex. When unilateral non-syndromic WT alone are compared, the difference in complication rate appears less pronounced (10% vs. 5%, p = 0.052) [3].
Nonetheless, surgical complications including urinary leak are problematic, requiring drainage that classically delays the resumption of adjuvant chemotherapy.
Oncological outcomes
In the International Society of Paediatric Oncology WT trial 2001 (published in 2014) the overall survival and event-free survival in unilateral WT were compared for NSS (91 patients) and TN (2709 patients). Both overall survival (NSS: 100% vs. TN: 94.4%, p = 0.06) and event-free survival (NSS: 94.8% vs. TN: 86.5%, p = 0.06) were similar amongst the two groups. However, in the NSS group, the tumours were smaller and more often limited to the kidney (65% vs. 48%). In this study, the incidence of positive surgical margins in the NSS group was 9% (8/91) and the incidence of positive surgical margins in the TN was 13% (355/2709) [3]. In a separate study, relapse rates were also found to be identical between NSS and TN (when stage and grade of tumour are controlled for) [70].
When considering NSS, the incidence of positive margin is critical. Flank radiotherapy will have consequences on the residual renal parenchyma, although this has been difficult to define [41]. The long-term impact of radiotherapy has also been well documented, with reduced life expectancy [1], and higher rates of second primary malignancies [71].
Kidney outcomes
Because of limited numbers and follow-up of patients with unilateral non-syndromic WT that have undergone NSS, broad and long-term evaluation of kidney function is not well documented. One long-term study following children after NSS or TN for renal tumours into the fifth decade showed significantly higher eGFR measurements associated with NSS, both after the second decade (110 ml/min/1.73 m2 vs. 91.2 ml/min/1.73 m2), and at last follow-up (110 ml/min/1.73 m2 vs. 95 ml/min/1.73 m2, p = 0.02) [72]. Although other studies with shorter follow-up are less impactful, a recent meta-analysis of all studies confirmed higher eGFR in children undergoing NSS (116 ml/min/1.73 m2 vs. 98 ml/min/1.73 m2) [73]. Recommendations for surveillance of kidney function and hypertension in WT survivors have been published, although they are based on personal opinion, and extrapolation from solitary kidney and cancer survivorship literature [74].
Conclusion
In the long term, a proportion of patients undergoing TN for unilateral non-syndromic WT will experience a decline in kidney function, hypertension, and/or cardiovascular morbidity. These patients cannot be accurately predicted prior to surgery. For these reasons, NSS must be considered and discussed with patients in whom it is technically feasible, in an effort to reduce morbidity and mortality into adulthood. To decrease the incidence of positive surgical margins, incomplete lymph node sampling, and complications, these procedures should be performed at specialised and experienced reference centres. Based on the impacts of individual treatment pathways, survivors of childhood WT need to be followed throughout adulthood for nephroprotection and to monitor kidney function, blood pressure, and albuminuria, and prevent cardiovascular events.
