Abstract
Background
During the COVID-19 pandemic, some continuous kidney replacement therapy (CKRT) initiations were transitioned to telemedicine to improve the timeliness of initiation, and minimize COVID-19 transmission. While telemedicine would appear acceptable for many clinical settings, safety and timeliness of telemedicine CKRT initiation is undescribed.
Methods
We conducted a single-center retrospective cohort study of pediatric patients on CKRT from January 2021–September 2022. Information on patient characteristics and CKRT therapy was extracted from the electronic health record. Multidisciplinary team provider attitudes and perspectives were assessed using survey.
Results
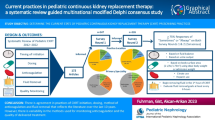
During the study period, there were 101 CKRT circuit initiations in patients not previously receiving CKRT, with 33% (33/101) initiated by telemedicine. There were no differences in patient characteristics, including age, weight at initiation, severity of illness, nor degree of fluid overload between the in-person and telemedicine initiation cohorts. CKRT telemedicine initiations were timelier, occurring on average 3.0 h after decision to initiate therapy compared to 5.8 h for all in-person CKRT starts (p < 0.001) and 5.5 h for night and weekend in-person starts (p < 0.001). Complications did not differ between telemedicine and in-person starts (15% vs. 15%, p = 0.99) and initial circuit life was similar. There were no differences in likelihood of death or duration of CKRT therapy. Telemedicine initiations were widely acceptable to multidisciplinary providers.
Conclusion
In appropriately selected patients, telemedicine initiation of CKRT is a timely and safe option. Further standardization of telemedicine initiation of CKRT should be considered to improve the timely delivery of CKRT and may improve nephrology workforce wellness.
Graphical abstract

A higher resolution version of the Graphical abstract is available as Supplementary information
Similar content being viewed by others
Data availability
De‐identified individual participant data will be made available to researchers who provide a methodologically sound proposal for use in achieving the goals of the approved proposal. The data is de‐identified and a limited access data is available through a request from the corresponding author. Data dictionaries, study protocol, and statistical analysis plan are available upon request.
References
Brophy PD (2017) Overview on the Challenges and Benefits of Using Telehealth Tools in a Pediatric Population. Adv Chronic Kidney Dis 24:17–21
Rohatgi R, Ross MJ, Majoni SW (2017) Telenephrology: current perspectives and future directions. Kidney Int 92:1328–1333
Williams S, Hill K, Xie L, Mathew MS, Ofori A, Perry T, Wesley D, Messiah SE (2021) Pediatric Telehealth Expansion in Response to COVID-19. Front Pediatr 9:642089
Pollack MM, Patel KM, Ruttimann UE (1996) PRISM III: an updated Pediatric Risk of Mortality score. Crit Care Med 24:743–752
Leteurtre S, Duhamel A, Salleron J, Grandbastien B, Lacroix J, Leclerc F (2013) PELOD-2: an update of the PEdiatric logistic organ dysfunction score. Crit Care Med 41:1761–1773
Goldstein SL, Akcan-Arikan A, Alobaidi R, Askenazi DJ, Bagshaw SM, Barhight M, Barreto E, Bayrakci B, Bignall ONR, Bjornstad E, Brophy PD, Chanchlani R, Charlton JR, Conroy AL, Deep A, Devarajan P, Dolan K, Fuhrman DY, Gist KM, Gorga SM, Greenberg JH, Hasson D, Ulrich EH, Iyengar A, Jetton JG, Krawczeski C, Meigs L, Menon S, Morgan J, Morgan CJ, Mottes T, Neumayr TM, Ricci Z, Selewski D, Soranno DE, Starr M, Stanski NL, Sutherland SM, Symons J, Tavares MS, Vega MW, Zappitelli M, Ronco C, Mehta RL, Kellum J, Ostermann M, Basu RK (2022) Consensus-Based Recommendations on Priority Activities to Address Acute Kidney Injury in Children: A Modified Delphi Consensus Statement. JAMA Netw Open 5:e2229442
Goldstein SL, Currier H, Graf C, Cosio CC, Brewer ED, Sachdeva R (2001) Outcome in children receiving continuous venovenous hemofiltration. Pediatrics 107:1309–1312
Clark SL, Begin B, De Souza HG, Mallett K, Hanna MG, Richardson T, Esporas M, Bowie A, Taylor K, Reyes LC, Hughey M, Neu A, Warady BA (2023) Telehealth survey of providers and caregivers of children on peritoneal dialysis during the COVID-19 pandemic. Pediatr Nephrol 38:203–210
Raina R, Nair N, Yap HK, Filler G, Sethi SK, Bagga A, Hari P, Bunchman T, Bartosh S, Twombley K, Kapur G, McCulloch M, Warady BA, Díaz-González de Ferris M, Rush S (2021) Survey of Telemedicine by Pediatric Nephrologists During the COVID-19 Pandemic. Kidney Int Rep 6:2316–2322
Ashoor I, Weidemann D, Elenberg E, Halbach S, Harshman L, Kula A, Mahan JD, Nada A, Quiroga A, Mahon AR, Smith J, Somers M, Brophy PD (2021) The Pediatric Nephrology Workforce Crisis: A Call to Action. J Pediatr 239:5-10.e14
Funding
This work was supported in part by the Indiana University School of Medicine Physician Scientist Initiative. Study data were collected and managed using REDCap electronic data capture tools hosted at the Indiana Clinical and Translational Sciences Institute (Indiana CTSI) funded, in part by Grant Numbers UL1TR001108, KL2TR001106, or TL1TR001107 from the National Institutes of Health, National Center for Advancing Translational Sciences, Clinical and Translational Sciences Award and at the Indiana University Pervasive Technology Institute (https://pti.iu.edu/) which supports REDCap with IT infrastructure and consulting resources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Prior presentation of study data
Elements of this research project were presented at the International Symposium on AKI in Children, Cincinnati, OH, October 1, 2022 and at the Pediatric Academic Societies and American Society of Pediatric Nephrology Annual Meeting, Washington, DC; April 30, 2023.
Competing interests
All authors report no real or perceived conflicts of interest that could affect the study design, collection, analysis, and interpretation of data, the writing of the report, or the decision to submit the manuscript for publication. For full disclosure, we provide the additional list of authors’ other funding not directly related to this study. M.S. is supported in part by the Indiana University School of Medicine Physician Scientist Initiative. No other disclosures were reported. Funding sources for this study had no role in study design, data collection, data analysis, data interpretation, or writing of the report.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Starr, M.C., Altemose, K., Parsley, J. et al. Safety and timeliness of telemedicine initiation of continuous kidney replacement therapy. Pediatr Nephrol 39, 325–329 (2024). https://doi.org/10.1007/s00467-023-06036-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06036-3