Abstract
Background
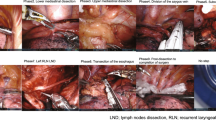
Artificial intelligence (AI) has been largely investigated in the field of surgery, particularly in quality assurance. However, AI-guided navigation during surgery has not yet been put into practice because a sufficient level of performance has not been reached. We aimed to develop deep learning-based AI image processing software to identify the location of the recurrent laryngeal nerve during thoracoscopic esophagectomy and determine whether the incidence of recurrent laryngeal nerve paralysis is reduced using this software.
Methods
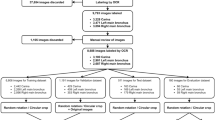
More than 3000 images extracted from 20 thoracoscopic esophagectomy videos and 40 images extracted from 8 thoracoscopic esophagectomy videos were annotated for identification of the recurrent laryngeal nerve. The Dice coefficient was used to assess the detection performance of the model and that of surgeons (specialized esophageal surgeons and certified general gastrointestinal surgeons). The performance was compared using a test set.
Results
The average Dice coefficient of the AI model was 0.58. This was not significantly different from the Dice coefficient of the group of specialized esophageal surgeons (P = 0.26); however, it was significantly higher than that of the group of certified general gastrointestinal surgeons (P = 0.019).
Conclusions
Our software’s performance in identification of the recurrent laryngeal nerve was superior to that of general surgeons and almost reached that of specialized surgeons. Our software provides real-time identification and will be useful for thoracoscopic esophagectomy after further developments.





Similar content being viewed by others
Change history
24 October 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00464-022-09705-w
References
Udagawa H, Ueno M, Shinohara H, Haruta S, Kaida S, Nakagawa M, Tsurumaru M (2012) The importance of grouping of lymph node stations and rationale of three-field lymphoadenectomy for thoracic esophageal cancer. J Surg Oncol 106:742–747
Cuschieri A, Shimi S, Banting S (1992) Endoscopic oesophagectomy through a right thoracoscopic approach. J R Coll Surg Edinb 37:7–11
Palanivelu C, Prakash A, Senthilkumar R, Senthilnathan P, Parthasarathi R, Rajan PS, Venkatachlam S (2006) Minimally invasive esophagectomy: thoracoscopic mobilization of the esophagus and mediastinal lymphadenectomy in prone position–experience of 130 patients. J Am Coll Surg 203:7–16
Osugi H, Takemura M, Lee S, Nishikawa T, Fukuhara K, Iwasaki H, Higashino M (2005) Thoracoscopic esophagectomy for intrathoracic esophageal cancer. Ann Thorac Cardiovasc Surg 11:221–227
Noshiro H, Miyake S (2013) Thoracoscopic esophagectomy using prone positioning. Ann Thorac Cardiovasc Surg 19:399–408
Gockel I, Kneist W, Keilmann A, Junginger T (2005) Recurrent laryngeal nerve paralysis (RLNP) following esophagectomy for carcinoma. Eur J Surg Oncol 31:277–281
Swanson SJ, Batirel HF, Bueno R, Jaklitsch MT, Lukanich JM, Allred E, Mentzer SJ, Sugarbaker DJ (2001) Transthoracic esophagectomy with radical mediastinal and abdominal lymph node dissection and cervical esophagogastrostomy for esophageal carcinoma. Ann Thorac Surg 72:1918–1924
van Sandick JW, van Lanschot JJ, ten Kate FJ, Tijssen JG, Obertop H (2002) Indicators of prognosis after transhiatal esophageal resection without thoracotomy for cancer. J Am Coll Surg 194:28–36
McKinney SM, Sieniek M, Godbole V, Godwin J, Antropova N, Ashrafian H, Back T, Chesus M, Corrado GS, Darzi A, Etemadi M, Garcia-Vicente F, Gilbert FJ, Halling-Brown M, Hassabis D, Jansen S, Karthikesalingam A, Kelly CJ, King D, Ledsam JR, Melnick D, Mostofi H, Peng L, Reicher JJ, Romera-Paredes B, Sidebottom R, Suleyman M, Tse D, Young KC, De Fauw J, Shetty S (2020) International evaluation of an AI system for breast cancer screening. Nature 577:89–94
Esteva A, Kuprel B, Novoa RA, Ko J, Swetter SM, Blau HM, Thrun S (2017) Dermatologist-level classification of skin cancer with deep neural networks. Nature 542:115–118
Berzin TM, Topol EJ (2020) Adding artificial intelligence to gastrointestinal endoscopy. Lancet (London, England) 395:485
Shelhamer E, Long J, Darrell T (2017) Fully convolutional networks for semantic segmentation. IEEE Trans Pattern Anal Mach Intell 39:640–651
Kitaguchi D, Takeshita N, Matsuzaki H, Hasegawa H, Honda R, Teramura K, Oda T, Ito M (2021) Computer-assisted real-time automatic prostate segmentation during TaTME: a single-center feasibility study. Surg Endosc 35:2493–2499