Abbreviations
- NSS:
-
Nephron-sparing surgery
- WT:
-
Wilms tumour
- TN:
-
Total nephrectomy
- GFR:
-
Glomerular filtration rate
- CSK:
-
Congenital single kidney
- ASK:
-
Acquired single kidney
References
Yeh JM, Ward ZJ, Chaudhry A, Liu Q, Yasui Y, Armstrong GT, Gibson TM, Howell R, Hudson MM, Krull KR, Leisenring WM, Oeffinger KC, Diller L (2020) Life expectancy of adult survivors of childhood cancer over 3 decades. JAMA Oncol 6:350–357
Van Den Heuvel-eibrink MM, Hol JA, Pritchard-Jones K, Van Tinteren H, Furtwängler R, Verschuur AC, Vujanic GM, Leuschner I, Brok J, Rübe C (2017) Rationale for the treatment of Wilms tumour in the UMBRELLA SIOP–RTSG 2016 protocol. Nat Rev Urol 14:743–752
Wilde JC, Aronson DC, Sznajder B, Van Tinteren H, Powis M, Okoye B, Cecchetto G, Audry G, Fuchs J, Schweinitz DV, Heij H, Graf N, Bergeron C, Pritchard-Jones K, Van Den Heuvel-Eibrink M, Carli M, Oldenburger F, Sandstedt B, De Kraker J, Godzinski J (2014) Nephron sparing surgery (NSS) for unilateral Wilms tumor (UWT): the SIOP 2001 experience. Pediatr Blood Cancer 61:2175–2179
Lopes RI, Lorenzo A (2017) Recent advances in the management of Wilms’ tumor. F1000Res 6:670
KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease (2013) Chapter 1: Definition and classification of CKD. Kidney Int Suppl 3:19–62. https://doi.org/10.1038/kisup.2012.64
Levey AS, Eckardt K-U, Dorman NM, Christiansen SL, Hoorn EJ, Ingelfinger JR, Inker LA, Levin A, Mehrotra R, Palevsky PM (2020) Nomenclature for kidney function and disease: report of a Kidney Disease: Improving Global Outcomes (KDIGO) Consensus Conference. Kidney Int 97:1117–1129
Pasala S, Carmody JB (2017) How to use… serum creatinine, cystatin C and GFR. Arch Dis Child Educ Pract Ed 102:37–43
Weinstein JR, Anderson S (2010) The aging kidney: physiological changes. Adv Chronic Kidney Dis 17:302–307
Hoy WE, Douglas-Denton RN, Hughson MD, Cass A, Johnson K, Bertram JF (2003) A stereological study of glomerular number and volume: preliminary findings in a multiracial study of kidneys at autopsy. Kidney Int 63:S31–S37
Nyengaard J, Bendtsen T (1992) Glomerular number and size in relation to age, kidney weight, and body surface in normal man. Anat Rec 232:194–201
Bertram JF, Douglas-Denton RN, Diouf B, Hughson MD, Hoy WE (2011) Human nephron number: implications for health and disease. Pediatr Nephrol 26:1529–1533
Hughson M, Farris AB III, Douglas-Denton R, Hoy WE, Bertram JF (2003) Glomerular number and size in autopsy kidneys: the relationship to birth weight. Kidney Int 63:2113–2122
Schaeffner ES, Ebert N, Delanaye P, Frei U, Gaedeke J, Jakob O, Kuhlmann MK, Schuchardt M, Tölle M, Ziebig R (2012) Two novel equations to estimate kidney function in persons aged 70 years or older. Ann Intern Med 157:471–481
Tantisattamo E, Dafoe DC, Reddy UG, Ichii H, Rhee CM, Streja E, Landman J, Kalantar-Zadeh K (2019) Current management of patients with acquired solitary kidney. Kidney Int Rep 4:1205–1218
Roos JF, Doust J, Tett SE, Kirkpatrick CM (2007) Diagnostic accuracy of cystatin C compared to serum creatinine for the estimation of renal dysfunction in adults and children—a meta-analysis. Clin Biochem 40:383–391
Stefanowicz J, Kosiak M, Romanowicz G, Owczuk R, Adamkiewicz-Drożyńska E, Balcerska A (2011) Glomerular filtration rate and prevalence of chronic kidney disease in Wilms’ tumour survivors. Pediatr Nephrol 26:759–766
