Abstract
Background
Ureteral injury is the most common urological complication of pelvic surgery, with a reported incidence during colon resection of 0.3–1.5%. Ureteral stenting is commonly performed preoperatively to prevent ureteral injury. Because tactile sensation is not reliable during laparoscopic surgery, the effect of the ureteral stent is considered limited. Recently, fluorescence imaging has been used in laparoscopic surgery. The Near-Infrared Ray Catheter (NIRC™) fluorescent ureteral catheter (NIRFUC) is a new catheter with built-in NIR fluorescent resin. This pilot study was performed to evaluate the utility of fluorescence ureteral navigation using the NIRFUC during laparoscopic colorectal surgery.
Methods
We evaluated the intraoperative utility of the NIRFUC and the short-term outcomes in 20 patients treated with colorectal surgery at Kawaguchi Municipal Medical Center between February and July 2020. In all, 18 patients with malignant tumors and 2 patients with benign disease, i.e., a sigmoid colovesical fistula, were included. Ten patients developed preoperative intestinal obstruction. One patient experienced preoperative perforation. Nine patients developed preoperative peritumoral abscesses. Laparoscopic surgery was performed with the VISERA ELITE2 system.
Results
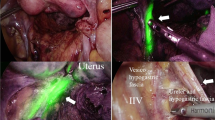
In all cases, the ureters were very clearly identified as fluorescent without the need for dissection. In all cases, only a moment was required to identify the ureter by fluorescence observation. In all cases, R0 resection was performed. The mean surgical duration was 334 min (161–1014), the mean blood loss was 10 ml (1–500), and the mean postoperative hospital stay was 11 days (8–47). There were no cases of ureteral injury.
Conclusion
The NIRFUC was very clearly identified as fluorescent in a moment during surgery without dissection around the ureter. Fluorescence ureteral navigation using the NIRFUC may make colorectal surgery easier and facilitate completion of complex minimally invasive surgery, especially during surgery in patients with invasion of the surrounding tissue or a history of pelvic surgery or radiation.






Similar content being viewed by others
References
Lezina MAST, Stoller ML (1991) Surgical ureteral injuries. Urology 38:497–506
Nam YS, Wexner SD (2002) Clinical value of prophylactic ureteral stent indwelling during laparoscopic colorectal surgery. J Korean Med Sci 17:633–635
Larach SW, Patankar SK, Ferrara A, Williamson PR, Perozo SE, Lord AS (1997) Complications of laparoscopic colorectal surgery. Dis Colon Rectum 40:592–596
Chahin F, Dwivedi AJ, Paramesh A, Chau W, Agrawal S, Chahin C, Kumar A, Tootla A, Tootla F, Silva YJ (2002) The implications of lighted ureteral stenting in laparoscopic colectomy. J Soc Laparoendosc Surg 6:49–52
Scala A, Huang A, Dowson HMP, Rockall TA (2007) Laparoscopic colorectal surgery? Results from 200 patients. Colorectal Dis 9:701–705
Fry DE, Milholen L, Harbrecht PJ (1983) Iatrogenic ureteral injury: options in management. Arch Surg 118:454–457
Goodno JA, Powers TW, Harris VD (1995) Ureteral injury in gynecologic surgery: a ten-year review in a community hospital. Am J Obstet Gynecol 172:1817–1822
Palaniappa NC (2012) Incidence of iatrogenic ureteral injury after laparoscopic colectomy. Arch Surg 147:267–271
Marcelissen TAT, Den Hollander PP, Tuytten TRAH, Sosef MN (2016) Incidence of iatrogenic ureteral injury during open and laparoscopic colorectal surgery: a single center experience and review of the literature. Surg Laparosc Endosc Percutan Tech 26:513–515
Chou MT, Wang CJ, Lien RC (2009) Prophylactic ureteral catheterization in gynecologic surgery: a 12-year randomized trial in a community hospital. Int Urogynecol J Pelvic Floor Dysfunct 20:689–693
Kuno K, Menzin A, Kauder HH, Sison C, Gal D (1998) Prophylactic ureteral catheterization in gynecologic surgery. Urology 52:1004–1008
