Abstract
Background
The obesity pandemic has worsened global disease burden, including type 2 diabetes, cardiovascular disease, and cancer. Metabolic/bariatric surgery (MBS) is the most effective and durable obesity treatment, but the mechanisms underlying its long-term weight loss efficacy remain unclear. MBS drives substrate oxidation that has been linked to improvements in metabolic function and improved glycemic control that are potentially mediated by mitochondria—a primary site of energy production. As such, augmentation of intestinal mitochondrial function may drive processes underlying the systemic metabolic benefits of MBS. Herein, we applied a highly sensitive technique to evaluate intestinal mitochondrial function ex vivo in a mouse model of MBS.
Methods
Mice were randomized to surgery, sham, or non-operative control. A simplified model of MBS, ileal interposition, was performed by interposition of a 2-cm segment of terminal ileum into the proximal bowel 5 mm from the ligament of Treitz. After a four-week recovery period, intestinal mucosa of duodenum, jejunum, ileum, and interposed ileum were assayed for determination of mitochondrial respiratory function. Citrate synthase activity was measured as a marker of mitochondrial content.
Results
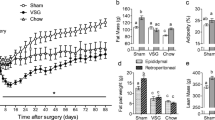
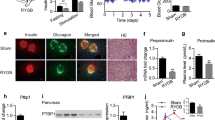
Ileal interposition was well tolerated and associated with modest body weight loss and transient hypophagia relative to controls. Mitochondrial capacity declined in the native duodenum and jejunum of animals following ileal interposition relative to controls, although respiration remained unchanged in these segments. Similarly, ileal interposition lowered citrate synthase activity in the duodenum and jejunum following relative to controls but ileal function remained constant across all groups.
Conclusion
Ileal interposition decreases mitochondrial volume in the proximal intestinal mucosa of mice. This change in concentration with preserved respiration suggests a global mucosal response to segment specific nutrition signals in the distal bowel. Future studies are required to understand the causes underlying these mitochondrial changes.


Similar content being viewed by others
References
Ciciurkaite G, Moloney ME, Brown RL (2019) The incomplete medicalization of obesity: physician office visits, diagnoses, and treatments, 1996–2014. Public Health Rep 134:141–149. https://doi.org/10.1177/0033354918813102
Hales CM, Carroll MD, Fryar CD, Ogden CL (2020) Prevalence of obesity and severe obesity among adults: United States, 2017–2018. NCHS Data Brief 1–8
Schauer PR, Bhatt DL, Kirwan JP, Wolski K, Aminian A, Brethauer SA, Navaneethan SD, Singh RP, Pothier CE, Nissen SE, Kashyap SR, Investigators S (2017) Bariatric surgery versus intensive medical therapy for diabetes—5-year outcomes. New Engl J Med 376:641–651. https://doi.org/10.1056/nejmoa1600869
Steenackers N, Vanuytsel T, Augustijns P, Tack J, Mertens A, Lannoo M, der Schueren BV, Matthys C (2021) Adaptations in gastrointestinal physiology after sleeve gastrectomy and Roux-en-Y gastric bypass. Lancet Gastroenterol Hepatol 6:225–237. https://doi.org/10.1016/s2468-1253(20)30302-2
Akalestou E, Miras AD, Rutter GA, le Roux CW (2021) Mechanisms of weight loss after obesity surgery. Endocr Rev 43:bnab22. https://doi.org/10.1210/endrev/bnab022
Clapp B, Ponce J, DeMaria E, Ghanem O, Hutter M, Kothari S, LaMasters T, Kurian M, English W (2022) American society for metabolic and bariatric surgery 2020 estimate of metabolic and bariatric procedures performed in the United States. Surg Obes Relat Dis 18:1134–1140. https://doi.org/10.1016/j.soard.2022.06.284
