Abstract
Background
Among bariatric surgery patients, body mass index (BMI) does not fully capture the severity of obesity and it may be complicated to stratify patients at higher risk of peri-operative complications. In our study, we surveyed the MBSAQIP database to determine whether bariatric patients with metabolic syndrome (MetS) are at higher risk for peri-operative complications.
Methods
MBSAQIP database was used to investigate the correlation between MetS and perioperative outcomes. All patients between 2015 and 2018, ≥ 18 years old, who underwent primary bariatric surgery were included. Patients were excluded if they underwent natural orifice transluminal endoscopic surgery or had surgery performed by gastroenterologist or interventional radiologist. We modified the International Diabetes Federation definition of MetS for our study to select patients with BMI > 30 in addition to two or more of the following comorbidities: hypertension, hyperlipidemia, or diabetes. The primary outcome was perioperative mortality. Secondary outcomes included post-operative surgical site infections (SSI), perioperative MI, stroke, acute renal failure, transfusion requirement, readmission, conversion to open and reoperation.
Results
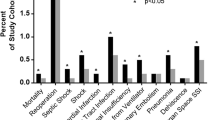
Between 2015 and 2018, 760,076 bariatric operations were performed. 670,935 met criteria for analysis. 190,239 patients were identified to have MetS. Patients with MetS were found to have higher odds of death (OR 2.32; 95% CI 1.97–2.72), SSI (OR 1.39; 95% CI 1.31–1.48), perioperative MI (OR 4.70; 95% CI 3.42–6.45), stroke (OR 3.30; 95% CI 2.08–5.24), acute renal failure (OR 3.04; 95% CI 2.48–3.72), and transfusion requirement (OR 1.30; 95% CI 1.33–1.39).
Conclusion
Patients with metabolic syndrome are at increased odds of peri-operative complications after bariatric surgery.

Adapted from Table 1, "IDF Consensus Worldwide Definition of the Metabolic Syndrome." International Diabetes Federation. (2006, updated 7/26/2020). BMI body mass index, BP blood pressure, HDL high-density lipoprotein
Similar content being viewed by others
References
World Health Organization (2020) Obesity and overweight. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
O’Neill S, O’Driscoll L (2015) Metabolic syndrome: a closer look at the growing epidemic and its associated pathologies. Obes Rev 16:1–12
Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA et al (2009) Harmonizing the metabolic syndrome: a joint interim statement of the international diabetes federation task force on epidemiology and prevention; national heart, lung, and blood institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 120:1640–1645
Sookoian S, Pirola CJ (2011) Metabolic syndrome: from the genetics to the pathophysiology. Curr Hypertens Rep 13:149–157
Saklayen MG (2018) The global epidemic of the metabolic syndrome. Curr Hypertens Rep 20:12
Cordero P, Li J, Oben JA (2017) Bariatric surgery as a treatment for metabolic syndrome. J R Coll Physicians Edinb 47:364–368
Arterburn DE, Bogart A, Sherwood NE, Sidney S, Coleman KJ, Haneuse S et al (2013) A multisite study of long-term remission and relapse of type 2 diabetes mellitus following gastric bypass. Obes Surg 23:93–102
Sjöström L, Peltonen M, Jacobson P, Ahlin S, Andersson-Assarsson J, Anveden Å et al (2014) Association of bariatric surgery with long-term remission of type 2 diabetes and with microvascular and macrovascular complications. JAMA 311:2297–2304
Sjöström L, Peltonen M, Jacobson P, Sjöström CD, Karason K, Wedel H et al (2012) Bariatric surgery and long-term cardiovascular events. JAMA 307:56–65
Hanipah ZN, Schauer PR (2020) Bariatric surgery as a long-term treatment for type 2 diabetes/metabolic syndrome. Annu Rev Med 71:1–15
Batsis JA, Romero-Corral A, Collazo-Clavell ML, Sarr MG, Somers VK, Lopez-Jimenez F (2008) Effect of bariatric surgery on the metabolic syndrome: a population-based, long-term controlled study. Mayo Clin Proc 83:897–906
Du X, Fu XH, Peng BQ, Luo R, Hu JK, Cheng Z (2018) Resolution of metabolic syndrome and related metabolic disorders after bariatric surgery: comparison of sleeve gastrectomy and gastric bypass. Surg Obes Relat Dis 14:1348–1356
Adams TD, Davidson LE, Litwin SE, Kim J, Kolotkin RL, Nanjee MN et al (2017) Weight and metabolic outcomes 12 years after gastric bypass. N Engl J Med 377:1143–1155
