Abstract
Background
With standardization of laparoscopic technique of groin hernia repair, the focus of surgical outcome has shifted to lesser studied parameters like sexual function and fertility.
Methods
This prospective randomized study was conducted in a single surgical unit at a tertiary care hospital. A sample size of 144 was calculated with 72 in each group (Group 1 TEP and Group 2 TAPP). Primary outcomes measured included comparison of sexual function using BMFSI, qualitative semen analysis and ASA levels between patients undergoing TEP or TAPP repair. Semen analysis and ASA was measured pre-operatively and 3 months post-operatively.
Results
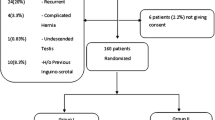
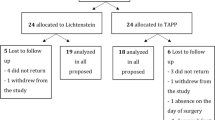
A total of 145 patients were randomized into two groups, TAPP (73) and TEP (72) patients. Both the groups were comparable in terms of demographic profile and hernia characteristics with majority of the patients in both the groups having unilateral inguinal hernia (89.0% in TAPP group and 79.2% in TEP group). Both the groups showed statistically significant improvement in overall sexual function score (BMFSI) at 3 months; however, there was no inter group difference. Both the groups were also comparable in terms of ASA and qualitative semen analysis.
Conclusion
Both TEP and TAPP repair are comparable in terms of sexual function and effect on semen analysis. Laparoscopic repair improves the overall sexual functions in patients with groin hernia.

Similar content being viewed by others
References
Skawran S, Weyhe D, Schmitz B, Belyaev O, Bauer KH (2011) Bilateral endoscopic total extraperitoneal (TEP) inguinal hernia repair does not induce obstructive azoospermia: data of a retrospective and prospective trial. World J Surg 35:1643–1648
Singh AN, Bansal VK, Misra MC, Kumar S, Rajeshwari S, Kumar A (2012) Testicular functions, chronic groin pain, and quality of life after laparoscopic and open mesh repair of inguinal hernia: a prospective randomized controlled trial. Surg Endosc 26(5):1304–1317
Beddy P, Ridgway PF, Geoghegan T, Peirce C, Govendcr P, Keane FBV et al (2006) Inguinal hernia repair protects testicular function: a prospective study of open and Laparoscopic herniorrhaphy. J Am Coll Surg 13:17–23
Junge K, Binnebösel M, Rosch R, Öttinger A, Stumpf M, Mühlenbruch G et al (2010) Influence of mesh materials on the integrity of the vas deferens following Lichtenstein hernioplasty: an experimental model. Hernia 12:621–626
Bischoff JM, Linderoth G, Aasvang EK, Werner MU, Kehlet H (2012) Dysejaculation after laparoscopic inguinal herniorrhaphy: a nationwide questionnaire study. Surg Endosc 26:979–983
Zieren J, Beyersdorff D, Beier KM, Müller JM (2001) Sexual function and testicular perfusion after inguinal hernia repair with mesh. Am J Surg 181:204–206
Myers E, Katherine M, Kavanagh D, Hurley M (2010) Laparoscopic (TEP) versus Lichtenstein inguinal hernia repair: a comparison of quality-of-life outcomes. World J Surg 34:3059–3064
SchutlzL GJ (1990) Laser laparoscopic herniorraphy; clinical trial preliminary results. J Laparoendosc Surg 1:41–45
Bignell M, Partridge G, Mahon D, Rhodes M (2012) Prospective randomized trial of laparoscopic (trans-abdominal pre-peritoneal-TAPP) versus open (mesh) repair for bilateral and recurrent inguinal hernia: incidence of chronic groin pain and impact on quality of life: results of 10 year follow-up. Hernia 16:635–640
Peiper C, Junge K, Klinge U, Strehlau E, Ottinger A, Schumpelick V (2006) Is there a risk of infertility after inguinal mesh repair? Experimental studies in the pig and the rabbit. Hernia 10:7–12
Hallen M, Westerdahl J, Nordin P, Gunnarsson U, Sandblom G (2012) Mesh hernia repair and male infertility: a retrospective register study. Surgery 151:94–98
Peeters E, Spiessens C, Oyen R, Wever LD, Dirk V, Freddy P, Miserez M (2010) Laparoscopic inguinal hernia repair in men with lightweight meshes may significantly impair sperm motility: a randomized controlled trial. Ann Surg 252:240–246
O’Leary MP, Fowler FJ, Lenderking WR, Barber B, Sagnier PP, Guess HA et al (1995 Nov) A brief male sexual function inventory for urology. Urology 46(5):697–706
Bittner R, Arregui ME, Bisgaard T, Dudai M, Ferzli GS, Fitzgibbons RJ (2011) Guidelines for laparoscopic (TAPP) and endoscopic (TEP) treatment of inguinal hernia [International Endohernia Society (IEHS)]. Surg Endosc 25(9):2773
Peeters E, Spiessens C, Oyen R, De Wever L, Vanderschueren D, Penninckx F, Miserez M (2014) Sperm motility after laparoscopic inguinal hernia repair with lightweight meshes: 3-year follow-up of a randomised clinical trial. Hernia 18:361–367
Štula I, Družijanić N, Sapunar A, Perko Z, Bošnjak N, Kraljević D (2014) Antisperm antibodies and testicular blood flow after inguinal hernia mesh repair. Surg Endosc 28:3413–3420
Funding
No funding received from any source.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Krishna Asuri, Aamir Mohammad, Om Prakash Prajapati, Rajesh Sagar, Atin Kumar, Mona Sharma, Pradeep Kumar Chaturvedi, Shardool Vikram Gupta, Sanjeet Kumar Rai, Mahesh Chandra Misra, Virinder Kumar Bansal declares that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asuri, K., Mohammad, A., Prajapati, O.P. et al. A prospective randomized comparison of sexual function and semen analysis following laparoscopic totally extraperitoneal (TEP) and transabdominal pre-peritoneal (TAPP) inguinal hernia repair. Surg Endosc 35, 2936–2941 (2021). https://doi.org/10.1007/s00464-020-07733-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07733-y