Steenackers N, Vanuytsel T, Augustijns P, Deleus E, Deckers W, Deroose CM, Falony G, Lannoo M, Mertens A, Mols R, Vangoitsenhoven R, Wauters L, der Schueren BV, Matthys C (2023) Effect of sleeve gastrectomy and Roux-en-Y gastric bypass on gastrointestinal physiology. Eur J Pharm Biopharm 183:92–101. https://doi.org/10.1016/j.ejpb.2022.12.018
Seeley RJ, Chambers AP, Sandoval DA (2015) The role of gut adaptation in the potent effects of multiple bariatric surgeries on obesity and diabetes. Cell Metab 21:369–378. https://doi.org/10.1016/j.cmet.2015.01.001
Williams JM, Duckworth CA, Burkitt MD, Watson AJM, Campbell BJ, Pritchard DM (2015) Epithelial cell shedding and barrier function. Vet Pathol 52:445–455. https://doi.org/10.1177/0300985814559404
Mulla CM, Middelbeek RJW, Patti M (2018) Mechanisms of weight loss and improved metabolism following bariatric surgery. Ann NY Acad Sci 1411:53–64. https://doi.org/10.1111/nyas.13409
Lahera V, de las Heras N, López-Farré A, Manucha W, Ferder L (2017) Role of mitochondrial dysfunction in hypertension and obesity. Curr Hypertens Rep 19:11. https://doi.org/10.1007/s11906-017-0710-9
Boengler K, Kosiol M, Mayr M, Schulz R, Rohrbach S (2017) Mitochondria and ageing: role in heart, skeletal muscle and adipose tissue. J Cachexia Sarcopenia Muscle 8:349–369. https://doi.org/10.1002/jcsm.12178
Cao K, Xu J, Zou X, Li Y, Chen C, Zheng A, Li H, Li H, Szeto IM-Y, Shi Y, Long J, Liu J, Feng Z (2014) Hydroxytyrosol prevents diet-induced metabolic syndrome and attenuates mitochondrial abnormalities in obese mice. Free Radical Bio Med 67:396–407. https://doi.org/10.1016/j.freeradbiomed.2013.11.029
Sergi D, Naumovski N, Heilbronn LK, Abeywardena M, O’Callaghan N, Lionetti L, Luscombe-Marsh N (2019) Mitochondrial (Dys)function and insulin resistance: from pathophysiological molecular mechanisms to the impact of diet. Front Physiol 10:532. https://doi.org/10.3389/fphys.2019.00532
Guerbette T, Boudry G, Lan A (2022) Mitochondrial function in intestinal epithelium homeostasis and modulation in diet-induced obesity. Mol Metab 63:101546. https://doi.org/10.1016/j.molmet.2022.101546
Axelrod CL, King WT, Davuluri G, Noland RC, Hall J, Hull M, Dantas WS, Zunica ER, Alexopoulos SJ, Hoehn KL, Langohr I, Stadler K, Doyle H, Schmidt E, Nieuwoudt S, Fitzgerald K, Pergola K, Fujioka H, Mey JT, Fealy C, Mulya A, Beyl R, Hoppel CL, Kirwan JP (2020) BAM15-mediated mitochondrial uncoupling protects against obesity and improves glycemic control. Embo Mol Med 12:e12088. https://doi.org/10.15252/emmm.202012088
Zunica ERM, Axelrod CL, Gilmore LA, Kirwan JP (2021) Analytical determination of mitochondrial function of excised solid tumor homogenates. J Vis Exp. https://doi.org/10.3791/62875
Larsen S, Nielsen J, Hansen CN, Nielsen LB, Wibrand F, Stride N, Schroder HD, Boushel R, Helge JW, Dela F, Hey-Mogensen M (2012) Biomarkers of mitochondrial content in skeletal muscle of healthy young human subjects. J Physiol 590:3349–3360. https://doi.org/10.1113/jphysiol.2012.230185
Strader AD, Vahl TP, Jandacek RJ, Woods SC, D’Alessio DA, Seeley RJ (2005) Weight loss through ileal transposition is accompanied by increased ileal hormone secretion and synthesis in rats. Am J Physiol-endocrinol M 288:E447–E453. https://doi.org/10.1152/ajpendo.00153.2004
Culnan DM, Albaugh V, Sun M, Lynch CJ, Lang CH, Cooney RN (2010) Ileal interposition improves glucose tolerance and insulin sensitivity in the obese Zucker rat. Am J Physiol-gastrointest L 299:G751–G760. https://doi.org/10.1152/ajpgi.00525.2009