Westland R, Abraham Y, Bökenkamp A, Stoffel-Wagner B, Schreuder MF, van Wijk JA (2013) Precision of estimating equations for GFR in children with a solitary functioning kidney: the KIMONO study. J Am Soc Nephrol 8:764–772
Stengel B, Metzger M, Froissart M, Rainfray M, Berr C, Tzourio C, Helmer C (2011) Epidemiology and prognostic significance of chronic kidney disease in the elderly–the Three-City prospective cohort study. Nephrol Dial Transplant 26:3286–3295
Hostetter T, Olson J, Rennke H, Venkatachalam M, Brenner B (1981) Hyperfiltration in remnant nephrons: a potentially adverse response to renal ablation. Am J Physiol Renal Physiol 241:F85–F93
Schreuder MF (2018) Life with one kidney. Pediatr Nephrol 33:595–604
Grapin M, Gaillard F, Biebuyck N, Ould-Rabah M, Hennequin C, Berthaud R, Dorval G, Blanc T, Hourmant M, Kamar N (2021) The spectrum of kidney function alterations in adolescents with a solitary functioning kidney. Pediatr Nephrol 36:3159–3168
Abou Jaoude P, Dubourg L, Bacchetta J, Berthiller J, Ranchin B, Cochat P (2011) Congenital versus acquired solitary kidney: is the difference relevant? Nephrol Dial Transplant 26:2188–2194
Kim S, Chang Y, Lee YR, Jung H-S, Hyun YY, Lee K-B, Joo KJ, Yun KE, Shin H, Ryu S (2019) Solitary kidney and risk of chronic kidney disease. Eur J Epidemiol 34:879–888
Büberci RK, Duranay M (2022) Risk factors for chronic kidney disease progression in patients with solitary kidney. J Health Sci Med 5:342–347
Groen S, Roeleveld N, Westland R, Renkema KY, Steffens MG, Gracchi V, Lilien MR, van Wijk JA, Feitz WF, Schreuder MF (2023) Uncovering risk factors for kidney injury in children with a solitary functioning kidney. Kidney Int 103:156–165
Akyol Onder EN, Yılmaz O, Taneli C, Ertan P (2023) Follow-up of renal outcomes in children with solitary kidney. Pediatr Int 65:e15488
Cozzi DA, Ceccanti S, Cozzi F (2018) Renal function up to the 5th decade of life after nephrectomy in childhood: a literature review. Nephrology 23:397–404
Cochat P, Febvey O, Bacchetta J, Berard E, Cabrera N, Dubourg L (2019) Towards adulthood with a solitary kidney. Pediatr Nephrol 34:2311–2323
Larsson L, Aperia A, Wilton P (1980) Effect of normal development on compensatory renal growth. Kidney Int 18:29–35
Grupper A, Angel Y, Baruch A, Schwartz IF, Schwartz D, Nakache R, Goykhman Y, Katz P, Nachmany I, Lubezky N, Weinstein T, Shashar M, Ben-Bassat OK, Berliner S, Rogowski O, Zeltser D, Shapira I, Shenhar-Tsarfaty S (2019) Long term metabolic and renal outcomes of kidney donors compared to controls with excellent kidney function. BMC Nephrol 20:30
Moody WE, Ferro CJ, Edwards NC, Chue CD, Lin EL, Taylor RJ, Cockwell P, Steeds RP, Townend JN, CRIB-Donor Study Investigators (2016) Cardiovascular effects of unilateral nephrectomy in living kidney donors. Hypertension 67:368–377
Ibrahim HN, Foley RN, Reule SA, Spong R, Kukla A, Issa N, Berglund DM, Sieger GK, Matas AJ (2016) Renal function profile in white kidney donors: the first 4 decades. J Am Soc Nephrol 27:2885–2893
Mjøen G, Hallan S, Hartmann A, Foss A, Midtvedt K, Øyen O, Reisæter A, Pfeffer P, Jenssen T, Leivestad T (2014) Long-term risks for kidney donors. Kidney Int 86:162–167
Massie AB, Holscher CM, Henderson ML, Fahmy LM, Thomas AG, Al Ammary F, Getsin SN, Snyder JJ, Lentine KL, Garg AX, Segev DL (2020) Association of early postdonation renal function with subsequent risk of end-stage renal disease in living kidney donors. JAMA Surg 155:e195472