Schaafsma BE, Mieog JSD, Hutteman M, Van der Vorst JR, Kuppen PJK, Löwik CWGM, Frangioni JV, Van de Velde CJH, Vahrmeijer AL (2011) The clinical use of indocyanine green as a near-infrared fluorescent contrast agent for image-guided oncologic surgery. J Surg Oncol 104:323–332
Ris F, Hompes R, Cunningham C, Lindsey I, Guy R, Jones O, George B, Cahill RA, Mortensen NJ (2014) Near-infrared (NIR) perfusion angiography in minimally invasive colorectal surgery. Surg Endosc 28:2221–2226
Jafari MD, Lee KH, Halabi WJ, Mills SD, Carmichael JC, Stamos MJ, Pigazzi A (2013) The use of indocyanine green fluorescence to assess anastomotic perfusion during robotic assisted laparoscopic rectal surgery. Surg Endosc 27:3003–3008
Sherwinter DA (2012) Transanal near-infrared imaging of colorectal anastomotic perfusion. Surg Laparosc Endosc Percutan Tech 22:433–436
Kudszus S, Roesel C, Schachtrupp A, Höer JJ (2010) Intraoperative laser fluorescence angiography in colorectal surgery: a noninvasive analysis to reduce the rate of anastomotic leakage. Langenbecks Arch Surg 395:1025–1030
Jafari MD, Wexner SD, Martz JE, McLemore EC, Margolin DA, Sherwinter DA, Lee SW, Senagore AJ, Phelan MJ, Stamos MJ (2015) Perfusion assessment in laparoscopic left-sided/anterior resection (PILLAR II): a multi-institutional study. J Am Coll Surg 220:82–92
Wada T, Kawada K, Takahashi R, Yoshitomi M, Hida K, Hasegawa S, Sakai Y (2017) ICG fluorescence imaging for quantitative evaluation of colonic perfusion in laparoscopic colorectal surgery. Surg Endosc 31:4184–4193
Ryu S, Suwa K, Kitagawa T, Aizawa M, Ushigome T, Okamoto T, Eto KEN, Yanaga K (2020) Evaluation of anastomosis with ICG fluorescence method using VISERA ELITE2 during laparoscopic colorectal cancer surgery. Anticancer Res 40:373–377
Watanabe J, Ota M, Suwa Y, Ishibe A, Masui H, Nagahori K (2016) Real-time indocyanine green fluorescence imaging-guided complete mesocolic excision in laparoscopic flexural colon cancer surgery. Dis Colon Rectum 59:701–705
Ryu S, Suwa K, Kitagawa T, Aizawa M, Ushigome T, Okamoto T, Eto KEN, Yanaga K (2019) Real-time fluorescence vessel navigation using indocyanine green during laparoscopic colorectal cancer surgery. Anticancer Res 39:3009–3013
Anayama T, Sato T, Hirohashi K, Miyazaki R, Yamamoto M, Okada H, Orihashi K, Inoue K, Kobayashi M, Yoshida M, Hanazaki K (2020) Near-infrared fluorescent solid material for visualizing indwelling devices implanted for medical use. Surg Endosc. https://doi.org/10.1007/s00464-020-07634-0,May2019
Quirke P, Steele R, Monson J, Grieve R, Khanna S, Couture J, O’Callaghan C, Myint AS, Bessell E, Thompson LC, Parmar M, Stephens RJ, Sebag-Montefiore D, MRC CR07/NCIC-CTG CO16 Trial Investigators, NCRI Colorectal Cancer Study Group (2009) Effect of the plane of surgery achieved on local recurrence in patients with operable rectal cancer: a prospective study using data from the MRC CR07 and NCIC-CTG CO16 randomised clinical trial. Lancet 373:821–828
Kusters M, Marijnen CAM, Van de Velde CJH, Rutten HJT, Lahaye MJ, Kim JH, Beets-Tan RGH, Beets GL (2010) Patterns of local recurrence in rectal cancer; a study of the Dutch TME trial. Eur J Surg Oncol 36:470–476
Nagtegaal ID, Quirke P (2008) What is the role for the circumferential margin in the modern treatment of rectal cancer? J Clin Oncol 26:303–312
Birbeck KF, Macklin CP, Tiffin NJ, Parsons W, Dixon MF, Mapstone NP, Abbott CR, Scott N, Finan PJ, Johnston D, Quirke P (2002) Rates of circumferential resection margin involvement vary between surgeons and predict outcomes in rectal cancer surgery. Ann Surg 235:449–457
García-Granero E, Faiz O, Muñoz E, Flor B, Navarro S, Faus C, García-Botello SA, Lledó S, Cervantes A (2009) Macroscopic assessment of mesorectal excision in rectal cancer. Cancer 115:3400–3411
Trakarnsanga A, Gonen M, Shia J, Goodman KA, Nash GM, Temple LK, Guillem JG, Paty PB, Garcia-Aguilar J, Weiser MR (2013) What is the significance of the circumferential margin in locally advanced rectal cancer after neoadjuvant chemoradiotherapy? Ann Surg Oncol 20:1179–1184