Madani A, Namazi B, Altieri MS, Hashimoto DA, Rivera AM, Pucher PH, Navarrete-Welton A, Sankaranarayanan G, Brunt LM, Okrainec A, Alseidi A (2020) Artificial intelligence for intraoperative guidance: using semantic segmentation to identify surgical anatomy during laparoscopic cholecystectomy. Ann Surg. https://doi.org/10.1097/SLA.0000000000004594
Mascagni P, Vardazaryan A, Alapatt D, Urade T, Emre T, Fiorillo C, Pessaux P, Mutter D, Marescaux J, Costamagna G, Dallemagne B, Padoy N (2020) Artificial intelligence for surgical safety: automatic assessment of the critical view of safety in laparoscopic cholecystectomy using deep learning. Ann Surg. https://doi.org/10.1097/SLA.0000000000004351
Yu KH, Beam AL, Kohane IS (2018) Artificial intelligence in healthcare. Nat Biomed Eng 2:719–731
Gulshan V, Peng L, Coram M, Stumpe MC, Wu D, Narayanaswamy A, Venugopalan S, Widner K, Madams T, Cuadros J, Kim R, Raman R, Nelson PC, Mega JL, Webster DR (2016) Development and validation of a deep learning algorithm for detection of diabetic retinopathy in retinal fundus photographs. JAMA 316:2402–2410
Randolph GW, Dralle H, Abdullah H, Barczynski M, Bellantone R, Brauckhoff M, Carnaille B, Cherenko S, Chiang FY, Dionigi G, Finck C, Hartl D, Kamani D, Lorenz K, Miccolli P, Mihai R, Miyauchi A, Orloff L, Perrier N, Poveda MD, Romanchishen A, Serpell J, Sitges-Serra A, Sloan T, Van Slycke S, Snyder S, Takami H, Volpi E, Woodson G (2011) Electrophysiologic recurrent laryngeal nerve monitoring during thyroid and parathyroid surgery: international standards guideline statement. Laryngoscope 121(Suppl 1):S1-16
Schneider R, Randolph GW, Dionigi G, Wu CW, Barczynski M, Chiang FY, Al-Quaryshi Z, Angelos P, Brauckhoff K, Cernea CR, Chaplin J, Cheetham J, Davies L, Goretzki PE, Hartl D, Kamani D, Kandil E, Kyriazidis N, Liddy W, Orloff L, Scharpf J, Serpell J, Shin JJ, Sinclair CF, Singer MC, Snyder SK, Tolley NS, Van Slycke S, Volpi E, Witterick I, Wong RJ, Woodson G, Zafereo M, Dralle H (2018) International neural monitoring study group guideline 2018 part I: staging bilateral thyroid surgery with monitoring loss of signal. Laryngoscope 128(Suppl 3):S1-s17
Gelpke H, Grieder F, Decurtins M, Cadosch D (2010) Recurrent laryngeal nerve monitoring during esophagectomy and mediastinal lymph node dissection. World J Surg 34:2379–2382
Zhong D, Zhou Y, Li Y, Wang Y, Zhou W, Cheng Q, Chen L, Zhao J, Li X, Yan X (2014) Intraoperative recurrent laryngeal nerve monitoring: a useful method for patients with esophageal cancer. Dis Esophagus 27:444–451
Hikage M, Kamei T, Nakano T, Abe S, Katsura K, Taniyama Y, Sakurai T, Teshima J, Ito S, Niizuma N, Okamoto H, Fukutomi T, Yamada M, Maruyama S, Ohuchi N (2017) Impact of routine recurrent laryngeal nerve monitoring in prone esophagectomy with mediastinal lymph node dissection. Surg Endosc 31:2986–2996
Kobayashi H, Kondo M, Mizumoto M, Hashida H, Kaihara S, Hosotani R (2018) Technique and surgical outcomes of mesenterization and intra-operative neural monitoring to reduce recurrent laryngeal nerve paralysis after thoracoscopic esophagectomy: a cohort study. Int J Surg (London, England) 56:301–306
Tsang RK, Law S (2016) Adaptation of continuous intraoperative vagus nerve stimulation for monitoring of recurrent laryngeal nerve during minimally invasive esophagectomy. World J Surg 40:137–141
Acknowledgements
We greatly appreciate the members of the Division of Esophageal Surgery for their critical discussion of our manuscript. We thank the members of the Surgical Device Innovation Office for reviewing and discussing the study. We also thank Kelly Zammit, BVSc and Coren Walters-Stewart, PhD, from Edanz (https://jp.edanz.com/ac), for editing a draft of this manuscript.
Funding
This work was supported by the National Cancer Center Research and Development Foundation, Budding Researchers Program [Grant Number 2020-S-3]. Drs. Kazuma Sato, Takeo Fujita, Hiroki Matsuzaki, and Nobuyoshi Takeshita are co-founders of Interpretable AI.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Kazuma Sato, Takeo Fujita, Hiroki Matsuzaki, Nobuyoshi Takeshita, Hisashi Fujiwara, Shuichi Mistunaga, Takashi Kojima, Kensaku Mori, Hiroyuki Daiko have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article was updated to This article was updated to add new affiliation for authors Kazuma Sato and Shuichi Mitsunaga.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 50698 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sato, K., Fujita, T., Matsuzaki, H. et al. Real-time detection of the recurrent laryngeal nerve in thoracoscopic esophagectomy using artificial intelligence. Surg Endosc 36, 5531–5539 (2022). https://doi.org/10.1007/s00464-022-09268-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09268-w