Abstract
Background
Edema is one of the cardinal clinical features of nephrotic syndrome (NS). It may vary from mild periorbital edema to severe generalized edema (anasarca). In patients where edema does not improve with prednisone therapy, the most common supportive medications are diuretics and albumin. However, due to the complex pathophysiology of edema formation in NS patients resulting in intravascular normovolemia or hypovolemia, optimal therapy for edema is still debated. We conducted a systematic review with the objective of evaluating the change in urine volume and urine sodium excretion after treatment with furosemide only versus furosemide with albumin in edematous patients with NS.
Objectives
(1) To evaluate efficacy of furosemide alone versus furosemide with albumin in the treatment of nephrotic edema in adults and children. (2) To compare the harms and benefits of different doses of furosemide for treating nephrotic edema.
Search methods
The search included all randomized or quasi-randomized controlled trials in English and French using MEDLINE, Embase, and CENTRAL Trials Registry of the Cochrane Collaboration using the Ovid interface. ClinicalTrials.gov and the International Clinical Trials Registry Platform were also searched.
Selection criteria
We included all RCTs and randomized cross-over studies in which furosemide and furosemide plus albumin are used in the treatment of children or adults with nephrotic edema. We excluded patients with hypoalbuminemia of non-renal origin and severe chronic kidney disease (CKD) with a glomerular filtration rate below 30 ml/min/1.74 m2 and patients with congenital NS.
Data collection and analysis
All abstracts were independently assessed by at least two authors to determine which studies met the inclusion criteria. Information on study design, methodology, and outcome data (urine volume, urine sodium excretion, adverse effects) from each identified study was entered into a separate data sheet. The differences in outcomes between the types of therapy were expressed as standardized mean difference (SMD) with 95% confidence intervals (CI).
Results
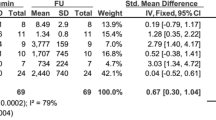
The search yielded 525 records, and after screening, five studies were included in the systematic review and four of those studies in the meta-analysis. One study had high risk of bias and the remaining three studies were deemed to have some concerns. Urine excretion was greater after treatment with furosemide and albumin versus furosemide (SMD 0.85, 95% CI = 0.33 to 1.38). Results for sodium excretion were inconclusive (SMD 0.37, 95%CI = − 0.28 to 1.02).
Authors’ conclusions
The current evidence is not sufficient to make definitive conclusions about the role of albumin in treating nephrotic edema. High-quality randomized studies with adequate samples sizes are needed. Including an assessment of intravascular volume status may be helpful.
Trial registration
Prospero: CRD4201808979. https://www.crd.york.ac.uk/PROSPERO
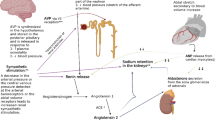
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information.





Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
N/A.
Abbreviations
- NS:
-
Nephrotic syndrome
- RAS:
-
Renin-aldosterone system
- IV:
-
Intravenous
- ADH:
-
Antidiuretic hormone
- RCT:
-
Randomized controlled trials
- GFR:
-
Glomerular filtration rate
- SMD:
-
Standardized mean difference
- CI:
-
Confidence intervals
- AKI:
-
Acute kidney injury
References
Vande Walle JG, Donckerwolcke RA (2001) Pathogenesis of edema formation in the nephrotic syndrome. Pediatr Nephrol 16:283–293
Cadnapaphornchai MA, Tkachenko O, Shchekochikhin D, Schrier RW (2014) The nephrotic syndrome: pathogenesis and treatment of edema formation and secondary complications. Pediatr Nephrol 29:1159–1167. https://doi.org/10.1007/s00467-013-2567-8
Zacchia M, Trepiccione F, Morelli F, Pani A, Capasso G (2008) Nephrotic syndrome: new concepts in the pathophysiology of sodium retention. J Nephrol 21:836–842
Vande Walle JG, Donckerwolcke RA, Koomans HA (1999) Pathophysiology of edema formation in children with nephrotic syndrome not due to minimal change disease. J Am Soc Nephrol 10:323–331
Doucet A, Favre G, Deschênes G (2007) Molecular mechanism of edema formation in nephrotic syndrome: therapeutic implications. Pediatr Nephrol 22:1983–1990. https://doi.org/10.1007/s00467-007-0521-3
Elwell RJ, Spencer AP, Eisele G (2003) Combined furosemide and human albumin treatment for diuretic-resistant edema. Ann Pharmacother 37:695–700. https://doi.org/10.1345/aph.1C320
Fliser D, Zurbrüggen I, Mutschler E, Bischoff I, Nussberger J, Franek E, Ritz E (1999) Coadministration of albumin and furosemide in patients with the nephrotic syndrome. Kidney Int 55:629–634. https://doi.org/10.1046/j.1523-1755.1999.00298.x
González-Martín G, Bravo I, Ibarra N, Arancibia A (1983) Clinical pharmacokinetics of furosemide in children with nephrotic syndrome. Int J Clin Pharmacol 21:598–601
Agarwal R, Gorski JC, Sundblad K, Brater DC (2000) Urinary protein binding does not affect response to furosemide in patients with nephrotic syndrome. J Am Soc Nephrol 11:1100–1105. https://doi.org/10.1681/ASN.V1161100
Ho JJ, Adnan AS, Kueh YC, Ambak NJ, Van Rostenberghe H, Jummaat F (2019) Human albumin infusion for treating oedema in people with nephrotic syndrome. Cochrane Database Syst Rev 7:CD009692. https://doi.org/10.1002/14651858.CD009692.pub2
Kitsios GD, Mascari P, Ettunsi R, Gray AW (2014) Co-administration of furosemide with albumin for overcoming diuretic resistance in patients with hypoalbuminemia: a meta-analysis. J Crit Care 29:253–259. https://doi.org/10.1016/j.jcrc.2013.10.004
Higgins JPT, Savović J, Page MJ, Elbers RG, et al. Chapter 8: Assessing risk of bias in a randomized trial. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane handbook for systematic reviews of interventions version 6.0 (updated July 2019). Cochrane, 2019. Available from www.training.cochrane.org/handbook. In.