Siddighi S, Yune JJ, Hardesty J (2014) Indocyanine green for intraoperative localization of ureter. Am J Obstet Gynecol 211:436.e1–2
Mandovra P, Kalikar V, Patankar RV (2019) Real-Time visualization of ureters using indocyanine green during laparoscopic surgeries: can we make surgery safer? Surg Innov 26:464–468
Barnes TG, Hompes R, Birks J, Mortensen NJ, Jones O, Lindsey I, Guy R, George B, Cunningham C, Yeung TM (2018) Methylene blue fluorescence of the ureter during colorectal surgery. Surg Endosc 32:4036–4043
Al-Taher M, Van den Bos J, Schols RM, Bouvy ND, Stassen LPS (2016) Fluorescence ureteral visualization in human laparoscopic colorectal surgery using methylene blue. J Laparoendosc Adv Surg Tech A 26:870–875
Matsui A, Tanaka E, Choi HS, Kianzad V, Gioux S, Lomnes SJ, Frangioni JV (2010) Real-Time, near-infrared, fluorescence-guided identification of the ureters using methylene blue. Surgery 148:78–86
Chahin F, Dwivedi AJ, Paramesh A, Chau W, Agrawal S, Chahin C, Kumar A, Tootla A, Tootla F, Silva Y (2002) The implications of lighted ureteral stenting in laparoscopic colectomy. JSLS 6:49–52
Kaku S, Shimizu Y, Wakinoue S, Takebayashi A, Takashima A, Tarumoto Y, Nakagawa T, Kita N, Takahashi K, Murakami T (2010) Prevention of ureteral damage by using ureteral illuminating catheter during laparoscopic surgery. Jpn J Gynecol Obstet Endosc 26:541–544 (in Japanese)
Lee Z, Kaplan J, Giusto L, Eun D (2016) Prevention of iatrogenic ureteral injuries during robotic gynecologic surgery: a review. Am J Obstet Gynecol 214:566–571
Uno K, Ueno T, Yamada T, Takeda T, Tano S, Suzuki T, Kishigami Y, Oguchi H (2019) Prevention of ureteral injury during laparoscopic surgery with lymph node dissection using infrared illumination system. Jpn J Gynecol Obstet Endosc 35:328–332 (in Japanese)
Douissard J, Meyer J, Ris F, Liot E, Morel P, Buchs NC (2019) Iatrogenic ureteral injuries and their prevention in colorectal surgery: results from a nationwide survey. Colorectal Dis 21:595–602
McGlone TP (1982) Survival following extended operations for extracolonic invasion by colon cancer. Arch Surg 117:595–599
Hashiguchi Y, Muro K, Saito Y, Ito Y, Ajioka Y, Hamaguchi T, Hasegawa K, Hotta K, Ishida H, Ishiguro M, Ishihara S, Kanemitsu Y, Kinugasa Y, Murofushi K, Nakajima TE, Oka S, Tanaka T, Taniguchi H, Tsuji A, Uehara K, Ueno H, Yamanaka T, Yamazaki K, Yoshida M, Yoshino T, Itabashi M, Sakamaki K, Sano K, Shimada Y, Tanaka S, Uetake H, Yamaguchi S, Yamaguchi N, Kobayashi H, Matsuda K, Kotake K, Sugihara K, Japanese Society for Cancer of the Colon and Rectum (2020) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2019 for the treatment of colorectal cancer. Int J Clin Oncol 25:1–42
Acknowledgements
The authors would like to thank Professor Masashi Yoshida (Department of Surgery, International University of Health and Welfare Hospital) for his invaluable advice regarding fluorescence navigation surgery. The authors would like to thank the medical staff of the Kawaguchi Municipal Medical Center, especially Ms. Keika Iijima for her assistance with the colorectal cancer database. Finally, the authors especially thank Sho Ohno, Yusuke Sasaki, and Taketo Ichinose (Department of urology, Kawaguchi Municipal Medical Center).
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Shunjin Ryu, Atsuko Okamoto, Keigo Nakashima, Keigo Hara, Kota Ishida, Ryusuke Ito, Yukio Nakabayashi have no conflicts of interest or financial ties to disclose.
Ethical approval
This study was approved by the Research Ethics Committee of the Kawaguchi Municipal Medical Center (Saitama, Japan) (Approval number: 2020–3).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ryu, S., Okamoto, A., Nakashima, K. et al. Ureteral navigation using a fluorescent ureteral catheter during laparoscopic colorectal surgery. Surg Endosc 35, 4882–4889 (2021). https://doi.org/10.1007/s00464-021-08538-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08538-3