Interiano RB, Delos Santos N, Huang S, Srivastava DK, Robison LL, Hudson MM, Green DM, Davidoff AM (2015) Renal function in survivors of nonsyndromic Wilms tumor treated with unilateral radical nephrectomy. Cancer 121:2449–2456
Neu MA, Russo A, Wingerter A, Alt F, Theruvath J, El Malki K, Kron B, Dittrich M, Lotz J, Stein R, Beetz R, Faber J (2017) Prospective analysis of long-term renal function in survivors of childhood Wilms tumor. Pediatr Nephrol 32:1915–1925
Mavinkurve-Groothuis AM, van de Kracht F, Westland R, van Wijk JA, Loonen JJ, Schreuder MF (2016) Long-term follow-up of blood pressure and glomerular filtration rate in patients with a solitary functioning kidney: a comparison between Wilms tumor survivors and nephrectomy for other reasons. Pediatr Nephrol 31:435–441
Mansouri I, Schwartz B, Vu-Bezin G, Bejarano-Quisoboni D, Fresneau B, El-Fayech C, Dufour C, Bolle S, Surun A, Orbach D (2023) Risk of renal or urinary related hospitalisation in survivors of childhood cancer: results from the French Childhood Cancer Survivor Study. Cancer Epidemiol Biomarkers Prev 32:572–581
Spreafico F, Fernandez CV, Brok J, Nakata K, Vujanic G, Geller JI, Gessler M, Maschietto M, Behjati S, Polanco A (2021) Wilms tumour Nat Rev Dis Primers 7:75
Weil BR, Murphy AJ, Liu Q, Howell RM, Smith SA, Weldon CB, Mullen EA, Madenci AL, Leisenring WM, Neglia JP (2023) Late health outcomes among survivors of Wilms tumor diagnosed over three decades: a report from the Childhood Cancer Survivor Study. J Clin Oncol:JCO 22:02111
Kieran K, Williams MA, Dome JS, McGregor LM, Krasin MJ, Davidoff AM (2013) Margin status and tumor recurrence after nephron-sparing surgery for bilateral Wilms tumor. J Pediatr Surg 48:1481–1485
Green DM, Wang M, Krasin MJ, Davidoff AM, Srivastava D, Jay DW, Ness KK, Shulkin BL, Spunt SL, Jones DP, Lanctot JQ, Shelton KC, Brennan RC, Mulrooney DA, Ehrhardt MJ, Gibson TM, Kurt BA, Robison LL, Hudson MM (2020) Long-term renal function after treatment for unilateral, nonsyndromic Wilms tumor. A report from the St. Jude Lifetime Cohort Study. Pediatr Blood Cancer 67:e28271
Wong KF, Reulen RC, Winter DL, Guha J, Fidler MM, Kelly J, Lancashire ER, Pritchard-Jones K, Jenkinson HC, Sugden E, Levitt G, Frobisher C, Hawkins MM (2016) Risk of adverse health and social outcomes up to 50 years after Wilms tumor: The British Childhood Cancer Survivor Study. J Clin Oncol 34:1772–1779
Fidler MM, Reulen RC, Henson K, Kelly J, Cutter D, Levitt GA, Frobisher C, Winter DL, Hawkins MM, British Childhood Cancer Survivor Study Steering Group (2017) Population-based long-term cardiac-specific mortality among 34 489 five-year survivors of childhood cancer in Great Britain. Circulation 135:951–963
Faber J, Wingerter A, Neu M-A, Henninger N, Eckerle S, Münzel T, Lackner KJ, Beutel ME, Blettner M, Rathmann W (2018) Burden of cardiovascular risk factors and cardiovascular disease in childhood cancer survivors: data from the German CVSS-study. Eur Heart J 39:1555–1562
Gudmundsdottir T, Winther FJ, de Fine Licht S, Bonnesen GT, Asdahl HP, Tryggvadottir L, Anderson H, Wesenberg F, Malila N, Hasle H (2015) Cardiovascular disease in adult life after childhood cancer in Scandinavia: a population-based cohort study of 32,308 one-year survivors. Int J Cancer 137:1176–1186