Sterne JAC, Savović J, Page MJ, Elbers RG et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898. https://doi.org/10.1136/bmj.l4898
Chandler J, McKenzie J, Boutron I, Welch V (eds) (2016) Cochrane methods. Cochrane Database Syst Rev (10 Suppl 1). https://doi.org/10.1002/14651858.CD201601
Elbourne DR, Altman DG, Higgins JP, Curtin F, Worthington HV, Vail A (2002) Meta-analyses involving cross-over trials: methodological issues. Int J Epidemiol 31:140–149. https://doi.org/10.1093/ije/31.1.140
Hedges LV (1981) Distribution theory for glass’s estimator of effect size and related estimators. J Educ Stat 6:107–128. https://doi.org/10.3102/10769986006002107
Balduzzi S, Rücker G, Schwarzer G (2019) How to perform a meta-analysis with R: a practical tutorial. Evid Based Ment Health 22:153–160. https://doi.org/10.1136/ebmental-2019-300117
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Na KY, Han JS, Kim YS, Ahn C, Kim S, Lee JS, Bae KS, Jang IJ, Shin SG, Huh W, Jeon US (2001) Does albumin preinfusion potentiate diuretic action of furosemide in patients with nephrotic syndrome? J Korean Med Sci 16:448–454. https://doi.org/10.3346/jkms.2001.16.4.448
Akcicek F, Yalniz T, Basci A, Ok E, Mees EJ (1995) Diuretic effect of frusemide in patients with nephrotic syndrome: is it potentiated by intravenous albumin? BMJ 310:162–163. https://doi.org/10.1136/bmj.310.6973.162
Dharmaraj R, Hari P, Bagga A (2009) Randomized cross-over trial comparing albumin and frusemide infusions in nephrotic syndrome. Pediatr Nephrol 24:775–782. https://doi.org/10.1007/s00467-008-1062-0
Ghafari A, Mehdizadeh A, Alavi-Darazam I, Rahimi E, Kargar C, Sepehrvand N (2011) Co-administration of albumin-furosemide in patients with the nephrotic syndrome. Saudi J Kidney Dis Transpl 22:471–475
Kapur G, Valentini RP, Imam AA, Mattoo TK (2009) Treatment of severe edema in children with nephrotic syndrome with diuretics alone–a prospective study. Clin J Am Soc Nephrol 4:907–913. https://doi.org/10.2215/CJN.04390808
Vande Walle JG, Donckerwolcke RA, van Isselt JW, Derkx FH, Joles JA, Koomans HA (1995) Volume regulation in children with early relapse of minimal-change nephrosis with or without hypovolaemic symptoms. Lancet 346:148–152. https://doi.org/10.1016/s0140-6736(95)91210-x
Hahn D, Hodson EM, Willis NS, Craig JC (2015) Corticosteroid therapy for nephrotic syndrome in children. Cochrane Database Syst Rev (3):CD001533. https://doi.org/10.1002/14651858.CD001533.pub5
Pasini A, Benetti E, Conti G, Ghio L et al (2017) The Italian Society for Pediatric Nephrology (SINePe) consensus document on the management of nephrotic syndrome in children: part I - diagnosis and treatment of the first episode and the first relapse. Ital J Pediatr 43:41. https://doi.org/10.1186/s13052-017-0356-x
Haws RM, Baum M (1993) Efficacy of albumin and diuretic therapy in children with nephrotic syndrome. Pediatrics 91:1142–1146
Lee S, Jeong J, Hwang S (2000) The effect of human albumin infusion on the clinical course of steroid sensitive nephrotic syndrome. J Korean Soc Pediatr Nephrol 4:102–110
Acknowledgements
We thank Katie O’Hearn, Msc, (Children’s Hospital of Eastern Ontario Research Institute) for methodological assistance and Margaret Sampson, MLIS, PhD, AHIP, (Children’s Hospital of Eastern Ontario) for developing the electronic search strategies.
Author information
Authors and Affiliations
Contributions
Dr. Erin Hedin helped design the study, carried out the systematic review, drafted the initial manuscript, and reviewed and revised the manuscript. Vid Bijelić and Dr. Nick Barrowman carried out the data analysis and reviewed and revised the manuscript. Dr. Pavel Geier conceptualized and designed the study, carried out the systematic review, helped draft the initial manuscript, and critically reviewed the manuscript for intellectual content.
All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics approval
N/A
Consent to participate
N/A
Consent for publication
All authors have consented to publication if accepted.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary Methods S1: Electronic search strategies.
Supplementary Material S2: Risk of bias assessment of included studies.
Supplementary Figure S3: Risk of bias assessment of included studies.
Supplementary Figure S4: Risk of bias assessment of included studies.(PDF 255 KB)
Rights and permissions
About this article
Cite this article
Hedin, E., Bijelić, V., Barrowman, N. et al. Furosemide and albumin for the treatment of nephrotic edema: a systematic review. Pediatr Nephrol 37, 1747–1757 (2022). https://doi.org/10.1007/s00467-021-05358-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-021-05358-4