Kohli R, Kirby M, Setchell KDR, Jha P, Klustaitis K, Woollett LA, Pfluger PT, Balistreri WF, Tso P, Jandacek RJ, Woods SC, Heubi JE, Tschoep MH, D’Alessio DA, Shroyer NF, Seeley RJ (2010) Intestinal adaptation after ileal interposition surgery increases bile acid recycling and protects against obesity-related comorbidities. Am J Physiol Gastrointest Liver Physiol 299:G652–G660. https://doi.org/10.1152/ajpgi.00221.2010
Nath S (2019) Integration of demand and supply sides in the ATP energy economics of cells. Biophys Chem 252:106208. https://doi.org/10.1016/j.bpc.2019.106208
Houten SM, Violante S, Ventura FV, Wanders RJA (2015) The biochemistry and physiology of mitochondrial fatty acid β-oxidation and its genetic disorders. Annu Rev Physiol 78:1–22. https://doi.org/10.1146/annurev-physiol-021115-105045
Sarparanta J, García-Macia M, Singh R (2017) Autophagy and mitochondria in obesity and type 2 diabetes. Curr Diabetes Rev 13:352–369. https://doi.org/10.2174/1573399812666160217122530
Dantas WS, Zunica ERM, Heintz EC, Vandanmagsar B, Floyd ZE, Yu Y, Fujioka H, Hoppel CL, Belmont KP, Axelrod CL, Kirwan JP (2022) Mitochondrial uncoupling attenuates sarcopenic obesity by enhancing skeletal muscle mitophagy and quality control. J Cachexia Sarcopenia Muscle 13:1821–1836. https://doi.org/10.1002/jcsm.12982
Franquet E, Watts G, Kolodny GM, Goldfine AB, Patti M-E (2019) PET-CT reveals increased intestinal glucose uptake after gastric surgery. Surg Obes Relat Dis 15:643–649. https://doi.org/10.1016/j.soard.2019.01.018
Cho A, Kwon IG, Kim S, Noh SH, Ku CR (2020) Altered systematic glucose utilization after gastrectomy: correlation with weight loss. Surg Obes Relat Dis 16:900–907. https://doi.org/10.1016/j.soard.2020.03.003
Saeidi N, Meoli L, Nestoridi E, Gupta NK, Kvas S, Kucharczyk J, Bonab AA, Fischman AJ, Yarmush ML, Stylopoulos N (2013) Reprogramming of intestinal glucose metabolism and glycemic control in rats after gastric bypass. Science 341:406–410. https://doi.org/10.1126/science.1235103
Koopmans H, Sclafani A, Fichtner C, Aravich P (1982) The effects of ileal transposition on food intake and body weight loss in VMH-obese rats. Am J Clin Nutr 35:284–293. https://doi.org/10.1093/ajcn/35.2.284
Acknowledgements
The authors would like to thank the staff of the Comparative Biology Core facility at Pennington Biomedical Research Center for exceptional animal care.
Funding
The research presented in this manuscript was in part supported by NIH Grants U54GM104940 and T32 AT004094 and received no additional specific funding from any agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Elizabeth Zunica receives support from the National Institute of Health grant T32AT004094; Dr. Philip Schauer receives support via institutional grants from Ethicon and Medtronic, consulting fees from GI Dynamics, Mediflix, and Persona, speaker fees from Ethicon, Medtronic, Lilly, and Novo Nordisk, and has equity in SE Healthcare LLC, Mediflix, and Metabolic Health International LTD. Dr. Robert C. Ross, Elizabeth Heintz, R. Leigh Townsend, Amanda Spence, Dr. John P. Kirwan, Christopher L. Axelrod, and Dr. Vance L. Albaugh have no financial relationships with any pharmaceutical or device company.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ross, R.C., Heintz, E.C., Zunica, E.R.M. et al. Bariatric surgery alters mitochondrial function in gut mucosa. Surg Endosc 37, 8810–8817 (2023). https://doi.org/10.1007/s00464-023-10351-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10351-z