Peyronnet B, Tondut L, Bernhard JC, Vaessen C, Doumerc N, Sebe P, Pradere B, Guillonneau B, Khene ZE, Nouhaud FX, Brichart N, Seisen T, Alimi Q, Beauval JB, Mathieu R, Rammal A, de la Taille A, Baumert H, Droupy S, Bruyere F, Roupret M, Mejean A, Bensalah K, Members of the French Committee of Urologic Oncology (2018) Impact of hospital volume and surgeon volume on robot-assisted partial nephrectomy outcomes: a multicentre study. BJU Int 121:916–922
Gow KW, Barnhart DC, Hamilton TE, Kandel JJ, Chen MK, Ferrer FA, Price MR, Mullen EA, Geller JI, Gratias EJ (2013) Primary nephrectomy and intraoperative tumor spill: report from the Children’s Oncology Group (COG) renal tumors committee. J Pediatr Surg 48:34–38
Godzinski J, Tournade M-F, Dekraker J, Lemerle J, Voute P-A, Weirich A, Ludwig R, Rapala M, Skotnicka G, Gauthier F (1998) Rarity of surgical complications after postchemotherapy nephrectomy for nephroblastoma. Experience of the International Society of Paediatric Oncology-Trial and Study. Eur J Pediatr Surg 8:83–86
Leclair MD, Floret A, Pellier I, Renaudin-Autain K, Quere MP, Thebaud E (2015) Supplement: Abstracts From the 47th Congress of the International Society of Paediatric Oncology (SIOP) Cape Town, South Africa October 8–11, 2015. O-069: Nephron-sparing surgery for unilateral unscreened Wilms tumour: how often is it feasible? Pediatr Blood Cancer 62:S163
Girón-Vallejo Ó, García-Calderón D, Ruiz-Pruneda R, Cabello-Laureano R, Doménech-Abellán E, Fuster-Soler JL, Ruiz-Jiménez JI (2018) Three-dimensional printed model of bilateral Wilms tumor: a useful tool for planning nephron sparing surgery. Pediatr Blood Cancer 65(4). https://doi.org/10.1002/pbc.26894
Wellens LM, Meulstee J, van de Ven CP, Terwisscha van Scheltinga CEJ, Littooij AS, van den Heuvel-Eibrink MM, Fiocco M, Rios AC, Maal T, Wijnen M (2019) Comparison of 3-dimensional and augmented reality kidney models with conventional imaging data in the preoperative assessment of children with Wilms tumors. JAMA Netw Open 2:e192633
Amparore D, Pecoraro A, Checcucci E, Piramide F, Verri P, De Cillis S, Granato S, Angusti T, Solitro F, Veltri A, Fiori C, Porpiglia F (2022) Three-dimensional virtual models’ assistance during minimally invasive partial nephrectomy minimizes the impairment of kidney function. Eur Urol Oncol 5:104–108
Piramide F, Kowalewski K-F, Cacciamani G, Belenchon IR, Taratkin M, Carbonara U, Marchioni M, De Groote R, Knipper S, Pecoraro A (2022) Three-dimensional model–assisted minimally invasive partial nephrectomy: a systematic review with meta-analysis of comparative studies. Eur Urol Oncol 5:640–650
Aldrink JH, Cost NG, McLeod DJ, Bates DG, Stanek JR, Smith EA, Ehrlich PF (2018) Technical considerations for nephron-sparing surgery in children: what is needed to preserve renal units? J Surg Res 232:614–620
Ferrer FA, Rosen N, Herbst K, Fernandez CV, Khanna G, Dome JS, Mullen E, Gow KW, Barnhart DC, Shamberger RC, Ritchey M, Ehrlich P (2013) Image based feasibility of renal sparing surgery for very low risk unilateral Wilms tumors: a report from the Children’s Oncology Group. J Urol 190:1846–1851
Cost NG, Lubahn JD, Granberg CF, Sagalowsky AI, Wickiser JE, Gargollo PC, Baker LA, Margulis V, Rakheja D (2012) Pathological review of Wilms tumor nephrectomy specimens and potential implications for nephron sparing surgery in Wilms tumor. J Urol 188:1506–1510
Ceccanti S, Cozzi F, Cervellone A, Zani A, Cozzi DA (2019) Volume and function of the operated kidney after nephron-sparing surgery for unilateral renal tumor. J Pediatr Surg 54:326–330