Puzziferri N, Roshek TB 3rd, Mayo HG, Gallagher R, Belle SH, Livingston EH (2014) Long-term follow-up after bariatric surgery: a systematic review. JAMA 312:934–942
Glance LG, Wissler R, Mukamel DB, Li Y, Diachun CA, Salloum R et al (2010) Perioperative outcomes among patients with the modified metabolic syndrome who are undergoing noncardiac surgery. Anesthesiology 113:859–872
Edelstein AI, Lovecchio F, Delagrammaticas DE, Fitz DW, Hardt KD, Manning DW (2017) The impact of metabolic syndrome on 30-day complications following total joint arthroplasty. J Arthroplasty 32:362–366
Selph JP, Whited WM, Smith AB, Matthews J, Pruthi RS, Wallen EM et al (2014) Metabolic syndrome as a predictor for postoperative complications after urologic surgery. Urology 83:1051–1059
Shariq OA, Fruth KM, Hanson KT, Cronin PA, Richards ML, Farley DR et al (2018) Metabolic syndrome is associated with increased postoperative complications and use of hospital resources in patients undergoing laparoscopic adrenalectomy. Surgery 163:167–175
Shariq OA, Hanson KT, McKenna NP, Kelley SR, Dozois EJ, Lightner AL et al (2019) Does metabolic syndrome increase the risk of postoperative complications in patients undergoing colorectal cancer surgery? Dis Colon Rectum 62:849–858
Tanaka A, Perlick A, Miller CC 3rd, Sandhu HK, Afaq S, Safi HJ et al (2018) Metabolic syndrome but not obesity adversely affects outcomes after open aortoiliac bypass surgery. Ann Vasc Surg 46:155–161
Zmistowski B, Dizdarevic I, Jacovides CL, Radcliff KE, Mraovic B, Parvizi J (2013) Patients with uncontrolled components of metabolic syndrome have increased risk of complications following total joint arthroplasty. J Arthroplasty 28:904–907
Surgeons ACo (2019) MBSAQIP standards manual 1996–2021
International Diabetes Federation (2006) IDF consensus worldwide definition of the metabolic syndrome. https://www.idf.org/e-library/consensus-statements/60-idfconsensus-worldwide-definitionof-the-metabolic-syndrome.html. Accessed 18 May 2021
Piché ME, Tchernof A, Després JP (2020) Obesity phenotypes, diabetes, and cardiovascular diseases. Circ Res 126:1477–1500
Csige I, Ujvárosy D, Szabó Z, Lőrincz I, Paragh G, Harangi M et al (2018) The impact of obesity on the cardiovascular system. J Diabetes Res 2018:3407306
Mullen JT, Moorman DW, Davenport DL (2009) The obesity paradox: body mass index and outcomes in patients undergoing nonbariatric general surgery. Ann Surg 250:166–172
Tjeertes EK, Hoeks SE, Beks SB, Valentijn TM, Hoofwijk AG, Stolker RJ (2015) Obesity—a risk factor for postoperative complications in general surgery? BMC Anesthesiol 15:112
Blüher M (2019) Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol 15:288–298
Goossens GH (2017) The metabolic phenotype in obesity: fat mass, body fat distribution, and adipose tissue function. Obes Facts 10:207–215
Lak KL, Helm MC, Kindel TL, Gould JC (2019) Metabolic syndrome is a significant predictor of postoperative morbidity and mortality following bariatric surgery. J Gastrointest Surg 23:739–744
Varela JE, Hinojosa MW, Nguyen NT (2008) Bariatric surgery outcomes in morbidly obese with the metabolic syndrome at US academic centers. Obes Surg 18:1273–1277
Purnell JQ, Selzer F, Smith MD, Berk PD, Courcoulas AP, Inabnet WB et al (2014) Metabolic syndrome prevalence and associations in a bariatric surgery cohort from the longitudinal assessment of bariatric surgery-2 study. Metab Syndr Relat Disord 12:86–94
Inabnet WB 3rd, Winegar DA, Sherif B, Sarr MG (2012) Early outcomes of bariatric surgery in patients with metabolic syndrome: an analysis of the bariatric outcomes longitudinal database. J Am Coll Surg 214:550–556
Funding
Non-funded research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
The author Matthew Sarna declares no conflict of interest for this research. Andrew Luhrs serves as a consultant for Medtronic, Bard Davol, and Activ Surgical. Marcoandrea Giorgi’s spouse is currently employed as a regulatory manager at BD medical technology company.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sarna, M.J., Giorgi, M. & Luhrs, A.R. Metabolic syndrome as a predictor of perioperative outcomes in primary bariatric surgery, a MBSAQIP survey. Surg Endosc 36, 6122–6128 (2022). https://doi.org/10.1007/s00464-021-08954-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08954-5