Godzinski J, van Tinteren H, de Kraker J, Graf N, Bergeron C, Heij H, von Schweinitz D, Fuchs J, Cecchetto G, Audry G (2011) Nephroblastoma: does the decrease in tumor volume under preoperative chemotherapy predict the lymph nodes status at surgery? Pediatr Blood Cancer 57:1266–1269
Saltzman A, Carrasco A Jr, Amini A, Aldrink J, Dasgupta R, Gow K, Glick R, Ehrlich P, Cost N (2018) Patterns of lymph node sampling and the impact of lymph node density in favorable histology Wilms tumor: an analysis of the national cancer database. J Pediatr Urol 14:161.e161-161.e168
Godzinski J, Graf N, Audry G (2014) Current concepts in surgery for Wilms tumor—the risk and function-adapted strategy. Eur J Pediatr Surg 24:457–460
Han DS, Walker JP, Nicklawsky A, Boxley P, Halstead NV, Tonzi M, Hecht SL, Staley A, Eguchi M, Cockburn MG (2022) Pediatric small renal masses: can tumor size predict histology and the potential for nephron-sparing surgery? J Urol 209:582–590. https://doi.org/10.1097/JU.0000000000003092
Wang H-HS, Abern MR, Cost NG, Chu DI, Ross SS, Wiener JS, Routh JC (2014) Use of nephron sparing surgery and impact on survival in children with Wilms tumor: a SEER analysis. J Urol 192:1196–1202
Lopes RI, Ming J, Koyle MA, Grant R, Fonseca A, Lorenzo AJ (2017) “Zero-ischemia” laparoscopic-assisted partial nephrectomy for the management of selected children with Wilms tumor following neoadjuvant chemotherapy. Urology 100:103–110
Blanc T, Pio L, Clermidi P, Muller C, Orbach D, Minard-Colin V, Harte C, Meignan P, Kohaut J, Heloury Y, Sarnacki S (2019) Robotic-assisted laparoscopic management of renal tumors in children: preliminary results. Pediatr Blood Cancer 66(Suppl 3):e27867
Warmann SW, Fuchs J (2019) Technical aspects of nephron-sparing surgery (NSS) in children with bilateral centrally located renal tumors. Semin Pediatr Surg 28:150865
Spiegl HR, Murphy AJ, Yanishevski D, Brennan RC, Li C, Lu Z, Gleason J, Davidoff AM (2020) Complications following nephron-sparing surgery for Wilms tumor. J Pediatr Surg 55:126–129
Kinn A-C, Lykkeskov-Andersen H (2002) Impact on ureteral peristalsis in a stented ureter. An experimental study in the pig. Urol Res 30:213–218
Cox S, Büyükünal C, Millar AJ (2020) Surgery for the complex Wilms tumour. Pediatr Surg Int 36:113–127
Schiavetti A, Bonci E, Varrasso G, De Grazia A, Cozzi DA (2020) Evaluation of nephron-sparing surgery as potential risk factor for relapse in unilateral Wilms tumor. J Surg Res 247:21–27
Bhatia S, Sklar C (2002) Second cancers in survivors of childhood cancer. Nat Rev Cancer 2:124–132
Cozzi DA, Ceccanti S, Frediani S, Mele E, Cozzi F (2013) Renal function adaptation up to the fifth decade after treatment of children with unilateral renal tumor: a cross-sectional and longitudinal study. Pediatr Blood Cancer 60:1534–1538
Chen H, Yang S, Qian C (2020) Effectiveness of nephron sparing surgery and radical nephrectomy in the management of unilateral Wilms tumor: a meta-analysis. Front Oncol 10:1248
Hsiao W, Denburg M, Laskin B (2023) Hypertension in Wilms tumor. Pediatr Nephrol. https://doi.org/10.1007/s00467-023-06011-y
Acknowledgements
The authors would like to thank Dr Rani Kassir for acquisition of the 3D reconstruction imaging.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Taghavi, K., Sarnacki, S., Blanc, T. et al. The rationale for nephron-sparing surgery in unilateral non-syndromic Wilms tumour. Pediatr Nephrol 39, 1023–1032 (2024). https://doi.org/10.1007/s00467-023-06099-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06099-2